From the moment her daughter, still in the womb, was diagnosed with hypoplastic left heart syndrome, it became difficult for Monica Albertson to picture the future.
“When I was pregnant I was so worried,” Monica says. “You feel you have to prepare for the worst. I could never see her being a normal 3-year-old. But now she is. It’s amazing.”
 Today her daughter, Maya, loves to finger-paint and play in the sandbox, and is beginning to read. It’s been a long journey for the Albertsons, one that will continue as Maya grows up as a survivor of a severe single ventricle heart defect. Along the way, the family will have a dedicated team from the Cardiac Center at The Children’s Hospital of Philadelphia by its side.
Today her daughter, Maya, loves to finger-paint and play in the sandbox, and is beginning to read. It’s been a long journey for the Albertsons, one that will continue as Maya grows up as a survivor of a severe single ventricle heart defect. Along the way, the family will have a dedicated team from the Cardiac Center at The Children’s Hospital of Philadelphia by its side.
From before birth
Monica was approximately 4 months pregnant when her obstetrician noticed something wrong during an ultrasound. “As she was looking at the images, she said, ‘There’s a problem,’” Monica recalls. “She told us right away it would require open heart surgery after our baby was born.”
The doctor recommended they visit the Fetal Heart Program at The Children's Hospital of Philadelphia, one of the largest such programs in the world. Monica and her husband, Jesse, made the 90-minute drive from their home in Bethlehem, Pa, to meet with cardiologist Jack Rychik, MD, director of the Fetal Heart Program.
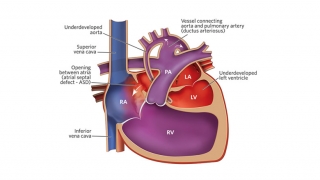
Dr. Rychik confirmed the diagnosis: hypoplastic left heart syndrome (HLHS), a single ventricle heart defect in which the left side of the heart is underdeveloped.
Dr. Rychik and his team explained that the baby would need a series of three open heart surgeries. After the surgeries, Maya’s heart would function as a one-sided pump, rather than a two-sided pump.
More About HLHS
The HLHS survival rate is much higher in children today than it was 30 years ago, when babies with HLHS did not survive beyond infancy. Doctors at Children's Hospital and other institutions have spent the last three decades working to continuously improve the surgeries that have now made survival possible.
As her pregnancy progressed, Monica and Jesse drove to CHOP approximately once a month for checkups. The team put together a careful plan for delivery and care after birth.
“We were very nervous,” Monica recalls, “but they did their best to make us feel comfortable. Anytime I needed to I could call and ask questions. They were all fantastic.”
The plan included the then newly opened Garbose Family Special Delivery Unit (SDU). This unit, the first of its kind, is for mothers carrying babies with diagnosed birth defects, including single ventricle heart defects like Maya’s. Delivery rooms are on the same floor as the Hospital’s state-of-the-art cardiac operating suite and Cardiac Intensive Care Unit, one of the largest and most sophisticated in the country.
Birth, then heart surgery
In mid-July, two weeks before her due date, Monica began to feel “strange.” She and her husband got in the car and drove to Philadelphia. The next day labor began and on July 15, 2008, Maya was born.
Even given her fragile condition, the family’s experience in the Special Delivery Unit was positive. Monica was able to try for a natural birth and to have the baby vaginally.
Monica and Jesse held Maya after she was born. Then Maya was handed into the adjacent infant stabilization room, just steps away.
Hospital staff started a drip of a medicine, prostaglandin, to help Maya survive until her first surgery, and began monitoring her heart rate and other vital signs.
“We could see everything they were doing through the glass window,” Monica recalls. “It wasn’t like she was taken away to some scary room somewhere. She was right there.”
After she was stabilized, Maya was taken to the Evelyn and Daniel M. Tabas Cardiac Intensive Care Unit (CICU) down the hall, and her parents were able to see her within a few hours. The Special Delivery Unit offers the unique benefit of keeping baby and mother close together. Otherwise, babies with severe single ventricle heart defects like HLHS are transported from their birth hospital to a pediatric center immediately after they are born, keeping mother and baby separated for days during the mother's recovery from labor.
Three-stage reconstructive surgery
J. William Gaynor, MD, one of the three cardiothoracic surgeons at Children's Hospital, spoke to the family about the first in the series of three open heart surgeries to treat Maya’s single ventricle heart defect: the Norwood procedure. Dr. Gaynor performed the Norwood procedure on Maya when she was just 3 days old.
The Cardiac Center's surgical team is one of the best and most experienced in fixing complex single ventricle heart defects such as hypoplastic left heart syndrome. Families travel from around the world seeking our team’s expertise for a better chance at hypoplastic left heart syndrome survival.
Six months later, Dr. Gaynor performed Maya's second-stage surgery, and will perform her third-stage surgery when she is 3 years old.
"He is fantastic," Monica says. "He answered all our questions. He checked on Maya and on us after surgery. He went to Japan and he called to check on her! He really cares about the kids and wants to make sure they're better. I can't say enough good things about Dr. Gaynor."
Maya's first three years
The past three years have been full of joys and challenges.
For example, Maya had a feeding tube in her stomach for her first year. Nurses at CHOP taught Monica to use the tube to feed Maya a mixture of breast milk and formula.
As is being seen with increasing frequency in children born with severe single ventricle heart defects, Maya experienced some delay in developmental milestones such as crawling and walking. An occupational therapist visits Maya at her home to help her with motor skills and with feeding.
Today, Maya is not as agile as some children on the playground, but she is very active and keeps up with her friends. She has not experienced cognitive or learning delays, and is already beginning to read.
Overall, her mom says, “She has been doing fantastic.”
The future
As the family waits for third-stage surgery, they visit Dr. Rychik every six months for checkups. After her surgery, Maya’s parents will enroll her in the Cardiac Center’s Single Ventricle Survivorship Clinic, part of the Fontan Rehabilitation, Wellness, Activity and Resilience Development (FORWARD) Program, led by Dr. Rychik. Most single ventricle defect survivors lead highly functional and active lives after early surgical intervention. There are, however, certain health problems, not limited to the heart, being recognized with increasing frequency.
Securing survival for patients with single ventricle heart defects was a challenge CHOP helped meet. The next challenge is to improve their quality of life and longevity. The Single Ventricle Survivorship Clinic brings together doctors and nurses from cardiology, gastroenterology and other specialties to provide focused care for these patients and conduct research to develop new and improved treatments to increase hypoplastic left heart syndrome survival.
“I believe Maya will live a pretty normal life, but I have fears about whether she will be able to have a long life,” Monica says. “That’s always in the back of your mind. But I feel good knowing that if they’re going to find the treatments and technology, it’s going to be at CHOP.
"CHOP is at the forefront, and we’re here.”
Originally posted: July 2011
Updated: September 2013