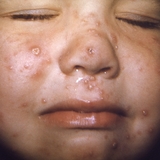
Varicella (Chickenpox): The Disease & Vaccines
It’s 1994.
A mom takes her 8-year-old daughter to the emergency room. Her daughter has had a low-grade fever for several days and blisters have started appearing over her entire body. The doctor diagnoses the girl with chickenpox. At first the mother is relieved because chickenpox is usually considered a “rite of passage”. Most kids get it. They stay home and are itchy for a couple of weeks, but that’s it.
But then the child starts to have difficulty breathing. Her breathing becomes rapid, shallow and difficult. A chest X-ray shows that the girl has pus between her lungs and chest wall (called an "empyema"). The pus causes one lung to be constricted. The child is admitted to the intensive care unit, but it is too late. The girl dies the next day, leaving mom to wonder how this could happen.
While chickenpox is often mild, it is not always mild. Before the chickenpox vaccine became available in 1995, one or two children in the U.S. died every week from chickenpox. Most of these children were previously healthy.

On the go? Watch or listen.
Get a summary of the information on this page:
The disease
What is chickenpox?
Chickenpox is an infection caused by varicella virus. This virus only infects people, and it’s highly contagious. It can spread in one of three ways:
- By coughing or sneezing
- Physical contact with broken blisters
- By virus particles sprayed in the air from broken blisters
The main symptom of chickenpox is a rash. A day or two before the rash, infected people may have fever, fatigue, lack of appetite and headache. The chickenpox rash usually begins on the chest, back and face before spreading to the rest of the body. The rash first appears as red bumps before turning into fluid-filled blisters. New groups of blisters, called crops, appear over several days. This staggered appearance means that a small area of the skin can have lesions in various stages of development: red bumps, fluid-filled blisters, and scabs. Someone with chickenpox can have 250-500 lesions. The rash can be itchy and if the fluid-filled blisters are scratched open, they can leave scars. Infected people can spread the virus to others from two days before the rash begins until all crops of the rash have become scabs.
The areas of broken skin increase the risk for bacteria to cause another infection, called a secondary infection. For example, a bacterium called Group A streptococcus, commonly known as "flesh-eating" bacteria, can cause severe, and sometimes fatal, disease. Chickenpox infections can also result in other severe complications like:
- Pneumonia (infection of the lungs)
- Encephalitis (infection of the brain)
- Lack of coordination and balance (called cerebral ataxia) — can occur before development of rash as well as weeks after recovery
- Damage to blood vessels causing profuse bleeding, including internal bleeding (called hemorrhagic bleeding)
- Sepsis (infection of the blood)
- Stroke — can occur in the months after recovery
- Inflammation of the heart, kidneys, testes, liver, appendix, joints, or iris
- Dehydration
Adults with chickenpox tend to have more severe illness and higher rates of death.
Infection with varicella during pregnancy can cause problems for the pregnant person and the baby. An infection during pregnancy increases the risk for pneumonia requiring mechanical ventilation and preterm delivery. Babies can be infected with varicella virus before birth causing small size at birth, shortened limbs, small head (called microcephaly), shrunken outer layer of the brain (called cortical atrophy), accumulation of cerebrospinal fluid in the brain and spinal cord (called hydrocephaly), developmental delays, eye disorders, and abnormalities of the muscles, digestive tract, urinary tract and circulatory system.
How contagious is chickenpox?
Chickenpox is very contagious. If one infected person spends several hours in a room of 100 susceptible people about 85 of them will get chickenpox.
The vaccine
How is the varicella vaccine made?
The chickenpox vaccine became available in 1995. The vaccine is a live, "weakened" form of natural varicella virus. The virus is "weakened" by growing it in cells that are different from the ones it infects in people. This process is called "cell culture adaptation" (see "How Are Vaccines Made?"). "Cell culture adaptation" changes natural varicella virus, so it does not infect our cells as efficiently when it is given in the vaccine.
Natural varicella virus normally grows in cells that line the skin or the back of the throat. Cells are the building blocks of all the different parts of the body, like skin, heart, muscles and lungs. Natural varicella virus reproduces itself thousands of times. The result can be mild or severe disease. We don’t know who will get mild disease and who will get severe disease when they get a natural chickenpox infection. During a chickenpox infection, the virus that is made in the infected person’s cells is passed on to the next person unchanged.
The process of "cell-culture adaptation" changes all of that. Natural varicella virus was first taken from a young child in Japan who had chickenpox. The family name of the child was Oka, so the strain of vaccine virus is called the "Oka" strain. The virus from the little boy was "grown" in human lung and embryo fibroblast cells. Fibroblast cells are the cells needed to hold skin and other connective tissue together. These cells were first obtained from two elective pregnancy terminations — one in England and one in Sweden in the early 1960s. These same embryonic cells have continued to grow in the laboratory and are used to make chickenpox vaccine today. To find out more about how the same cells can be used so many years later, check this article that describes cell passage, a common laboratory technique (see the section titled, “No additional fetuses needed”). The varicella virus used in the vaccine was also grown in guinea pig fibroblast cells.
By growing varicella virus in fibroblast cells, it became less able to grow in human cells that lined the back of the throat or skin.
When this adapted vaccine virus was given as a vaccine, it grew very poorly. The chickenpox vaccine virus reproduces itself probably fewer than 20 times (compared with thousands of times after natural infection). That is why natural varicella virus causes illness, but chickenpox vaccine virus doesn't. The good news is that the chickenpox vaccine virus reproduces enough to induce immunity against chickenpox that is lifelong. (See "How vaccines work.")
Who should get the chickenpox vaccine?
The chickenpox vaccine is given in two doses. The first dose is recommended between 12 and 15 months. The second dose is recommended between 4 and 6 years of age. Anyone who got only one dose should get a second dose. People not immunized before 7 years of age should get two doses of vaccine, but the time between doses varies by age:
- Those 7 to 12 years of age should receive the second dose at least 3 months after the first dose.
- Those 13 years and older should receive the second dose between 4 and 8 weeks after the first dose.
Does the varicella vaccine work?
Yes. The chickenpox vaccine was introduced in the U.S. in 1995. A second dose was recommended in 2006. Since then, cases of chickenpox have decreased by about 97%, but chickenpox infections still occur fairly frequently in the U.S. Before a vaccine was available, chickenpox caused millions of cases and about 100 deaths each year in the U.S. Now, about 100,000 to 150,000 cases occur each year with fewer than 30 deaths.
What are the side effects of the chickenpox vaccine?
Side effects of the chickenpox vaccine include tenderness in the area where the shot was given. Some people also have a low-grade fever. About 4-6 of every 100 people who get the vaccine develop a rash. The rash usually occurs around the area of the shot, but it can also appear on other parts of the body. Most people who get the rash after vaccination only have about 10- 30 blisters. The rash can develop about 5 to 26 days after vaccination.
If someone develops blisters, they can, on rare occasions, spread chickenpox to someone who is susceptible (i.e., a person who has not been immunized and never had a varicella infection). The blisters contain viruses, so a susceptible person who comes into contact with the blisters before they scab can get chickenpox. To decrease the chance for this, a vaccinated person who develops a rash should cover the rash and avoid contact with susceptible people until the rash scabs or heals.
The chickenpox vaccine contains gelatin, so people severely allergic to gelatin cannot get it. Gelatin is also contained in foods, like Jell-O, so the allergy may already be known before it is time to get the vaccine. If it is not known whether someone has an allergy, you can stay at the location where the vaccine was given for 15-30 minutes. That way, if a reaction occurs, healthcare providers will be able to quickly assist. People with severe allergic reactions to previous doses of chickenpox vaccine or to other ingredients in the vaccine should not get it.
People who are severely immune compromised or pregnant should not get the chickenpox vaccine. Children with a parent or sibling who has an inherited immune deficiency (one they were born with) should delay vaccination until their immune status is known. If they do not have the same condition, they will likely be able to get the vaccine.
Other questions you might have
My daughter had chickenpox at 10 months old, but now that she is 1 year old, her doctor said she should still get the chickenpox vaccine. Is this really necessary?
The Centers for Disease Control and Prevention (CDC) recommends vaccination of all children at 12 months of age who do not have evidence of immunity. Evidence can include:
- A diagnosis of chickenpox or shingles made by a healthcare provider
- Laboratory confirmation of disease
- Laboratory evidence of immunity (blood test)
Because many rashes are misclassified, the CDC states that “if there is any doubt that the illness was actually varicella [chickenpox], the child should be vaccinated.”
Your daughter could be tested for evidence of antibodies to chickenpox, but the test will require a blood draw and if it is negative, she will still need to get the vaccine. On the other hand, a dose of vaccine even if she has had chickenpox will not hurt her; it will make her immunity stronger.
If we immunize children against chickenpox, will they be more likely to develop shingles later in life?
Shingles is a rash with extremely painful blisters that occur along a nerve, usually on the face, chest or abdomen. Shingles usually affects people 45 years old or older. It occurs when the varicella virus reawakens (or reactivates). Although people usually completely recover from a chickenpox infection, the virus never really goes away. It lives silently in the nervous system and, when we get older, it can occasionally reawaken, causing shingles.
Like the natural virus, the vaccine virus can also live silently in the nervous system. However, it has been shown that the varicella vaccine virus is much less likely to reawaken. If it does reawaken, it is much less likely to cause severe shingles compared with natural varicella virus. This makes sense because the varicella vaccine virus is much weaker than the natural virus.
The important question to ask yourself is whether you would rather have version that reproduces thousands of times (natural or “wildtype” virus) or the version that reproduces less than 20 times (vaccine virus) living in your nerve cells. Of note: Since the chickenpox vaccine became available, the incidence of shingles has decreased in the U.S.
If we immunize children with the chickenpox vaccine, won't they be more likely to get chickenpox as adults?
Chickenpox is much more likely to cause severe disease in adults than in children. Adults are 10 times more likely to be hospitalized when they have chickenpox compared with children. Given this, it would never be desirable to have the vaccine shift chickenpox disease from childhood to adulthood. The vaccine has now been out long enough that we can be confident this is unlikely:
- Several studies have shown that immunity to chickenpox lasts at least 20 years and is probably life-long.
- The chickenpox vaccine is made in a manner similar to the rubella vaccine. We immunize little girls with rubella vaccine to protect them from getting rubella when they become pregnant as adults. That means we are preventing something that typically occurs 20, 30, or even 40 years after vaccination. This strategy has worked. We eliminated rubella from the U.S., and babies are no longer born with birth defects from maternal infections during pregnancy.
- Measles vaccine, also made in a similar way, has been successfully used for more than 60 years without seeing a shift in age of disease..
Therefore, fading immunity, and a consequent shift of chickenpox infections from childhood to adulthood, is extremely unlikely to occur.
Should teenagers and adults get the varicella vaccine?
Any teenager or adult who has not had chickenpox or the chickenpox vaccine should receive the vaccine. Adults are 10 times more likely than children to be hospitalized with severe consequences of chickenpox.
I got the chickenpox vaccine as an adult, but I got a fever and a rash, so should I get the second dose of the vaccine?
Like children, adults can develop a fever and rash after getting the chickenpox vaccine. This reaction indicates that your body has made an immune response to the vaccine. It is less likely to have the same thing happen after the second dose. The second dose will strengthen your immunity, so if you are exposed to chickenpox virus, you will be better protected.
The second dose should be received four to eight weeks after the first dose for those 13 years and older. A child between 7 and 12 years of age should get the second dose three months after the first dose.
Why is varicella called chickenpox?
Unlike some other nicknames, the origin of chickenpox is less clear. Several ideas have been suggested. One is that the disease was not that bad, so it was called chickenpox. Another suggestion is that it distinguished this infection from other common terms at the time: syphilis was referred to as the great pox and smallpox was also prevalent. Some people suggest it came from the look of the rash — either as marks made by the beak of a chicken or like soaked chickpeas. If you are interested in more details, you can check this paper.
Relative risks and benefits
Do the benefits of chickenpox the vaccine outweigh its risks?
Before the chickenpox vaccine became available in 1995, about 4 million children were infected every year. In addition, chickenpox caused about 10,000 hospitalizations and 100 deaths a year. Most hospitalizations and deaths occurred in previously healthy young children.
So, although chickenpox causes much less severe disease, fewer permanent disabilities and fewer deaths than some other vaccine-preventable diseases, it can still occasionally cause severe disease in children. On the other hand, the chickenpox vaccine does not have serious side effects. Therefore, the benefits of the chickenpox vaccine clearly outweigh its risks.
Disease risks
- Rash (250 -500 blisters)
- Secondary bacterial infections, such as with Group A streptococcus (flesh-eating bacteria)
- Pneumonia (infection of the lungs)
- Encephalitis (infection of the brain)
- Lack of coordination and balance (called cerebral ataxia) — can occur before development of rash as well as weeks after recovery
- Damage to blood vessels causing profuse bleeding, including internal bleeding (called hemorrhagic bleeding)
- Sepsis (infection of the blood)
- Stroke — can occur in the months after recovery
- Inflammation of the heart, kidneys, testes, liver, appendix, joints, or iris
- Dehydration
- Death
Vaccine risks
- Pain and tenderness at the injection site
- Low-grade fever
- Rash (4-6 of 100 recipients)
References
Orenstein W, Offit PA, Edwards KM and Plotkin SA. Varicella vaccine in Plotkin’s Vaccines, 8th Edition, 2024,1215-1250.
Chickenpox Vaccine Saves Lives and Prevents Serious Illness Infographic. Centers for Disease Control and Prevention. May 9, 2024
The Varicella Vaccination Program in the United States: 25 Years of Saving Lives and Preventing Illness, The Journal of Infectious Diseases, November 1, 2022.
Impact of U.S. Chickenpox Vaccination Program, Centers for Disease Control and Prevention. April 22, 2024.
Reviewed by Paul A. Offit, MD on May 30, 2025