What are arteriovenous malformations
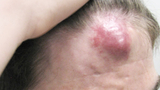
Arteriovenous malformations (AVM) are high-flow vessel abnormalities characterized by dilated arteries that connect directly with draining veins without any capillaries in between. The skin overlying an AVM is usually warmer than the rest of the body, pulsatile, and sometimes even has a detectable vibration (also called a thrill) due to the turbulent high blood flow.
A stethoscope may detect a low rumble (also called a bruit) with each heartbeat. AVMs can cause significant enlargement of the involved area, resulting in soft tissue distortion and bony overgrowth. Growth hormones may result in significant enlargement of the AVM during puberty.
An MRI scan combined with an MRA scan can help to determine the extent and pattern of the abnormal vessels, which impacts possible treatment options. An MRI scan demonstrates the location and extent of an arteriovenous malformation. An MRA scan shows both normal arteries and the abnormal arteries that feed the AVM.
An arteriogram will offer precise anatomic detail as well as a possible opportunity for treatment. In some cases genetic testing is indicated.
Treatment
Treatment may consist of the following:
- Conservative observation. In many cases small or asymptomatic AVMs can be followed without requiring treatment.
- Palliative or sometimes curative embolization (selective, intentional clotting of the feeding arterial branches combined with injection of the draining veins). This is done with catheters and injection of clotting chemicals or metallic coils by an interventional radiologist. Sometimes blockage of the feeding arteries and the draining veins will cure an AVM. More often, the benefit is temporary, as new arteries will usually begin to feed the AVM
- Radical surgical removal (sometimes combined with pre-surgical embolization). Surgery aims to cure the AVM by complete removal. These challenging cases may require blood transfusions because of the risk for significant intraoperative bleeding. Intentional blockage of the feeding arteries by interventional radiology is often done the day before surgery to decrease the bleeding risk
Surgical removal with the intention of curing the malformation may warrant complex soft tissue reconstruction.
Resources to help
Comprehensive Vascular Anomalies Program (CVAP) Resources
Reviewed by David W. Low, MD
