What is glottic stenosis?
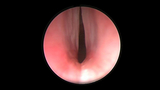
Glottic stenosis is a narrowing of the larynx (or voicebox) where the vocal cords are scarred together. This scarring can develop between the two vocal folds or on the tissue surrounding the vocal folds, which impedes their movement.
Posterior glottic stenosis (narrowing in the back of the vocal fold area) may occur in conjunction with subglottic stenosis. In 90 percent of cases, glottic stenosis is the result of prolonged endotracheal intubation. Ten percent of cases are congenital, or present at birth.
Signs and symptoms
The restricted outward motion of the vocal cords causes severe respiratory symptoms.
- Noisy breathing on inhalation and exhalation (Biphasic stridor)
- Shortness of breath with activity
- Difficulty eating
- Difficulty breathing
Testing and diagnosis
Endoscopic view of glottic stenosis in the pediatric airway.
To diagnose glottic stenosis, your child's doctor will first perform a flexible nasopharyngolaryngoscopy (NPL) in the office while the child is awake to examine the back of the throat, larynx and vocal cords. NPL will show the degree of vocal cord movement. Posterior glottic stenosis is suggested when there is reduced movement.
An important part of the diagnosis is differentiating glottic stenosis from vocal cord paralysis. In glottic stenosis, the vocal folds are immobilized by scar tissue. In vocal cord paralysis the nerves controlling the vocal cords are not functioning.
To differentiate between these conditions, the doctor will also perform a microlaryngoscopy and bronchoscopy in the operating room under general anesthesia to determine what condition is causing the respiratory symptoms. During these procedures, the vocal cords and arytenoids may be gently touched to determine if they are attached by scar tissue or if the vocal cord immobility is caused by paralysis.
GI, nutrition, and pulmonary evaluation are also necessary, so your child may have to see all of these specialists during his airway visit.
Glottic stenosis staging system
- Stage I: Glottic-interarytenoid scar; posterior commissure normal
- Stage II: Interarytenoid and posterior commissure scarring
- Stage III: Posterior commissure scarring and one cricoarytenoid joint scarred
- Stage IV: Posterior commissure scarring and both CA joints scarred
Treatment
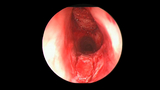
Posterior glottic stenosis may be treated endoscopically or with open surgery. Treatment typically depends on the size and thickness of the scar band.
Treating a small scar band
A small scar band may be treated endoscopically in the operating room under anesthesia. During the microlaryngoscopy and bronchoscopy, the scar band is identified and cut. The area may be gently dilated with a balloon catheter.
Treating a large scar band
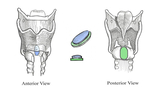
More significant scarring and narrowing of the larynx at the level of the vocal folds requires an open surgical procedure called a laryngotracheal reconstruction to divide the scar band and enlarge the airway with a cartilage graft. This can be performed in either a single-stage or double-stage fashion depending on whether or not the child already has a tracheostomy. The safest technique will be chosen by your surgeon and the airway team.
References
Bogdasarian RS, Olson NR. Posterior glottic laryngeal stenosis. Otolaryngol Head Neck Surg (1979). 1980 Nov-Dec;88(6):765-72.
What to know before your appointment
Prepare for your child's upcoming appointment with the Center for Pediatric Airway Disorders.
Resources to help
Center for Pediatric Airway Disorders Resources
We have created resources to help you find answers to your questions about airway disorders and feel confident with the care you are providing your child.
