What is laryngomalacia?
Laryngomalacia is a congenital softening of the tissues of the larynx (voice box) above the vocal cords. This is the most common cause of noisy breathing in infancy. The laryngeal structure is malformed and floppy, causing the tissues to fall over the airway opening and partially block it.
In most cases, laryngomalacia in infants is not a serious condition — they have noisy breathing, but are able to eat and grow. For these infants, laryngomalacia will resolve without surgery by the time they are 18 to 20 months old. However, a small percentage of babies with laryngomalacia do struggle with breathing, eating and gaining weight. These symptoms require prompt attention.
When to seek help
Go to the hospital immediately if your baby:
- Stops breathing for more than 10 seconds
- Turns blue around the lips while breathing noisily
- Pulls in the neck or chest without relief after being repositioned or awakened
Causes
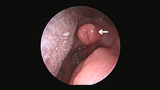
Laryngomalacia as seen in a child’s airway during microlaryngoscopy.
The exact cause of laryngomalacia is not known. Relaxation or a lack of muscle tone in the upper airway may be a factor. The malformation is usually present at birth or appears within the first month of life. Gastroesophageal reflux (GE reflux) may contribute to the severity of the symptoms. The noisy breathing is often worse when the infant is on his back or when crying.
Signs and symptoms
If your child is born with laryngomalacia, symptoms may be present at birth, and can become more obvious within the first few weeks of life. It is not uncommon for the noisy breathing to get worse before it improves, usually around 4 to 8 months of age. Most children outgrow laryngomalacia by 18 to 20 months of age. Symptoms include:
- Noisy breathing (stridor) — An audible wheeze when your baby inhales (breathes in). It is often worse when the baby is agitated, feeding, crying or sleeping on his back.
- High pitched sound
- Difficulty feeding
- Poor weight gain
- Choking while feeding
- Apnea (breathing stoppage)
- Pulling in neck and chest with each breath
- Cyanosis (turning blue)
- Gastroesophageal reflux (spitting, vomiting and regurgitation)
- Aspiration (inhalation of food into the lungs)
Testing and diagnosis
Your doctor will ask you some questions about your baby’s health problems and may recommend a test called a nasopharyngolaryngoscopy (NPL) to further evaluate your baby’s condition.
During this test, done in your doctor’s office, a tiny camera that looks like a strand of spaghetti with a light on the end is passed through your baby’s nostril and into the lower part of the throat where the larynx is. This allows your doctor to see your baby’s voice box.
If laryngomalacia is diagnosed, the doctor may want to do other diagnostic tests to evaluate the extent of your child’s problems and to see whether the lower airway is affected. These tests may include:
- X-ray of the neck
- Airway fluoroscopy
- Microlaryngoscopy and bronchoscopy (MLB)
- Esophagogastroduodenoscopy (EGD) and pH probe
- Functional endoscopic evaluation of the swallow (FEES)
Treatment
In 90 percent of cases, laryngomalacia resolves without treatment by the time your child is 18 to 20 months old. However, if the laryngomalacia is severe, your child’s treatment may include medication or surgery.
Medication
Your child’s doctor may prescribe an anti-reflux medication to help manage the gastroesophageal reflux (GERD). This is important because your child’s chronic neck and chest retractions from the laryngomalacia can worsen reflux. Also, the acid reflux can cause swelling above the vocal cords and worsen the noisy breathing.
Laryngomalacia surgery
A surgery called supraglottoplasty is the treatment of choice if your child's condition is severe. Symptoms that signal the need for laryngomalacia surgery include:
- Life-threatening apneas (stoppages of breathing)
- Significant blue spells
- Failure to gain weight with feeding
- Significant chest and neck retractions
- Need for extra oxygen to breathe
- Heart or lung issues related to your child's inability to get enough oxygen
This surgery may not completely eliminate the noisy breathing but it should help to:
- Reduce the severity of the symptoms
- Lessen the apneas (breathing stoppages)
- Reduce the extra oxygen requirements
- Improve swallowing
- Help your child gain weight
The safety of your child's swallow should be reevaluated after the surgical procedure.
Resources to help
Center for Pediatric Airway Disorders Resources
We have created resources to help you find answers to your questions about airway disorders and feel confident with the care you are providing your child.
