What is mucopolysaccharidosis type 1?
Mucopolysaccharidosis type 1 (MPS 1) is a rare lysosomal storage disorder characterized by an abnormal build-up of various toxic materials, called glycosaminoglycans (GAGs) in the body's cells. MPS 1 is a spectrum of disease ranging from a mild (attenuated) form, called Scheie, to severe disease, called Hurler syndrome. Hematopoietic stem cell transplantation and/or enzyme replacement therapy is the mainstay of treatment for individuals with severe MPS 1.
Causes of mucopolysaccharidosis type 1
MPS 1 is a genetic condition caused by disease-causing (pathogenic) changes in the IDUA gene. The IDUA gene provides the body with the instructions it needs to produce the alpha-L-iduronidase enzyme. The role of this enzyme is to break down the GAGs in the body. If the body does not produce enough of this enzyme, GAGs build up in various parts of the body and cause symptoms of disease.
MPS 1 is inherited in an autosomal recessive manner. This means that in order to have the condition, an individual needs to have two disease-causing changes in the DNA. One change must be present in the copy of the IDUA gene that the individual inherits from their mother, and another change must be present in the copy of the IDUA gene the individual inherits from their father. In individuals with MPS 1, neither copy of the IDUA gene is able to provide the proper instructions to produce the enzyme.
Symptoms of mucopolysaccharidosis type 1
Children with MPS 1 often have no signs or symptoms of the condition at birth. However, babies with severe MPS 1 generally begin to show symptoms within the first year of life. Children with a more mild form of the disease tend to show symptoms later in childhood.
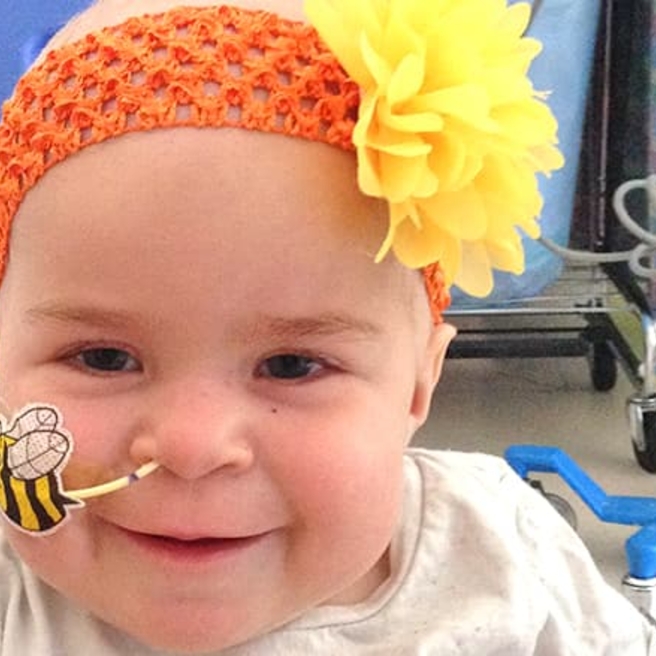
In the severe form of MPS 1, coarsening facial features, skeletal and spinal deformities, and developmental delays are present within the first 1-2 years of life. Individuals with severe MPS 1 may have a large head (macrocephaly), clouding of the cornea, hearing loss, recurrent ear and upper respiratory infections, enlarged organs including liver, spleen and vocal cords, heart disease, short stature, hernias, and carpal tunnel syndrome. In the more mild forms, symptoms can vary in severity. Some children with the milder forms have no intellectual impairment.
Diagnosis of mucopolysaccharidosis type 1
Early diagnosis is challenging because the early symptoms can be attributed to many other more common disorders. However, the addition of MPS 1 to state newborn screening programs has helped identify affected children shortly after birth. Diagnosis of MPS 1 is typically established in symptomatic individuals who have at least one of two additional findings:
- Low alpha-L-iduronidase enzyme activity
- Two pathogenic genetic variants identified through IDUA gene sequencing
In addition to this testing, elevated levels of GAGs in urine and/or blood can support a clinical diagnosis of MPS 1.
Treatment for mucopolysaccharidosis type 1
There is no cure for MPS 1, however, there are effective treatments that are proven to slow the progression of disease. Hematopoietic stem cell transplantation (HSCT) can help some patients who have the severe form of the disease, and is generally recommended within the first 1-2 years of life.
Enzyme replacement therapy (ERT) is recommended for individuals with the milder forms of MPS 1. ERT uses an intravenous solution to replace the deficient or missing alpha-L-iduronidase enzyme in the body.
Neither treatment will completely prevent symptoms of disease, and other treatments/procedures are still commonly recommended, even for patients who have undergone transplant. Regardless of severity, individuals with MPS 1 need lifelong follow up with a metabolic specialist to ensure appropriate care.
Treatment is also geared towards management of the individual symptoms of MPS 1. Patients are followed at least every six months by the Lysosomal Storage Disease (LSD) Center at Children’s Hospital of Philadelphia (CHOP) in the multidisciplinary MPS clinic which includes appointments with Physical Therapy and Developmental Pediatrics. Patients are also followed by other subspecialists including Pulmonology, Cardiology, and Orthopedics, among others.
The Cell and Gene Therapy Collaborative at Children’s Hospital of Philadelphia is conducting gene therapy clinical trials for MPS 1, with the aim of developing new gene therapies for this disease.
Resources to help
Lysosomal Storage Disease (LSD) Center Resources
Caring for a child with a lysosomal storage disease can be overwhelming. We have created resources to help you find answers to your questions and feel confident in the care you are providing your child.
Reviewed by Can Ficicioglu, MD, PhD, Nicole L. Luongo, Caitlin Menello, MS, LCGC