What is selective intrauterine growth restriction (also called selective fetal growth restriction)?
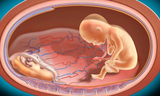
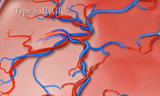
Monochorionic twins are twins that share a single placenta. Selective intrauterine growth restriction (sIUGR), also called selective fetal growth restriction (sFGR), occurs when there is unequal placental sharing which leads to suboptimal growth of one twin. In cases of sIUGR, the estimated fetal weight of the smaller, growth-restricted twin usually falls below the 10th percentile. This will usually result in more than a 25 percent weight difference between the twins.
sIUGR is estimated to occur in approximately 10 percent of monochorionic twin pregnancies. There are three types of sIUGR that are determined by the blood flow pattern in the umbilical artery of the growth-restricted twin.
Causes of sIUGR
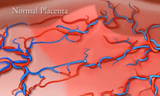
The principle cause for the development of sIUGR in monochorionic twins is unequal placental sharing. The growth-restricted twin has a smaller share of the placenta, which over time results in abnormal blood flow and less growth. This could lead to death of the growth-restricted twin. Because the shared placenta also contains shared blood vessels between the twins (vascular communications), sIUGR can also impact the development of the brain and nervous system in the normal twin (neurodevelopment).
Symptoms of sIUGR
There are no physical symptoms of sIUGR that you, as a mother, would feel. sIUGR is a diagnosis made exclusively through ultrasound examination.
Evaluation and diagnosis of sIUGR during pregnancy
Accurate diagnosis is extremely important in distinguishing sIUGR from other diagnoses such as twin-twin transfusion syndrome (TTTS). TTTS and sIUGR both involve a shared placenta, but are differentiated by amniotic fluid levels.
The differences between the two can be very subtle. In TTTS, there is a characteristic and progressive series of changes that happens to each twin. In sIUGR, the distribution of blood is more balanced, but because the growth-restricted twin has a much smaller portion of the placenta, the resistance in the umbilical artery is higher than normal, resulting in suboptimal fetal growth.
Watch this video to learn more about the differences between TTTS and sIUGR and how they are diagnosed.
If you are referred to CHOP’s Richard D. Wood Jr. Center for Fetal Diagnosis and Treatment (CFDT), you will be scheduled for a comprehensive, one-day evaluation. During this first visit, you will meet with multiple team members, including a genetic counselor, nurse coordinator and maternal-fetal medicine specialist. You’ll also meet with a research coordinator to discuss ongoing research studies.
Your evaluation will include a high-resolution fetal ultrasound and fetal echocardiogram (a focused ultrasound that provides a detailed view of the fetal heart, performed by our fetal cardiology experts) to identify the direction, velocity and patterns of blood flow in specific blood vessels. This detail can help our experts distinguish between TTTS and sIUGR and confirm your diagnosis.
Your test results and treatment options will be discussed in detail on the day of your evaluation. If fetal intervention is recommended, you can also expect to meet with an advanced practice nurse to complete preoperative testing, and a social worker to arrange your temporary accommodations. Our team is here to help and support you and your family throughout this experience.
“When we came to you, we had been told that our little girl had no chance of survival. We wanted to thank you for giving us a bit of faith that our little girl could make it through. Sydney was born on May 8, one of the many lives I’m convinced you have saved. Words cannot express how much we owe our happiness to you!” — Jamie, about her sIUGR pregnancy
Types of sIUGR
sIUGR has been classified into three types based on specific blood flow patterns in the umbilical artery of the growth-restricted twin.
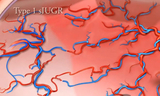
Type 1
- Consistent forward flow in the umbilical artery of the growth-restricted twin
- Average age at delivery is 34-35 weeks gestation
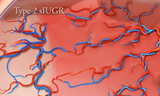
Type 2
- Either persistent absent blood flow or persistent reversal of blood flow in the umbilical artery of the growth-restricted twin
- Average age at delivery is 26-28 weeks gestation
Type 3
- Unpredictable pattern of intermittent blood flow in the umbilical artery of the growth-restricted twin (forward, absent and reversed)
- Average age at delivery is 30 weeks gestation
- In up to 15 percent of cases, the growth-restricted twin may not survive, which can also impact the neurodevelopment of the normally growing twin
Treatment for selective intrauterine growth restriction
Management of sIUGR may include continued observation with ultrasound surveillance or fetal therapy. Your recommended treatment will depend upon the type of sIUGR your twins are diagnosed with.
Type 1 sIUGR
You will undergo continued weekly observation with your local maternal-fetal medicine specialist. Weekly or twice weekly ultrasounds closely monitor the blood flows of both twins and watch for progression to Type 2 or Type 3 sIUGR which may indicate prompt referral for fetal therapy. Interval growth scans are also performed locally.
Because preterm deliveries are common in pregnancies affected by sIUGR, consultation with neonatology and a specialized delivery center can help you plan for this possibility.
Type 2 and Type 3 sIUGR
Along with at least weekly observation by your maternal-fetal medicine specialist, we may offer fetal therapy in the form of selective cord occlusion.
Selective cord occlusion is a minimally invasive surgical procedure that seeks to improve the outcome for the normally growing twin by stopping the blood flow to the growth-restricted twin in a way that minimizes the impact on the neurodevelopment and survival of the normally growing twin. Selective cord occlusion can be performed using bipolar cord coagulation (BCC) or radiofrequency ablation (RFA) procedures.
Volumes & outcomes
Our team at the Wood Center for Fetal Diagnosis and Treatment cares for a high volume of monochorionic twin pregnancies each year. Since 1995, more than 4,745 complicated multiple gestation pregnancies have been referred to our Center.
This experience helps to continuously expand our understanding of these complex pregnancies and our ability to differentiate between conditions such as sIUGR/sFGR, TTTS, twin anemia polycythemia sequence (TAPS), and twin reversed arterial perfusion (TRAP) sequence.

Tour our Fetal Center
The Wood Center for Fetal Diagnosis and Treatment has cared for many families and will help you through your journey, too.

What to expect
From the moment of referral through delivery and postnatal care, your family can expect a supportive experience when you come to us with a diagnosis of a birth defect.
Resources to help
Selective Intrauterine Growth Restriction (sIUGR) Resources
Richard D. Wood Jr. Center for Fetal Diagnosis and Treatment Resources
Learning your baby has a birth defect is a life-changing experience. We want you to know that you are not alone. To help you find answers to your questions, we've created this list of educational health resources.