
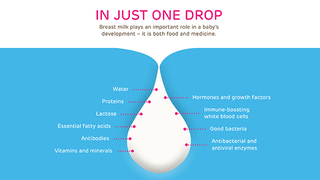
For a newborn baby, breastmilk serves as both food and medicine. In addition to providing vital nutrients, human milk plays an important role in a baby’s development. Breast milk helps protect newborns from infection and other diseases by delivering immune-boosting antibodies, white blood cells and immune factors. Some of these immune-boosting effects continue even after a baby has been weaned. Breastfeeding also plays an important role in the development of a baby’s brain and IQ. The skin-to-skin contact that occurs during breastfeeding promotes a baby’s sensory and emotional development. Breastfeeding also benefits a nursing mother, reducing her risk of high blood pressure, type 2 diabetes and some types of cancer.
The World Health Organization (WHO), the United Nations Children’s Fund (UNICEF), the National Academy of Medicine and the American Academy of Pediatrics (AAP) all recommend exclusive breastfeeding for at least the first 6 months of a baby’s life and continued breastfeeding, up to 1 year or longer, in combination with solid food.
The Breastfeeding and Lactation Program
For medically fragile neonates, however, these recommendations can be difficult to follow. The Breastfeeding and Lactation Program at Children’s Hospital of Philadelphia (CHOP), led by nurse scientist Diane Spatz, PhD, RN-BC, FAAN, is world-renowned for its work with medically-fragile neonates and medically complex infants. The Spatz 10-Step and Breastfeeding Resource Nurse Model has been used for more than 10 years at CHOP and implemented in other neonatal intensive care units across the U.S. and around the world. Soon, an adapted version will be piloted in Botswana.
Only 40% of healthy Batswana newborns are breastfed within an hour of birth, and only 20% continue to be exclusively breastfed for six months. These percentages are even lower for medically fragile neonates, for whom human milk can be a lifesaving medical intervention. The pilot project, led by Tonya Arscott-Mills, MD, MPH; Thabiso Mogotsi, MBBS, MMed; Elizabeth Lowenthal, MD, MSCE; and Diane Spatz, will implement an adapted version of the 10-Step Model in the neonatal unit (NNU) at Princess Marina Hospital, Botswana’s primary teaching hospital.
Although mothers in the Princess Marina NNU are encouraged to breastfeed, there is a lack of support around the importance of early milk expression. When a mother misses this critical window of opportunity to establish an adequate milk supply, she is often unable to meet her baby’s feeding needs by the time the infant is 2 weeks old. This project will focus on early milk expression through the use of hospital-grade, computer chip technology pumps — the same kind used in the Breastfeeding and Lactation Program at CHOP — to ensure mothers maintain an adequate milk supply. The project also aims to begin oral care with human milk, as well as education around the remaining steps of the 10-Step Model.
Rolling out the pilot
Dr. Arscott-Mills and Dr. Mogotsi have conducted interviews about the Spatz 10-Step Model with various stakeholders, including Princess Marina Hospital leaders, NNU nurses and clinicians, supply chain staff and mothers/caregivers of infants in the NNU. Feedback from these interviews is informing the rollout of the model with 20 mother-baby pairs to assess the adapted model’s effectiveness. In Feb. 2020, Dr. Spatz trained Princess Marina pediatricians and nursing staff to equip everyone with the skills needed for the program’s launch.
Drs. Arscott-Mills and Mogotsi plan to use the results of the pilot to advocate for sustained breastfeeding support with hospital leadership and the Botswana Ministry of Health and Wellness. Their goal is to ensure that all babies — including medically fragile infants — are given the healthiest start to life.
Featured in this article
Specialties & Programs
For a newborn baby, breastmilk serves as both food and medicine. In addition to providing vital nutrients, human milk plays an important role in a baby’s development. Breast milk helps protect newborns from infection and other diseases by delivering immune-boosting antibodies, white blood cells and immune factors. Some of these immune-boosting effects continue even after a baby has been weaned. Breastfeeding also plays an important role in the development of a baby’s brain and IQ. The skin-to-skin contact that occurs during breastfeeding promotes a baby’s sensory and emotional development. Breastfeeding also benefits a nursing mother, reducing her risk of high blood pressure, type 2 diabetes and some types of cancer.
The World Health Organization (WHO), the United Nations Children’s Fund (UNICEF), the National Academy of Medicine and the American Academy of Pediatrics (AAP) all recommend exclusive breastfeeding for at least the first 6 months of a baby’s life and continued breastfeeding, up to 1 year or longer, in combination with solid food.
The Breastfeeding and Lactation Program
For medically fragile neonates, however, these recommendations can be difficult to follow. The Breastfeeding and Lactation Program at Children’s Hospital of Philadelphia (CHOP), led by nurse scientist Diane Spatz, PhD, RN-BC, FAAN, is world-renowned for its work with medically-fragile neonates and medically complex infants. The Spatz 10-Step and Breastfeeding Resource Nurse Model has been used for more than 10 years at CHOP and implemented in other neonatal intensive care units across the U.S. and around the world. Soon, an adapted version will be piloted in Botswana.

Only 40% of healthy Batswana newborns are breastfed within an hour of birth, and only 20% continue to be exclusively breastfed for six months. These percentages are even lower for medically fragile neonates, for whom human milk can be a lifesaving medical intervention. The pilot project, led by Tonya Arscott-Mills, MD, MPH; Thabiso Mogotsi, MBBS, MMed; Elizabeth Lowenthal, MD, MSCE; and Diane Spatz, will implement an adapted version of the 10-Step Model in the neonatal unit (NNU) at Princess Marina Hospital, Botswana’s primary teaching hospital.
Although mothers in the Princess Marina NNU are encouraged to breastfeed, there is a lack of support around the importance of early milk expression. When a mother misses this critical window of opportunity to establish an adequate milk supply, she is often unable to meet her baby’s feeding needs by the time the infant is 2 weeks old. This project will focus on early milk expression through the use of hospital-grade, computer chip technology pumps — the same kind used in the Breastfeeding and Lactation Program at CHOP — to ensure mothers maintain an adequate milk supply. The project also aims to begin oral care with human milk, as well as education around the remaining steps of the 10-Step Model.
Rolling out the pilot
Dr. Arscott-Mills and Dr. Mogotsi have conducted interviews about the Spatz 10-Step Model with various stakeholders, including Princess Marina Hospital leaders, NNU nurses and clinicians, supply chain staff and mothers/caregivers of infants in the NNU. Feedback from these interviews is informing the rollout of the model with 20 mother-baby pairs to assess the adapted model’s effectiveness. In Feb. 2020, Dr. Spatz trained Princess Marina pediatricians and nursing staff to equip everyone with the skills needed for the program’s launch.
Drs. Arscott-Mills and Mogotsi plan to use the results of the pilot to advocate for sustained breastfeeding support with hospital leadership and the Botswana Ministry of Health and Wellness. Their goal is to ensure that all babies — including medically fragile infants — are given the healthiest start to life.
Contact us
Global Health Center