M was 7 years old when his mother brought him to see me after 6 months of recurrent “black out” episodes. During these episodes, he had a behavioral arrest, eye rolling, staring, and blinking. The episodes occurred multiple times per day, and he did not react to mom when she called his name or shook him. During this time, M also had behavioral problems. He had recently returned to live with his mother after some time living with his father, with whom he had negative experiences.
In my initial encounter with M, I considered a common saying among neurologists: “All staring is not necessarily seizure.” M had been under stress at home recently. Perhaps his staring spells were behavioral events. Alternatively, he might be showing signs of inattention due to ADHD. Perhaps an ocular tic could explain his blinking and eye rolling. In such cases, it is often helpful to ask the family if staring spells interrupt choice activities like playing or if the child snaps out of the spells with adequate stimulation (vigorous touch, loudly calling the child). If the answer to the first question is yes and the answer to the second question is no, then the staring spells may be seizures.
To further evaluate M, I obtained an EEG that showed typical findings of childhood absence epilepsy (CAE): 3 hertz spike-wave discharges and an absence seizure brought on by hyperventilation. However, he also had another staring spell during the EEG that did not have an EEG correlate. (See Figure 4.) M had both true absence seizures and non-epileptic staring spells!
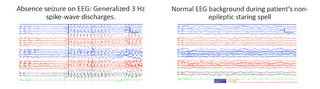
Figure 4: M’s EEG showed 3 Hertz spike-wave discharges and an absence seizure brought on by hyperventilation, typical of childhood absence epilepsy (left). However, another staring spell did not show up on the EEG.
M’s diagnosis of CAE is not an uncommon one. CAE represents 10% to 17% of all cases of childhood epilepsy. Patients with CAE often present during the school-age years. Absence seizures are the defining seizure type. Typical absence seizures are generalized seizures, characterized by behavioral arrest and unresponsiveness, lasting several seconds. Children may also have eye rolling, eyelid fluttering, and automatisms during their absence seizures. Given that absence seizures may occur hundreds of times per day, it is not surprising that these children often present with a decline in school performance as attention to school work may be interrupted many times per hour. Fortunately, the absence seizures are often easily treatable with medications—usually ethosuximide, valproic acid, or lamotrigine—and most (56% to 84%) children outgrow their epilepsy.
In M’s case, absence seizures were controlled with ethosuximide, and he ultimately outgrew his epilepsy by age 10. However, during this time, he continued to struggle with behavioral problems, feelings of sadness, and non-epileptic staring spells. Psychogenic non-epileptic events (PNEE) are often comorbid with epilepsy, as they were in M’s case.
More common than PNEE, comorbid psychological and cognitive problems are prevalent among children with CAE, with significantly higher rates than age-matched peers. These problems can persist into adulthood and may pose an even greater challenge than the absence seizures themselves. Psychiatric diagnoses, including anxiety and ADHD, occur in about two-thirds of patients with CAE. Furthermore, when compared to peers with non-neurologic chronic illness, patients with CAE are at greater risk for behavioral problems, special education needs, lower high school graduation rates, underemployment, and poor relationships with siblings and friends. These academic, personal, and behavioral issues can persist even after epilepsy has remitted.
As is often the case in pediatrics, screening is critical when it comes to childhood absence epilepsy. Pediatricians must consider the diagnosis, as well as the differential, when meeting children with staring spells. Once CAE is diagnosed and treated, a high level of suspicion must be maintained to help these children navigate the comorbid attention, behavioral, and mood problems that often accompany this diagnosis.
References and suggested readings
Wirrell EC, Camfield CS, Camfield PR, et al. Long-term psychosocial outcome in typical absence epilepsy. Sometimes a wolf in sheep's clothing. Arch Pediatr Adolesc Med. 1997;151(2):152-158.
Kessler SK, McGinnis E. A practical guide to treatment of childhood absence epilepsy. [Published online ahead of print February 2019.] Pediatr Drugs.
Caplan R, Siddarth P, Stahl L, et al. Childhood absence epilepsy: behavioral, cognitive, and linguistic comorbidities. Epilepsia. 2008;49(11):1838-1846.
Glauser TA, Cnaan A, Shinnar S, et al. Ethosuximide, valproic acid, and lamotrigine in childhood absence epilepsy. N Engl J Med. 2010;362(9):790- 799.
Holmes GL, McKeever M, Adamson M. Absence seizures in children: Clinical and electroencephalographic seizures. Ann Neurol. 1987;21:268-273.
Wyllie E. Wyllie’s Treatment of Epilepsy, 6th ed. Philadelphia, PA: Wolters Kluwer; 2015.
Featured in this article
Specialties & Programs
M was 7 years old when his mother brought him to see me after 6 months of recurrent “black out” episodes. During these episodes, he had a behavioral arrest, eye rolling, staring, and blinking. The episodes occurred multiple times per day, and he did not react to mom when she called his name or shook him. During this time, M also had behavioral problems. He had recently returned to live with his mother after some time living with his father, with whom he had negative experiences.
In my initial encounter with M, I considered a common saying among neurologists: “All staring is not necessarily seizure.” M had been under stress at home recently. Perhaps his staring spells were behavioral events. Alternatively, he might be showing signs of inattention due to ADHD. Perhaps an ocular tic could explain his blinking and eye rolling. In such cases, it is often helpful to ask the family if staring spells interrupt choice activities like playing or if the child snaps out of the spells with adequate stimulation (vigorous touch, loudly calling the child). If the answer to the first question is yes and the answer to the second question is no, then the staring spells may be seizures.
To further evaluate M, I obtained an EEG that showed typical findings of childhood absence epilepsy (CAE): 3 hertz spike-wave discharges and an absence seizure brought on by hyperventilation. However, he also had another staring spell during the EEG that did not have an EEG correlate. (See Figure 4.) M had both true absence seizures and non-epileptic staring spells!

Figure 4: M’s EEG showed 3 Hertz spike-wave discharges and an absence seizure brought on by hyperventilation, typical of childhood absence epilepsy (left). However, another staring spell did not show up on the EEG.
M’s diagnosis of CAE is not an uncommon one. CAE represents 10% to 17% of all cases of childhood epilepsy. Patients with CAE often present during the school-age years. Absence seizures are the defining seizure type. Typical absence seizures are generalized seizures, characterized by behavioral arrest and unresponsiveness, lasting several seconds. Children may also have eye rolling, eyelid fluttering, and automatisms during their absence seizures. Given that absence seizures may occur hundreds of times per day, it is not surprising that these children often present with a decline in school performance as attention to school work may be interrupted many times per hour. Fortunately, the absence seizures are often easily treatable with medications—usually ethosuximide, valproic acid, or lamotrigine—and most (56% to 84%) children outgrow their epilepsy.
In M’s case, absence seizures were controlled with ethosuximide, and he ultimately outgrew his epilepsy by age 10. However, during this time, he continued to struggle with behavioral problems, feelings of sadness, and non-epileptic staring spells. Psychogenic non-epileptic events (PNEE) are often comorbid with epilepsy, as they were in M’s case.
More common than PNEE, comorbid psychological and cognitive problems are prevalent among children with CAE, with significantly higher rates than age-matched peers. These problems can persist into adulthood and may pose an even greater challenge than the absence seizures themselves. Psychiatric diagnoses, including anxiety and ADHD, occur in about two-thirds of patients with CAE. Furthermore, when compared to peers with non-neurologic chronic illness, patients with CAE are at greater risk for behavioral problems, special education needs, lower high school graduation rates, underemployment, and poor relationships with siblings and friends. These academic, personal, and behavioral issues can persist even after epilepsy has remitted.
As is often the case in pediatrics, screening is critical when it comes to childhood absence epilepsy. Pediatricians must consider the diagnosis, as well as the differential, when meeting children with staring spells. Once CAE is diagnosed and treated, a high level of suspicion must be maintained to help these children navigate the comorbid attention, behavioral, and mood problems that often accompany this diagnosis.
References and suggested readings
Wirrell EC, Camfield CS, Camfield PR, et al. Long-term psychosocial outcome in typical absence epilepsy. Sometimes a wolf in sheep's clothing. Arch Pediatr Adolesc Med. 1997;151(2):152-158.
Kessler SK, McGinnis E. A practical guide to treatment of childhood absence epilepsy. [Published online ahead of print February 2019.] Pediatr Drugs.
Caplan R, Siddarth P, Stahl L, et al. Childhood absence epilepsy: behavioral, cognitive, and linguistic comorbidities. Epilepsia. 2008;49(11):1838-1846.
Glauser TA, Cnaan A, Shinnar S, et al. Ethosuximide, valproic acid, and lamotrigine in childhood absence epilepsy. N Engl J Med. 2010;362(9):790- 799.
Holmes GL, McKeever M, Adamson M. Absence seizures in children: Clinical and electroencephalographic seizures. Ann Neurol. 1987;21:268-273.
Wyllie E. Wyllie’s Treatment of Epilepsy, 6th ed. Philadelphia, PA: Wolters Kluwer; 2015.
Contact us
Division of Neurology