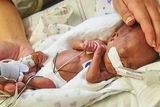
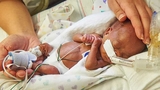
Learning to perform retinal examinations on extremely low birth weight babies is essential to pediatric ophthalmology. It is also one of the most daunting, unique, and meaningful experiences of our training. As fellows, the neonatal intensive care unit (NICU) allows us to develop this skill without disturbing the healing process of our most delicate patients. Thankfully, we rely on multidisciplinary support for guidance along the way.
Annually, 16,000 United States infants are affected by a disease of abnormal retinal blood vessel growth called retinopathy of prematurity (ROP). The youngest (≤ 30 weeks gestational age), smallest (≤ 1500 grams birth weight), and most clinically unstable patients are also the most at risk. Of those who develop ROP, 90% will spontaneously regress with time, but 1500 will require treatment and 500 are rendered legally blind each year. The goal of ROP screening is to identify and treat the 10% who do not regress before developing devastating ocular sequelae, such as retinal detachment.
ROP screening examinations, however, are not benign. Despite the use of anesthetic eye drops, the pressure of an eyelid speculum, bright light from the ophthalmoscope, and repositioning of the eye with a cotton swab, can produce extreme distress in our tiny patients. The examination can also be impeded by the need to circumvent visually obstructive tubes, masks, and positioning restrictions. Unstable babies are prone to episodes of apnea, bradycardia, and desaturations during the exam, requiring us to take breaks that frustrate our attempts to reduce exam times in order to minimize morbidity. On rare occasions, we are even forced to abort or reschedule the examination of a critically unstable child so a different treatment team can take priority of care—a humbling reminder of our shared mission not only to save eyes, but to save lives.
The critical nature of this process typically requires every exam conducted by a fellow to be repeated by the supervising attending, which can add risk. This means our primary task is to vigilantly identify which babies would benefit from a combined fellow-attending exam, and we do so in partnership with the parents and by working with our Neonatology colleagues during the initial assessment. Evaluating unstable infants is a multidisciplinary effort: a music therapist plays calming acoustic guitar to soothe the baby; a child life specialist swaddles and directly comforts the baby with touch; nurses perform acrobatics to stabilize and safely reposition intubation tubes; and technicians sterilize our equipment between examinations for infection control. The coordination, execution, and training of ROP screening at CHOP is made possible by a diverse and dedicated team that prioritizes above all the health and safety of our patients.
Fellowship training happens quickly, and at times under stressful conditions. Having to slow down evaluations and treatment feels unnatural at first, but it also creates an opportunity to appreciate the hard work, patience, and selflessness of the patients, families, care teams, and physicians who make our training possible.
References and suggested readings
Quinn GE, Barr C, Bremer D, et al. Changes in course of retinopathy of prematurity from 1986 to 2013: comparison of three studies in the United States. Ophthalmology. 2016;123(7):1595-1600.
Lad EM, Hernandez-Boussard T, Morton JM, Moshfeghi DM. Incidence of retinopathy of prematurity in the United States: 1997 through 2005. Am J Ophthalmol. 2009 Sep;148(3):451-8.
Fierson WM, American Academy of Pediatrics Section on Ophthalmology, American Academy of Ophthalmology, American Association for Pediatric Ophthalmology and Strabismus, American Association of Certified Orthoptists. Screening examination of premature infants for retinopathy of prematurity. Pediatrics. 2018;142(6).
Contributed by: Marcela Estrada, MD, and Stephanie Kletke, MD
Featured in this article
Specialties & Programs

Learning to perform retinal examinations on extremely low birth weight babies is essential to pediatric ophthalmology. It is also one of the most daunting, unique, and meaningful experiences of our training. As fellows, the neonatal intensive care unit (NICU) allows us to develop this skill without disturbing the healing process of our most delicate patients. Thankfully, we rely on multidisciplinary support for guidance along the way.
Annually, 16,000 United States infants are affected by a disease of abnormal retinal blood vessel growth called retinopathy of prematurity (ROP). The youngest (≤ 30 weeks gestational age), smallest (≤ 1500 grams birth weight), and most clinically unstable patients are also the most at risk. Of those who develop ROP, 90% will spontaneously regress with time, but 1500 will require treatment and 500 are rendered legally blind each year. The goal of ROP screening is to identify and treat the 10% who do not regress before developing devastating ocular sequelae, such as retinal detachment.
ROP screening examinations, however, are not benign. Despite the use of anesthetic eye drops, the pressure of an eyelid speculum, bright light from the ophthalmoscope, and repositioning of the eye with a cotton swab, can produce extreme distress in our tiny patients. The examination can also be impeded by the need to circumvent visually obstructive tubes, masks, and positioning restrictions. Unstable babies are prone to episodes of apnea, bradycardia, and desaturations during the exam, requiring us to take breaks that frustrate our attempts to reduce exam times in order to minimize morbidity. On rare occasions, we are even forced to abort or reschedule the examination of a critically unstable child so a different treatment team can take priority of care—a humbling reminder of our shared mission not only to save eyes, but to save lives.
The critical nature of this process typically requires every exam conducted by a fellow to be repeated by the supervising attending, which can add risk. This means our primary task is to vigilantly identify which babies would benefit from a combined fellow-attending exam, and we do so in partnership with the parents and by working with our Neonatology colleagues during the initial assessment. Evaluating unstable infants is a multidisciplinary effort: a music therapist plays calming acoustic guitar to soothe the baby; a child life specialist swaddles and directly comforts the baby with touch; nurses perform acrobatics to stabilize and safely reposition intubation tubes; and technicians sterilize our equipment between examinations for infection control. The coordination, execution, and training of ROP screening at CHOP is made possible by a diverse and dedicated team that prioritizes above all the health and safety of our patients.
Fellowship training happens quickly, and at times under stressful conditions. Having to slow down evaluations and treatment feels unnatural at first, but it also creates an opportunity to appreciate the hard work, patience, and selflessness of the patients, families, care teams, and physicians who make our training possible.
References and suggested readings
Quinn GE, Barr C, Bremer D, et al. Changes in course of retinopathy of prematurity from 1986 to 2013: comparison of three studies in the United States. Ophthalmology. 2016;123(7):1595-1600.
Lad EM, Hernandez-Boussard T, Morton JM, Moshfeghi DM. Incidence of retinopathy of prematurity in the United States: 1997 through 2005. Am J Ophthalmol. 2009 Sep;148(3):451-8.
Fierson WM, American Academy of Pediatrics Section on Ophthalmology, American Academy of Ophthalmology, American Association for Pediatric Ophthalmology and Strabismus, American Association of Certified Orthoptists. Screening examination of premature infants for retinopathy of prematurity. Pediatrics. 2018;142(6).
Contributed by: Marcela Estrada, MD, and Stephanie Kletke, MD
Contact us
Division of Ophthalmology