As part of a busy children’s hospital, the Division of Ophthalmology at CHOP consults on many challenging situations. Stevens-Johnson syndrome (SJS) is a lifethreatening cutaneous immune-mediated reaction involving blistering and desquamation of the skin and mucous membranes. When more than 30 percent body surface area is involved, the disease is called toxic epidermal necrolysis (TEN). Most often a drug is the cause, but infectious triggers and idiopathic cases also occur.
Ocular complications of SJS/TEN are vision-threatening and require quick and aggressive intervention. Acute inflammation of the entire ocular surface, from eyelid margins to conjunctiva to cornea, can cause symblepharon, corneal epithelial defects, and limbal stem cell loss, which can lead to vision loss and problems that persist long after the rest of the body has healed.
Gil Binenbaum, MD, MSCE, chief of the inpatient consultation service at CHOP, stresses a few key points:
- Act quickly. Use amniotic membranes as soon as there is any epithelial defect. Initial management is frequent topical steroids and lubricants when the eyes are red. Daily exams allow early identification of any epithelial surface breakdown, at which point cryopreserved amniotic membrane grafts (AMGs) should be placed without delay. AMGs suppress inflammation and scarring while promoting healing. After symblepharon lysis, free grafts are placed with sutures and/or fibrin glue to cover the conjunctival and corneal surfaces all the way from one lid margin to the other (see Figure A). Another option is to insert an amniotic membrane ring (Prokera) in conjunction with a symblepharon ring or large scleral shell spacer to maintain the fornices, but this approach does not protect the lid margins from long-term damage. Subconjunctival steroid injections into the fornices help to suppress inflammation. AMGs dissolve quickly in these patients (see Figure B) and may require replacement.
- Continue treatment. Ocular inflammation may persist after the skin has improved. Topical steroids and lubricants often need to be continued long after the child has recovered from the acute skin disease. Ideally, preservative-free preparations are used. Suppression of inflammation is necessary to prevent limbal stem cell loss and progressive conjunctival and corneal scarring.
- Follow patient long term. Complications can arise even years later (See Figure C). Long-term ocular complications are unfortunately a real concern for children who survive SJS/TEN. Multiple interrelated and synergistic disease processes may occur. Limbal epithelial stem cell deficiency may not become fully apparent for up to a year, when progenitor cell reserves become depleted. Even children who appear to be stable with good vision can decompensate, and parents should be counseled of this possibility. Stem cell deficiency can result in pain, photophobia, and vision loss from chronic inflammation, recurrent erosions, poorly healing ulceration, subepithelial fibrosis and scarring, and corneal neovascularization and conjunctivization. Static or progressive conjunctival scarring can lead to repeated mechanical trauma with trichiasis, keratinization, exposure, goblet cell loss, dry eye, and blepharitis. Late-onset scleritis and ocular cicatricial pemphigoid are both associated with SJS/TEN, and may require aggressive systemic immunosuppression and complicated ocular surface reconstructive procedures.
We have found it critical to maintain long-term follow-up of these children, educate parents on concerning signs such as new photophobia or pain, and have a low threshold for performing examinations under anesthesia. When necessary, we repeatedly place amniotic membrane grafts for new or repeated surface defects, work closely with corneal specialists who have expertise in ocular surface failure and inflammatory diseases such as pemphigoid, and involve pediatric rheumatologists to guide the management of systemic immunosuppression. However, aggressive, early, and continued treatment in the acute phase of SJS/TEN is the first step in preventing long-term complications from developing.
An enlightening study of the long-term ocular complications of SJS/TEN is De Rojas et al., BJO, 2007;91:1048-1053.
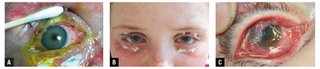
A) Amniotic membrane graft sewn in place with external bolsters. B) Patient in recovery phase. The AMGs have dissolved. The bolsters have not yet been removed. C) Child who developed ocular surface failure and ocular cicatricial pemphigoid 1 year after acute SJS/TEN event.
Featured in this article
Specialties & Programs
As part of a busy children’s hospital, the Division of Ophthalmology at CHOP consults on many challenging situations. Stevens-Johnson syndrome (SJS) is a lifethreatening cutaneous immune-mediated reaction involving blistering and desquamation of the skin and mucous membranes. When more than 30 percent body surface area is involved, the disease is called toxic epidermal necrolysis (TEN). Most often a drug is the cause, but infectious triggers and idiopathic cases also occur.
Ocular complications of SJS/TEN are vision-threatening and require quick and aggressive intervention. Acute inflammation of the entire ocular surface, from eyelid margins to conjunctiva to cornea, can cause symblepharon, corneal epithelial defects, and limbal stem cell loss, which can lead to vision loss and problems that persist long after the rest of the body has healed.
Gil Binenbaum, MD, MSCE, chief of the inpatient consultation service at CHOP, stresses a few key points:
- Act quickly. Use amniotic membranes as soon as there is any epithelial defect. Initial management is frequent topical steroids and lubricants when the eyes are red. Daily exams allow early identification of any epithelial surface breakdown, at which point cryopreserved amniotic membrane grafts (AMGs) should be placed without delay. AMGs suppress inflammation and scarring while promoting healing. After symblepharon lysis, free grafts are placed with sutures and/or fibrin glue to cover the conjunctival and corneal surfaces all the way from one lid margin to the other (see Figure A). Another option is to insert an amniotic membrane ring (Prokera) in conjunction with a symblepharon ring or large scleral shell spacer to maintain the fornices, but this approach does not protect the lid margins from long-term damage. Subconjunctival steroid injections into the fornices help to suppress inflammation. AMGs dissolve quickly in these patients (see Figure B) and may require replacement.
- Continue treatment. Ocular inflammation may persist after the skin has improved. Topical steroids and lubricants often need to be continued long after the child has recovered from the acute skin disease. Ideally, preservative-free preparations are used. Suppression of inflammation is necessary to prevent limbal stem cell loss and progressive conjunctival and corneal scarring.
- Follow patient long term. Complications can arise even years later (See Figure C). Long-term ocular complications are unfortunately a real concern for children who survive SJS/TEN. Multiple interrelated and synergistic disease processes may occur. Limbal epithelial stem cell deficiency may not become fully apparent for up to a year, when progenitor cell reserves become depleted. Even children who appear to be stable with good vision can decompensate, and parents should be counseled of this possibility. Stem cell deficiency can result in pain, photophobia, and vision loss from chronic inflammation, recurrent erosions, poorly healing ulceration, subepithelial fibrosis and scarring, and corneal neovascularization and conjunctivization. Static or progressive conjunctival scarring can lead to repeated mechanical trauma with trichiasis, keratinization, exposure, goblet cell loss, dry eye, and blepharitis. Late-onset scleritis and ocular cicatricial pemphigoid are both associated with SJS/TEN, and may require aggressive systemic immunosuppression and complicated ocular surface reconstructive procedures.
We have found it critical to maintain long-term follow-up of these children, educate parents on concerning signs such as new photophobia or pain, and have a low threshold for performing examinations under anesthesia. When necessary, we repeatedly place amniotic membrane grafts for new or repeated surface defects, work closely with corneal specialists who have expertise in ocular surface failure and inflammatory diseases such as pemphigoid, and involve pediatric rheumatologists to guide the management of systemic immunosuppression. However, aggressive, early, and continued treatment in the acute phase of SJS/TEN is the first step in preventing long-term complications from developing.
An enlightening study of the long-term ocular complications of SJS/TEN is De Rojas et al., BJO, 2007;91:1048-1053.

A) Amniotic membrane graft sewn in place with external bolsters. B) Patient in recovery phase. The AMGs have dissolved. The bolsters have not yet been removed. C) Child who developed ocular surface failure and ocular cicatricial pemphigoid 1 year after acute SJS/TEN event.
Contact us
Division of Ophthalmology