Resuscitation Education and Simulation
Directing the resuscitation of a child is more than just being able to intubate or start an IV. Our curriculum provides residents with the opportunity to participate in resuscitations in a variety of settings including the CHOP and HUP NICUs, the PICU, and the ED. There is always support for the residents’ role provided by more senior physicians including senior residents, fellows and attending physicians. In addition, through participation in simulated resuscitations in a variety of settings, residents have the opportunity to learn to lead in critical situations. PALS and NRP training are provided during Intern Orientation and residents are recertified in these courses during their third year of training.
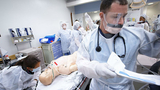
The Residency Program and many clinical teams partner with the Center for Simulation, Advanced Education and Innovation at CHOP to provide a comprehensive curriculum related to critical situations. In keeping with the Center’s philosophy, the vast majority of this education is done in situ where teams are actively engaged in providing care to patients. The Pediatric Chief residents coordinate a curriculum of floor based simulated resuscitations also known as mock codes. These are conducted with pediatric resident teams while on PL1 and PL2 inpatient rotations; common inpatient critical scenarios are presented.
Resident participation is tracked and each resident participates in a variety of different resuscitation scenarios. Senior residents lead care provided by interdisciplinary teams including other residents, nurses, respiratory therapists and other ancillary staff. Feedback related to medical care, team dynamics, and communication is provided by the chief residents, faculty, and facilitators from the Simulation Center.
In the Emergency Department, Friday mornings are devoted to education. As part of that series, a mock resuscitation is presented. Senior residents lead interdisciplinary teams in scenarios presented by faculty and fellows from the Division of Emergency Medicine and facilitators from the Simulation Center. Simulation based scenarios are also presented by the Division of Neonatology in the CHOP and HUP NICUs as well as by the Division of Critical Care Medicine of the Department of Anesthesiology and Critical Care in the PICU on a regular basis. The Emergency Department resuscitation day presented near the end of the PL1 year also allows residents to practice resuscitation skills during several simulated scenarios.
This preparation allows residents to actively participate, under the direction of fellows and attending physicians, in resuscitations in all critical care settings (HUP delivery room, HUP and CHOP NICU, PICU and ED). In addition, residents are active members of the Hospital-wide Code Blue Team. Residents play important roles in these settings and gain experience that can be used regardless of the path their future career.