What is amplified musculoskeletal pain syndrome (AMPS)?
Amplified musculoskeletal pain syndrome (AMPS) is a very painful medical condition that can cause pain anywhere in the body. These episodes of pain can be intermittent or constant, can affect the whole body or be localized to one area of the body or affect just a limb. Whenever it occurs, the degree of pain children with AMPS experience is more intense than one would normally expect.
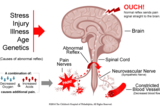
To understand what amplified pain is, first look at the illustration to see how pain is normally felt. Normally, pain is triggered in response to tissue damage such as would occur when a child steps on a tack. When that happens, the following events occur:
- The damage sends a signal through the pain nerve to the spinal cord.
- The signal is transferred up to the brain.
- The brain recognizes the signal as being painful.
In AMPS, there is an abnormal short circuit in the spinal cord. The normal pain signal not only travels up to the brain, but also goes to the neurovascular nerves (also known as autonomic or “flight or fight” nerves) that control blood flow through the blood vessels.
These nerves cause the blood vessels to become smaller (constrict). This constriction restricts blood flow and oxygen to muscles and bone and leads to an increase in waste products such as lactic acid. It is this lack of oxygen and acid build-up that causes pain.
This new pain signal also goes across the abnormal short circuit in the spinal cord and causes a further decrease in blood flow leading to more pain. The pain then becomes greatly “amplified” through this continuous cycle.
Forms of amplified pain
- Diffuse amplified pain – also called total body pain or pediatric fibromyalgia
- Intermittent amplified pain
- Complex regional pain syndrome (CRPS) with autonomic changes
- Localized amplified pain without autonomic changes (autonomic changes include color and temperature changes - for example, cold and blue - as well as swelling and sweating.)
Causes of amplified musculoskeletal pain syndrome (AMPS)
There are three major causes for amplified pain: injury, illness and psychological stress. There may be other factors such as age, genetics or hormones that can also affect amplified pain. It is often a combination of these factors that lead to amplified pain.
Injuries
These children have suffered a significant specific injury such as a broken bone, moderate to severe musculoskeletal injury or have developed pain after surgery. The symptoms of AMPS can occur suddenly or take weeks to develop.
Illnesses
Illness is an infrequent cause of AMPS, but can be more commonly seen in conjunction with inflammatory conditions such as arthritis, tendonitis, myositis or enthesitis. Other illnesses that may be the initial cause are infections such as mononucleosis, gastroenteritis or influenza.
Psychological stress
Stress can be both a complicating factor and trigger for amplified pain. Stressors can be positive or negative, big or small, and can include not just events, but feelings and personality styles.
Many children with AMPS and their families have been negatively affected by peers, school officials and even health care professional who have dismissed the child’s symptoms.
Chronic pain can also significantly affect individual and family dynamics. Exploring individual and family dynamics does not imply that the pain is not real or is entirely due to psychological cause.
Children with AMPS and their families can benefit from various forms of psychotherapy such as cognitive-behavior therapy (CBT) which can help the child with more immediate coping strategies to deal with the pain and dysfunction as well as identify stressors, such as school, family, and friendship, and to practice expression of feelings and emotions.
Testing and diagnosis of amplified musculoskeletal pain syndrome (AMPS)
Amplified pain is diagnosed by listening carefully to the child’s history, both physical and emotional.
Some children have autonomic changes at the time of examination or can be extremely sensitive to touch.
Blood tests are generally normal unless there are other conditions present.
In some children, a bone scan or MRI can show abnormalities that are very suggestive of AMPS, but the results may be normal.
Early diagnosis may be difficult for several reasons:
- Not all AMPS symptoms may be present at first but may evolve over time.
- Urgent problems such as infections or musculoskeletal injuries may need to be ruled out before starting a treatment plan for AMPS.
- There is a wide spectrum of AMPS, so unless a clinician has seen a variety of children with AMPS they may not recognize it.
Treatment for amplified musculoskeletal pain syndrome (AMPS)
FAQs about AMPS
Get answers to frequently asked questions about amplified musculoskeletal pain syndrome.
AMPS is an often elusive and misunderstood condition. Get answers to frequently asked questions about the syndrome and learn about treatment options at CHOP. Learn more
Treatment for children diagnosed with AMPS focuses on a return to wellness and includes aerobic exercise to increase cardiovascular tone, desensitization therapies, individualized outpatient therapy for coping strategies and stress management, and as well as eliminating medications for the treatment of amplified pain. It is important to address all of these in order to break the pain cycle and retrain the affected nerves.
The goal is to return the child to functional activities such as school, sports, socializing with friends, and returning to normal lifestyle activities. It is important to remember that function returns before pain entirely resolves. Once children with AMPS understand that using their bodies in a normal way is not damaging they are often able to work through their pain, restore function, and resolve their pain on their own using an outpatient treatment plan.
Psychological therapy focuses on the connection between the mind and body. Those children who are unable to work through their AMPS pain and restore function over time with an outpatient treatment plan may require a therapeutic hospital treatment program for AMPS.
Outlook
Patients who have completed treatment in our Center, both in outpatient treatment and hospital-based treatment, have exhibited a positive change in their functional ability as measured by the Functional Disability Inventory (FDI), returning to full function and normal functional activities such as school, friendships, and sports.
In our published results of 103 children with complex regional pain syndrome, type 1, 100 percent became fully functional, 92 percent became completely symptom-free, and the long-term significant relapse rate was only 15 percent. At 5 years, 88 percent were still doing well.
Resources to help
Amplified Musculoskeletal Pain Syndrome (AMPS) Resources
Center for Amplified Musculoskeletal Pain Syndrome Resources
We have created resources to help you find answers to your questions about amplified musculoskeletal pain syndrome and feel confident with the care you are providing your child.


