What is craniofacial fibrous dysplasia?
Craniofacial fibrous dysplasia is a bone disease of the face and skull that replaces normal bone with fibrous-type tissue. This tissue is not as hard as normal bone, and because it is soft and stringy, it makes the bone more fragile and prone to break.
Craniofacial fibrous dysplasia is related to fibrous dysplasia, which can affect any bone in the body but most commonly affects the long bones in the legs and arms. The condition, sometimes called facial fibrous dysplasia or fibrous dysplasia of the skull, may affect one bone or multiple bones. Involvement of the skull and face can be present in 30% of all patients with fibrous dysplasia.
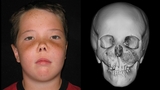
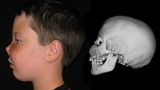
Patient with fibrous dysplasia involving the orbits, jaw and cranial base. Note the spongy-like appearance in the CT images as well as the overgrowth of the middle of the face and nasal distortion.
Craniofacial fibrous dysplasia may cause shifting of facial features and facial asymmetry, such as incorrect placement of the eyes, misalignment of the jaw, and other problems.
There are two forms of fibrous dysplasia:
- Monostotic, which affects one bone and is active while the child is growing but often becomes inactive after puberty
- Polyostotic, which affects multiple bones and may remain active throughout a person’s life
Fibrous dysplasia may appear in childhood, usually between the ages of 3 and 15. Boys are more often diagnosed with fibrous dysplasia than girls, except one specific type of polyostotic fibrous dysplasia — McCune-Albright syndrome — which is more common in girls and affects the bones and skin and is associated with hormonal imbalance and often precocious (premature) puberty.
Causes
While the exact cause of fibrous dysplasia is unknown, recent studies point to a mutation of Gs alpha protein during prenatal development as a contributing factor. Fibrous dysplasia is not hereditary, meaning parents do not pass the condition to their children.
Signs and symptoms
Signs and symptoms of fibrous dysplasia affecting the skull may include:
- Facial asymmetry
- Shifting facial structure that can affect any bone in the face
- Nasal airway obstruction
- Jaw and bite misalignment, in some cases making it difficult to chew and swallow
- Visual and hearing problems due to compression of the optic nerve or acoustic nerve
Additionally, children with craniofacial fibrous dysplasia may experience symptoms related to bone weakness in other parts of the body, including bone fractures or deformities, bone pain, or bone lesions which may stop growing when the child reaches puberty.
Children with polyostotic fibrous dysplasia may also experience:
- Endocrine gland problems, such as early puberty, thyroid disorders and related issues
- Unusual skin patches, called café-au-lait pigmentation, ranging from light brown to dark brown in color
Testing and diagnosis
At The Children’s Hospital of Philadelphia (CHOP), your child's diagnostic evaluation begins with a thorough medical history and physical examination.
Clinical experts use a variety of diagnostic tests to diagnose facial fibrous dysplasia, including:
- X-rays, which produce images of bones.
- Computed tomography (CT) scan, which uses a combination of X-rays and computer technology to produce cross-sectional images ("slices") of the body. These may be used to construct a 3D image used for intervention planning.
Depending on your child’s condition and symptoms, CHOP clinicians may recommend additional testing including blood work and hormone testing.
Treatment
At CHOP, experts in the Craniofacial Program take a team approach to treatment of fibrous dysplasia of the skull. Specialists from plasticsurgery, neurosurgery, ophthalmology, orthodontics and oral surgery collaborate to provide your child with individualized care and the best possible outcomes.

Patient with fibrous dysplasia involving the forehead and left upper orbit (left). Long term results (right) after surgery and showing stable, non-progressive, craniofacial fibrous dysplasia. Surgery involved a combination of reducing the excess tumor and placement of bone grafts. Note absence of visible facial scars.
Non-Surgical Treatment
Non-surgical treatment can be used to manage pain associated with fibrous dysplasia. Although many drugs have been utilized in treatment of fibrous dysplasia, none at present are known to slow growth of the disease. Clinical trials are underway for some promising new drugs.
Surgical treatment
Surgical treatment includes resection and reconstruction of the deformed bone if it is in a small area, but more common is reduction/ contouring of the bony excess when it becomes symptomatic or visible.
When Fibrous Dysplasia involves the bone around the eye, careful observation with serial eye exam and CT scans may be required to prevent injury to the nerve from tumor growth. Depending on the location, surgery will be tailored to your child’s functional and appearance needs. As children grow serial surgery may be required as the disease process ceases growing, usually in late adolescence or early adulthood.
While several surgical options are available to treat facial fibrous dysplasia, your child’s treatment will depend on the location of the bones affected and the severity of the condition.
- Surgery is usually done through limited incision approaches and hidden incisions in the hair. This can help reduce visible scarring.
- If the affected areas of the face are small and easily accessible, treatment usually involves complete surgical removal (resection) of the area and reconstruction using a combination of bone grafts and materials such as titanium plates and screws.
- If the area affected is too large or too important to be removed, the size of the bone may be reduced to normal using a high speed burr.
- In some patients, a combination of bone reduction with a burr and bone grafting may be utilized.
- If the facial fibrous dysplasia is in an area where it is growing and compressing nerves, removing some of the surrounding bone can decompress the nerve.
- In severe cases where the jaw is displaced and malocclusion occurs, a combined therapy with orthodontics will utilize osteotomies (bone cuts) to reposition abnormally placed bones.
If surgery is required on a particular facial region such as the skull base, your plastic surgeon may work together with a neurosurgeon or ophthalmologist to ensure the most effective treatment. If your child's condition involves the jaw, plastic surgeons will collaborate with orthodontics at CHOP, or local orthodontists if needed.
Your child may need additional surgeries over the course of treatment for facial fibrous dysplasia. In severe cases, the excess bone may grow back over time and require repeated treatments. However, the disease process tends to burn itself out cease-growing) usually in late adolescence or early adulthood.
After surgery for facial fibrous dysplasia, your child should expect to stay overnight in the Hospital. Depending on the complexity of the surgery required, your child may be hospitalized anywhere from one to several days.
Follow-up care
Your child will need to return for evaluation approximately one to two weeks after surgery. Regular follow-up visit will be needed and are commonly done every three months for the first year, and then yearly, based on your child's condition.
In cases where the bone has been shaped or contoured — usually to preserve vital structures and because the disease affects a large volume of bone — recurrence of the bony overgrowth may occur and secondary procedures may be necessary.
During follow-up visits, your child’s physician will perform a physical exam and may order X-rays or CT scan of the affected area until your child reaches skeletal maturity. If your child was diagnosed with polyostotic fibrous dysplasia, he may also be referred to an endocrinologist for periodic testing of any endocrine or hormone related disorder.
Outlook
Outcomes for children treated for craniofacial fibrous dysplasia at CHOP have been excellent. Because this disease is persistent, continued clinical monitoring is essential in long-term management of the condition.

Why Choose the Craniofacial Program
CHOP’s Craniofacial Program is one of the Nation’s leading treatment programs for children with both congenital and acquired anomalies of the face and skull.
Resources to help
Craniofacial Program Resources
We have gathered resources to give you information and help you find answers to your questions. We hope this makes your family's life a little easier.
Reviewed by Scott P. Bartlett, MD
Reviewed on 06/13/2025
