What are posterior urethral valves?
Posterior urethral valves (PUV) are obstructive membranes that develop in the urethra (tube that drains urine from the bladder), close to the bladder. The valve can obstruct or block the outflow of urine through the urethra. When this occurs, the bladder, ureters and kidneys become progressively dilated, which can lead to damage.
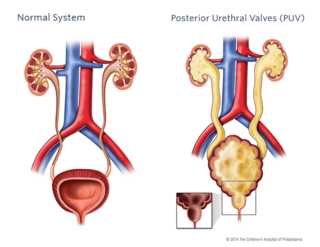
The degree that the urine is blocked will determine the severity of the urinary tract problems.
Causes of posterior urethral valves
PUV are thought to develop in the early stages of fetal development. The abnormality affects only male infants and occurs in about 1 in 8,000 births. This disorder is usually sporadic (occurs by chance). However, some cases have been seen in twins and siblings, suggesting a genetic component.
Signs and symptoms of PUV
PUV occur in varying degrees from mild to severe. Due to increased use of prenatal imaging, PUV may be identified before any symptoms are present. If any dilation (hydronephrosis) is identified, your baby will be monitored throughout the pregnancy and after birth. Once your baby is born, further imaging studies will confirm the diagnosis.
Children who are diagnosed later may have the following signs or symptoms that require treatment:
- Urinary tract infection
- Weak urine stream
- Difficulty with urination
- Urinary frequency
- New onset of urinary incontinence
Testing and diagnosis
We use voiding cystourethrogram (VCUG) to diagnose PUV. During this test, a catheter (tube) is placed through your child’s urethra into the bladder. The tube will be used to slowly fill the bladder with a solution called contrast. While the bladder is being filled, a special machine (fluoroscopy) is used to take pictures. The radiologist looks to see if any of the contrast goes back up into the kidneys. This study is used to diagnose vesicoureteral reflux (VUR). Additional pictures are taken while your child is urinating. The radiologist will look at the urethra while urine is passing to identify the blockage (PUV).
We will also look at your child’s kidneys and bladder with a renal bladder ultrasound (RBUS). This procedure uses sound waves to outline the kidneys and bladder. It will enable us to see the degree of hydronephrosis and the shape of the bladder.
We may also order blood tests to check how well the kidneys are functioning.
Treatment for posterior urethral valves
Surgical treatment
Treatment for PUV depends on the severity of the condition, your child’s age, bladder and kidney status. The surgical goal is to preserve kidney and bladder function.
- Valve ablation: Once PUV are identified, they need to be surgically incised. During valve ablation, the urologist will insert a cystoscope, a small device with a light and a camera lens at the end. He will use this instrument to make incisions in the valves so they collapse and no longer obstruct the urethra.
- Vesicostomy: In a situation where your baby is too small to undergo valve ablation or when a severe obstruction is noted, a vesicostomy may be recommended. A vesicostomy provides an opening to the bladder, so that urine drains freely from the lower abdominal opening. During surgery, a small part of the bladder wall is turned inside out and sewn to the abdomen. It looks like a small slit, surrounded by pink tissue. The vesicostomy is a temporary option and can be closed in the future.
After successful bladder drainage, either by the valve ablation or vesicostomy, we will continue to monitor your child's condition throughout his childhood and adolescence. We will need to assess the kidney function, watch for kidney growth and see how your child does through toilet training. Some children need ultrasounds every year while others may benefit from medications and additional surgeries. Our team will work with you and your family to tailor a plan based on your child's condition.
Visit the Center for Fetal Diagnosis and Treatment (CFDT) to learn more about lower urinary tract obstruction (LUTO) and watch our LUTO video on how our Urology and CFDT teams collaborate to provide accurate diagnosis before birth and expert evaluation and treatment after birth.
Long-term care
As your child nears adulthood, our dedicated Urology Transitional Care Program is here to help you and your child prepare for the transition from pediatric to adult medical care. For patients with complex urologic conditions like PUV, it is especially important that the care they receive remains effective and streamlined. Learn more about how this collaboration between CHOP and the Hospital of the University of Pennsylvania (HUP) can support you through this process.
Reviewed by: Division of Urology
Date: May 2011
Resources to help
Division of Urology Resources
Caring for a child with an illness or injury can be overwhelming. We have resources to help you find answers to your questions and feel confident in the care you are providing your child.
