What is protein-losing enteropathy (PLE)?
Protein-losing enteropathy refers to the loss of serum proteins from the digestive track. In many cases, this loss of protein is due to abnormalities in lymphatic flow.
The lymphatic system plays a crucial role in immune function and in the delivery of vital nutrients to the body. Functioning almost like a sponge, the lymphatic system absorbs excess lymph fluid — watery fluid containing protein, electrolytes, cells and other substances — from the body’s organs and returns it to the blood stream.
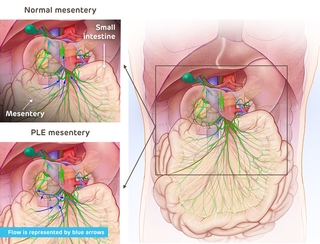
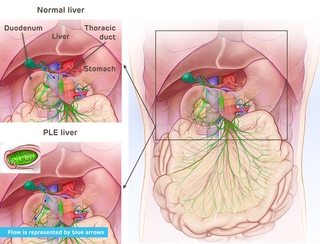
In a healthy body, the lymphatic channels from the liver and mesentery drain toward the thoracic duct, which is the main lymphatic vessel responsible for lymph drainage. In children and adults with PLE, however, channels originating in the intestine or originating in the liver and connecting to the intestine begin to flow in the opposite direction, creating leaks in the intestinal wall. The duodenum (part of the small intestine) appears to be especially susceptible to this abnormality. As lymphatic fluid spills in, there is no way for the body to absorb it. This fluid loss results in an abnormally low level of albumin (a protein made by the liver), electrolytes, coagulants and even T-cells. It can also lead to diarrhea and edema.
What causes PLE?
Experts in the Jill and Mark Fishman Center for Lymphatic Disorders at Children’s Hospital of Philadelphia (CHOP) are leaders in lymphatic research, diagnostics and treatment. This research is changing the way the scientific and medical communities think about PLE. PLE can be caused by primary and secondary disorders. Regardless of the cause, our imaging has shown that lymphatic leaks are localized and in PLE, the duodenum is often the common site of lymphatic leaks.
Etiologies of PLE
Primary PLE
Intestinal Lymphangiectasia (Disordered lymphatic flow)
- Poor mesenteric efferent lymphatic flow
- Poor hepatic efferent lymphatic flow
- Aberrant hepatoduodenal connections
- Aberrant mesenteric-duodenal connections
Lymphatic Channel Disorders (Lymphatic malformations)
- RASopathies
- Central conducting lymphatic anomaly (CCLA)
- Lymphangiomatosis/Generalized lymphatic anomaly (GLA)
- Kaposiform lymphatic anomaly (KLA)
- Gorham-Stout disease (GSD)
Secondary PLE
Mechanical Obstruction
- Elevated central venous pressure (CVP)
- Elevated intrathoracic pressure (ITP)
- Obstructing tumors or masses
- Thoracic duct (TD) occlusion
Mucosal Disruption
- Diffuse inflammatory disorders (systemic lupus erythematosus [SLE], CHAPLE syndrome)
- Localized disruption (Inflammatory bowel disease, Ménétrier syndrome, celiac disease)
What are the signs and symptoms of PLE?
Some of the symptoms associated with protein-losing enteropathy include:
- Diarrhea
- Feeding intolerance (unable to eat or digest food without getting sick)
- Edema (fluid retention or swelling, particularly in the extremities)
- Ascites (fluid retention in the abdomen)
- Problems with tissue healing
- Blood clotting disorders
- Lymphocyte (a type of white blood cell) deficiency
- Susceptibility to infection
- Hypocalcemia (low calcium)
- Hypoalbuminemia (low albumin)
How is PLE diagnosed?
The world-renowned experts in the Jill and Mark Fishman Center for Lymphatic Disorders developed a specialized imaging technique — dynamic contrast magnetic resonance lymphangiography (DCMRL) — that is used to pinpoint the exact source of lymphatic leaks.
During this procedure, an MRI contrast agent (a safe, injectable dye) is injected directly into the lymphatic system and tracked by MRI.
There are three points of access through which the contrast agent is injected:
- Intranodal (inguinal lymph nodes)
- Intrahepatic (liver)
- Intramesenteric (mesentery)
Each point of access for DCMRL provides a different view of the lymphatic system for the most comprehensive lymphatic imaging. Patients with PLE receive all three points of access, allowing our physicians to clearly see the anatomy of the lymphatic system, the direction and speed of lymphatic flow and the exact source of any leaks. This is especially important in PLE diagnosis and treatment to identify the source of protein loss and to target an intervention.
In some cases, a special blue dye injected into lymphatic channels can further aid localization of lymphatic leaks.
How is PLE treated?
In the Jill and Mark Fishman Center for Lymphatic Disorders, children and adults with PLE are treated by the world’s most experienced specialists in lymphatic imaging and intervention. The team’s recently published algorithm streamlines the plan of care for what can otherwise be a complicated and difficult-to-treat condition.
Medications such as diuretics and steroids, which can reduce the inflammation associated with PLE, are typically a first line of treatment. If symptoms persist, your doctor may recommend comprehensive lymphatic imaging and intervention — a selective or targeted embolization which seals off leaking lymphatic channels.
During a lymphatic embolization, several different types of embolization agents may be used. These agents — including tiny metal coils or a special glue — are injected through a catheter to stop the leaks and seal abnormal lymphatic vessels.
For patients with multicompartment lymphatic failure or PLE that is unresponsive to embolization, transcatheter or surgical decompression of the thoracic duct is another available treatment. This procedure reduces the thoracic duct afterload by decompressing it into a lower pressure compartment.
What is the long-term outlook for patients with PLE?
The highly advanced treatment options for PLE are cutting-edge, and there is more to learn about them. The team of experts in the Jill and Mark Fishman Center for Lymphatic Disorders is invested in further research to determine the long-term outlook for PLE patients and the role of lymphatic imaging and intervention in the treatment of this condition.
Our publications
Kylat RI, Witte MH, Barber BJ, Dori Y, Ghishan FK: Resolution of Protein-Losing Enteropathy after Congenital Heart Disease Repair by Selective Lymphatic Embolization. Pediatr Gastroenterol Hepatol Nutr 22(6): 594-600, November 2019.
Rychik J, Dodds KM, Goldberg D, Glatz AC, Fogel M, Rossano J, Chen J, Pinto E, Ravishankar C, Rand E, Rome JJ, Dori Y: Protein Losing Enteropathy After Fontan Operation: Glimpses of Clarity Through the Lifting Fog. World J Pediatr Congenit Heart Surg 11(1): 92-96, January 2020.
Brownell JN, Biko DM, Mamula P, Krishnamurthy G, Escobar F, Srinivasan A, Laje P, Piccoli DA, Pinto E, Smith CL, Dori Y: Dynamic Contrast Magnetic Resonance Lymphangiography Localizes Lymphatic Leak to the Duodenum in Protein-losing Enteropathy. Journal of Pediatric Gastroenterology and Nutrition 74(1): 38-45, January 2022.
Gartenberg AJ, Krishnamurthy G, Srinivasan A, Escobar FA, Brownell JN, Mamula P, O'Byrne ML, Dori Y, Smith CL. Intrahepatic and Periduodenal Embolization for Protein-Losing Enteropathy Patients With Congenital Heart Disease. J Am Coll Cardiol. 2023 Jun 27;81(25):2476-2478. doi: 10.1016/j.jacc.2023.04.033. PMID: 37344050.
Follow-up care
Follow-up care will be managed primarily by your child’s primary physician in coordination with the physicians from the Jill and Mark Fishman Center for Lymphatic Disorders for specific treatments like medication changes or medication weans. In patients with certain types of congenital heart disease, follow-up care will also be managed in coordination with CHOP’s Single Ventricle Survivorship Clinic, part of the Fontan Rehabilitation, Wellness, Activity and Resilience Development (FORWARD) Program.
PLE Research
Experts are collaborating on research to better understand the lymphatic system, develop new lymphatic interventional procedures, and to improve lymphatic imaging modalities.
Why choose us
Our team has the most experience in the world treating both children and adults with protein losing enteropathy. We have developed a variety of innovative imaging and interventional techniques that have advanced the minimally invasive treatment options available to patients.
Resources to help
Jill and Mark Fishman Center for Lymphatic Disorders Resources
We know that caring for a child with a health condition can be stressful. To help you find answers to your questions and feel confident in the care you're providing your child, we’ve created this list of educational health resources.
Reviewed by Yoav Dori, MD, PhD
