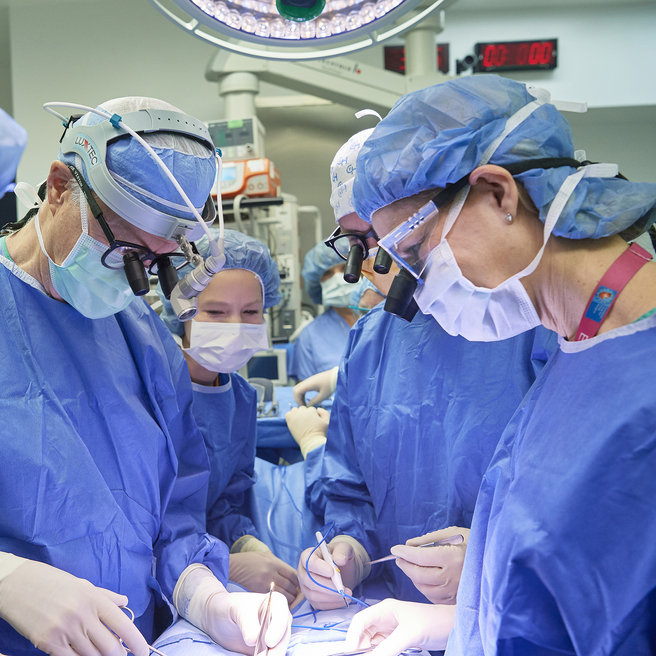
What are skeletal dysplasias
Skeletal dysplasias are a complex group of bone and cartilage disorders that may affect the fetal skeleton as it develops in utero.
As a whole, skeletal dysplasias are not common. They affect one in every 4,000-5,000 births, although the incidence may be higher since the symptoms may not manifest until early childhood, when short stature, joint abnormalities or other complications arise.
Symptoms
To date, more than 350 distinct skeletal disorders have been described which may result in numerous anomalies in the shape and size of the skeleton.
Some common symptoms of skeletal dysplasias include:
- Shortening in the bones of the legs and/or arms
- Bowed or fractured bones
- A small thorax
- Abnormal ribs
- Absence of a limb
- Asymmetric bone growth (e.g., one leg is longer than the other)
- Duplication of fingers or toes
- Irregular, thickened or thin bones
- Demineralization
Distinct skeletal disorders are identified by a common grouping of symptoms and characteristics. Common skeletal dysplasias and associated symptoms include:
- Thanatophoric dysplasia is typically characterized by abnormal shortness of limbs; a bowed femur (thigh bone) or other bones of the extremities; a small chest cage; thickened soft tissues; flattened vertebrae; unusually prominent forehead and depressed nasal bridge; and Cloverleaf skull (type II).
- Campomelic dysplasia is generally associated with a bowed femur (thigh bone) or other bones of the extremities; shortened limbs clubfeet; missing ribs; ambiguous genitalia; flattened facial features; and an unusually prominent forehead.
- Achondroplasia is characterized by shortened limbs, short forearms and lower legs; stubby fingers unusually prominent forehead; and abnormally decreased distance of the lumbar vertebrae in the lower back.
- Osteogenesis imperfecta typically includes fractures; bowed, irregular thickened bones; short/normal size extremities; soft, thin skull
- Achondrogenesis presents with thickened soft tissues; short limbs; bones of the spine that are not mineralized or fully formed; and a small thorax.
Causes
The causes of skeletal dysplasias are nearly as diverse as the number of distinct disorders. Generally, however, the causes can be cataloged into three groups:
- Genetically inherited as dominant or recessive traits or X-linked disorders
- The result of spontaneous mutations
- Secondary to exposure to a toxic substance or infectious agent that results in the disruption of normal skeletal development
Nearly half of the documented skeletal dysplasias are caused by a genetic mutation that makes prenatal diagnosis possible through genetic testing. For details, see common skeletal dysplasias and symptoms.
Evaluation and diagnosis
The fetal skeleton is usually evaluated as part of a routine ultrasound around week 20 of the pregnancy.
If a skeletal dysplasia is suspected, the expectant mother will likely be referred to a facility that specializes in diagnosing, treating and caring for babies with congenital anomalies, such as the Center for Fetal Diagnosis and Treatment at The Children’s Hospital of Philadelphia.
At our Center, prenatal evaluation of skeletal dysplasias includes a detailed ultrasound of the fetal skeleton in the second or third trimester of gestation, and an extensive genetic family history work up.
Prenatal diagnosis of skeletal dysplasias remains challenging, especially when there is no family history of the disorders. This is because:
- Each skeletal dysplasia is rare. Some display the same physical characteristics, yet are molecularly different. Conversely, some skeletal dysplasias display different physical characteristics, yet have similar genetic abnormalities.
- Some skeletal dysplasias are not apparent during the second trimester ultrasound. They only become evident in the third trimester, or even after birth, further complicating timely diagnosis.
- Ultrasound remains a limited imaging tool, even in the most experienced hands. Studies have indicated ultrasound has sensitivity in the range of 40 percent to 60 percent.
In the evaluation of skeletal dysplasias, CHOP has expanded its fetal imaging abilities beyond ultrasound and MRI to also include low-dose fetal computed tomography (CT). Low-dose fetal CT is a powerful imaging tool that aids in diagnosing skeletal dysplasias and improves our ability to counsel patients with these fetal anomalies.
When the ultrasound exam demonstrates severe bone abnormalities and the diagnosis is indeterminate, a multidisciplinary team involving obstetricians, geneticists, radiologists and sonographers will assess if your baby is a candidate for low-dose fetal CT. Radiation dose is kept to a strict minimum, adhering to the principles of, or as low as reasonably achievable. Low-dose CT scans are only performed in the second and third trimesters of gestation, when fetal organs have already formed and developed, and never during the first trimester, when the fetus is most sensitive to radiation.
The CT scan includes only the part of the uterus where the fetus is. Once the scan is done, the images then undergo post-imaging computer-aided renderings to create multiple two- and three-dimensional pictures of the fetal skeletal system that depict the bones in exquisite detail.
Initial interpretation of the fetal CT is performed by pediatric radiologists who work closely with the Center for Fetal Diagnosis and Treatment and who have vast experience and expertise in prenatal diagnosis. The final diagnosis for each specific patient requires a multidisciplinary team including radiologists, obstetricians and geneticists.
By providing detailed visualization of the fetal bones, low-dose fetal CT allows us to provide improved parental counseling, pre-delivery planning and postnatal management in fetuses with a diagnosis of skeletal dysplasia.
Long-term outlook
The long-term outlook for babies with skeletal dysplasias varies greatly depending on the type of dysplasia, as well as associated abnormalities. About half of fetuses with skeletal dysplasia are stillborn or die within the first six weeks of life.
But not all children with dysplasias have severe medical problems. Many of these children can live relatively normal lives.
It is recommended that children born with or later diagnosed with a skeletal dysplasia be treated by a multidisciplinary team of experts, such as the one at The Children’s Hospital of Philadelphia.
By working with a coordinated team of geneticists, neonatologists, radiologists, orthopedists, pediatricians and specialists, your child will receive individualized care that addresses your child’s health, developmental and psychosocial issues.

Why Choose Us
At the Wood Center for Fetal Diagnosis and Treatment, you and your baby are in the hands of one of the most experienced fetal programs in the world.
Resources to help
Richard D. Wood Jr. Center for Fetal Diagnosis and Treatment Resources
Learning your baby has a birth defect is a life-changing experience. We want you to know that you are not alone. To help you find answers to your questions, we've created this list of educational health resources.