What is tracheal stenosis?
Tracheal stenosis is a narrowing of the trachea (windpipe) that is caused by an injury or a birth defect. There are two different types of tracheal stenosis:
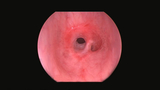
Endoscopic view of tracheal stenosis. Acquired tracheal stenosis (narrowing from injury) is a reaction to repeated irritation or injury. Causes can include ongoing irritation from a breathing tube, reaction to tissue injury due to pressure from a breathing tube cuff, or reaction to injury from external factors such as inhalational injury from fire.
- Congenital tracheal stenosis (narrowing due to a birth defect) is a rare condition in which the cartilage support structure of the trachea can cause a narrowing of the airway. A normal tracheal cartilage is C-shaped with a softer, posterior membrane which consists of muscle. Abnormalities of this cartilage can include tracheal cartilaginous sleeves, prone to obstruction and crusting, and complete tracheal rings, in which the trachea consists of several or more complete rings of cartilage with a narrowed diameter.
Signs and symptoms
Symptoms of tracheal stenosis can be present shortly after birth or develop after an acute injury to the trachea. Affected children may present with rapidly worsening symptoms in the face of an upper respiratory infection. Symptoms include:
- Noisy breathing (stridor)
- Recurring pneumonia
- Wheezing
- Cyanosis (blue-spells)
- Apnea (breathing pauses)
- Chest congestion
Testing and diagnosis
Imaging. Evaluation for tracheal stenosis may include X-rays and more advanced imaging such as CT or MR imaging. Imaging can provide information not only about the extent of airway narrowing, but also any other lesions that might be present such as cardiac problems.
Microlaryngoscopy and bronchoscopy. These diagnostic tests are essential to fully diagnose and characterize tracheal stenosis. Microlaryngoscopy and bronchoscopy help differentiate between tracheal lesions and other lesions in the larynx that can cause stridor and respiratory distress, and can help show the degree and length of narrowing in the trachea.
Evaluations by pulmonologists and gastroenterologists. Illnesses in the lungs or esophagus/stomach can affect the overall health of the patient and surgical outcomes. Advanced evaluation may include endoscopic examinations by these specialty services at the same time as a microlaryngoscopy and bronchoscopy.
Treatment
Treatment for tracheal stenosis depends on the nature and severity of the condition. There are a wide range of treatment options including:
Observation. Milder forms of tracheal stenosis which do not significantly affect the patient may be monitored with close observation and regular doctor’s visits. As the child and the airway grows, the condition may improve over time.
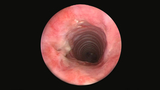
Balloon dilation. In less severe cases of tracheal stenosis, scar tissue may be divided with a sickle knife and then dilated with an angioplasty-like balloon during an endoscopic, non-surgical procedure. The formation of new scarring can be avoided by injecting the tissue with a steroid during the time of balloon dilation.
Tracheal resection and primary anastamosis. More severe cases may require open surgical intervention with reconstruction. For severe narrowing involving a few tracheal rings, tracheal resection and anastomosis may be performed. This involves surgically removing the defective tracheal segment and then repairing the airway by suturing the remaining ends back together. Surgery for complete tracheal rings usually involves more than just a few defective tracheal rings and thus can not usually be addressed with a tracheal resection.
Slide tracheoplasty. In long-segment tracheal stenosis, a slide tracheoplasty is required. In this surgery, the narrow part of the trachea is cut horizontally. Then a vertical incision is made in the back part of one segment and the front part of the other tracheal segment. Finally, the two sections are slid together and sutured so that they overlap, providing a wider tracheal airway.
Resources to help
Center for Pediatric Airway Disorders Resources
We have created resources to help you find answers to your questions about airway disorders and feel confident with the care you are providing your child.

