The patient was born at 24 weeks' gestation at an outside hospital after C-section for severe maternal pre-eclampsia. Birthweight was 885 grams. The infant’s early course included intubation for respiratory distress syndrome and surfactant administration and treatment of a patent ductus arteriosus with Indocin.
On DOL 5, he developed bilateral grade IV intraventricular hemorrhage (IVH). Follow-up head ultrasound showed worsening hydrocephalus that was accompanied by rapid head growth of 2 cm over the course of a week.
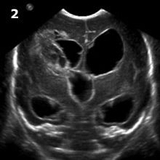
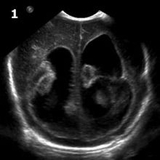
Around 3 weeks of life, the referring site contacted CHOP neurosurgeon Greg Heuer, MD, PhD, who recommended transfer. On arrival, the infant’s head ultrasound was repeated. (Figures 1 and 2: Coronal images from head ultrasound obtained prior to surgery showing ventriculomegaly.) The fronto-occipital ratio (FOR) was 0.69, and he developed apnea/bradycardia for which he was intubated (also in anticipation of planned surgery).
On the day of arrival, Heuer performed bedside reservoir placement in the N/IICU to avoid temperature instability. The patient tolerated the procedure well. In the subsequent days, the reservoir was tapped for tense fontanelle and rapid head growth. The frequency of the apnea/bradycardia has also improved.
Pathway for the Treatment of Preterm Infants with Post-hemorrhagic Hydrocephalus
Our team of neonatologists has collaborated with CHOP neurosurgeons to create a pathway to aid clinicians in diagnosing and treating hydrocephalus after intraventricular hemorrhage (IVH) in preterm infants.
The goals of the pathway are to:
- Standardize timing of shunt/reservoir placement based on radiologic measurements and clinical factors
- Monitor for increases in shunt/reservoir failures and infections
Find this pathway and other pathways our Hospital has created, visit chop.edu/pathways.
Featured in this article
Specialties & Programs

The patient was born at 24 weeks' gestation at an outside hospital after C-section for severe maternal pre-eclampsia. Birthweight was 885 grams. The infant’s early course included intubation for respiratory distress syndrome and surfactant administration and treatment of a patent ductus arteriosus with Indocin.
On DOL 5, he developed bilateral grade IV intraventricular hemorrhage (IVH). Follow-up head ultrasound showed worsening hydrocephalus that was accompanied by rapid head growth of 2 cm over the course of a week.

Around 3 weeks of life, the referring site contacted CHOP neurosurgeon Greg Heuer, MD, PhD, who recommended transfer. On arrival, the infant’s head ultrasound was repeated. (Figures 1 and 2: Coronal images from head ultrasound obtained prior to surgery showing ventriculomegaly.) The fronto-occipital ratio (FOR) was 0.69, and he developed apnea/bradycardia for which he was intubated (also in anticipation of planned surgery).
On the day of arrival, Heuer performed bedside reservoir placement in the N/IICU to avoid temperature instability. The patient tolerated the procedure well. In the subsequent days, the reservoir was tapped for tense fontanelle and rapid head growth. The frequency of the apnea/bradycardia has also improved.
Pathway for the Treatment of Preterm Infants with Post-hemorrhagic Hydrocephalus
Our team of neonatologists has collaborated with CHOP neurosurgeons to create a pathway to aid clinicians in diagnosing and treating hydrocephalus after intraventricular hemorrhage (IVH) in preterm infants.
The goals of the pathway are to:
- Standardize timing of shunt/reservoir placement based on radiologic measurements and clinical factors
- Monitor for increases in shunt/reservoir failures and infections
Find this pathway and other pathways our Hospital has created, visit chop.edu/pathways.
Contact us
Division of Neonatology