The last several decades have seen remarkable progress in the care of children born with cleft lip and palate. Improved surgical techniques and technological advances, as well as a better understanding of the factors that affect outcomes, have significantly transformed this journey for children with clefts and their families.
Whereas in the past, it was expected to take multiple operations to repair the lip and many more to close the palate, and even afterward, patients would experience ongoing stigmatization due to a distinctive speech quality and facial appearance, today the expectation and typical course is far different. In most cases, a single surgery can reconstruct the lip and nose, and a single surgery can restore the palatal form and function. Both procedures are performed in infancy to normalize the facial structures early, and thus allow the child to progress on a typical course of physical, social and emotional development.
Although revisional surgery is often performed on the lip and nose, these are typically minor and performed later in childhood and adolescence. In our experience at CHOP, revisional surgery on the palate is needed in only 5.2% of patients for a fistula, or hole in the palate, and in only 8.1% of patients to improve speech quality; rates are similar in children with associated genetic syndromes. Depending on the type of cleft, later surgeries on the gums and jaw may still be required, although continued research into the determinants of facial growth in children with clefts may lessen the need for some of these procedures in the future.
Prenatal Evaluation of Cleft Lip/Palate
Advances in imaging to allow early and more accurate diagnosis of a cleft in the prenatal period has transformed the process of parental education. The challenge for a cleft surgeon is to prepare the family appropriately as they embark on their cleft journey. While having a congenital appearance difference may present a variety of challenges for children and their families, we convey the expectation that the child will lead a normal life, balanced with the facts that multiple surgeries are required and often complemented by additional treatments and therapies for speech and orthodontics.
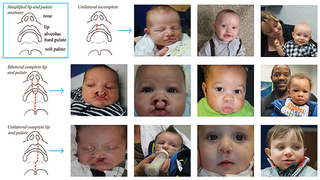
Increasingly, the first visit with the surgeon occurs as a prenatal consultation. As the exact characteristics of the cleft are yet unknown, education must cover the spectrum of cleft conditions and treatments, and care must be taken not to overwhelm the family at this critical time. Families benefit from the use of visual guides to illustrate the anatomic differences across the range of cleft presentations, with before and after photographs of patients through the spectrum of cleft severity and at different stages of healing and scar maturation. The most impactful images are often those of smiling children at play, images like those presented in this newsletter from our Annual Cleft Family Picnic event, which can help reassure the expecting family that their child will thrive.
Many families express concern about facial scarring. We emphasize that although children with clefts of the lip will have a permanent external scar, it is our earnest goal to make this scar barely visible. And internally, this mark reflects the child’s inner strength, resilience and journey.
References
The reducing opioid use in children with clefts protocol: A multidisciplinary quality improvement effort to reduce perioperative opioid use in patients undergoing cleft surgery. Lee A, Chang BL, Yan C, Fox JP, Magee L, Scott M, Maguire MA, Ross K, Rakow C, Drake F, McGinnis A, Watson A, Burlingame C, Kraemer FW, Muhly WT, Ruby J, Jackson OA. Plast Reconstr Surg. 2020;145(2):507-516.
The Children’s Hospital of Philadelphia modification of the Furlow double-opposing Z-palatoplasty: 30-year experience and long-term speech outcomes. Jackson O, Stransky CA, Jawad AF, Basta M, Solot C, Cohen M, Kirschner R, Low DW, Randall P, LaRossa D. Plast Reconstr Surg. 2013;132(3):613-622.
A 35-year experience with syndromic cleft palate repair: Operative outcomes and long-term speech function. Basta MN, Silvestre J, Stransky C, Solot C, Cohen M, McDonald-McGinn D, Zackai E, Kirschner R, Low DW, Randall P, LaRossa D, Jackson OA. Ann Plast Surg. 2014;73 Suppl 2:S130-135.
Featured in this article
Specialties & Programs
The last several decades have seen remarkable progress in the care of children born with cleft lip and palate. Improved surgical techniques and technological advances, as well as a better understanding of the factors that affect outcomes, have significantly transformed this journey for children with clefts and their families.
Whereas in the past, it was expected to take multiple operations to repair the lip and many more to close the palate, and even afterward, patients would experience ongoing stigmatization due to a distinctive speech quality and facial appearance, today the expectation and typical course is far different. In most cases, a single surgery can reconstruct the lip and nose, and a single surgery can restore the palatal form and function. Both procedures are performed in infancy to normalize the facial structures early, and thus allow the child to progress on a typical course of physical, social and emotional development.
Although revisional surgery is often performed on the lip and nose, these are typically minor and performed later in childhood and adolescence. In our experience at CHOP, revisional surgery on the palate is needed in only 5.2% of patients for a fistula, or hole in the palate, and in only 8.1% of patients to improve speech quality; rates are similar in children with associated genetic syndromes. Depending on the type of cleft, later surgeries on the gums and jaw may still be required, although continued research into the determinants of facial growth in children with clefts may lessen the need for some of these procedures in the future.
Prenatal Evaluation of Cleft Lip/Palate
Advances in imaging to allow early and more accurate diagnosis of a cleft in the prenatal period has transformed the process of parental education. The challenge for a cleft surgeon is to prepare the family appropriately as they embark on their cleft journey. While having a congenital appearance difference may present a variety of challenges for children and their families, we convey the expectation that the child will lead a normal life, balanced with the facts that multiple surgeries are required and often complemented by additional treatments and therapies for speech and orthodontics.
Increasingly, the first visit with the surgeon occurs as a prenatal consultation. As the exact characteristics of the cleft are yet unknown, education must cover the spectrum of cleft conditions and treatments, and care must be taken not to overwhelm the family at this critical time. Families benefit from the use of visual guides to illustrate the anatomic differences across the range of cleft presentations, with before and after photographs of patients through the spectrum of cleft severity and at different stages of healing and scar maturation. The most impactful images are often those of smiling children at play, images like those presented in this newsletter from our Annual Cleft Family Picnic event, which can help reassure the expecting family that their child will thrive.
Many families express concern about facial scarring. We emphasize that although children with clefts of the lip will have a permanent external scar, it is our earnest goal to make this scar barely visible. And internally, this mark reflects the child’s inner strength, resilience and journey.

References
The reducing opioid use in children with clefts protocol: A multidisciplinary quality improvement effort to reduce perioperative opioid use in patients undergoing cleft surgery. Lee A, Chang BL, Yan C, Fox JP, Magee L, Scott M, Maguire MA, Ross K, Rakow C, Drake F, McGinnis A, Watson A, Burlingame C, Kraemer FW, Muhly WT, Ruby J, Jackson OA. Plast Reconstr Surg. 2020;145(2):507-516.
The Children’s Hospital of Philadelphia modification of the Furlow double-opposing Z-palatoplasty: 30-year experience and long-term speech outcomes. Jackson O, Stransky CA, Jawad AF, Basta M, Solot C, Cohen M, Kirschner R, Low DW, Randall P, LaRossa D. Plast Reconstr Surg. 2013;132(3):613-622.
A 35-year experience with syndromic cleft palate repair: Operative outcomes and long-term speech function. Basta MN, Silvestre J, Stransky C, Solot C, Cohen M, McDonald-McGinn D, Zackai E, Kirschner R, Low DW, Randall P, LaRossa D, Jackson OA. Ann Plast Surg. 2014;73 Suppl 2:S130-135.
Contact us
Cleft Lip and Palate Program