
Proton therapy, which uses a highly precise beam to target radiation directly at a tumor site, is indicated for many different types of malignancies, but is mainly used for solid tumors. The goal is to give as much radiation as indicated to the tumor while sparing normal tissue surrounding the tumor, so as to limit short- and long-term side effects from radiation, especially in children. Children’s Hospital of Philadelphia’s Pediatric Proton Therapy Center is located in the Roberts Proton Therapy Center in Penn Medicine’s Perelman Center for Advanced Medicine, across the street from CHOP. The facility is child-friendly, with a waiting area and anesthesia suite designed with pediatric patients in mind.
A successful application of pediatric proton therapy at CHOP is demonstrated in the case of Elena, now 10. She was diagnosed in 2014 with craniopharyngioma, a rare type of benign brain tumor that begins near the brain’s pituitary gland. As the tumor grows, it can affect the function of the pituitary gland and other brain structures.
Elena had been experiencing vision loss over the course of several weeks. She had an MRI at a children’s hospital in her home state of Ohio, and the results showed the tumor pressing against the optic nerve. Surgery to remove as much of the tumor as possible was performed. The tumor recurred 18 months later.
Considering the options
Because these tumors generally grow slowly, the family had time to research how to address the recurrence. They contacted several children’s hospitals, including CHOP, where they talked to pediatric radiation oncologist Christine Hill-Kayser, MD, Chief of the Pediatric Service for the Department of Radiation Oncology at the Hospital of the University of Pennsylvania. Hill-Kayser was confident Elena’s tumor could be treated using only proton therapy, but reassured the family that CHOP has world-class pediatric neurosurgeons if that route was needed. The family decided to travel to CHOP from Ohio for proton therapy in spring 2016.
The CHOP team includes pediatric oncologists, radiation oncologists, pediatric anesthesiologists, pediatric neuropsychologists, physicists, dosimetrists, nurses, radiation therapists, child life specialists and other medical professionals who are experts on the unique needs of children with cancer.
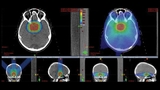
“We worked closely with Elena’s family to design an approach to treatment that would allow her the best potential to be cured of her disease while minimizing risk of damage to her visual structures, pituitary gland, and brain,” explains Hill-Kayser. “We designed a proton therapy plan that utilized 3 beams converging on the tumor target, each delivering a third of the needed dose.”
How proton therapy works
Proton particles are heavy. They deposit most of their dose at the end of their track in what’s known as the Bragg peak. Then they stop. This arc is different from photons, which are very light particles that continue to emit doses as they travel beyond the tumor’s site.
“Using complex hardware and software,” says Hill-Kayser, “we can make each proton beam stop exactly where we need it to — in Elena’s case, we designed 3 beams to enter her brain from different angles and stop as soon as the tumor target had been treated. Through this approach, we were able to minimize radiation dose to the normal brain, nerves, and blood vessels.”
Elena had 30 rounds of proton therapy in 49 days. During that time, Elena underwent MRI scans every 2 weeks to ensure that her tumor had not shifted in a way that would require modification of the radiation plan. More than two years later, Elena remains free of disease. She’s living a normal life and is in the gifted program at school.
Elena’s mother, Lina, reports that Elena was able to stay active during the entire treatment phase, exercising and going on long walks. When she was first admitted to the Ohio hospital, she was legally blind. Today her vision is 20/20, with minor issues with peripheral vision. “There was no cognitive or hearing damage, no arterial damage,” says Lina. “It’s such an amazing technology.”
Featured in this article
Specialties & Programs
Proton therapy, which uses a highly precise beam to target radiation directly at a tumor site, is indicated for many different types of malignancies, but is mainly used for solid tumors. The goal is to give as much radiation as indicated to the tumor while sparing normal tissue surrounding the tumor, so as to limit short- and long-term side effects from radiation, especially in children. Children’s Hospital of Philadelphia’s Pediatric Proton Therapy Center is located in the Roberts Proton Therapy Center in Penn Medicine’s Perelman Center for Advanced Medicine, across the street from CHOP. The facility is child-friendly, with a waiting area and anesthesia suite designed with pediatric patients in mind.
A successful application of pediatric proton therapy at CHOP is demonstrated in the case of Elena, now 10. She was diagnosed in 2014 with craniopharyngioma, a rare type of benign brain tumor that begins near the brain’s pituitary gland. As the tumor grows, it can affect the function of the pituitary gland and other brain structures.
Elena had been experiencing vision loss over the course of several weeks. She had an MRI at a children’s hospital in her home state of Ohio, and the results showed the tumor pressing against the optic nerve. Surgery to remove as much of the tumor as possible was performed. The tumor recurred 18 months later.
Considering the options
Because these tumors generally grow slowly, the family had time to research how to address the recurrence. They contacted several children’s hospitals, including CHOP, where they talked to pediatric radiation oncologist Christine Hill-Kayser, MD, Chief of the Pediatric Service for the Department of Radiation Oncology at the Hospital of the University of Pennsylvania. Hill-Kayser was confident Elena’s tumor could be treated using only proton therapy, but reassured the family that CHOP has world-class pediatric neurosurgeons if that route was needed. The family decided to travel to CHOP from Ohio for proton therapy in spring 2016.
The CHOP team includes pediatric oncologists, radiation oncologists, pediatric anesthesiologists, pediatric neuropsychologists, physicists, dosimetrists, nurses, radiation therapists, child life specialists and other medical professionals who are experts on the unique needs of children with cancer.

“We worked closely with Elena’s family to design an approach to treatment that would allow her the best potential to be cured of her disease while minimizing risk of damage to her visual structures, pituitary gland, and brain,” explains Hill-Kayser. “We designed a proton therapy plan that utilized 3 beams converging on the tumor target, each delivering a third of the needed dose.”
How proton therapy works
Proton particles are heavy. They deposit most of their dose at the end of their track in what’s known as the Bragg peak. Then they stop. This arc is different from photons, which are very light particles that continue to emit doses as they travel beyond the tumor’s site.
“Using complex hardware and software,” says Hill-Kayser, “we can make each proton beam stop exactly where we need it to — in Elena’s case, we designed 3 beams to enter her brain from different angles and stop as soon as the tumor target had been treated. Through this approach, we were able to minimize radiation dose to the normal brain, nerves, and blood vessels.”
Elena had 30 rounds of proton therapy in 49 days. During that time, Elena underwent MRI scans every 2 weeks to ensure that her tumor had not shifted in a way that would require modification of the radiation plan. More than two years later, Elena remains free of disease. She’s living a normal life and is in the gifted program at school.
Elena’s mother, Lina, reports that Elena was able to stay active during the entire treatment phase, exercising and going on long walks. When she was first admitted to the Ohio hospital, she was legally blind. Today her vision is 20/20, with minor issues with peripheral vision. “There was no cognitive or hearing damage, no arterial damage,” says Lina. “It’s such an amazing technology.”
Contact us
Pediatric Proton Therapy Center