Case
D.M. is a 5-year-old girl with no medical or surgical history with persistent urinary leakage. She had been wet through potty training, but had achieved perfect stool continence. She had no fevers, respiratory symptoms, or diarrhea. Her urinalysis was normal. Her ultrasound showed normal kidneys. Her bladder was normal, emptied well, and held 15 cc. D.M. had been seen by her primary physician, who placed her on a timed voiding schedule, but she seemed to be nearly continuously incontinent of urine.
Her abdomen was soft and nontender. The anus was in a normal position. The kidneys were not palpable. The bladder was empty on percussion. The outward appearance of the mons pubis was normal with the exception of a subtle defect, which suggested that there was a mild separation of her pubic rami of about 1 cm. Her perineum was red and irritated near the urethra and vagina from the incontinence of urine we presumed. Close inspection of the introitus showed a bifid clitoris.
Discussion
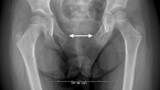
A plain film confirmed the pubic separation. In addition to the bifid clitoris and the irritated perineum, the labia minora were slightly patulous and separated superiorly along with the clitoral halves. The urethra was wide open and dripping urine when the labia were separated.
The urethral meatus appeared to be more anterior than normal and the mons pubis was displaced laterally.
The physical appearance is enough to make the diagnosis of epispadias, but a careful exam that includes separating the labia is essential.
Treatment for epispadias begins before toilet training. The most important goals in the care of a child with the exstrophy-epispadias spectrum are to preserve normal kidney function, develop adequate bladder function, promote urinary continence, and provide acceptable appearance and function of the external genitalia. Epispadias in the male or female is a minor form of bladder exstrophy. In this case, as in complete exstrophy, our surgical therapy would attempt to reconstruct the bladder neck and urethra to a normal caliber.
Our next step was an exam under anesthesia in the OR, which, combined with a cystoscopic exam, completed the diagnosis. The bladder outlet (urethra and bladder neck) was wide open. The ureteral orifices were in their normal locations. We placed a double lumen suprapubic tube that would allow us to measure bladder pressures during filling and emptying and assess D.M.’s ability to hold urine.
Four days later, we took her to our videourodynamics suite and filled her bladder with contrast. There was constant leakage from the urethra. Her bladder capacity was small, likely due to poor coaptation of the bladder neck muscle, which is part of the defect in complete epispadias. She had mild vesicoureteral reflux, which is common in the exstrophy/epispadias complex.
After a discussion with her parents, we arranged for bilateral anterior innominate osteotomies, along with bladder neck reconstruction that helped restore the normal anatomy of the bladder outlet and urethra. After 6 weeks recovery time, a long period of physical therapy (PT)—3 weeks inpatient and 12 weeks outpatient—followed. PT encouraged and helped D.M. develop an understanding of the perineal muscles required to provide continence, and her dry interval between voids gradually became more robust. Over the next 4 to 6 years, her bladder will grow and her continence will improve.
More About MIBEC
In an effort to optimize surgical technique and overall patient care and outcome, we formed the Multi-Institutional Bladder Exstrophy Consortium (MIBEC) to increase experience and expertise with the surgery and management of those with a diagnosis on the exstrophy-epispadias spectrum. The consortium, launched in 2013, comprises three institutions: Children’s Hospital of Philadelphia, Boston Children’s Hospital, and Children’s Hospital of Wisconsin, each having enlisted pediatric urologic surgeons with a specific interest and dedication to the care of patients with these conditions. Complete primary repair of bladder exstrophy (CPRE) is the technique of choice at all 3 institutions. During each patient’s surgery, including D.M.’s, the participating surgeons travel to the others’ operating rooms to observe, provide helpful commentary, and record all procedures with high-definition video.
References and suggested readings
Docimo SG, Canning DA, Khoury AE, ed. Kelalis-King-Belman Textbook of Clinical Pediatric Urology. 5th ed. Abingdon (Oxon), United Kingdom: Informa Healthcare UK, Ltd.; 2007, p. 1003.
Borer JG, Vasquez E, Canning DA, et al. Short-term outcomes of the multi-institutional bladder exstrophy consortium: successes and complications in the first two years of collaboration. J Pediatr Urol. 2017;13(3):275.e1-275.e6.
Featured in this article
Specialties & Programs
Case
D.M. is a 5-year-old girl with no medical or surgical history with persistent urinary leakage. She had been wet through potty training, but had achieved perfect stool continence. She had no fevers, respiratory symptoms, or diarrhea. Her urinalysis was normal. Her ultrasound showed normal kidneys. Her bladder was normal, emptied well, and held 15 cc. D.M. had been seen by her primary physician, who placed her on a timed voiding schedule, but she seemed to be nearly continuously incontinent of urine.
Her abdomen was soft and nontender. The anus was in a normal position. The kidneys were not palpable. The bladder was empty on percussion. The outward appearance of the mons pubis was normal with the exception of a subtle defect, which suggested that there was a mild separation of her pubic rami of about 1 cm. Her perineum was red and irritated near the urethra and vagina from the incontinence of urine we presumed. Close inspection of the introitus showed a bifid clitoris.
Discussion
A plain film confirmed the pubic separation. In addition to the bifid clitoris and the irritated perineum, the labia minora were slightly patulous and separated superiorly along with the clitoral halves. The urethra was wide open and dripping urine when the labia were separated.
The urethral meatus appeared to be more anterior than normal and the mons pubis was displaced laterally.
The physical appearance is enough to make the diagnosis of epispadias, but a careful exam that includes separating the labia is essential.

Treatment for epispadias begins before toilet training. The most important goals in the care of a child with the exstrophy-epispadias spectrum are to preserve normal kidney function, develop adequate bladder function, promote urinary continence, and provide acceptable appearance and function of the external genitalia. Epispadias in the male or female is a minor form of bladder exstrophy. In this case, as in complete exstrophy, our surgical therapy would attempt to reconstruct the bladder neck and urethra to a normal caliber.
Our next step was an exam under anesthesia in the OR, which, combined with a cystoscopic exam, completed the diagnosis. The bladder outlet (urethra and bladder neck) was wide open. The ureteral orifices were in their normal locations. We placed a double lumen suprapubic tube that would allow us to measure bladder pressures during filling and emptying and assess D.M.’s ability to hold urine.
Four days later, we took her to our videourodynamics suite and filled her bladder with contrast. There was constant leakage from the urethra. Her bladder capacity was small, likely due to poor coaptation of the bladder neck muscle, which is part of the defect in complete epispadias. She had mild vesicoureteral reflux, which is common in the exstrophy/epispadias complex.
After a discussion with her parents, we arranged for bilateral anterior innominate osteotomies, along with bladder neck reconstruction that helped restore the normal anatomy of the bladder outlet and urethra. After 6 weeks recovery time, a long period of physical therapy (PT)—3 weeks inpatient and 12 weeks outpatient—followed. PT encouraged and helped D.M. develop an understanding of the perineal muscles required to provide continence, and her dry interval between voids gradually became more robust. Over the next 4 to 6 years, her bladder will grow and her continence will improve.
More About MIBEC
In an effort to optimize surgical technique and overall patient care and outcome, we formed the Multi-Institutional Bladder Exstrophy Consortium (MIBEC) to increase experience and expertise with the surgery and management of those with a diagnosis on the exstrophy-epispadias spectrum. The consortium, launched in 2013, comprises three institutions: Children’s Hospital of Philadelphia, Boston Children’s Hospital, and Children’s Hospital of Wisconsin, each having enlisted pediatric urologic surgeons with a specific interest and dedication to the care of patients with these conditions. Complete primary repair of bladder exstrophy (CPRE) is the technique of choice at all 3 institutions. During each patient’s surgery, including D.M.’s, the participating surgeons travel to the others’ operating rooms to observe, provide helpful commentary, and record all procedures with high-definition video.
References and suggested readings
Docimo SG, Canning DA, Khoury AE, ed. Kelalis-King-Belman Textbook of Clinical Pediatric Urology. 5th ed. Abingdon (Oxon), United Kingdom: Informa Healthcare UK, Ltd.; 2007, p. 1003.
Borer JG, Vasquez E, Canning DA, et al. Short-term outcomes of the multi-institutional bladder exstrophy consortium: successes and complications in the first two years of collaboration. J Pediatr Urol. 2017;13(3):275.e1-275.e6.
Contact us
Division of Urology