Reversing Severe Lymphatic Disorder Caused by Noonan Syndrome: Maria’s Story
Reversing Severe Lymphatic Disorder Caused by Noonan Syndrome: Maria’s Story
For the first two-plus years of Maria’s life, her parents, Elizabeth and Patrick, wondered why their daughter was so small. After Maria was diagnosed with a genetic disorder, she nonetheless remained generally healthy until she was in eighth grade, when she started experiencing internal bleeding that would require lifelong blood transfusions. Under the care of the team at the Jill and Mark Fishman Center for Lymphatic Disorders at Children's Hospital of Philadelphia (CHOP), Maria became the first person with her condition to try an experimental drug.

Born prematurely at 26 weeks, Maria needed to stay on life support for three months. She was also born with a minor cardiac issue, a small hole in her heart, that resolved itself without any intervention. “Once we were home, everything was pretty normal,” says Elizabeth. “She was just very tiny.” Her premature birth was assumed to be the cause of her small size.
When the family moved from Virginia to the Philadelphia area, their new pediatrician suggested that Maria, now 2, should have a follow-up visit with a cardiologist just to make sure all was still well with her heart. “As soon as we walked in, the doctor said, ‘Oh, she’s a Noonan!’” says Elizabeth. “It was the first time someone mentioned she might have a genetic disorder.”
Genetic tests verified that Maria had Noonan syndrome, a disorder that can affect the development of various parts of the body. The syndrome’s effects can manifest themselves in short stature, specific facial characteristics, heart defects, other physical problems and possible developmental delays. Each person has different combinations and various degrees of these symptoms. Despite the heart complication Maria had been born with, “We felt fortunate she didn’t have any of the cardiac issues that a lot of the Noonan kids have,” says Elizabeth. Ultimately, Maria seemed to have only mild Noonan symptoms.
‘There was no tumor’
Maria progressed through her toddler years without incident, but when she was 5, she began having pains in her hands and feet. Doctors performed a whole-body scan and discovered what appeared to be a tumor near her spine. “It was in an odd location,” explains Elizabeth. “The oncologist wasn’t sure what it was. So they decided to perform exploratory surgery. And there was no tumor.”
What the scan had picked up might have been a lymphatic system abnormality, a complication that appears in about one-fifth of people with Noonan syndrome. The lymphatic system is the body-wide network that circulates a clear, protein-rich fluid that plays a role in filtering toxins, redistributing excess fluids and fighting infection. Sometimes lymph vessels become blocked or leak, or — what seemed to be the case with Maria — the whole system can be functioning abnormally.
Two months after the surgery, Maria developed a chylothorax, a lymphatic leak into the thoracic cavity that holds the lungs. “She was having a hard time breathing, so we took her to the ER,” says Elizabeth. Doctors inserted a chest tube to drain the fluid, and Maria stayed in the hospital for six weeks, causing her to miss the first day of kindergarten.
At the time, the family was considering bringing Maria to CHOP. “We thought, ‘If this doesn’t resolve, then we’ll go there,’ but it did resolve on its own,” says Elizabeth. Maria lost some function in her left lung. But after this scare, everything was fine. For eight years, Maria was, overall, healthy.
Mysterious internal bleeding
“Eight years with no issues lulled us into a false sense of security,” says Elizabeth. But as Maria was nearing the end of eighth grade, she started feeling not well. “She couldn’t put her finger on it,” says Elizabeth. “She had bouts of abdominal pain and nausea, and she was tired and really pale.”
When the exhaustion persisted, the family again headed to the ER, where tests showed that Maria’s hemoglobin level was very low, making her anemic. She had internal bleeding of an unknown cause, and was admitted and received a blood transfusion.
Doctors soon figured out that Maria’s abnormal lymphatic system was leaking lymphatic fluid into her gut, a condition known as protein losing enteropathy, which involves abnormal lymphatics in the gut. Over time, this was also causing bleeding in her gastrointestinal tract. Needing to stay in the hospital because of her deteriorating condition, Maria missed her eighth-grade graduation ceremony.
A drug to break the cycle
Until recently, there wasn’t much that could be done to treat children with lymphatic problems. Discoveries made at CHOP’s Jill and Mark Fishman Center for Lymphatic Disorders changed that. Lymphatic center director Yoav Dori, MD, PhD, and colleagues developed the first diagnostic test that gave clinicians a clear view of the anatomy and flow of the lymphatic system. They also determined how to plug leaking lymph vessels using a minimally invasive procedure perfected at CHOP.
In June 2018, Maria came to CHOP and was seen by Dr. Dori, who within two days performed the procedure to seal the leaks. It helped, somewhat. Maria, however, had lost weight and was under 70 pounds — “What my second-grader weighs now,” notes Elizabeth. Maria went home with a feeding tube but remained weak and underweight. Several months later, the GI bleeding returned, Maria received another blood transfusion, and Dr. Dori again sealed the leaks.
It was becoming clear that these fixes were temporary. Dr. Dori, Maria and her family were looking at a future where the cycle of bleeding, transfusions and interventions would just keep happening.
From the start, Dr. Dori had told the family about a drug called a MEK inhibitor. It had already utterly transformed the life of an extremely sick patient at CHOP named Daniel, who had a different kind of rare central lymphatic anomaly that caused his lymphatic vessels to enlarge and multiply. The MEK inhibitor triggered his lymphatic vessels to remodel themselves, which completely stopped the leaking.
Did Maria want to be the first person with Noonan syndrome and severe lymphatic disorder to try the MEK inhibitor? It would require applying to the U.S. Food and Drug Administration (FDA) to get approval for off-label compassionate use of the drug. Jean Belasco, MD, an oncologist in CHOP’s Cancer Center who is part of Maria’s care team, put in the application.
“We had no hesitation whatsoever,” says Elizabeth. “Deciding to do the drug was kind of a relief. Dr. Dori had prepared us all along. And Maria saw the value from the beginning. It was all she talked about until everything had been submitted to the FDA and approved. She saw the value for herself, but she was also thinking of other Noonan kids.”
‘Everything went away’
In July 2019, the FDA gave its approval for using the MEK inhibitor — and the effect within three months was remarkable. “It’s been lifesaving,” Elizabeth says. Maria’s lymphatic channels have remodeled themselves in a way that stopped the gastrointestinal protein leak and bleeding from her intestinal wall. Even the lung that had been damaged by the chylothorax when Maria was 5 unexpectedly cleared up. Maria put on 30 pounds, bringing her weight up to just under 100 pounds, and for the first time in years, she outgrew her jeans and shoes.
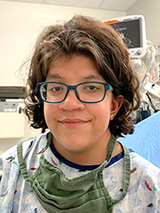
“Everything completely went away,” says Dr. Dori of Maria’s problems, with a note of amazement.
Dr. Belasco sees a future full of possibility: “Although we are in the early days of this type of personalized medicine, the hope is that by looking at patients’ mutations, we can find more drugs and better care for patients with genetic diseases.”
While Maria and previous patient Daniel had different conditions that involved different genetic mutations, there was a commonality, explains Hakon Hakonarson, MD, PhD, Director of the Center for Applied Genomics at CHOP. “Both genes are on a pathway that influences the expression of MEK,” Dr. Hakonarson says. “You can look at it like a pathway where, say, 15 things need to happen for a cell to function properly. Daniel’s mutation was item number three, and Maria’s mutation was maybe item number nine. But both are part of a chain that ultimately passes through a tunnel that leads to the MEK molecule. Both patients’ mutations led to an overexpression of MEK, which resulted in the uncontrolled proliferation of lymphatic vessels.”
Hakonarson is also part of CHOP’s Comprehensive Vascular Anomalies Program (CVAP), a CHOP Frontier Program that uses state-of-the-art genomics and personalized research strategies to determine the causes of complex vascular conditions and identify targeted therapies. The program works closely with the Lymphatic Imaging and Interventions Frontier Program, which is led by Dori. CHOP’s Frontier Programs conduct cutting-edge research that translates into advanced clinical care. The CVAP, in particular, draws on the extensive clinical and genomic research capacity within the Cancer Center and Center for Applied Genomics.
The drug blocks MEK and thus puts the brakes on a lymphatic system in overdrive. The MEK inhibitor remodels the lymphatic system, although how the drug is accomplishing this feat is not fully understood.
Regardless of the mysteries about the drug that remain to be solved, it has made one significant change in Maria that Elizabeth can’t talk about without getting choked up: “She’s a lot happier. I think she knew deep down she was dying. The medicine gave her hope.” And it might do the same for others suffering from lymphatic problems related to Noonan syndrome.