Zion’s story: The gift of hands
Zion’s story: The gift of hands
(Originally published July, 2015. View latest update on Zion's progress.)
An 8-year-old boy holds a mini football in the palm of his hand, gently squeezing it between thumb and fingers, dreaming of the day he can get out on the field and throw a pass. It’s an utterly ordinary scenario, except for one thing: only a few weeks ago, this child had no hands.
In 2008, at the age of 2, Zion Harvey developed sepsis, a life-threatening infection that attacked his entire body and eventually required amputation of both of his hands and his legs below the knee. The infection also damaged Zion’s kidneys and two years later, he underwent an organ transplant, receiving a kidney from his mother, Pattie Ray.

Despite this rocky start, in the years that followed Zion grew strong and healthy. A happy and outgoing child, he adapted well to life without hands, learning to eat, write and even play video games with his residual limbs. He figured out ways to perform most of the activities other kids his age could do. (Zion received prosthetics for his feet, and was able to walk, run and jump with complete independence.)
A radical idea
In 2012, Pattie brought Zion, now 6, from their home in Baltimore to see Scott Kozin, MD, a surgeon and chief of staff at Philadelphia Shriners Hospitals for Children — Philadelphia, and his partner, Dan Zlotolow, MD. They came to talk about fitting Zion with prosthetic hands, but the doctors had a different and radical suggestion: a hand transplant.
This extremely rare procedure, also known as vascularized composite allotransplantation (VCA), is being performed by only a few surgical teams around the world — and none had performed it in a child. The operation requires exceptional expertise in complex microvascular surgery and hand surgery, connecting muscles, tendons and blood vessels — the latter with sutures finer than a human hair. Patients undergoing the surgery also require a vast network of support services.
Dr. Kozin and Dr. Zlotolow referred the family to the Hand Transplantation Program at The Children’s Hospital of Philadelphia. Led by director L. Scott Levin, MD, FACS, who is also the Paul B. Magnuson Professor, chairman of the Department of Orthopaedics, and professor of surgery (Plastic Surgery) at Penn Medicine, the program combines the expertise of CHOP’s Division of Plastic, Reconstructive and Oral Surgery and the Orthopedic Center with that of physicians in Penn’s Transplant Institute. Dr. Levin is a world-renowned authority in the field, having performed Penn’s first bilateral adult hand transplant in 2011.
A careful evaluation
Over the course of 18 months, Zion underwent extensive evaluation of his medical condition and level of function without hands, and of his and his family’s readiness to cope with the transplant process and its aftermath.
Paradoxically, the unfortunate circumstances that resulted in his needing a kidney transplant proved to be in some ways fortuitous for Zion. In hand transplantation, doctors must weigh the potential benefits of the transplant surgery against the risks of immunosuppression medication patients must take for their entire life to prevent rejection. Zion was already taking immunosuppressants for his transplanted kidney, making the decision about hand transplantation less complicated in terms of the adverse effects of these medications.
Dr. Levin and his team quickly came to believe Zion was an excellent candidate for what would be the first pediatric bilateral hand transplant ever performed in the world. “As far as we know, it’s never even been attempted in a child,” says surgeon Benjamin Chang, MD, co-director of CHOP’s Hand Transplantation Program.
“The only shortcut”
Dr. Levin began assembling the massive and highly experienced team that would perform the surgery and care for Zion afterwards. It included hand surgeons (both orthopedic and plastic surgeons), nursing staff, pediatric anesthesiologists, occupational and physical therapists, social workers, pharmacists, psychologists, child life specialists and others. “The skills necessary to perform such a complex surgery at CHOP come from lessons learned over the past 20-plus years of performing pediatric solid organ transplantation,” says Abraham Shaked, MD, PhD, director of Penn’s Transplant Institute.
The OR team gathered several times for rehearsals, planning and practicing every step of the operation they would perform on Zion. Physicians at CHOP created 3D hand models, based on Zion’s measurements, to help identify appropriate donor hands. “There’s a saying in surgery,” says Dr. Levin. “’The only shortcut is preparation.’”
When Dr. Levin was convinced that the team was fully ready, Zion was listed for transplant with the United Network for Organ Sharing (UNOS), and the wait began.
Acquiring donor hands that were a match for Zion would be challenging. Considering factors of blood type, size, skin color and gender, Dr. Levin estimated that no more than 15 potential donors a year would be available nationwide. The difficult search, which would be expertly managed by the Gift of Life Donor Program, might take years.
But just three months later, Pattie received a call from Hand Transplantation Coordinator Christine McAndrew, PA-C: “Come to CHOP right away — a donor has been found.”
A historic surgery
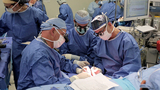
Led by Dr. Levin, the landmark surgery lasted 10 and a half hours, with 40 people — including 10 attending surgeons — performing various parts of the procedure. The hands and forearms were attached by connecting bones, blood vessels, nerves, muscles, tendons and finally, skin. After the first blood vessels between Zion’s arms and the donor hands were connected, the team was encouraged as the palms and fingers gradually turned pink — blood was circulating as it should.
Just a few days after the operation, Zion was already displaying his resilience and positive attitude as he adjusted to the incredible experience of having new hands. In daily sessions with CHOP physical and occupational therapists, he works hard, slowly gaining movement and strength in each hand, learning to pick up and hold objects. His therapy will be ongoing for many months. He will also be monitored closely for any signs of rejection or other complications.
The challenges facing Zion are new, but his determination isn’t. “He’s already done so many amazing things,” Pattie says of her son. “This is just one more hurdle he’s jumped.”
View an update from one year after Zion's hand transplant surgery.