What are atrioventricular canal defects?
A common atrioventricular (AV) canal defect (also known as an atrioventricular septal defect) is a problem in the part of the heart that connects the upper chambers (atria) to the lower chambers (ventricles). There are two types of atrioventricular canal defects: complete and partial. Of note, many children with Down syndrome (also known as Trisomy 21) have a common AV canal defect.
Complete atrioventricular canal (CAVC) defect
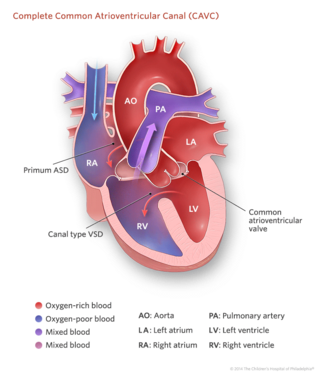
Complete common atrioventricular canal (CAVC) defect is a congenital heart disease in which there is a large hole in the tissue (the septum) that separates the left and right sides of the heart. The hole is in the center of the heart, where the upper chambers and lower chambers meet.
As the heart formed abnormally, the valves that separate the upper and lower chambers also developed abnormally. In a normal heart, two valves separate the upper and lower chambers of the heart: the tricuspid valve separates the right chambers, and the mitral valve separates the left chambers. In a child with a complete atrioventricular canal defect, there is one large valve over both ventricles and often that valve leaks back into the upper chambers.
As a result of the abnormal passageway between the two sides of the heart, blood from both sides mix, and too much blood circulates back to the lungs before it travels through the body. This means the heart works harder than it would normally, often becoming enlarged and damaged if the problems aren't repaired.
Partial common atrioventricular canal defects
A partial atrioventricular canal defect is the less severe form of this heart defect. The hole does not extend between the lower chambers of the heart and the valves are better formed. Usually, it is necessary only to close the hole between the upper chambers (this hole is called an atrial septal defect or ASD) and to do a minor repair of the valve.
Signs and symptoms of atrioventricular canal defects
In a complete atrioventricular canal defect, the following symptoms may be present within several days or weeks of birth:
- Blue or purple tint to lips, skin and nails (cyanosis)
- Difficulty breathing
- Poor weight gain and growth
- Heart murmur: the heart sounds abnormal when a doctor listens with a stethoscope
Partial atrioventricular canal defects may cause fewer symptoms than some other heart defects and may not be diagnosed until later in children or rarely in early adulthood. Then, the young adult may begin to experience an irregular heartbeat (arrhythmia), leaky heart valves or other effects.
Testing and diagnosis of AVCD
Often, a complete CAVC is diagnosed on a fetal ultrasound and/or echocardiogram. Our Fetal Heart Program can prepare a plan for delivery and care immediately after birth.
The pediatrician who evaluates your baby in the hospital might also make the diagnosis. Or a primary care pediatrician might notice a heart murmur and other symptoms and refer your child to the Cardiac Center at Children's Hospital.
Diagnosis of AV canal defects may require some or all of these tests:
- Echocardiogram: sound waves are used to create an image of the heart
- Electrocardiogram (ECG): a record of the electrical activity of the heart
- Chest X-ray
- Pulse oximetry: a noninvasive way to monitor the oxygen content of the blood
- Cardiac catheterization: a thin tube is inserted into the heart through a vein and/or artery in either the leg or through the umbilicus ("belly button")
- Cardiac MRI: a three-dimensional image shows the heart's abnormalities
Treatment for atrioventricular canal defects
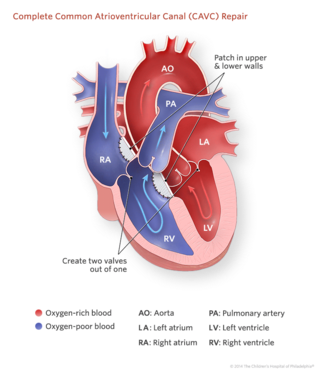
Complete CAVC requires surgery, usually within the first two or three months of life. The surgeon will close the large hole with one or two patches. The patches are stitched into the heart muscle, and as the child grows, the tissue grows over the patches.
The surgeon will also separate the single large valve into two valves and will reconstruct the valves so they are as close to normal as possible, depending on the child's heart anatomy.
Partial CAVC also requires surgery, whether diagnosed in childhood or adulthood. A surgeon will patch or stitch the atrioventricular septal defect closed, then repair the left sided valve. If the valve leaks too much, it may require replacement with an artificial valve or a valve from a donated organ.
After surgery, patients initially recover in the Evelyn and Daniel M Tabas Cardiac Intensive Care Unit (CICU), where they receive around-the-clock attention from a team of dedicated cardiac critical care medicine specialists and specially trained cardiac nurses. As patients improve, they are moved to the Cardiac Care Unit before ultimately discharged home.
Follow-up care for AVCD
Early years (0-5 years)
As a group, children with complex congenital heart defects who have had open heart surgery as infants are at a higher risk for neurodevelopmental issues when compared to children without congenital heart defects. The Cardiac Center at CHOP created the Cardiac Kids Developmental Follow-up Program to provide evaluation, screening and clinical care for children with complex congenital heart disease who are at risk for neurodevelopmental problems.
Through age 18
A child who has had surgical repair of an atrioventricular canal defect will require life-long care by a cardiologist.
Our pediatric cardiologists follow patients until they are young adults, coordinating care with the primary care physician. Patients will need to carefully follow doctors' advice, including staying on any medications prescribed.
Sometimes children with atrioventricular canal defects experience heart problems later in life, including irregular heartbeat (arrhythmia) and leaky or narrowing valves. Medicine, additional surgery and/or cardiac catheterization may be required.
Into adulthood
At Children’s Hospital of Philadelphia (CHOP), our pediatric cardiologists follow patients until they are young adults and coordinate care with primary care physicians. We can also help with the transition to an adult cardiologist, who has experience working with adult patients with congenital heart disease.
The Philadelphia Adult Congenital Heart Center, a joint program of CHOP and Penn Medicine, meets the unique needs of adults who were born with heart defects.

Patient Outcomes at the Cardiac Center
Children’s Hospital of Philadelphia's pediatric heart surgery survival rates are among the best in the nation.
Resources to help
Cardiac Center Resources
We know that caring for a child with a heart condition can be stressful. To help you find answers to your questions – either before or after visiting the Cardiac Center – we’ve created this list of educational health resources.
Reviewed by Stephanie Fuller, MD
