What is hypospadias?
Hypospadias is a condition that affects the penis. There are three common signs of hypospadias:
- The location of the opening through which a child urinates (urethral meatus) is located at a lower than normal position
- A bend to the penis, typically a downward curve of the penis or forward tilt of the head of the penis
- An incompletely formed foreskin
Despite these findings, children with hypospadias are typically able to empty their bladder at birth without any difficulty and do not experience any pain related to their hypospadias. Some may have a higher chance of developing a hernia or having a testicle which did not fully descend into the scrotum.
Hypospadias is typically diagnosed at birth, but for some it can be noted later in life.
Each year, the Division of Urology at Children's Hospital of Philadelphia (CHOP) evaluates and treats patients with hypospadias at more than 1,200 clinic visits. This includes patients who have had prior surgeries and those who have never undergone a procedure.
Treatment will depend on the degree of your child’s hypospadias, which will be determined upon evaluation by a pediatric urologist. At CHOP, the evaluation for hypospadias will include an exam to identify the location of the urethral opening, the degree of curvature, and the appearance of the foreskin.
Some children will have a minor hypospadias and may not need surgery. For others, we will discuss potential concerns such as deflection of the urinary stream and curvature of the penis with erections, and consider these factors when determining the best approach to correcting their hypospadias.
Signs and symptoms of hypospadias
Location of urethral opening
The most common sign of hypospadias is when the location of the opening through which a child urinates (the urethral meatus) is not present at its typical location at the tip of the penis.
In a child born with hypospadias, the urethral meatus can be located just below the tip of the penis (glanular or coronal), the shaft of the penis (penile), the scrotum (scrotal), and occasionally below the scrotum (perineal).
This illustration depicts the many locations where the urethral meatus can appear in hypospadias. Each child has only one opening through which they urinate.
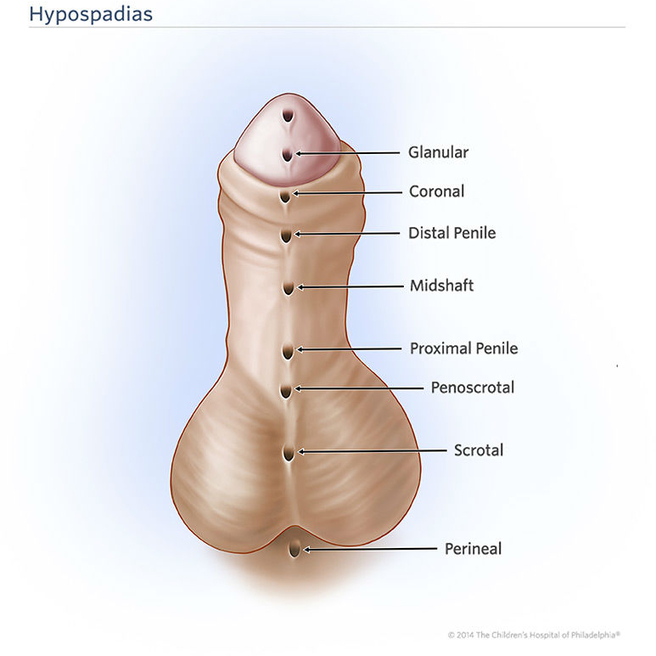
The milder form of hypospadias, where the opening is closer to the tip of the penis (glanular or coronal), occurs in the majority of cases (75% to 80%). The more severe form of hypospadias, when the opening is further down (penoscrotal, scrotal or perineal), occurs in 20% to 25%.
In addition to the urethral opening being located in a different location than normal, the head of the penis (or glans) is often not fused together. This is referred to as an open glans. Closure of the urethra and the head of the penis is a common step in hypospadias repair.

Curved penis
The second thing that parents may notice is that the penis is not straight but instead has a curve to it. This curvature is sometimes referred to as chordee. The penis bends in a forward direction which can make it appear shorter than it really is. The skin can also appear underdeveloped on the front of the penis.
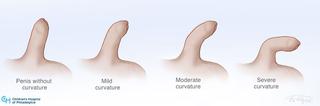
The amount of bend can range in degree from a slight tilt of the head of the penis to a severe bend of the entire penis. This bend can be corrected with surgery. Based on studies done at Children’s Hospital of Philadelphia, if the curvature is severe, this may be best corrected with two surgeries. The first procedure corrects the bend while the second creates the new urethra.
Incomplete foreskin
Another finding typically associated with hypospadias is an incompletely formed foreskin. The foreskin forms on the back of the head of the penis but does not completely join on the front side of the glans. This can make your child look partially circumcised.
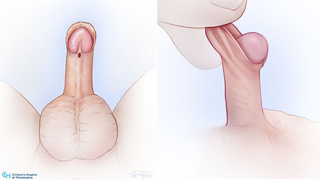
A small percentage (approximately 5%) have hypospadias with a completely formed foreskin. We typically recommend delaying newborn circumcision until after evaluation by a pediatric urologist.
Causes of hypospadias
While we know how to surgically correct hypospadias, we know less about why it occurs.
Hypospadias occurs fairly frequently and is present in approximately 1 out of every 150 to 300 newborn boys. It is a congenital anomaly, meaning it is present at birth.
The penis is nearly fully formed by the fifth month of pregnancy. Hypospadias is thought to occur as a result of a disruption or stoppage of normal penile development. Although the exact cause of hypospadias is unknown, there are several potential risk factors:
- Hormones: The formation of the penis and foreskin are dependent upon hormones such as testosterone. There is some thought that hormones present in the environment have a negative impact on testosterone levels and contribute to hypospadias development.
- Genetics: Some individuals are more likely to have hypospadias if their brother or father has the condition.
- Reproductive technology: There is a higher risk of hypospadias based on the type of conception (such as use of in-vitro fertilization).
- Prematurity: Babies with a low birth weight who are born premature have a higher chance of having hypospadias.
Although these have all been identified as risk factors for hypospadias, it is more common for hypospadias to occur without an identifiable cause.
Evaluation and diagnosis of hypospadias
When you make an appointment at Children’s Hospital of Philadelphia for a hypospadias evaluation, you can expect our pediatric urologists to ask questions about the following:
- Your child’s medical history
- Whether any medication was taken to get pregnant or during the pregnancy
- Whether you have noticed any curvature to the penis. At a young age, boys will get erections because of a full bladder. You may notice this while they are in the bath or you are changing their diaper.
- The direction and strength of the urinary stream
- Whether your child has been circumcised
During your first visit, we will examine your child to identify the location of the urethral meatus, assess for any curvature of the penis, and determine the degree of hypospadias.
As part of the exam, we may take a few measurements — such as the length of the penis and the size of the head of the penis — to help determine the best treatment options.
The rest of the consultation will be spent discussing whether surgery is the right treatment option for your child, and if so, what type of surgery is recommended.
Hypospadias treatment
Surgery to repair hypospadias involves rebuilding the urethra so that it extends into the head of the penis as well as straightening any curvature of the penis.
If hypospadias repair surgery is indicated, we typically recommend repair between 6 and 18 months of age. This is a time period during which children are less aware of and less interested in their genitalia, which leads to an easier recovery.
Some children will require surgery outside of this time frame. Our team has extensive experience treating patients of all ages with hypospadias. We perform approximately 300 hypospadias surgeries each year.
It is important to note that not all individuals require surgery for hypospadias. When there is no penile curvature and the urethral opening is near the tip of the penis there may be minimal benefit to surgery.
Preparing for hypospadias surgery
At birth, we typically advise against circumcision, as the extra foreskin may be needed at the time of the surgical repair.
Hypospadias surgery is usually done on an outpatient basis and rarely requires an overnight hospital stay.
For some patients we recommend one or two pre-operative injections of testosterone to help increase the size of the penis prior to surgery to help improve surgical outcomes. If we feel that the patient is a candidate for this, we will discuss the timing and details of the injections and give you a prescription for the testosterone at the time of your child’s office visit.
Types of hypospadias repair
There are many different surgical approaches used to correct hypospadias. The method of hypospadias repair depends on the surgeon’s assessment, which includes the location of the meatus, the degree of curvature of the penis, the quality of the penile skin, and whether there has been any prior surgery to the penis. The exact approach is typically best decided at the time of the operation but the options and approach will be reviewed with the family in the office visit.
Our techniques have been refined over the years to significantly improve the surgical outcomes of our patients with hypospadias. We use a variety of techniques to obtain the optimal outcomes based upon your child’s anatomy and surgical history.
For instance, a two-stage repair is often used for patients with severe curvature as this has proven to be a more effective approach than a single operation. We will discuss the specifics of the operation with you during your child’s surgical consultation.
Questions about Hypospadias repair?
Find answers to questions that are often asked regarding hypospadias surgery. This is general medical information and not specific medical advice for any individual patient.
What to expect after hypospadias surgery
During surgery, the surgeon may place a temporary drainage catheter (tube) in the urethra to divert the urine in order to help the healing process.
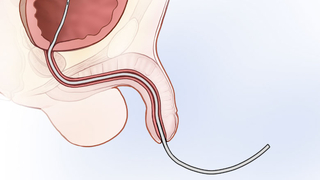
The catheter may be stitched to the head of penis to keep it in place. The catheter is typically removed in the urology clinic one to two weeks after surgery. The remainder of the stitches used during surgery dissolve on their own and will not have to be removed.
Your child will most likely have a bandage on the penis for several days after surgery to help prevent any bleeding. We typically have parents remove this at home by soaking the penis in the tub, which releases the bandage.
It is common for the penis to be swollen, red and bruised for the first several days to weeks as it heals following surgery. After the bandage is removed, parents will be instructed to apply petroleum jelly to the penile area with each diaper change to help the healing process. We often have parents email pictures or follow up in the office to verify that the healing process is progressing nicely.
View our hypospadias resources for more information about caring for your child at home after hypospadias surgery.
Hypospadias surgery outcomes
Hypospadias surgery is complex. The risk of having a complication or issue after the repair depends on the degree of hypospadias. Published complication rates (the need for an additional, unplanned procedure) for distal (mild) hypospadias range from 10% to 20% and up to 70% for proximal (severe) hypospadias.
The most common complication after hypospadias repair surgery is a leak in the new urethral tube (a urethrocutaneous fistula). The newly created urethral opening can narrow with time, a condition called meatal stenosis.
In more severe cases of hypospadias, an outpouching in the urethra (urethral diverticulum) and persistent penile curvature can occur after repair.
Some children with complex hypospadias may require more extensive surgical reconstruction. We have expertise in working with babies with more complex cases of hypospadias, including those who have undergone several prior repairs with a less than satisfactory result.
Whether your child requires more than one procedure or a single repair, our team of pediatric urology experts is prepared to provide whatever level of care is needed. Our comprehensive team includes pediatric urologic surgeons with years of experience operating on all types of hypospadias, and expertise performing all the different surgical techniques that may be used. We receive referrals from all over the world to help these children and can offer a second opinion regardless of the distance from CHOP.
Our main focus is to achieve the best outcome for your child, something our surgical team can typically do in one procedure. We continue to seek out innovative techniques to improve surgical outcomes and provide the best results for our hypospadias patients. For example, we now use microscope magnification for some procedures, which allows us to see the small, delicate tissues at 10 times the size of the normal eye. We are also currently investigating potential risk factors for complications after hypospadias repair in order to improve care and better prepare families for what lies ahead.
Follow-up care for hypospadias
Recent research suggests that long-term follow-up extending into puberty is important for hypospadias patients. We will monitor your child with periodic visits to ensure that the goals of surgery are met: They urinate (void) normally, have straight erections, and the penis has an appropriate cosmetic appearance.
Follow-up visits may include having your child urinate and asking questions about erections (when age appropriate). We realize that this is potentially an embarrassing process and will respect the patient’s privacy in an appropriate fashion.
Our dedicated team includes a pediatric psychologist who is available to work with families as needed. This resource can be helpful as children approach potty-training age, if a child requires additional procedures and needs tools to help them cope, and to work on issues related to body image as they age.
Studies have shown that the adolescent age group is at risk for potentially conflicting feelings about their diagnosis of hypospadias, particularly as they enter puberty. We are available to support patients and their families every step of the way.
For patients with complex urologic conditions like hypospadias, it is especially important that the care they receive remains effective and streamlined. As your child nears adulthood, our dedicated Urology Transitional Care Program — a collaborative effort between CHOP and the Hospital of the University of Pennsylvania (HUP) — can help you and your child prepare for the transition from pediatric to adult medical care and support you through this process.
Why choose CHOP for hypospadias treatment
We place a great amount of emphasis on delivering the best possible care to patients with hypospadias. This involves not only evaluation, surgery and follow-up care, but also constant assessment of our outcomes and areas for improvement.
We have an active research team in place focused on a few core values and goals:
- Improving surgical outcomes: We are active in national meetings and committees designed to identify risk factors and methods to decrease them. Our efforts include identifying the ideal approach to correct penile curvature and how best to approach proximal or more severe hypospadias.
- Psychosocial support: We have identified the need for extending follow-up into the adolescent period in order to provide optimal care for our patients. We are incorporating a patient and parental survey into our follow-up appointments to assess for any psychological impact that hypospadias has on our patients.
- Improving care for hypospadias patients worldwide: We are amongst the world leaders in management of hypospadias. Several of our surgeons lead committees focused on coordinating national research efforts to improve hypospadias. We also perform hypospadias surgery around the world, teaching our techniques to surgeons in other countries. In October 2019, Children’s Hospital of Philadelphia will be hosting an international meeting for the Hypospadias International Society. This event is specifically designed to improve the care of patients with hypospadias throughout the world.
Reviewed by: Division of Urology
Date: April 2019
Resources to help
Hypospadias Resources
Division of Urology Resources
Caring for a child with an illness or injury can be overwhelming. We have resources to help you find answers to your questions and feel confident in the care you are providing your child.

