What is thoracic insufficiency syndrome?
Thoracic insufficiency syndrome is a complex condition that involves chest wall deformities that affect normal breathing and lung growth. In most cases, children with thoracic insufficiency syndrome are also born with congenital spinal disorders, such as scoliosis.
Thoracic insufficiency syndrome is the inability of the thorax to support normal breathing or lung growth. The thorax is the part of your child’s body between the neck and abdomen that includes the spine, ribs and sternum (breastbone). In normal developing children, lung growth parallels chest and spine growth. In children with thoracic insufficiency syndrome, lung growth is limited by rib deformities and spinal curves.
Children with thoracic insufficiency syndrome cannot support normal breathing or lung growth. As they grow, their rib cage and spine do not keep pace. As a result, their chest wall becomes deformed (sunken) and the children may become dependent on nasal oxygen or ventilator support to breathe.
Orthopedic surgeons at the Wyss/Campbell Center for Thoracic Insufficiency Syndrome at CHOP were the first to identify thoracic insufficiency syndrome as a disease that required specialized care and treatment. Our experts invented the vertical expandable prosthetic titanium rib (VEPTR) device, the first FDA-approved device for treatment of thoracic insufficiency syndrome.
This revolutionary implant allows a surgeon to expand a child’s rib cage surgically to nurture lung growth and correct spinal deformity. Then, the gains in chest volume are continued by further expanding the device in outpatient surgery twice a year.
Causes
Thoracic insufficiency syndrome is a rare disease that affects fewer than 4,000 children in the United States. If your child has this progressive, congenital condition, she was born with the disorder but it will continue to worsen as she grows.
The most common cause of thoracic insufficiency syndrome occurs when a baby is born with progressive scoliosis (spinal curvature) and severe rib fusion.
Other causes of thoracic insufficiency syndrome include physical deformities and syndromes including:
- Congenital absence of ribs
- Early-onset scoliosis
- A narrow chest and rib cage, including these conditions:
- Cerebrocostomandibular syndrome
- Jeune syndrome
- Escobar
- Arthrogryposis
- Spinal muscular atrophy (SMA)
- A short chest and rib cage, including these conditions:
- Jarcho-Levin syndrome (spondylocostal dysplasia)
- Excessive kyphosis
- Pierre-Robin syndrome
- Other conditions that can affect lung growth and health, such as:
- Goldenhar syndrome
- Spina bifida
- VATER syndrome
Signs and symptoms
Symptoms of thoracic insufficiency syndrome vary from child to child, and can be related to other medical conditions and genetic syndromes.
Symptoms can include:
- Spinal deformities, such as scoliosis (sideways curve) and kyphosis (hunchback)
- Severe rib fusion
- Congenital absence of ribs
- Shortened body trunk and rib cage
- Narrow body trunk and rib cage
Testing and diagnosis
Thoracic insufficiency syndrome is diagnosed in very young children by a pediatric orthopedic surgeon or pediatric pulmonologist. The child usually will be less than 5 years old and always less than 10 years old.
At the Wyss/Campbell Center for Thoracic Insufficiency Syndrome at Children’s Hospital of Philadelphia (CHOP), we fully evaluate pediatric patients with a combination of tests and consultations with our team of orthopedic surgeons, general surgeons, radiologists, pulmonologists, neurologists, geneticists, anesthesiologists, bioengineers, nurses and other clinical specialists.
Diagnostic evaluation begins with a thorough medical history and physical examination of your child. We use a variety of diagnostic tests to diagnose thoracic insufficiency syndrome and possible complications, including:
- Pulmonary function tests, which measure how well your child's lungs take in and release air and how well they move gases, such as oxygen, from the atmosphere into the body’s circulation. These tests include spirometry, whole body plethysmography, single and multiple breath nitrogen washout, carbon monoxide diffusion capacity, respiratory muscle strength and lung compliance.
- Dynamic lung MRI, which uses a combination of large magnets, radiofrequencies and a computer to reveal the movement of the lungs and the breathing muscles. The dynamic MRI allows clinicians to better understand each child’s thoracic insufficiency syndrome.
- EOS imaging, an imaging technology that creates 3-dimensional models from two planar images. EOS images are taken while the child is in an upright or standing position, enabling improved diagnosis due to weight-bearing positioning.
- X-rays, which produce images of bones of the neck, spine, and scapula (shoulder blades).
- Magnetic resonance imaging (MRI), which uses a combination of large magnets, radiofrequencies and a computer to produce detailed images of organs and structures within the body.
- Genetic testing, in which a sample of your child’s saliva is used to identify your child’s DNA and possible genetic conditions or syndromes.
All of these medical tests allow clinicians to gather a full picture of your child’s medical health and help in determining an individualized care plan.
Each patient with thoracic insufficiency syndrome is discussed in detail at our Center’s bimonthly team meetings. The goal of these clinical discussions is to define your child’s condition from each consultant’s area of expertise, and to arrive at a consensus about the best treatment options possible for your child.
Treatments
Our team considers all possible treatment options for children with thoracic insufficiency syndrome, but the most commonly used treatment is the vertical expandable prosthetic titanium rib (VEPTR), a device that expands a child’s chest, stabilizes spine curvatures and is lengthened with periodic outpatient expansions to keep up with the growth of the child.
Our core team of pediatric orthopedists, general surgeons, pulmonologists, advanced practice nurses and other experts provide complete care for children with thoracic insufficiency syndrome — from our unique multidisciplinary evaluation system to implant surgery, expansion surgeries and long-term supportive follow-up.
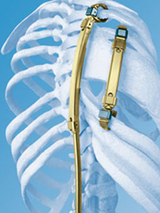
The Wyss/Campbell Center for Thoracic Insufficiency Syndrome at Children’s Hospital of Philadelphia is one of only a few institutions in the United States that offers an FDA-approved treatment for thoracic insufficiency syndrome. The treatment involves use of a special titanium implant called a vertical expandable prosthetic titanium rib (VEPTR).
In VEPTR surgery, the expandable titanium ribs are implanted into a child's back and chest, and anchored to the spine and ribs. The VEPTR was designed to allow orthopedic surgeons to expand the device at regular intervals in outpatient surgery.
The Center uses a unique multidisciplinary approach to provide comprehensive care for patients with rare scoliosis, fused or absent ribs, and hypoplastic thorax, complementing the longstanding early-onset scoliosis program at CHOP.

Why Choose CHOP for TIS Care
Children’s Hospital of Philadelphia offers world-class care for children with thoracic insufficiency syndrome.
Follow-up care
After the initial surgery to place the vertical expandable prosthetic titanium rib (VEPTR), your child will receive follow-up care in our center on a regular basis. We will monitor your child's progress and schedule additional surgeries about twice a year to expand the device to accommodate your child's growth.
Expansion surgeries
VEPTR expansion is a short surgical procedure involving an approximately 1-inch incision. Typically, children spend one night in the Hospital on a medical/surgical floor and are discharged the following day.
Final surgery and "graduation"
When your child's spine and chest have matured and the titanium rib has been fully expanded — at approximately 10 to 16 years old — your child will "graduate" and a final surgery will be scheduled.
During this procedure, the spine-supporting expandable titanium rib will be removed and a spinal fusion will be performed. In a spinal fusion, your child's abnormal curved spinal bones are realigned, fused together and metal implants may be inserted to further stabilize the spine. Spinal fusion is often needed to better support a child's spine and minimize the effects of scoliosis and other spine-curving disorders.
This final step in your child's journey generally requires several days of recovery in the Hospital. Our multidisciplinary team continues to monitor your child and assess other health issues that your child may have.
In rare cases, such as if your child has missing ribs; a VEPTR device may be left in place permanently to help your child retain chest wall form and function.
Outlook
Outcomes for patients undergoing VEPTR surgery are generally good. The expandable titanium rib allows the lungs of patients with thoracic insufficiency syndrome to grow as your child grows. Spinal fusion makes the spine correction permanent.
Patients who receive treatment for thoracic insufficiency syndrome should continue to be monitored by an orthopedic physician at regular intervals — even after spinal fusion. We will help transition your child's care to appropriate specialists when they become young adults, generally between the ages of 18 and 21.
More experience with thoracic insufficiency syndrome and VEPTR as a treatment option are needed to provide more complete answers about long-term outcomes for children with thoracic insufficiency syndrome. We hope to learn more about patients' quality of life, comorbidities and survival.
Research is underway to help clinicians better understand what causes thoracic insufficiency syndrome, what normal lung growth and capacity is, and how patients with thoracic insufficiency compare.
Resources to help
Wyss/Campbell Center for Thoracic Insufficiency Syndrome Resources
We have created resources – including videos and websites – to help you find answers to your questions and feel confident with the care you are providing your child.


