Brachial plexus birth injury (BPBI) is an upper extremity paralysis that occurs from a traction injury to the brachial plexus during birth. Research performed at Children’s Hospital of Philadelphia (CHOP) suggests that shoulder dystocia and macrosomia are the largest risk factors, but breech delivery, instrumented delivery and birth hypoxia also independently increase the risk of injury (1). The incidence of BPBI in the United States decreased from 1.7 to 0.9 per 1,000 live births from 1997 to 2012 in the setting of decreasing rates of macrosomia as well as increasing rates of multiparity and cesarean section (1).
Approximately 10% to 30% of children with BPBI have residual neurologic deficits with an associated impact on upper limb function. Management of BPBI with a multidisciplinary team allows optimization of functional recovery while avoiding unnecessary intervention. At CHOP, this team is directed by orthopaedic surgeon Apurva Shah, MD, MBA, and neurologist Sabrina Yum, MD, but also includes neurosurgery, plastic surgery and occupational therapy.
For infants with BPBI, early occupational therapy should be initiated with a focus on passive range of motion. The need for microsurgical reconstruction of the brachial plexus can be predicted based on early physical examination findings and is generally performed at 3 to 9 months of age when necessary.
The majority of children with residual neurologic deficits will develop associated glenohumeral dysplasia. These children may require secondary procedures including botulinum toxin injection, shoulder tendon transfers and humeral derotational osteotomy.
We have selected a recent case to highlight how our multidisciplinary team functions.
Clinical scenario
A boy was delivered vaginally at 39 weeks gestation with a birthweight of 3.66 kilograms. Delivery was complicated by a left shoulder dystocia and resulted in a left upper trunk BPBI and right humeral shaft fracture, which was immobilized for four weeks in a soft wrap. The diagnosis of left BPBI was confirmed by our team’s neurologist and orthopaedic surgeon.
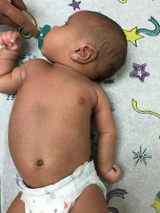
At initial presentation, there was no deltoid or biceps activation on the left (Figure 1). The patient did demonstrate antigravity elbow, wrist and digital extension. Full passive shoulder range of motion was noted. The patient was followed by the multidisciplinary team monthly for serial examinations. Return of biceps and deltoid function was evident at 3 months of age.
Figure 1: Initial presentation of a newborn male with a left upper trunk brachial plexus birth injury (Narakas type 1, Erb’s palsy). The photograph demonstrates the classic “waiter’s tip” positioning with the shoulder in a position of adduction and internal rotation, the elbow in extension, and the wrist in flexion.
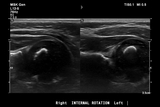
Clinical examination revealed a worsening shoulder internal rotation contracture between 2 and 5 months of age, with no evidence of active shoulder external rotation. The patient was referred for a shoulder ultrasound (US) examination at 5 months of age that revealed a posterior glenohumeral dislocation (Figure 2). Instead of surgery, the medical team recommended botulinum toxin type A injection of the subscapularis, pectoralis major and teres major by neurology along with closed reduction and shoulder external rotation spica casting by orthopaedic surgery.
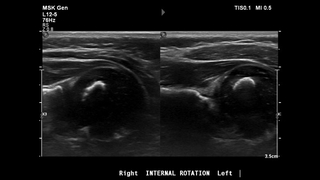
Figures 2: Ultrasound assessment of glenohumeral dysplasia. The right shoulder (image on left) demonstrates a normal alpha angle without posterior humeral head dislocation. In the left shoulder (image on right), there is an increased alpha angle and more than 50% of the humeral head is displaced posterior to the axis of the scapula, both of which suggest shoulder dislocation.
Treatment outcomes
The procedure was completed at 5 months of age. The cast was removed four weeks thereafter and the patient was transitioned to a custom nighttime SupER (forearm supination, shoulder external rotation) orthotic with weekly occupational therapy to maximize strength of posterior shoulder and scapular muscles.
Repeat US three months after the procedure revealed relocation of the shoulder joint. Significantly improved passive and active shoulder external rotation were also noted at this time.
The patient will be followed by the multidisciplinary team periodically throughout childhood to monitor progress. A shoulder MRI may be indicated in the future to better characterize residual glenohumeral dysplasia and determine the potential need for secondary shoulder surgery.
This case highlights the value of a multidisciplinary team to manage complex conditions like BPBI. The diagnosis of shoulder dislocation was detected with a highly-trained pediatric musculoskeletal radiology team that has great expertise in shoulder ultrasonography. With botulinum injection and a closed shoulder reduction, the team was able to relocate the baby’s shoulder while avoiding an invasive surgical procedure.
References
- DeFrancesco CJ, Shah DK, Rogers BH, Shah AS. The epidemiology of brachial plexus birth palsy in the United States: Declining incidence and evolving risk factors. J Pediatr Orthop. 2019;39(2):e134-e140.
Figure Legends
- Figure 1: Initial presentation of a newborn male with a left upper trunk brachial plexus birth injury (Narakas type 1, Erb’s palsy). The photograph demonstrates the classic “waiter’s tip” positioning with the shoulder in a position of adduction and internal rotation, the elbow in extension, and the wrist in flexion.
- Figures 2: Ultrasound assessment of glenohumeral dysplasia. The right shoulder (image on left) demonstrates a normal alpha angle without posterior humeral head dislocation. In the left shoulder (image on right), there is an increased alpha angle and more than 50% of the humeral head is displaced posterior to the axis of the scapula, both of which suggest shoulder dislocation.
Featured in this article
Specialties & Programs
Brachial plexus birth injury (BPBI) is an upper extremity paralysis that occurs from a traction injury to the brachial plexus during birth. Research performed at Children’s Hospital of Philadelphia (CHOP) suggests that shoulder dystocia and macrosomia are the largest risk factors, but breech delivery, instrumented delivery and birth hypoxia also independently increase the risk of injury (1). The incidence of BPBI in the United States decreased from 1.7 to 0.9 per 1,000 live births from 1997 to 2012 in the setting of decreasing rates of macrosomia as well as increasing rates of multiparity and cesarean section (1).
Approximately 10% to 30% of children with BPBI have residual neurologic deficits with an associated impact on upper limb function. Management of BPBI with a multidisciplinary team allows optimization of functional recovery while avoiding unnecessary intervention. At CHOP, this team is directed by orthopaedic surgeon Apurva Shah, MD, MBA, and neurologist Sabrina Yum, MD, but also includes neurosurgery, plastic surgery and occupational therapy.
For infants with BPBI, early occupational therapy should be initiated with a focus on passive range of motion. The need for microsurgical reconstruction of the brachial plexus can be predicted based on early physical examination findings and is generally performed at 3 to 9 months of age when necessary.
The majority of children with residual neurologic deficits will develop associated glenohumeral dysplasia. These children may require secondary procedures including botulinum toxin injection, shoulder tendon transfers and humeral derotational osteotomy.
We have selected a recent case to highlight how our multidisciplinary team functions.
Clinical scenario
A boy was delivered vaginally at 39 weeks gestation with a birthweight of 3.66 kilograms. Delivery was complicated by a left shoulder dystocia and resulted in a left upper trunk BPBI and right humeral shaft fracture, which was immobilized for four weeks in a soft wrap. The diagnosis of left BPBI was confirmed by our team’s neurologist and orthopaedic surgeon.

At initial presentation, there was no deltoid or biceps activation on the left (Figure 1). The patient did demonstrate antigravity elbow, wrist and digital extension. Full passive shoulder range of motion was noted. The patient was followed by the multidisciplinary team monthly for serial examinations. Return of biceps and deltoid function was evident at 3 months of age.
Figure 1: Initial presentation of a newborn male with a left upper trunk brachial plexus birth injury (Narakas type 1, Erb’s palsy). The photograph demonstrates the classic “waiter’s tip” positioning with the shoulder in a position of adduction and internal rotation, the elbow in extension, and the wrist in flexion.
Clinical examination revealed a worsening shoulder internal rotation contracture between 2 and 5 months of age, with no evidence of active shoulder external rotation. The patient was referred for a shoulder ultrasound (US) examination at 5 months of age that revealed a posterior glenohumeral dislocation (Figure 2). Instead of surgery, the medical team recommended botulinum toxin type A injection of the subscapularis, pectoralis major and teres major by neurology along with closed reduction and shoulder external rotation spica casting by orthopaedic surgery.

Figures 2: Ultrasound assessment of glenohumeral dysplasia. The right shoulder (image on left) demonstrates a normal alpha angle without posterior humeral head dislocation. In the left shoulder (image on right), there is an increased alpha angle and more than 50% of the humeral head is displaced posterior to the axis of the scapula, both of which suggest shoulder dislocation.
Treatment outcomes
The procedure was completed at 5 months of age. The cast was removed four weeks thereafter and the patient was transitioned to a custom nighttime SupER (forearm supination, shoulder external rotation) orthotic with weekly occupational therapy to maximize strength of posterior shoulder and scapular muscles.
Repeat US three months after the procedure revealed relocation of the shoulder joint. Significantly improved passive and active shoulder external rotation were also noted at this time.
The patient will be followed by the multidisciplinary team periodically throughout childhood to monitor progress. A shoulder MRI may be indicated in the future to better characterize residual glenohumeral dysplasia and determine the potential need for secondary shoulder surgery.
This case highlights the value of a multidisciplinary team to manage complex conditions like BPBI. The diagnosis of shoulder dislocation was detected with a highly-trained pediatric musculoskeletal radiology team that has great expertise in shoulder ultrasonography. With botulinum injection and a closed shoulder reduction, the team was able to relocate the baby’s shoulder while avoiding an invasive surgical procedure.
References
- DeFrancesco CJ, Shah DK, Rogers BH, Shah AS. The epidemiology of brachial plexus birth palsy in the United States: Declining incidence and evolving risk factors. J Pediatr Orthop. 2019;39(2):e134-e140.
Figure Legends
- Figure 1: Initial presentation of a newborn male with a left upper trunk brachial plexus birth injury (Narakas type 1, Erb’s palsy). The photograph demonstrates the classic “waiter’s tip” positioning with the shoulder in a position of adduction and internal rotation, the elbow in extension, and the wrist in flexion.
- Figures 2: Ultrasound assessment of glenohumeral dysplasia. The right shoulder (image on left) demonstrates a normal alpha angle without posterior humeral head dislocation. In the left shoulder (image on right), there is an increased alpha angle and more than 50% of the humeral head is displaced posterior to the axis of the scapula, both of which suggest shoulder dislocation.
Contact us
Brachial Plexus Injury Program