Cleft lip with or without cleft palate is the most common craniofacial anomaly detected on routine prenatal screening ultrasound. Failed fusion of the developing primary and secondary palates leads to a variety of orofacial clefts, with the severity ranging from a subtle unilateral incomplete cleft to a more complex bilateral cleft that extends into the nasal floor. Although cleft lip with or without cleft palate is often isolated, craniofacial clefts may be associated with other anomalies in 30% of cases.
In each case of suspected orofacial cleft, the primary goals at our institution are determining whether the defect is unilateral or bilateral, whether the defect is confined to the lip or involves the palate, and whether the defect is isolated or associated with other congenital anomalies. Ultrasound and MRI are complementary modalities in the assessment of all facial clefts, and patients referred to our Center for Fetal Diagnosis and Treatment typically undergo both examinations.
Two-dimensional ultrasound readily depicts most cases of cleft lip and is often superior to MRI in evaluating small or less severe clefts, especially when fetal motion degrades MR image quality. Three-dimensional ultrasound surface renderings are routinely obtained as they help establish whether the defect is complete and extends to the naris, or incomplete and spares the naris. These surface renderings are also valuable in visually conveying the cleft to the parents. While maternal habitus may make sonographic assessment challenging, recent advances in transducer technology now allow for both soundwave penetration and superb detailed anatomic resolution. These advances, as well as advances in 3-D reconstructions, have similarly improved assessment of the palate.
Knowing whether the cleft involves the palate is another important component in preparing parents for what to expect with respect to postnatal surgical management. MRI is especially valuable in assessing both the hard and soft palate and traditionally has been superior to ultrasound in detailing defects of the palate. MRI is also helpful in evaluating cases where fetal positioning and oligohydramnios limit sonographic assessment.
The last component of evaluation at our hospital is to establish whether the defect is isolated or associated with other anomalies. While less common, cleft lip with or without palate may be seen in aneuploidy and multiple syndromes. Subtle brain malformations may also occur in high-resolution ultrasound and fetal MRI at our center ensures detection of any other associated anomalies that may affect final diagnosis and prognosis.
A prenatal diagnosis of cleft lip with or without palate can be difficult for expecting parents to receive. Members of our fetal imaging team make every effort to provide the maternal-fetal medicine specialists and plastic surgeons with the most comprehensive assessment of the facial cleft so that patients receive the most accurate counseling and preparation for postnatal treatment.
27-week fetus with right cleft lip and palate and left cleft lip
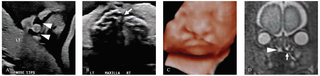
A. Coronal image of the nose and lips demonstrates bilateral cleft lips (arrowheads). B. Transverse image through the maxilla reveals a unilateral defect in the right maxilla and hard palate (arrow). C. Three-dimensional ultrasound surface rendering depicts the bilateral cleft lip with extension to the nares. D. Coronal fast spin echo T2-weighted MR image through the hard palate demonstrates fluid signal extending through the cleft in the right palate (arrowhead) into the nasal cavity and the intact hard palate on the contralateral side (arrow).
References
Radiology of cleft lip and palate: Imaging for the prenatal period and throughout life. Abramson ZR, Peacock ZS, Cohen HL, Choudhri AF. Radiographics. 2015;35(7):2053-2063.
Prenatal diagnosis of cleft lip/palate: The surface rendered oro-palatal (SROP) view of the fetal lips and palate, a tool to improve information-sharing within the orofacial team and with the parents. Levaillant JM, Nicot R, Benouaiche L, Couly G, Rotten D. J Craniomaxillofac Surg. 2016;44(7):835-842.
Featured in this article
Specialties & Programs
Cleft lip with or without cleft palate is the most common craniofacial anomaly detected on routine prenatal screening ultrasound. Failed fusion of the developing primary and secondary palates leads to a variety of orofacial clefts, with the severity ranging from a subtle unilateral incomplete cleft to a more complex bilateral cleft that extends into the nasal floor. Although cleft lip with or without cleft palate is often isolated, craniofacial clefts may be associated with other anomalies in 30% of cases.
In each case of suspected orofacial cleft, the primary goals at our institution are determining whether the defect is unilateral or bilateral, whether the defect is confined to the lip or involves the palate, and whether the defect is isolated or associated with other congenital anomalies. Ultrasound and MRI are complementary modalities in the assessment of all facial clefts, and patients referred to our Center for Fetal Diagnosis and Treatment typically undergo both examinations.
Two-dimensional ultrasound readily depicts most cases of cleft lip and is often superior to MRI in evaluating small or less severe clefts, especially when fetal motion degrades MR image quality. Three-dimensional ultrasound surface renderings are routinely obtained as they help establish whether the defect is complete and extends to the naris, or incomplete and spares the naris. These surface renderings are also valuable in visually conveying the cleft to the parents. While maternal habitus may make sonographic assessment challenging, recent advances in transducer technology now allow for both soundwave penetration and superb detailed anatomic resolution. These advances, as well as advances in 3-D reconstructions, have similarly improved assessment of the palate.
Knowing whether the cleft involves the palate is another important component in preparing parents for what to expect with respect to postnatal surgical management. MRI is especially valuable in assessing both the hard and soft palate and traditionally has been superior to ultrasound in detailing defects of the palate. MRI is also helpful in evaluating cases where fetal positioning and oligohydramnios limit sonographic assessment.
The last component of evaluation at our hospital is to establish whether the defect is isolated or associated with other anomalies. While less common, cleft lip with or without palate may be seen in aneuploidy and multiple syndromes. Subtle brain malformations may also occur in high-resolution ultrasound and fetal MRI at our center ensures detection of any other associated anomalies that may affect final diagnosis and prognosis.
A prenatal diagnosis of cleft lip with or without palate can be difficult for expecting parents to receive. Members of our fetal imaging team make every effort to provide the maternal-fetal medicine specialists and plastic surgeons with the most comprehensive assessment of the facial cleft so that patients receive the most accurate counseling and preparation for postnatal treatment.
27-week fetus with right cleft lip and palate and left cleft lip

A. Coronal image of the nose and lips demonstrates bilateral cleft lips (arrowheads). B. Transverse image through the maxilla reveals a unilateral defect in the right maxilla and hard palate (arrow). C. Three-dimensional ultrasound surface rendering depicts the bilateral cleft lip with extension to the nares. D. Coronal fast spin echo T2-weighted MR image through the hard palate demonstrates fluid signal extending through the cleft in the right palate (arrowhead) into the nasal cavity and the intact hard palate on the contralateral side (arrow).
References
Radiology of cleft lip and palate: Imaging for the prenatal period and throughout life. Abramson ZR, Peacock ZS, Cohen HL, Choudhri AF. Radiographics. 2015;35(7):2053-2063.
Prenatal diagnosis of cleft lip/palate: The surface rendered oro-palatal (SROP) view of the fetal lips and palate, a tool to improve information-sharing within the orofacial team and with the parents. Levaillant JM, Nicot R, Benouaiche L, Couly G, Rotten D. J Craniomaxillofac Surg. 2016;44(7):835-842.
Contact us
Richard D. Wood Jr. Center for Fetal Diagnosis and Treatment