Every year, more than 23,000 children and teens experience a sudden cardiac arrest (SCA) in the U.S. Many of these cases result in death but can be prevented if children and parents recognize the early warning signs of SCA and seek medical attention before a crisis occurs.
Sudden cardiac arrest occurs when the heart suddenly and unexpectedly stops beating due to an abnormality in its electrical pulses. This abnormal rhythm can result in rapid quivering of the heart (ventricular fibrillation) or no heartbeat at all (asystole).
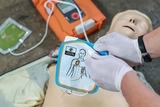
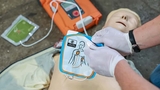
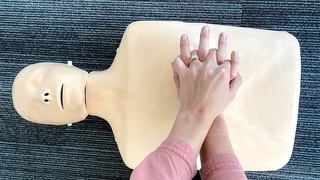
A child who experiences a sudden cardiac arrest loses consciousness, stops breathing or gasps for breath and becomes unresponsive, possibly with shaking (seizure-like) movement. CPR and use of an automated external defibrillator (AED) within two to three minutes of the event can prevent an interruption in blood flow to the brain.
SCA warning signs and symptoms
In as many as half of all cases of sudden cardiac arrests, warning signs and symptoms are present beforehand. But too often they are ignored or misunderstood. Parents and children should be aware of these signs and symptoms and seek medical help immediately when they occur.
Victoria Vetter, MD, MPH, a cardiologist in the Cardiac Center and Medical Director of the Youth Heart Watch program at Children’s Hospital of Philadelphia (CHOP), and Lindsey Flanagan, MPH, program coordinator of the Youth Heart Watch program, detail the warning signs and symptoms of sudden cardiac arrest:
- Racing heart rate or heart palpitations
- Dizziness or lightheadedness especially with exercise
- Repeated unexplained fainting
- Fainting when excited, startled, during exercise or right after exercise
- Seizures during or immediately after exercise
- Chest pain or discomfort with exercise
- Excessive shortness of breath or unusual fatigue during exercise (not related to asthma)
Additionally, there are certain factors or genetic predispositions that can increase an individual's risk of SCA — whether they have symptoms or not. These include:
- A family member with unexplained recurrent fainting or seizures
- A family member who died suddenly before age 50 or a family history of sudden unexplained infant death, drowning, or unexplained motor vehicle accidents
- Family history of heart disease or abnormalities, such as coronary artery disease, heart rhythm disorders (including long QT syndrome or Brugada syndrome), congenital heart defects, heart failure or cardiomyopathy (dilated or hypertrophic)
- Personal history of congenital or acquired heart disease or abnormalities
- Use of drugs such as cocaine, illegal inhalants, “recreational” or club drugs
Suspect an SCA? What you can do
If your child has any of the warning signs of sudden cardiac arrest, make an immediate appointment with your pediatrician or take your child to an emergency department if the symptom just occurred.
If your child has any of the hereditary or lifestyle risk factors for SCA, ask your pediatrician for a referral to a pediatric cardiologist. The cardiologist can perform a thorough cardiac examination on your child and recommend next steps, which could include regular monitoring, lifestyle changes, medication initiation or other interventions.
Your family’s awareness of SCA warning signs — and your child’s ability to recognize them and come to you with concerns — could make the difference between life and death.
Contributed by: Victoria Vetter, MD, MPH, and Lindsey Flanagan, MPH
Featured in this article
Specialties & Programs

Every year, more than 23,000 children and teens experience a sudden cardiac arrest (SCA) in the U.S. Many of these cases result in death but can be prevented if children and parents recognize the early warning signs of SCA and seek medical attention before a crisis occurs.
Sudden cardiac arrest occurs when the heart suddenly and unexpectedly stops beating due to an abnormality in its electrical pulses. This abnormal rhythm can result in rapid quivering of the heart (ventricular fibrillation) or no heartbeat at all (asystole).
A child who experiences a sudden cardiac arrest loses consciousness, stops breathing or gasps for breath and becomes unresponsive, possibly with shaking (seizure-like) movement. CPR and use of an automated external defibrillator (AED) within two to three minutes of the event can prevent an interruption in blood flow to the brain.

SCA warning signs and symptoms
In as many as half of all cases of sudden cardiac arrests, warning signs and symptoms are present beforehand. But too often they are ignored or misunderstood. Parents and children should be aware of these signs and symptoms and seek medical help immediately when they occur.
Victoria Vetter, MD, MPH, a cardiologist in the Cardiac Center and Medical Director of the Youth Heart Watch program at Children’s Hospital of Philadelphia (CHOP), and Lindsey Flanagan, MPH, program coordinator of the Youth Heart Watch program, detail the warning signs and symptoms of sudden cardiac arrest:
- Racing heart rate or heart palpitations
- Dizziness or lightheadedness especially with exercise
- Repeated unexplained fainting
- Fainting when excited, startled, during exercise or right after exercise
- Seizures during or immediately after exercise
- Chest pain or discomfort with exercise
- Excessive shortness of breath or unusual fatigue during exercise (not related to asthma)
Additionally, there are certain factors or genetic predispositions that can increase an individual's risk of SCA — whether they have symptoms or not. These include:
- A family member with unexplained recurrent fainting or seizures
- A family member who died suddenly before age 50 or a family history of sudden unexplained infant death, drowning, or unexplained motor vehicle accidents
- Family history of heart disease or abnormalities, such as coronary artery disease, heart rhythm disorders (including long QT syndrome or Brugada syndrome), congenital heart defects, heart failure or cardiomyopathy (dilated or hypertrophic)
- Personal history of congenital or acquired heart disease or abnormalities
- Use of drugs such as cocaine, illegal inhalants, “recreational” or club drugs
Suspect an SCA? What you can do
If your child has any of the warning signs of sudden cardiac arrest, make an immediate appointment with your pediatrician or take your child to an emergency department if the symptom just occurred.
If your child has any of the hereditary or lifestyle risk factors for SCA, ask your pediatrician for a referral to a pediatric cardiologist. The cardiologist can perform a thorough cardiac examination on your child and recommend next steps, which could include regular monitoring, lifestyle changes, medication initiation or other interventions.
Your family’s awareness of SCA warning signs — and your child’s ability to recognize them and come to you with concerns — could make the difference between life and death.
Contributed by: Victoria Vetter, MD, MPH, and Lindsey Flanagan, MPH
Contact us
Youth Heart Watch