Chronic Lung Disease: Leila’s Story
Chronic Lung Disease: Leila’s Story
Born prematurely at 26 weeks, Leila still struggled to breathe two months later.
Despite supplemental oxygen and mechanical ventilation, her tiny lungs – Leila’s birth weight registered just 1 pound, 10 ounces – had failed to develop.

“They told us they couldn’t do anything else for her,” Jasmine, Leila’s mother, said. Doctors at her birth hospital said Children’s Hospital of Philadelphia (CHOP) could help.
Lucky for Leila, she was born in Philadelphia near CHOP, one of the few places in the world capable of providing specialized care for chronic lung disease in infants. Her family credits CHOP’s best-in-class team of specialists with providing expert complex care and family-centered support to help Leila breathe on her own at home.
“At CHOP, they are very passionate about what they do. They are very caring, loving and supportive,” Jasmine says. “It is awesome.”
World class, family-centered care for bronchopulmonary dysplasia
When Leila arrived at CHOP, she needed a breakthrough.
On a mechanical ventilator since birth, Leila’s oxygen levels remained critically low. Once inside CHOP’s Newborn/Infant Intensive Care Unit (N/IICU), Leila received a detailed evaluation that revealed severe chronic lung disease, also called bronchopulmonary dysplasia (BPD). So small she could be held in one hand, Leila received food through a nasogastric (NG) tube.
As the N/IICU team and neonatology and pulmonary specialists managed Leila’s treatment, CHOP’s family-friendly layout and services helped family members stay connected to their medically fragile newborn.
Jasmine or Leila’s dad, Daniel, slept next to her bed in its own corner of the treatment space or could seek deeper rest in a nearby parent sleeping area.
“We were able to have privacy with our child. And if I needed it, I could go get some quiet and really sleep,” her mother says. “CHOP was kind of like our home away from home.”
When both parents were away tending two older daughters, they could see Leila anytime through a phone app streaming from a camera suspended above her hospital bed.
“Even though I wasn’t there sometimes, I knew she was in the best hands, that the care she was receiving was beyond measure,” Jasmine says. “CHOP is such a friendly hospital. Everyone is really sweet. They try to make sure that you are OK.”
Care for the caregiver
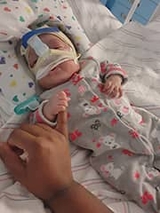
That attention and understanding meant a lot to Jasmine, who says she felt depressed and helpless that her daughter remained ill. Leila’s stay at CHOP lasted from December 2020 through April 2021. During that 140-day hospital stay and afterward, her mother says CHOP also made a difference for her own well-being.
One time that stands out is when a CHOP nurse helped Jasmine care for an infected cut on her hand. Returning to Leila’s bedside after getting medical attention for herself, Jasmine says a nurse took time to see her wound had been properly cleaned and bandaged. “That meant so much to me. She was one of so many CHOP angels that came my way.”
Giving families the confidence to manage complex care at home
After four-and-a-half months inside CHOP, Leila was discharged without oxygen or breathing support. To continue her care at home, nurses in the CHOP Family Learning Center taught Jasmine how to feed Leila via her gastronomy tube and track an oxygen monitor tracked remotely by the hospital. Going home was daunting, especially assisting with Leila’s G-tube and complex care, Jasmine says.
“I was doing so much with Leila and her treatment,” she says. “CHOP gave me confidence. They built me up to keep going and keep striving and push harder. The love they showed me until I was comfortable taking care of Leila by myself at home was just amazing.”
Expert outpatient follow-up overcomes setbacks
For follow-up care, Leila was referred to Sharon McGrath-Morrow, MD, MBA, Associate Chief of the Division of Pulmonary and Sleep Medicine and leader of the Post-preemie Lung Disease Clinic. For Jasmine, the doctor’s specialized experience in BPD and rare lung diseases made all the difference.
Dr. McGrath-Morrow “was very hands on with Leila,” Jasmine says. “She told me that anytime Leila had trouble breathing, to call her right away. And she said, if I can’t reach her, to reach her team, and she would find out about it and be right there.”
Jasmine grew close to the doctor as Leila faced setbacks in the summer of 2021 that sometimes required brief hospitalizations for breathing treatments and monitoring until she stabilized enough to go home again.
When self-doubt plagued Jasmine, Dr. McGrath-Morrow reassured her that Leila would get better and that she was doing an amazing job. “She helped me understand that I was already doing everything that I could.”

As Leila approached her first birthday, Dr. McGrath-Morrow diagnosed sleep apnea after a sleep study. The CHOP team stepped in to train family members how to help Leila with a bilevel positive airway pressure machine (Bi-Pap), a non-invasive machine that pushes air into the lungs.
“She is one doctor I will always remember,” the mother says. “She was always there when I needed her.”
Improving at home
Now nearly 2 years old, Leila breathes on her own around the clock.
CHOP specialists continue to monitor Leila’s progress. That includes physical and occupational therapy, for example, to teach her how to eat with a spoon. Speech therapy helps her talk to her family for the first time, with words like “go” and “dad.” Her grandmother has begun feeding Leila soft foods, like mashed potatoes, as she learns how to swallow. The experience has even led her mom to a new purpose.
“CHOP is such a big support system. It made me want to be in a NICU and take care of kids that are just like Leila,” Jasmine says, adding she is studying to become a nurse.