Critical Care and Resuscitation Science Center/Academy for Resuscitation of Children: Emma’s Story
Critical Care and Resuscitation Science Center/Academy for Resuscitation of Children: Emma’s Story
For 11 long, heart-wrenching minutes, 16-month-old Emma’s heart stopped beating.
The critical care team at Children’s Hospital of Philadelphia not only revived her, but the high-quality cardiopulmonary resuscitation (CPR) that brought her back to life and additional life-saving treatments enabled her to recover fully.
“There’s no way to fully thank the people who gave you your daughter back,” says Emma’s mom, Christine. “We are eternally grateful to the unbelievable care Emma received. They didn’t just save Emma; they saved our whole family.”
From a common cold to the PICU

It all started with a cold in late summer. When nebulizer treatments didn’t clear Emma’s congestion, Christine took her to their local hospital, which immediately sent her by ambulance to CHOP. Shortly after arriving in the Emergency Department, Emma was sent to the Pediatric Intensive Care Unit (PICU), where she was put on a ventilator since she was in respiratory distress. As doctors and the ICU staff were working feverishly to try to stabilize and support her, Emma’s heart stopped beating.
Christine and Emma’s father, Sean, were waiting in a conference room on the PICU floor for Emma to get settled in when they heard the loudspeakers bark: CODE BLUE!
As doctors were placing an arterial line, a thin tube to facilitate drawing blood and monitoring blood pressure, Emma went into cardiac arrest. Sean raced down the hall and saw the crowd around Emma’s bed.
The code team follows a well-practiced plan that adjusts moment by moment to each patient’s changing condition. Many advances in pediatric CPR have been developed, researched and validated at CHOP, which long ago determined that methods that work for adults aren’t always appropriate for children. CHOP has led the nation, and the world, in training clinicians in the most advanced methods of CPR. The team at Emma’s bed knew what it was doing.
When those interminable 11 minutes passed and Emma’s heart began beating on its own, she still wasn’t out of the woods.
Hour by hour
Christine and Sean were able go to Emma’s room and met critical care specialist Neethi Pinto, MD. “She told us that she would do everything necessary to get her better,” Sean says. “We were taking it hour by hour.”
After the resuscitation, Dr. Pinto tried a series of different ventilators to improve Emma’s ventilation and her oxygen levels, but none were bringing relief. After consulting with anesthesiologist Todd Kilbaugh, MD, Medical Director of the ECMO Center and Co-Director of CHOP’s Resuscitation Science Center, the recommendation was to start Emma on a trial of inhaled anesthetic and then extracorporeal membrane oxygenation (heart-lung bypass pump), commonly known as ECMO, an advanced life support technique used for patients with life-threatening heart or lung problems.
“Neither of us even knew what ECMO was,” Sean says. “But the doctors and nurses explained to us step by step what was happening.”
‘Gave us hope’
“They also gave us the one thing we needed the most: hope. When you’re going through something like this, hope is the most powerful emotion.”
During the four days the ECMO machine pumped and oxygenated Emma’s blood for her and the additional day she remained on a ventilator, her parents were by her side.
“One of us was always with her,” Christine says, “talking to her — even though she was sedated. That was important to us, making sure she knew she was not alone and to keep fighting.”
Critical care attending physician Martha F. Kienzle, MD, was a calm voice during those tense days. “She told us that the team was experienced and knew what to do,” Sean says. “She was right. Everybody was the best.”
After Emma was weaned off the sedatives, she underwent another evaluation and then an all-important brain scan.
“We were very nervous since she had such a long cardiac arrest,” Sean says. “I’m a special education teacher, and Christine works in homecare. We knew first-hand what we could be facing if she had sustained severe brain injury. We were overjoyed when the neurologist told us there was no damage.”
Long road to recovery
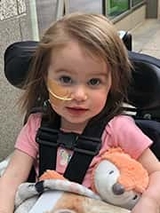
Still, there was long road ahead as Emma had to regain the strength and skills she had lost from being immobile for more than a week. “She couldn’t even hold her head up at first,” Sean says.
Emma gained strength and after a few days, she was able to leave the PICU for a regular medical unit, where intensive therapy began. They started to re-teach her how to swallow so she could eat and drink.
“They were so happy with her progress. She kept impressing us and surprising us. She’s destined for great things,” Christine says.
Ten days after she came off ECMO, Emma had progressed rapidly. She was transferred to the rehabilitation unit in CHOPs Seashore House to continue her therapies. “She went from not even being able to get herself into the crawl position to learning how to walk again,” Sean says.
Her swallowing had improved enough that she was given regular food. Physical and occupational therapy were helping her regain her strength and coordination.
Beyond care
What impressed the family as much as the exceptional care Emma received was the way everyone treated them.
“Their bedside manner was phenomenal,” Christine says. “They were always asking us: What questions do you have for me? I also loved how the nurses spoke to Emma all the time. They were patient and kind.
“We were confident and comfortable with the care Emma was receiving, and being treated with such respect by the whole team made the whole situation so much more bearable.”
While all this was happening, Emma’s twin brother Patrick and 3-year-old brother Jack were home, being cared for by friends and relatives as Sean and Christine took turns being with Emma. “It was a challenge,” Sean says. “We were lucky to have friends and family nearby to support us.”
A special good-bye

After two weeks in rehab, Emma was cleared to go home. Discharge day was special as many of the doctors, nurses and therapists who had been part of Emma’s journey stopped by to say good-bye, including Dr. Pinto, who told the family how meaningful it was to see Emma’s complete recovery.
“She told us that Emma helped the code team understand that even after 11 minutes of CPR, you don’t stop,” Christine says. “She said, ‘We needed Emma as much as she needed us.’”
Emma, now 21 months old, is back at home in Montgomery County and back to her spunky, happy-go-lucky, girly-girl self. She adores her brothers and thinks that Jack is funniest person in the world. Between reading books and playing with trucks, she can be found singing and dancing to her favorite songs.
Emma will continue to be followed up to ensure her remarkable recovery is complete. The family signed on to participate in research in CHOP’s Resuscitation Science Center and Academy for Resuscitation of Children, which strives to improve CPR and other interventions so children like Emma have the best possible outcomes.
“Christine and I were at the bottom of the bottom of the bottom during the code blue,” Sean says. “Anything that we can do so other families don’t have to feel that way, we will be happy to do.”