Fetoscopic Endoluminal Tracheal Occlusion Offers Hope for Prenatally Diagnosed Cases of Severe Congenital Diaphragmatic Hernia
Fetoscopic Endoluminal Tracheal Occlusion Offers Hope for Prenatally Diagnosed Cases of Severe Congenital Diaphragmatic Hernia
For a select group of babies with the most severe form of CDH, treatment before birth may allow the lungs to grow enough so these children are capable of surviving and thriving. Since the early ’90s, our team has investigated tracheal occlusion — blocking the fetal airway — as a viable treatment in severe CDH. Hear from three mothers whose children underwent this treatment option before birth and are now growing and thriving.
It’s a devastating diagnosis for an expecting parent to receive. A hole in the diaphragm — the breathing muscle that separates the chest from the abdomen — has allowed the abdominal organs to move up into the chest and prevent the growth of the lungs while their unborn baby is in the womb. In some cases, left untreated before birth, the lungs will be too underdeveloped for a baby to breathe on their own after birth.
CDH: Illustrated
Over the past 26 years, the Richard D. Wood Jr. Center for Fetal Diagnosis and Treatment at Children’s Hospital of Philadelphia (CHOP) has worked to establish the very best program in the world for congenital diaphragmatic hernia (CDH). We have unparalleled experience providing the most detailed prenatal diagnosis, determining the spectrum of severity, and using that information to predict a baby’s prognosis after birth in order to determine the best options. We have made advances that have improved the outcome for many children.
Yet, despite our best efforts, there remains a significant risk of death and long-term complications in children with severe CDH. Respiratory and cardiovascular functions are often severely compromised at birth. Approximately 25% of all children born with CDH — and 45% of those with severe CDH — require a complex form of heart-lung bypass called extracorporeal membrane oxygenation (ECMO). Children also may suffer long-term problems with breathing, feeding, heart function, hearing and brain development.
For this select group of babies with the severest form of CDH, treatment before birth may allow the lungs to grow enough so these children are capable of surviving and thriving. Since the early ’90s, our team has investigated tracheal occlusion — i.e., blocking the fetal airway — as a viable treatment in severe CDH.
Fetoscopic endoluminal tracheal occlusion (FETO) is a minimally invasive procedure that involves placing a balloon in an unborn baby's airway for several weeks. The balloon blocks fluid created by the lungs, causing the lungs to fill with fluid and expand. Lungs stimulated to grow before birth are more capable of sustaining life after birth. CHOP began offering FETO as a treatment option to select fetuses with severe CDH in 2015.
The following anecdotes from Alyssa, Ashley and Emma — three mothers whose children underwent this treatment option before birth and are now growing and thriving — offer first-hand insight into the experience.
A fetal technique to encourage lung growth
Alyssa and Louis traveled to CHOP from their home in northern New Jersey for the opportunity to undergo FETO. The CDH team at CHOP, including fetal surgeon Holly Hedrick, MD, and a maternal-fetal medicine specialist went over the potential benefits and risks of the procedure, which include preterm birth. They were so calm, comforting and competent that Alyssa and Louis knew they had their family’s best interest in mind.
“Knowing your care is in the hands of people who are so knowledgeable, capable and caring, it alleviates the stress you feel.”
“They really wanted us to make a decision that we were comfortable with,” says Alyssa.
FETO involves two minimally invasive procedures before birth. In the first, a small incision is made in the mother’s abdomen, an endoscope is inserted through the abdominal wall and uterus into the amniotic cavity, and a balloon is placed in the unborn baby's airway. The balloon blocks the airway and distends the lungs with fluid. This stretch signals the lungs to grow. Lungs stimulated to grow before birth are more capable of sustaining life after birth.
While the balloon is in place, mothers must stay close to CHOP so the balloon can be removed by the Center’s experienced team in the event they go into labor unexpectedly. After several weeks, a second minimally invasive procedure is performed to remove the balloon from the fetus’s airway.
Delivering at CHOP
After the balloon is removed, the plan is to prolong the pregnancy a few more weeks allowing the lungs to mature until delivery in CHOP’s Garbose Family Special Delivery Unit (SDU). Delivery in the SDU gives babies immediate access to CHOP’s neonatal CDH experts.
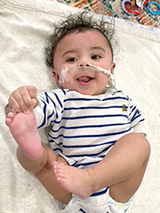
“We wanted to do whatever we could to be proactive,” says Alyssa of choosing to go ahead with the procedure. “We thought we would regret it if we didn’t.”
After the first procedure, Alyssa and Louis were thrilled to see during weekly follow-up appointments that their son Hendrix’s lungs were doing what they and the doctors hoped they would: growing in the womb.
“FETO saved his life,” Alyssa says.
Ashley had the same reaction when she saw the fetal MRI after her son, Grier, underwent the FETO procedure.
“It was a miracle,” says Ashley, who traveled to CHOP from North Carolina for care. “The first thing I said when I saw the MRI was, ‘He has lungs!’”
Leveling the playing field for kids with severe CDH

Like many children born with CDH, Hendrix and Grier both needed breathing support after birth and have struggled with feeding issues.
“Even though he was born premature, the fact that his lungs grew made all the difference,” says Alyssa of Hendrix.
For all the similarities between children with CDH, each family’s experience is also very unique. Hendrix had to be delivered before the second procedure to remove the balloon could be performed. Preterm birth is a known risk with FETO, and the care team is always prepared to mobilize 24/7/365. They quickly and successfully removed the balloon while Hendrix was still attached to the placenta and stabilized him.
Emma was living in Australia when she found out the child she was expecting had severe CDH. She moved back to the U.S. to seek out the best possible care and chose to undergo FETO because she knew it offered her son, Alexander, the best hope. While Emma’s water broke early, she was able to stay on bed rest in the SDU and undergo the second FETO procedure to remove the balloon. Three days later, she went into labor.
Alexander is now a happy little boy who loves gymnastics and playing with tractors and trucks. His family is very outdoorsy, and Alexander skis and hikes right along with them. He loves school so much he comes home singing the alphabet every day.

“He is my hero,” says Emma. “He has overcome so much, and I am so proud to be his mother.”
There is no one-size-fits-all approach to treating CDH, which is why it’s so important to develop a custom treatment plan for each baby's and family's unique needs. CHOP’s team has decades of experience providing the most detailed prenatal diagnosis and using that information to provide families with the most accurate information and options for their unborn baby. FETO is one of many treatment options we are able to utilize based on a baby's unique needs.
Our colleagues in Europe recently released a study showing that FETO offers real benefits for babies with severe CDH. Read more about the study here.