Heterotaxy Syndrome: Finn’s Story
Heterotaxy Syndrome: Finn’s Story
Finn, 3, is an extremely energetic toddler who loves to run, dance, climb the stairs, and go down the slide at his neighborhood playground. Watching him, you would never guess he was born with serious heart defects, or that he had heart surgery at Children’s Hospital of Philadelphia.

Kelly and Michael found out there was something wrong with their second child’s heart at a scheduled 19-week ultrasound. “The technician looked like she had seen a ghost,” Kelly remembers.
The couple were put in a conference room to wait. After reviewing the images, a doctor explained that their baby had no separate chambers in his heart (there should be four), and had both extra and missing vessels connected to his heart. The heart defects were elements of a condition known as heterotaxy syndrome, a rare birth defect that involves the heart and other organs. In addition to his heart anomalies, his lungs were reversed and his bowel was misplaced.
“We were told he wouldn’t make it,” says Kelly, “That if he survived to term, he would pass away soon after he was born.”
A ray of hope
The couple went for second and third opinions with specialists in Richmond, VA, and Washington, DC, near where they live. They received the same prognosis — their child would not survive.
“I just kept going back to my OB,” says Kelly. “I was convinced that this was not his destiny.”
A nearby local hospital agreed to take her on for the rest of her pregnancy and delivery, with a plan to have pediatric heart specialists on hand to care for the baby at birth.
Eight months in the hospital
Finn spent his first eight months in the hospital, during which he had open heart surgery to reroute the blood flow around his heart. Unfortunately, the procedure resulted in a string of complications, including fluid around his lungs and chest and irregular heartbeat (arrhythmia), which required a number of invasive procedures.
When Finn finally went home at 8 months, he was at the developmental level of a newborn. He couldn’t hold his head up. But, free from tubes and other medical devices, and with a break from surgeries, he started to make up for lost time. He sat up at 16 months and walked at 18 months.
New concerns and a second opinion at CHOP
As Finn got older, his parents looked into seeking second opinions regarding his management given the complexity of his condition.
They got permission from their insurance provider to get a second opinion, and did research on the hospitals and doctors with expertise in treating children with heart malformations and heterotaxy syndrome. There were only a handful with the deep expertise they were looking for – Finn would need care from a number of different specialists. Before they contacted any hospitals or doctors, they read about them and got in touch with other patients’ families.
In their research, Children’s Hospital of Philadelphia (CHOP) stood out.
“On paper, they had the expertise,” says Kelly. “In all of the specialties that mattered to us — cardiology, GI, neurology — they were making breakthroughs.”
“Then when I spoke with CHOP families, they all just raved about the place. Over and over, people got emotional about Children’s Hospital of Philadelphia.”
Lifting the burden
Kelly contacted the Cardiac Center at CHOP and arranged for a telephone consultation with Matthew O'Connor, MD, an attending cardiologist and the Medical Director of CHOP’s Heart Failure and Transplant Program.
Dr. O’Connor reviewed Finn’s medical records, including images of his heart, before the call. “He was wonderful,” says Kelly. “CHOP will not say ‘It’s going to be OK.’ No one can know that. Instead, Dr. O’Connor told us he could help. He said he would be there for us and that he would do the very best he could for Finn. He took every one of our concerns seriously. When I got off the phone I cried happy tears. The burden was gone. I knew that this was the place.”
At their appointment, Dr. O’Connor evaluated Finn and confirmed that he would need another heart surgery within the next few months. His heart required staged reconstruction. The Glenn procedure, performed when he was 12 weeks old, was one of these stages. Now he would need a modified version of the Fontan procedure to improve his altered circulation.
Life-saving surgery
The family returned to CHOP for more detailed imaging of Finn’s heart, including an MRI and a cardiac catheterization performed by Jonathan J. Rome, MD, an attending cardiologist and Director of CHOP’s Cardiac Catheterization Laboratory. Drs. O’Connor and Rome then consulted with Thomas L. Spray, MD, Chief of the Division of Cardiothoracic Surgery.
The team sat down with the family to explain their recommended approach to repairing Finn’s heart. Finn’s circulation had already been modified to work with his non-chambered heart. Dr. Spray would make two small additional modifications to improve the blood flow, particularly the circulation of oxygenated blood.
Finn went in for his surgery. Kelly and Michael, while confident in Dr. Spray, were understandably nervous.
“We had handed our child off many times by that point,” says Kelly. “His earlier heart surgery had led to weeks of complications.”
So, they were alarmed when Dr. Spray came out well before they were expecting him. But instead of bad news, it was to tell them that the surgery had been a success. Dr. Spray’s part of the procedure had taken just 37 minutes. Finn was already off of life support.
“A miracle to us”

Kelly and Michael walked into Finn’s room to find that color had returned to his skin — it was pink, not the greyish blue it had been before — and he looked healthier already.
“Seeing the difference so immediately was a miracle to us,” says Kelly. “That night I stayed in the ICU next to him, and I slept better than I had in three years. I knew he was going to be OK, that he would be there in the morning. I knew that I would see birthdays and graduations in the years ahead.”
A week later, Finn was discharged from the hospital. The family spent another week in Philadelphia to be nearby for follow-up appointments, and used the time to go to the zoo, go pumpkin picking, and enjoy time with their freshly energized little boy.
Once they returned home, the family delighted in Finn’s many new “firsts.” He climbed the stairs by himself for the first time, slept through the night for the first time, and ran for the first time. (That first run was down the driveway toward the street, but it still was a joy for his parents — who stopped him.)
“I used to look at the scar on his chest, the one from the first heart surgery, with pain,” says Kelly.
“Now I don’t see pain in the scar. I see hope and life.”
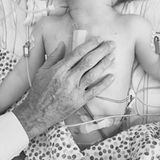
One of the most moving mementos of their brief stay at CHOP is a picture Kelly took with Dr. Spray’s hand gently resting on Finn’s chest while he slept. It’s a tender picture of a healing boy, with the hand of the man who healed him.