Sofia-Rose’s Spina Bifida Fetal Surgery Story
Sofia-Rose’s Spina Bifida Fetal Surgery Story

When Alicia and Matthew first learned their unborn baby had a devastating birth defect, the prognosis was grim. But the team at CHOP offered them hope through fetal surgery.
Rylan, age 5, watched intently as the child life specialist used a baby doll to explain his little sister Sofia-Rose’s condition. She pointed to the doll’s back and described what it meant to have spina bifida. She said surgeons were going to operate on his mom’s belly to fix Sofia-Rose’s back before she was born and provided age appropriate language and preparation regarding the newborn intensive care unit. Rylan told his mother, Alicia, “I’m ready.” And despite the stress of the situation, so was Alicia.
She and her husband, Matthew, of Sicklerville, N.J., had tried for nearly four years to get pregnant again. Rylan was so excited to be a big brother, he would kneel with his mother in church and pray for a sibling. “It was the cutest thing ever,” says Alicia.

Where to start
For parents who find out their unborn baby has spina bifida, the biggest question is often “what do I do next?” Here’s advice on where to start.
Learning their long-awaited child had spina bifida — a birth defect in which the spinal column doesn’t form properly, leaving a section of spinal cord and nerves exposed through an opening in the back — was devastating. They received the diagnosis during an anatomy scan about 21 weeks into the pregnancy. Their physician provided some information about the situation that seemed grim to the couple.
“He said, ‘She will certainly be in a wheelchair,’” Alicia recalls. “He said 64 percent of families usually abort their child when they find out they have this disability, and he told us we had two weeks to decide if we wanted to terminate the pregnancy.”

The experience left them shaken and depressed.
“I had to tell my son that there was something wrong with the sister he had prayed for,” Alicia shares. “I just kept thinking, ‘What did I do wrong? Why me?”
CHOP offers hope before birth
Termination was not an option for the couple, so their physician connected them with the Richard D. Wood Jr. Center for Fetal Diagnosis and Treatment (CFDT) at Children’s Hospital of Philadelphia (CHOP). Alicia began to feel more hopeful from the first call with the CFDT fetal coordinator. The coordinator calmly explained the condition in detail and that physicians aren’t certain what causes it. She said there were treatment options depending on the location of the spinal lesion and scheduled the couple to meet with the center’s team.
Advanced imaging tests and a detailed evaluation at the center confirmed the location of the defect and the presence of hindbrain herniation, in which part of the brain descends into the upper portion of the spinal canal in the neck, blocking the circulation of cerebrospinal fluid. It can cause hydrocephalus and injure the developing brain.
The evaluation confirmed Sofia-Rose was a candidate for fetal surgery, a delicate procedure in which fetal surgeons open the uterus and close the opening in the baby’s back. Closing the spinal opening before the baby is born protects the spinal cord from continued exposure to amniotic fluid, which can cause progressive damage, and can reverse the devastating effects of hindbrain herniation.
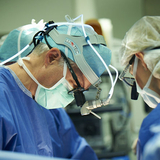
Why choose us
Our surgeons pioneered fetal surgery for spina bifida, and have the greatest collective experience in the world.
Preparing for fetal surgery
The couple met with the treatment team to discuss the surgery and potential outcomes. The plan was for Alicia to have a cesarean delivery at 37 weeks in the Garbose Family Special Delivery Unit (SDU), the world's first birth facility in a pediatric hospital specifically designed for healthy mothers carrying babies with known birth defects. Sofia-Rose would then receive postnatal care in the Harriet and Ronald Lassin Newborn/Infant Intensive Care Unit (N/IICU). The team explained that Sofia-Rose might need a catheter and orthotics once she got older.
“They fully explained how it could help and what Sofia-Rose’s life could be like,” says Alicia. “I felt hopeful that we were giving her the best chance at life.”
Two weeks later, Alicia underwent fetal surgery. She was relieved to feel Sofia-Rose kicking the next day. Alicia took medical leave from work and spent the next 12 weeks on bedrest. She stayed at her mother’s house to be closer to CHOP for weekly follow-up appointments. Her mother, father and sister were a huge help, caring for both her and Rylan.
“Without the support of my husband, immediate family and CHOP, I don’t think I would have been able to do it,” she says. She also joined an online Facebook group for moms who undergo fetal surgery and was able to connect with women from all over the country with this shared experience.
At 36 weeks and six days, clinicians discovered during a pre-op appointment that Alicia had global membrane separation. Sofia-Rose needed to be delivered immediately. To everyone’s glee, she came out kicking and screaming. After birth, Sofia-Rose was cared for in the N/IICU by a dedicated Neonatal Surgical Team. Her hindbrain herniation was completely reversed and she didn’t require any special care for spina bifida.
Leaving smiles in her wake

Sofia-Rose is now a happy, independent 3-year-old who always has a smile on her face, and leaves everyone she meets with one as well. She wants to do everything all by herself. She loves making new friends, painting, drawing, playing dress-up, singing, dancing, and playing with her big brother. She can count to 20 and knows her shapes, even the hard ones like a hexagon, and is learning to write her name. In fact, Sofia can write and draw with both hands.
According to her doctors, she's doing "exceptionally well." She currently does not need any assistance with bracing, and has not needed a shunt or any other surgeries. She has good bladder and bowel control, and is in the process of being potty trained. They're watching for tethered cord since she is at the age where it typically starts to appear, but she's doing great overall.
She continues to be followed through CHOP’s Spina Bifida Clinic, where she's always happy to see the familiar faces of her care team, and loves showing off what she can do to.
"Having spina bifida doesn't stop Sofia," says Alicia. "She is aware that she has spina bifida and doesn't mind telling her friends about it. We stay very open as a family about her disability so she and Rylan can understand and feel comfortable speaking about it. She will keep defying odds and raising awareness!"
Hear from Sofia-Rose's family about their journey.
Updated November 2020