Extracorporeal Membrane Oxygenation: ECMO
What is ECMO?
Extracorporeal membrane oxygenation, or ECMO, is an advanced life support technique used for patients with life-threatening heart and/or lung problems. ECMO is not a cure. It is a temporary mechanical breathing and heart support used only when all of the standard treatments for those problems have already been tried. A highly specialized treatment, ECMO can support patients for days to weeks while doctors treat their underlying illness.
What does ECMO stand for?
- Extracorporeal: means outside the body
- Membrane: a type of artificial lung
- Oxygenation: the process of getting oxygen into the blood
How does ECMO work?
ECMO is performed using a heart-lung bypass machine similar to the one used during open heart surgery. The ECMO machine, often referred to as a “circuit,” is quite large. It pumps blood through sterile plastic tubing from your child to the “ECMO membrane lung.” The ECMO membrane lung is an extracorporeal device, meaning it is located outside of the body. The ECMO lung removes carbon dioxide from the blood and adds oxygen to the blood, as a healthy lung would. The ECMO lung then pumps the oxygenated blood back to your child.
There are two types of ECMO:
- Venovenous (V-V) ECMO is used when the heart is functioning well and only the lungs need to rest and heal. This type of ECMO drains blood from a vein, oxygenates the blood in the circuit, and returns the blood through a vein.
- Venoarterial (V-A) ECMO can be used when the heart and the lungs need to rest and heal. This type of ECMO drains blood from a vein, oxygenates the blood in the circuit, and returns the blood to the body through an artery.
The type of ECMO support needed depends on a child’s illness.
When does a child need ECMO?
The reasons for ECMO vary. ECMO can help infants and children with a variety of medical problems and conditions, including:
- Meconium aspiration syndrome (MAS): A condition that occurs when meconium, the first stool of a newborn, is inhaled by the baby before or during delivery, and causes lung problems.
- Persistent pulmonary hypertension of the newborn (PPHN): A disorder characterized by abnormally high blood pressure in the arteries that supply blood to the lungs.
- Congenital diaphragmatic hernia (CDH): A condition in which part of the stomach and/or intestines protrude through an opening in the diaphragm into the chest cavity.
- Respiratory distress syndrome (RDS): a lung condition, usually in premature babies, that makes it difficult for babies to breathe on their own.
- Pneumonia
- Congenital heart conditions
- Sepsis
- End-stage cardiac or respiratory failure (as a bridge to transplant)
Our ECMO Center customizes the ECMO circuit for each patient, depending on their diagnosis, to allow healing.
The ECMO team
To help ensure the best outcomes, it's important to choose an experienced and qualified ECMO team with rigorous training in this complex level of life support.
While your child is on ECMO at Children's Hospital of Philadelphia, they will be cared for by a team of pediatric surgeons, cardiac surgeons, neonatologists, intensivists, cardiologists, perfusionists, nurses, respiratory therapists and other specialists.
A specially trained attending pediatric surgeon will perform the operation to insert the cannulas at the start of ECMO and will remove them when treatment is finished.
Our ECMO Core Team consists of approximately ten nurses (RNs) and respiratory therapists (RRTs) specially trained to manage the ECMO circuit. Additionally, there are more than 25 nurses and respiratory therapists trained as bedside ECMO specialists. All CHOP ECMO specialists have a minimum of two years of ICU experience and vigorous training requirements including annual recertification.
There will always be a nurse and an ECMO specialist at your child’s bedside. They will constantly monitor vital signs and comfort, perform care and maintain the ECMO circuit. An “in-house ECMO specialist” is available as a resource to staff 24/7. That person may be the program manager, a Core Team member or a perfusionist (for cardiac cases).
ECMO Center Earns Highest Honor
A team of doctors will make rounds (visit the bedside) every morning, assess the progress of your child, and share that information with you. Doctors will also check on your child throughout the day. ECMO patients at CHOP have around-the-clock access to an attending physician through the program’s “ECMO Resource MD” position. In addition, a wide range of specialists are on-call at all times.
Learn more about what sets our team apart in providing the best care for your child on ECMO.

ECMO Center
Children’s Hospital of Philadelphia’s ECMO Center receives the “Platinum Level ELSO Award for Excellence in Life Support.”
What to expect when your child is on ECMO
Your child will have one or more large plastic tubes, called cannulas, inserted into large blood vessels, most often in the neck. A surgeon places the tubes while your child is under anesthesia. These cannulas provide access directly into the heart and are needed for ECMO to work. Our team will request your consent before performing these operations. Every baby on ECMO receives blood products (we will ask you to sign a consent for this, too).
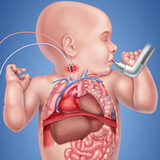
The blue cannula takes de-oxygenated blood, which has circulated through the body, out of the heart and into the ECMO machine, which adds oxygen to it.
Blood that has been oxygenated by the ECMO machine is pumped into the aorta through the red cannula. The aorta is the large blood vessel that normally carries oxygenated blood out of the heart to the rest of the body.
Even though ECMO does most of the work for the lungs, your child will remain on a breathing machine to deliver controlled amounts of pressure and oxygen to his lungs. The machine also allows the body to get rid of carbon dioxide, usually expelled when you exhale. The breathing tube inserted in the nose or mouth that connects the lungs to the breathing machine is called an endotracheal tube (ET tube).
Your child will also continue to need tubes and lines as she did before receiving ECMO. Most commonly, these include a nasogastric tube, which is placed in the nose and guided into the stomach to decompress and keep the stomach empty of acid; intravenous lines to provide fluids and medications; and a tube into your baby’s bladder to drain urine. Your child may also have a chest tube placed into the chest through the chest wall to drain air or fluid outside the lungs.
Your child will receive medication to treat any pain or discomfort while on ECMO. Pain medication is usually given as a continuous infusion into the ECMO circuit. Other medications frequently given during ECMO include diuretics to help your child urinate.
Swelling, also known as edema, is an expected side effect of ECMO. The medical staff caring for your child will monitor the condition closely.
While on ECMO, your child may undergo a variety of tests to monitor her condition, including:
- Blood gases (such as an arterial blood gas, or ABG) to monitor the oxygen and carbon dioxide levels in the blood.
- Complete blood count (CBC): This test monitors levels of red and white blood cells and platelets (cells in the blood that help to form blood clots) and tells us if we need to transfuse your baby with blood products.
- Basic metabolic panel (BMP): These tests monitor electrolytes (including calcium, potassium and other substances), which are needed in a certain balance for the body’s systems to run. These tests tell us which electrolytes we need to give your baby through the IV lines to keep them at normal levels. The BMP also helps us monitor kidney function, which is very important to your baby’s health.
- Tests to check your baby’s blood so we can adjust anticoagulant medications (“blood thinners” such as Heparin) during ECMO support and hemoglobin/hematocrit levels in the blood.
- Imaging tests done at bedside to monitor your baby’s progress, including X-rays to check the location of the cannulas and monitor inflation of the lungs; ultrasound of the head to monitor for complications related to bleeding; electroencephalogram (EEG) to monitor brain activity: and echocardiogram (an ultrasound of the heart) to assess how the heart is doing as we attempt to wean your baby from ECMO support.
Your child will be given sedation medications to keep her from moving around. This is necessary to keep the ECMO circuit in place and working correctly. The sedation medications will make your child sleep most of the time. Even though your child is sleeping, you can still talk to and carefully touch your child. Because it is important to let your baby rest while on ECMO, the ECMO specialist can guide you when it is safe for your baby to be stimulated.
Children, including infants, can hear and recognize the sound of their parents’ voices while sedated. Your child (and you) may find it comforting if you talk to him or hold her hand gently. Ask a child life specialist or other staff member for ideas on how to interact with your child.
The equipment being used to treat your child is quite delicate, so it is very important that you do not touch the cannulas, the machinery or the settings. For this reason, you won’t be able to hold your child while she is on ECMO. Keep a safe distance from the circuit, so you don’t accidentally bump into it. If you have questions about the equipment, please feel free to ask the ECMO specialist on duty who is caring for your child.
Your child will come off of ECMO when the heart and lungs have recovered enough to function without the ECMO circuit. This can take several days or several weeks, and it depends on your child’s specific diagnosis and course of treatment. As daily test results begin to show progress, the care team may slowly lower settings on the circuit to allow your child’s body to gradually function on its own, at which time the cannulas will be surgically removed.
After ECMO
Immediately following removal of the cannulas and ECMO circuit, your child will need to remain on a ventilator to maintain oxygenation. Nitric oxide is a gas given through the ventilator to relax blood vessels. Over time, the goal is to wean your child slowly from the ventilator and medications. A nurse will continue to closely monitor vital signs and signs of pain and perform ordered lab work. While each child is different, be prepared that your child’s recovery period from ECMO may be measured in weeks and months, rather than days.
Advice for parents when your child is on ECMO
Having a child on ECMO can be emotional, even traumatic, for parents, guardians and family. You will likely find that the experience is filled with many ups and downs. The following is advice from other parents who have been in your shoes.
- First and foremost, take care of yourself. Eat, sleep and get outside every day. You will need to make decisions about your child’s medical care, which you can do only if you are rested and alert.
- Be an active participant in your child’s care. Most parents have no medical training and find it difficult to understand much of the medical terminology and information. Ask questions to help you understand what is happening and to help you make decisions. The Hospital staff will make every attempt to answer all your questions.
- Use Hospital resources. There are many resources available at CHOP, free of charge, that may make your time less stressful. These include: sleep rooms (when available), a reference library, laundry, computers with Internet access, emotional counseling and more. Ask your bedside nurse for information.
- Talk to a Hospital social worker, who can help ease your stress by talking about issues that concern you.
Departments that offer Extracorporeal Membrane Oxygenation: ECMO
- Division of Pediatric General, Thoracic and Fetal Surgery
- Division of Neonatology in the Newborn/Infant Intensive Care Unit (N/IICU)
- Pediatric Intensive Care Unit (PICU)
- Cardiac Center in the Cardiac Intensive Care Unit (CICU)
Updated: November 2017