Intestinal Rehabilitation Program
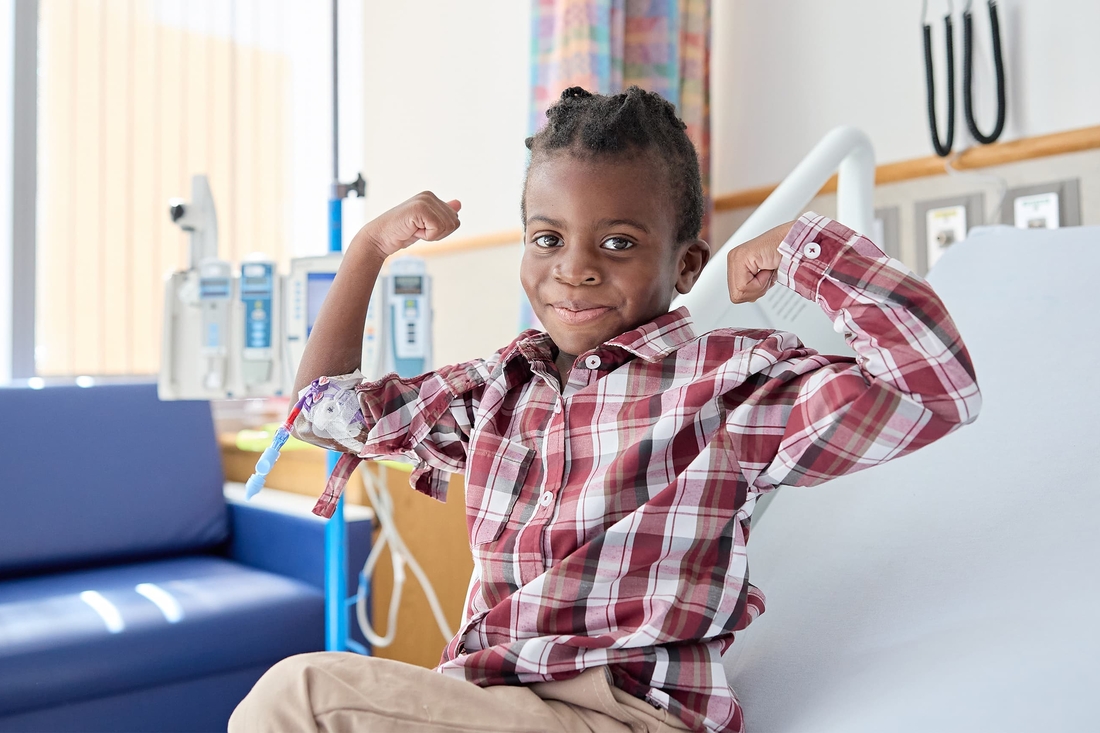
The Intestinal Rehabilitation Program (IRP) treats children with bowel disorders that affect their growth and development. Most patients come to us as infants born prematurely, have short or malformed intestines, or have lost part of their intestines due to disease. Others come after large portions of their intestines have been damaged by disease, trauma or infection.
Children with these rare bowel conditions can’t absorb enough nutrients from their food to survive and grow. Instead, they must rely on intravenous (IV) nutrition. Over time – and with medical treatment and supportive therapies – many children with intestinal failure can gain enough bowel function to eliminate the need for IV nutrition.
Conditions we treat
The Intestinal Rehabilitation Program treats children with bowel disorders that affect their growth and development, including those listed below.

Why Choose CHOP for Intestinal Rehabilitation Care?
The Intestinal Rehabilitation Program at Children’s Hospital of Philadelphia is led by a multidisciplinary team dedicated to delivering complex nutritional and medical/surgical management to pediatric patients with short or malformed intestines.
Meet our team
Our experienced team of gastroenterologists, general surgeons, nurses and nutritionists are experts in treating children with short bowel syndrome and intestinal failure. We provide complete and individualized care for your child.

Our research
Our mission includes conducting ongoing research to seek new ways to support patients with short bowel disorders.

Intestinal Rehabilitation resources
We have created patient instructions to support families caring for children with special nutrition and feeding needs.

Our approach to treatment
Our team works with parents to support patients’ nutritional and medical needs. We help your child become more independent using long-term medical management, medication, diet and nutritional therapy, vitamin and mineral supplements, surgery and other interventions. Collaboration with families is critical for patients’ long-term success.
Your donation changes lives
A gift of any size helps us make life-saving breakthroughs for children everywhere.
