Christine Goodbody, MD, MBE, Keith Baldwin, MD, MPH, B. David Horn, MD, David Spiegel, MD
The neurologic insult underlying cerebral palsy results in the primary impairments of spasticity, co-contraction, weakness, and loss of selective motor control, which inhibit the normal muscle stretch signals that stimulate muscles to grow. The resulting imbalance between muscle and bone growth leads to short, stiff muscles and, ultimately, contractures and bone or joint deformity—the so-called secondary impairments in cerebral palsy (CP). These secondary impairments lead to a loss of function, pain, and more arduous care needs. This is where the orthopedic surgeon can intervene to help.
When we think of deformity in the congenital and idiopathic populations, we largely (although not exclusively) speak of coronal plane issues (ie, varus/valgus) or longitudinal issues (ie, limb length discrepancies). However, deformity in the neuromuscular population very often involves the sagittal plane. Our lower extremity muscles function largely in the sagittal plane—ankle dorsiflexion and plantarflexion, knee flexion and extension, hip flexion and extension—to achieve locomotion and propel ourselves forward. Given that their main direction of pull is in the sagittal plane, this is the plane that tends to be affected by muscle contracture. As such, muscle contracture can severely impact a patient’s gait and function, and impair their ability to maintain an energy-efficient upright posture necessary for standing and walking.
The standard of care of orthopedic management in ambulatory cerebral palsy surgery is single event multilevel surgery (SEMLS). The idea is that addressing all bone and soft tissue deformities at one time will get the child upright and ready for one big rehab session without unmasking concomitant deformity and causing further gait impairment. SEMLS surgery improves the likelihood of achieving sagittal plane balance and has been shown to reduce the need for repeated anesthetics, number of hospitalizations, cost of care, missed school, and disruption to the family—all with improved functional outcomes.
Key: surgical timing
Surgical timing is critical in patients under consideration for intervention, as the brain injury in CP is static but the secondary impairments progress with time. Indications for surgery include later childhood (ideally 6 to 10 years old, except for in the case of hip displacement which is treated as soon as identified), a 6-month plateau in function, and exhaustion of nonoperative options like bracing, PT, and tone control to manage the impairment. At Children’s Hospital of Philadelphia (CHOP), we are fortunate to partner with our amazing multidisciplinary Cerebral Palsy Program to optimize our nonoperative options. Prior to any surgery, it is also imperative the patient and family are on board for a long-term rehabilitation commitment, since we know it takes kids about 6 months to get back to baseline and up to 2 years to reach their peak benefit.
When considering intervention in the ambulatory CP patient, we consider the diagnostic matrix, which is the web of information we need to put together in order to make the best decisions for if and which surgery will best serve our patients with gait disturbances. The components we need to weigh are the history (any underlying pathology, prior walking ability, past surgeries); the physical exam (range of motion noting contractures, tone, abnormalities in version); classification and functional scales (FMS/GMFCS); radiology (hip subluxation, patella alta, foot deformity); and gait analysis (both visual and instrumented if available). The more of these puzzle pieces that fit together and point toward a potential deformity being an impairment, the more confidently we can recommend an intervention.
Putting this information together, we look at each joint and possible contributing deformities. In the hip, we assess if flexion and/or adduction contractures limit range of motion or upright posture, and can lengthen the offending muscles as needed. At the knee we assess for contracture, and dose our intervention—PT and botox, hamstring release, anterior distal femur guided growth, or distal femoral extension osteotomy—based on the magnitude of deformity. At the level of the foot and ankle we assess for and treat positional or rotational deformities, as malalignment can contribute to what is known as lever arm dysfunction. This is a functional weakness due to an ineffective or poorly positioned lever. That is to say that if the bones are malaligned and the muscles are acting in an abnormal direction, out of the plane of motion, the effective force and therefore locomotive power is decreased. Torsional disorders such as femoral anterversion or tibial torsion can also cause lever arm issues, creating reduced efficacy of already weak muscles, making ambulation an even more arduous task.
Once a complete assessment of all the impairments at play has been performed, we form a list, or surgical recipe of all the impairments involved and what intervention is most appropriate, so all deformities are corrected simultaneously (see list below). Getting the legs straight and ready to rehab for these patients is critical for maintaining their ambulatory ability (see Figure 1 below). Among the things we do as orthopedic surgeons, helping a child walk longer, straighter, and more confidently is one of the most rewarding, and with the help of our Cerebral Palsy Program team, we hope to optimize function for these kids for the entirety of their childhood and beyond.
Example list of impairments and planned interventions for a patient after taking into account all elements of the diagnostic matrix:Sagittal plane
Problem
- Hip flexor contractures 15-20 degrees
- Knee flexion contractures 25-30 degrees
- Patella alta/extensor lag
Solution
- Bilateral hop flexor releases
- Bilateral distal femoral extension osteotomies
- Bilateral patellar tendon advancements
Axial Plane
Problem
- Mild femoral IR 30 degrees ante
- Severe Tibial IR 35-40 degrees
Solution
- Femoral derotation through extension osteotomies
- Bilateral tibial derotation osteotomies
Coronal Plane
Problem: Hip adduction contracture R>L
Solution: Adductor tenotomies
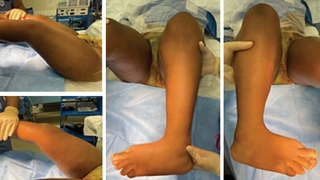
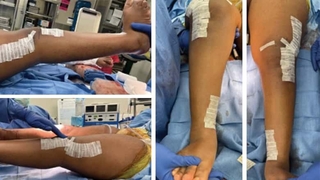
Figure 1: Preoperative clinical photos (top), showing the knee fl exion contractures and severe internal tibial torsion, which are corrected postoperatively (bottom), with the knee now coming to full extension and the foot pointing forward. All of the deformities were corrected simultaneous to allow for immediate upright posture and a single rehab course.
Reference and suggested reading
The Diagnostic Matrix. From: Davids JR, Ounpuu S, DeLuca PA, Davis RB 3rd. Optimization of walking ability of children with cerebral palsy. Instructional Course Lectures. 2004 ;53:511-522.
Featured in this article
Specialties & Programs
Christine Goodbody, MD, MBE, Keith Baldwin, MD, MPH, B. David Horn, MD, David Spiegel, MD
The neurologic insult underlying cerebral palsy results in the primary impairments of spasticity, co-contraction, weakness, and loss of selective motor control, which inhibit the normal muscle stretch signals that stimulate muscles to grow. The resulting imbalance between muscle and bone growth leads to short, stiff muscles and, ultimately, contractures and bone or joint deformity—the so-called secondary impairments in cerebral palsy (CP). These secondary impairments lead to a loss of function, pain, and more arduous care needs. This is where the orthopedic surgeon can intervene to help.
When we think of deformity in the congenital and idiopathic populations, we largely (although not exclusively) speak of coronal plane issues (ie, varus/valgus) or longitudinal issues (ie, limb length discrepancies). However, deformity in the neuromuscular population very often involves the sagittal plane. Our lower extremity muscles function largely in the sagittal plane—ankle dorsiflexion and plantarflexion, knee flexion and extension, hip flexion and extension—to achieve locomotion and propel ourselves forward. Given that their main direction of pull is in the sagittal plane, this is the plane that tends to be affected by muscle contracture. As such, muscle contracture can severely impact a patient’s gait and function, and impair their ability to maintain an energy-efficient upright posture necessary for standing and walking.
The standard of care of orthopedic management in ambulatory cerebral palsy surgery is single event multilevel surgery (SEMLS). The idea is that addressing all bone and soft tissue deformities at one time will get the child upright and ready for one big rehab session without unmasking concomitant deformity and causing further gait impairment. SEMLS surgery improves the likelihood of achieving sagittal plane balance and has been shown to reduce the need for repeated anesthetics, number of hospitalizations, cost of care, missed school, and disruption to the family—all with improved functional outcomes.
Key: surgical timing
Surgical timing is critical in patients under consideration for intervention, as the brain injury in CP is static but the secondary impairments progress with time. Indications for surgery include later childhood (ideally 6 to 10 years old, except for in the case of hip displacement which is treated as soon as identified), a 6-month plateau in function, and exhaustion of nonoperative options like bracing, PT, and tone control to manage the impairment. At Children’s Hospital of Philadelphia (CHOP), we are fortunate to partner with our amazing multidisciplinary Cerebral Palsy Program to optimize our nonoperative options. Prior to any surgery, it is also imperative the patient and family are on board for a long-term rehabilitation commitment, since we know it takes kids about 6 months to get back to baseline and up to 2 years to reach their peak benefit.
When considering intervention in the ambulatory CP patient, we consider the diagnostic matrix, which is the web of information we need to put together in order to make the best decisions for if and which surgery will best serve our patients with gait disturbances. The components we need to weigh are the history (any underlying pathology, prior walking ability, past surgeries); the physical exam (range of motion noting contractures, tone, abnormalities in version); classification and functional scales (FMS/GMFCS); radiology (hip subluxation, patella alta, foot deformity); and gait analysis (both visual and instrumented if available). The more of these puzzle pieces that fit together and point toward a potential deformity being an impairment, the more confidently we can recommend an intervention.
Putting this information together, we look at each joint and possible contributing deformities. In the hip, we assess if flexion and/or adduction contractures limit range of motion or upright posture, and can lengthen the offending muscles as needed. At the knee we assess for contracture, and dose our intervention—PT and botox, hamstring release, anterior distal femur guided growth, or distal femoral extension osteotomy—based on the magnitude of deformity. At the level of the foot and ankle we assess for and treat positional or rotational deformities, as malalignment can contribute to what is known as lever arm dysfunction. This is a functional weakness due to an ineffective or poorly positioned lever. That is to say that if the bones are malaligned and the muscles are acting in an abnormal direction, out of the plane of motion, the effective force and therefore locomotive power is decreased. Torsional disorders such as femoral anterversion or tibial torsion can also cause lever arm issues, creating reduced efficacy of already weak muscles, making ambulation an even more arduous task.
Once a complete assessment of all the impairments at play has been performed, we form a list, or surgical recipe of all the impairments involved and what intervention is most appropriate, so all deformities are corrected simultaneously (see list below). Getting the legs straight and ready to rehab for these patients is critical for maintaining their ambulatory ability (see Figure 1 below). Among the things we do as orthopedic surgeons, helping a child walk longer, straighter, and more confidently is one of the most rewarding, and with the help of our Cerebral Palsy Program team, we hope to optimize function for these kids for the entirety of their childhood and beyond.
Example list of impairments and planned interventions for a patient after taking into account all elements of the diagnostic matrix:Sagittal plane
Problem
- Hip flexor contractures 15-20 degrees
- Knee flexion contractures 25-30 degrees
- Patella alta/extensor lag
Solution
- Bilateral hop flexor releases
- Bilateral distal femoral extension osteotomies
- Bilateral patellar tendon advancements
Axial Plane
Problem
- Mild femoral IR 30 degrees ante
- Severe Tibial IR 35-40 degrees
Solution
- Femoral derotation through extension osteotomies
- Bilateral tibial derotation osteotomies
Coronal Plane
Problem: Hip adduction contracture R>L
Solution: Adductor tenotomies


Figure 1: Preoperative clinical photos (top), showing the knee fl exion contractures and severe internal tibial torsion, which are corrected postoperatively (bottom), with the knee now coming to full extension and the foot pointing forward. All of the deformities were corrected simultaneous to allow for immediate upright posture and a single rehab course.
Reference and suggested reading
The Diagnostic Matrix. From: Davids JR, Ounpuu S, DeLuca PA, Davis RB 3rd. Optimization of walking ability of children with cerebral palsy. Instructional Course Lectures. 2004 ;53:511-522.
Contact us
Orthopedic Center