One Becomes Two: Abby and Erin’s Journey to Separation
One Becomes Two: Abby and Erin’s Journey to Separation
Two months after their marriage, Heather and Riley were delighted to learn Heather was expecting. Their first prenatal ultrasound showed that they were having twins. That wasn’t a complete surprise: Heather has sisters who are identical twins. The huge surprise that followed? The babies were connected.

While reviewing the ultrasound, their doctor noticed that the babies’ heads were very close together, so close that they might be conjoined. He advised them to see a specialist in nearby Charlotte, N.C., and they made an appointment for the following Monday.
The specialist confirmed that the twins were joined at the top of their heads, a connection type called craniopagus conjoined twins. Craniopagus is the least common type of conjoined twins, accounting for only about 2 percent of cases.
At that point, it was too soon to tell how the babies would develop and whether they might be candidates for separation surgery. It would depend, in large part, on whether they shared brain tissue. Their growth would need to be monitored in periodic ultrasounds for the next few weeks.
If separation turned out to be a possibility, the specialist recommended Children’s Hospital of Philadelphia (CHOP). Doctors at CHOP had separated 23 pairs of conjoined twins since 1957, more than any other hospital in the Western Hemisphere. That level of experience is what led their doctor to refer the couple there, and it is what convinced the couple to put their trust in CHOP.
Candidates for separation
At the 19-week ultrasound, Heather and Riley learned that their twins were girls. The doctor also gave them some hopeful news: the twins did not appear to share any part of their brains, which improved their outlook for separation. Heather had already been in touch with Richard D. Wood Jr. Center for Fetal Diagnosis & Treatment at CHOP, and with this new information she set up an appointment for the following week.
The couple drove the 11 hours to Philadelphia. Over two days, Heather had a series of tests, including a high-resolution fetal ultrasound, a fetal MRI and a fetal echocardiogram to look at the babies’ hearts.
“We met with genetic counselors, psychologists, surgeons, maternal-fetal medicine specialists,” Heather recalls. “Everybody was trying to find the best way to care for our girls when they were born.” After all the tests and meetings, they sat down in a conference room with Gregory Heuer, MD, PhD, a neurosurgeon, and Nahla Khalek, MD, MPH, a maternal-fetal medicine specialist.
Dr. Heuer explained that girls had separate brains, but they shared a portion of the main vein that drains blood from the brain during circulation: the sagittal sinus. The fact that they shared a part of this vein added risk to the separation. He wanted them to understand that there was a possibility that they could lose one or even both of their daughters.
Though there was still uncertainty and fear, Heather and Riley felt confident they were in good hands.
Welcoming Abby and Erin
Heather began traveling to Philadelphia every two weeks for appointments. When an ultrasound at the 26-week appointment showed that the girls’ umbilical cords had become entangled, the medical team advised her to stay in Philadelphia so they could monitor the babies more closely. She moved to the Ronald McDonald House in Camden, N.J., then was admitted to CHOP’s Garbose Family Special Delivery Unit, for mothers expecting babies with medical problems who will need immediate specialized care after delivery.
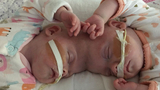
Abby and Erin were born on July 24, 2016, ten weeks premature. They each weighed 2 pounds, 1 ounce. “They did much better than anybody anticipated,” Heather says. “The team had been prepared for breathing tubes and all sorts of things for them, but when they were born, they came out crying.”
The twins were cared for in the Newborn/Infant Intensive Care Unit (N/IICU) at CHOP for the next seven months. Nurses worked with Heather to figure out a way to hold them. Though they made an awkward bundle, she and Riley both soon mastered the technique.
Once they were born, doctors could get a clearer picture of precisely how the twins were joined. Dr. Heuer brought in Jesse Taylor, MD, a pediatric plastic surgeon, as his surgical partner. Together, they came up with an approach that would involve a series of procedures.
Steps toward separation

In October, they operated on the twins to cut through the bone where the skulls were joined, and to place a device that would be used to gradually push the two apart. Called “distraction,” the process would add one or two millimeters of separation a day. Similar procedures had been used successfully in other types of reconstructive surgery, but this was a new technique in the separation of conjoined twins. The distraction process added more than an inch of separation.
Over the next five months, the girls had several more surgeries as steps toward separation, including the placement of tissue expanders below the skin where their heads were joined. Like water balloons, the expanders were gradually filled with fluid to slowly stretch the skin. The extra skin was needed to cover the gap when the twins were separated.
While the surgical team worked and planned, Heather and Riley and the rest of the medical team took care of the twins, who were growing wonderfully. Over the next few months they hit all the major developmental milestones, rewarding their parents with their first smiles in November.
The physical and occupational therapy team at CHOP found creative ways to help the twins continue to develop, despite being conjoined. One innovation was a specially built swing large enough to hold both girls.
It was a major milestone when the twins were released from the N/IICU after seven months. They moved to a room upstairs in the hospital. For the first time, their parents could take them out into the halls and even outdoors. In a blog entry, Heather described their first taste of fresh air: “It was glorious. Watching their little faces squint as the sun shone on them was a moment I want to remember forever. The wind would blow and they would gasp and then smile.”
One becomes two: The separation surgery

On June 6, 2017, more than 10 months after they were born, the girls were separated during an 11-hour surgery. A team of approximately 30 people, including surgeons, nurses, anesthesiologists and other staff, worked together during this complex, high-risk surgery.
Each baby was monitored by a separate anesthesiology team, led by Alison Reed Perate, MD, and Matthew Pearsall, MD.
Three neurosurgeons worked for hours to separate the blood flow between the two girls. This required cauterizing blood vessels and separating their shared dura, the covering of the brain that lies under the skull. They found that the girls did share a small amount of brain tissue, and they separated this as well.
More than halfway through the surgery, the teams flipped the girls, and the surgeons began the same painstaking process from the other side.
As expected, separation of the sagittal sinus, the large vessel that carries blood from the brain to the heart, was the most difficult part of the surgery. After a few very tense hours, with the whole team working to keep the girls alive despite significant blood loss, the girls were finally separated. The time was 8:43 p.m.
After the separation, the surgical team divided into two, one for each of the girls. The teams used artificial material to replace missing dura (the thick outer membrane surrounding the brain), and the stretched skin created by the expanders was sewn to cover the gap.
The hardest work was done, but there were many ups and downs in the weeks after the surgery, as the girls slowly recovered.
What comes next for the girls?
As soon as their conditions permitted it, Erin and Abby began intensive physical and occupational therapy at CHOP. On July 24, they celebrated their first birthday, receiving more than 300 cards from people around the world.
And on Nov. 20, 2017, after 485 days in the Hospital, Erin and Abby were discharged to return home to North Carolina — just in time for Thanksgiving.
Over the next few years, the twins will need additional plastic and reconstructive surgery to replace the missing bone areas at the tops of their heads and to normalize their hairlines and minimize scarring. But after spending more than a year at CHOP, their parents are just thrilled to have them home.
“The girls are inspiring,” Heather says. “It’s very neat for me to be their mom and to be able to have a front row seat to this and watch them overcome these incredible obstacles. We cannot wait to see what their future holds!”
Originally published October 2017
Updated: November 2017