What are conjoined twins?
Conjoined twins are twins that are born with their bodies physically connected. Conjoined twins occur once in every 50,000 to 60,000 births. Approximately 70 percent of conjoined twins are female, and most are stillborn.
Approximately 75 percent of conjoined twins are joined at least partially in the chest and share organs with one another. If they have separate sets of organs, chances for surgery and survival are greater than if they share the same organs. As a rule, shared heart conjoined twins cannot be separated.
Doctors at Children's Hospital of Philadelphia have separated 32 sets of conjoined twins and have managed the care of many others whose separation was not surgically possible. We have diagnosed and delivered more conjoined twins than any hospital in the world.
Our experience with conjoined twins
- More than 133 sets of conjoined twins referred to the CFDT
- 72 pairs prenatally evaluated
- 32 pairs successfully separated
Numbers reflect data as of February 2025 at Children's Hospital of Philadelphia.
Evaluation and diagnosis
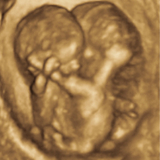
Conjoined twins are typically diagnosed early in pregnancy with prenatal ultrasound. The optimal evaluation period for additional prenatal testing is after 18 weeks gestation.
A thorough prenatal evaluation is particularly important for conjoined twins, as the location and extent of where the twins are joined and what organs are shared play a crucial role in deciding whether the twins will be separable.
Expectant mothers visiting the Center for Fetal Diagnosis and Treatment at CHOP will undergo a full day of advanced imaging. This helps us to collect a detailed picture of the shared organs and any associated problems. Prenatal diagnosis will help identify the optimal treatment and delivery plan, and the potential for separation after birth.
The following imaging tests are used to diagnose and evaluate conjoined twins:
- Fetal ultrasound: a safe, non-invasive procedure that uses high-frequency sound waves to provide detailed high-resolution images, including 3-D and 4-D views. Our team of board-certified radiologists uses highly specialized equipment to ensure the best images possible are obtained.
- Fetal echocardiogram: a noninvasive ultrasound procedure that assesses the structure and function of the fetal heart. Fetal echocardiogram is the most important test for the evaluation of conjoined twins, as it determines if the twins share a heart and if so, where that connection occurs.
- Ultrafast fetal MRI: an imaging technique pioneered at Children's Hospital that can include 3-D MRI reconstruction. It requires no sedation of the mother or muscle relaxants for the fetus to obtain images. Used with the ultrasound images, the fetal MRI adds another level of detail.
Indicators of conjoined twins include lack of a separating membrane between the twins, inability to separate the fetal bodies, and constant position of the fetal heads.
At the end of the day, expectant parents will meet with a multidisciplinary team to discuss the results of your tests, and outline all options for prenatal management, delivery, and treatment so that your family can make an informed decision about how to move forward. After the visit, our team will also contact your referring physician to provide details about the consultation.
Connection patterns
The prognosis for conjoined twins depends on where the twins are connected.
Conjoined twins are generally classified in three ways:
- 75 percent are joined at the chest wall or upper abdomen (thoracopagus and omphalopagus)
- 23 percent are joined at the hips, legs, or genitalia (pygopagus and ischiopagus)
- 2 percent are joined at the head (craniopagus)
The common twin types include:
Thoracopagus: the most common type of conjoined twin, which along with omphalopagus, represents about 75 percent of cases. The two babies lie face to face and share a common sternum, diaphragm, and upper abdominal wall. In cases of conjoined hearts at the ventricular (pumping chamber) level, there are no known survivors.
Omphalopagus: the least-complicated connection, usually considered a subgroup of thoracopagus. The babies face one another and are joined at the anterior abdominal wall from the xiphoid to the umbilicus. The peritoneal cavity of one tends to be joined with the other, but upper intestinal tracts are usually separate. In the majority of cases, a bridge of the liver connects the infants.
Pygopagus: represents about 20 percent of cases, joined at the buttocks and perineum, facing away from each other. A significant length of the sacrum may be fused, and as a result, the twins often share the sacral spinal canal. A single lower rectum and anus is common, and often the lower genital tract and external genitalia are fused.
Ischiopagus: represents less than 5 percent of cases, the connection occurs at a single bony pelvis. Four normal legs may be attached, but often two of the four are fused into one malformed limb. The intestinal tracts often join and empty into a single colon.
Craniopagus: the least common type of conjoined twins, accounting for 2 percent of cases, is represented by fusion of the skull. The twins often share large dural sinuses and vascular structures. Rarely, the brains are separated by bone and each brain has separate leptomeninges. In others, the brains are connected, or separated only by arachnoid, making separation extremely difficult and dependent upon a superior sagittal sinus for each brain.
For the duration of the pregnancy, the Center team will work closely with your referring obstetrician to ensure comprehensive prenatal monitoring. In some cases, care will be transferred to the Center around 28 weeks' gestation or earlier to optimize the management of the pregnancy and prepare for delivery.
Planning for delivery
Patients carrying conjoined twins have the option of delivering in CHOP’s Garbose Family Special Delivery Unit, the world's first birthing unit dedicated to mothers carrying babies with known birth defects. The SDU offers unmatched continuity of care for both mother and baby, with complete labor and delivery services in immediate proximity to the care your babies will need after birth — neonatal intensive care, cardiac intensive care, pediatric operating rooms, and more.
Delivering in a location with direct access to all the advanced, specialized services both mom and baby might need is particularly important for high-risk conjoined twin pregnancies that require a C-section or a potential ex utero intrapartum therapy (EXIT) delivery. The EXIT procedure is a "partial delivery" in which the fetus is partially removed from the uterus but remains attached to the circulation carried by the umbilical cord and placenta so that surgeons can correct airway blockages before performing a full delivery.
After delivery
A comprehensive post-delivery assessment will determine the long-term plan for a potential separation surgery. While some life-threatening conditions may require immediate emergency surgery, a full assessment of shared structures should be performed before separation is attempted. Comprehensive evaluation of the cardiovascular system is particularly important in determining if separation is an option.

Tour our Fetal Center
Watch this video tour to learn what to expect at your first visit to the Wood Center for Fetal Diagnosis and Treatment.
Separation surgery
If the conjoined twins are candidates for separation surgery, CHOP’s pediatric surgical team (which may include general surgeons, plastic and reconstructive surgeons, neurosurgeons, and other surgical specialties) will work with a multidisciplinary team to monitor the babies and determine the timeline and approach for the surgical procedure. Specialists involved in your care will likely include neonatologists, cardiologists, advanced practice nurses, and maternal-fetal medicine specialists, among others.
One of the many procedures required to prepare twins for separation is the insertion of tissue expanders to increase the skin surface available to cover exposed tissue after surgery.
As separated twins recover after surgery, they are closely followed by nutritionists, developmental pediatricians, and other specialists to ensure their ability to thrive and grow.
When the conjoined twins share a heart, successful surgical division is usually not possible.
Separation success rates
Since 1995, 133 pairs of conjoined twins have been referred to the Center for Fetal Diagnosis and Treatment, and 72 pairs have undergone prenatal evaluation. Not all conjoined twins are candidates for separation, and the success rates for separating conjoined twins vary depending on the connection.
Children’s Hospital of Philadelphia has successfully separated 32 pairs of conjoined twins, the first in 1957.
Additional resources: MacKenzie TC, Crombleholme TM, Johnson MP, Schnaufer L, Flake AW, Hedrick HL, Adzick NS. The natural history of prenatally diagnosed conjoined twins. Journal of Pediatric Surgery 37:303-309, 2002.
Resources to help
Conjoined Twins Resources
Richard D. Wood Jr. Center for Fetal Diagnosis and Treatment Resources
Learning your baby has a birth defect is a life-changing experience. We want you to know that you are not alone. To help you find answers to your questions, we've created this list of educational health resources.
Reviewed by Holly L. Hedrick, MD, FACS