Pediatric Proton Therapy Center
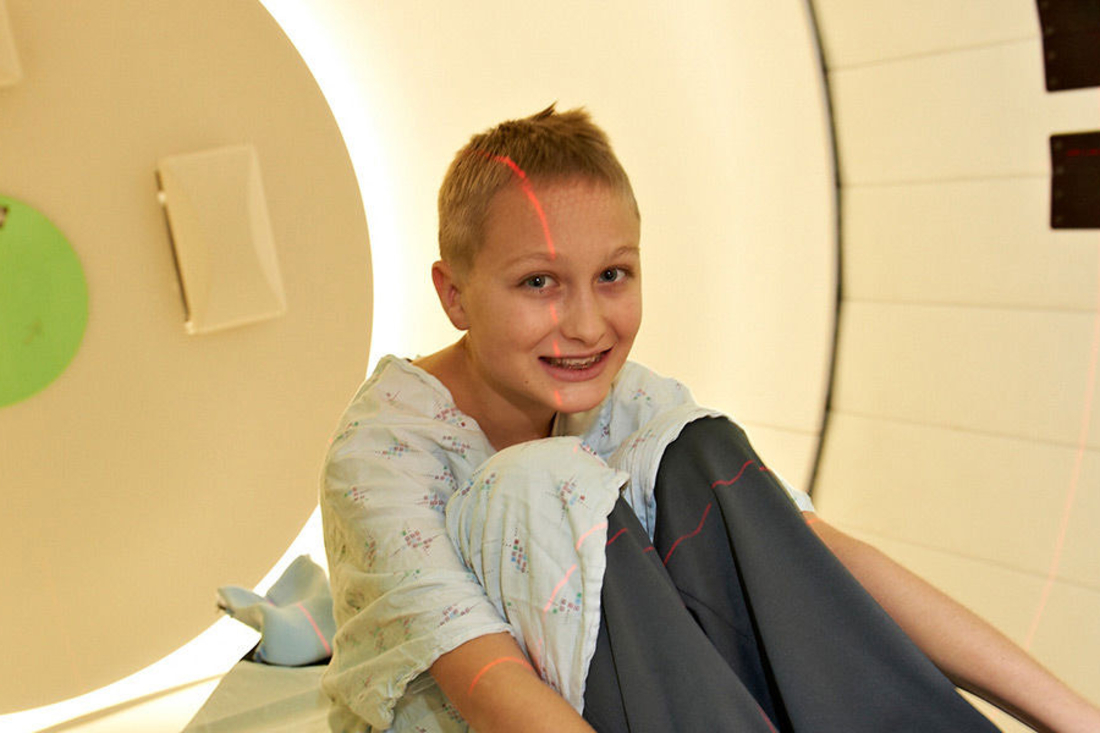
For your child with cancer, your hope is that treatment is not only effective but also safe, with few long-term side effects. Proton therapy’s greatest benefit is that it delivers radiation doses directly to your child’s tumor, minimizing damage to surrounding healthy tissue.
CHOP's Cancer Center offers one of the most experienced pediatric proton therapy programs, in collaboration with Penn Medicine. The Roberts Proton Therapy Center is designed to be child-friendly, from the waiting areas to the private treatment rooms.
The benefits of proton therapy are especially important to children. Less damage to healthy tissue — especially tissue in organs like the brain, heart, lungs and eyes — means better chances of overall health.
How we serve you
Conditions we treat
Proton therapy can be part of the treatment plan for many types of cancer.
-
Brain and central nervous system tumors - Astrocytoma
- Atypical teratoid rhabdoid tumors (ATRT)
- Craniopharyngioma
- Ependymoma
- Germ cell tumors (choriocarcinoma, teratoma, germinoma)
- Glioma (glioblastoma, low-grade glioma)
- Medulloblastoma
- Meningioma
- Optic nerve tumors
- Optic pathway/hypothalamic glioma
- Pinoblastoma
- Primitive neuro-ectodermal tumor (intracranial PNET)
-
Chondrosarcoma - Chordoma
-
Ewing sarcoma - Head and neck carcinomas (parotid, nasopharyngeal)
-
Neuroblastoma -
Osteosarcoma -
Retinoblastoma -
Rhabdomyosarcoma -
Soft tissue sarcomas -
Tumors of the head and neck -
Wilms' tumor -
Hodgkin lymphoma -
Non-Hodgkin lymphoma

Why choose us
Our Proton Therapy Center offers the most advanced proton beam technology. We are at the cutting edge of new technology and treatment techniques, many of which were developed by scientists here. Our team combines this expertise with compassion and skill to make every step as easy and comfortable as possible for your child.
Meet your team
Your child will be cared for by a world-class teams of pediatric proton therapy specialists. Every member of the team understands the unique needs of children with cancer.

Pediatric Proton Therapy Center location
Get information about the Perelman Center for Advanced Medicine.

Pediatric Proton Therapy Center resources
We have gathered resources to help you find answers to the questions you might have about pediatric proton therapy.
Events

Parkway Run & Walk, presented by Citadel Credit Union
Sunday, Sep 28, 2025

Preparing your child for proton therapy
Before your child begins proton therapy treatment, they will undergo an extensive evaluation so our team of experts can plan their treatment.
Give to the Cancer Center
There are many ways to support CHOP's Cancer Center. A gift of any size can help us make life-changing breakthroughs and advance our work for children everywhere.


