Medical imaging is frequently obtained prior to surgery to clarify anatomic relationships and the extent of pathology. While radiologists have developed expertise in interpreting 2-dimensional (2D) images and visualizing 3-dimensional (3D) structures, surgeons more readily relate to 3-dimensional images corresponding to their physical examination and the surgical appearance of the body.
Often 3D anatomical renderings are created from 2D source images and are included in imaging studies such as bone computed tomography (CT) and contrast-enhanced vascular imaging. Dynamic imaging that captures physiologic movement or blood flow can be sequentially displayed or superimposed to create a time-course series that depicts organ perfusion or changing anatomic relationships over time.
The Children’s Hospital Additive Manufacturing for Pediatrics (CHAMP) Lab was started in 2017 in the Department of Radiology to:
- Create simulation models to help trainees learn procedural skills
- Create patient-specific models to enable surgeons to plan complex surgical procedures
- Design and prototype pediatric-specific biomedical devices
The CHAMP Lab is run by Elizabeth Silvestro, MSE, and Raymond Sze, MD, MAMS.
Over the last year, the CHAMP Lab has created numerous 3D models to aide in the surgical care of patients with complex congenital anomalies and tumors. The modeling process begins when images are obtained during clinical CT and MRI examinations. Imaging examinations are tailored to the clinical question and optimized for printing. For some patients and indications this means obtaining images in arterial, venous, and delayed phases of contrast enhancement; at other times intracavitary contrast is administered to distend and define body cavities, such as the bladder or bowel.
Following the examination, the images are reviewed and the relevant anatomy is identified and segmented to create a dynamic PDF. The PDF can be manipulated so the structures are viewed from different vantage points, added or subtracted from the image to better understand anatomic relationships. After reviewing this document with the surgeon, a 3D model can be printed to facilitate presurgical discussion among team members and for intraoperative reference.
This method allows the surgeon to plan for the best surgical approach to maximize outcomes while minimizing complications.

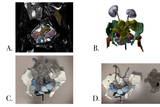
As an example, a young patient had a large recurrent Wilms tumor in the middle of a solitary kidney, dangerously close to the main blood supply to the kidney and pressing on the collection system. The 3D model (see Figure 7) allowed the urologist to preoperatively and repeatedly review the anatomy from multiple viewpoints, increasing his familiarity with the patient’s anatomy. Enabling surgeons to hold the model in their own hands is extremely valuable and a major advantage over volumetric displays on a computer monitor. The 3D model clarified the arterial supply to the tumor, which was only distinctly visible when viewed in the coronal split of the model and also from the back of the kidney, views that would not be feasible intraoperatively. During the surgery, this allowed the surgeon to recognize this arterial supply though a small surgically created window near the renal hilum and tie off the blood supply early, minimizing blood loss and enabling the surgeon to perform a partial nephrectomy to preserve the function of the remaining kidney.
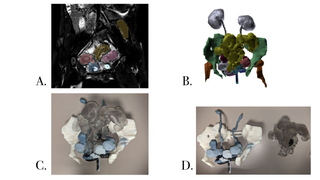
Figure 8 (A, B, C, D): 3D modeling process of a teenage girl with a history of cloacal exstrophy.
A. Coronal T2 weighted magnetic resonance image of the pelvis. Parts of her anatomy are shaded in different colors as part of the segmenting process.
B. 3D image from the dynamic PDF created from her MRI.
C. 3D model printed in grayscale.
D. The bowel (printed in clear) could be snapped in and out of the model.
Contributors also included Elizabeth Silvestro, MSE
Featured in this article
Specialties & Programs
Medical imaging is frequently obtained prior to surgery to clarify anatomic relationships and the extent of pathology. While radiologists have developed expertise in interpreting 2-dimensional (2D) images and visualizing 3-dimensional (3D) structures, surgeons more readily relate to 3-dimensional images corresponding to their physical examination and the surgical appearance of the body.
Often 3D anatomical renderings are created from 2D source images and are included in imaging studies such as bone computed tomography (CT) and contrast-enhanced vascular imaging. Dynamic imaging that captures physiologic movement or blood flow can be sequentially displayed or superimposed to create a time-course series that depicts organ perfusion or changing anatomic relationships over time.
The Children’s Hospital Additive Manufacturing for Pediatrics (CHAMP) Lab was started in 2017 in the Department of Radiology to:
- Create simulation models to help trainees learn procedural skills
- Create patient-specific models to enable surgeons to plan complex surgical procedures
- Design and prototype pediatric-specific biomedical devices
The CHAMP Lab is run by Elizabeth Silvestro, MSE, and Raymond Sze, MD, MAMS.
Over the last year, the CHAMP Lab has created numerous 3D models to aide in the surgical care of patients with complex congenital anomalies and tumors. The modeling process begins when images are obtained during clinical CT and MRI examinations. Imaging examinations are tailored to the clinical question and optimized for printing. For some patients and indications this means obtaining images in arterial, venous, and delayed phases of contrast enhancement; at other times intracavitary contrast is administered to distend and define body cavities, such as the bladder or bowel.
Following the examination, the images are reviewed and the relevant anatomy is identified and segmented to create a dynamic PDF. The PDF can be manipulated so the structures are viewed from different vantage points, added or subtracted from the image to better understand anatomic relationships. After reviewing this document with the surgeon, a 3D model can be printed to facilitate presurgical discussion among team members and for intraoperative reference.
This method allows the surgeon to plan for the best surgical approach to maximize outcomes while minimizing complications.

As an example, a young patient had a large recurrent Wilms tumor in the middle of a solitary kidney, dangerously close to the main blood supply to the kidney and pressing on the collection system. The 3D model (see Figure 7) allowed the urologist to preoperatively and repeatedly review the anatomy from multiple viewpoints, increasing his familiarity with the patient’s anatomy. Enabling surgeons to hold the model in their own hands is extremely valuable and a major advantage over volumetric displays on a computer monitor. The 3D model clarified the arterial supply to the tumor, which was only distinctly visible when viewed in the coronal split of the model and also from the back of the kidney, views that would not be feasible intraoperatively. During the surgery, this allowed the surgeon to recognize this arterial supply though a small surgically created window near the renal hilum and tie off the blood supply early, minimizing blood loss and enabling the surgeon to perform a partial nephrectomy to preserve the function of the remaining kidney.

Figure 8 (A, B, C, D): 3D modeling process of a teenage girl with a history of cloacal exstrophy.
A. Coronal T2 weighted magnetic resonance image of the pelvis. Parts of her anatomy are shaded in different colors as part of the segmenting process.
B. 3D image from the dynamic PDF created from her MRI.
C. 3D model printed in grayscale.
D. The bowel (printed in clear) could be snapped in and out of the model.
Contributors also included Elizabeth Silvestro, MSE
Contact us
Department of Radiology