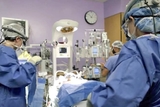
The Neonatal Surgical Team at Children’s Hospital of Philadelphia (CHOP), formed in 2004, is the first team of its kind in the United States. The team consists of neonatologists, surgical attendings, surgery fellows, bedside nurses and surgical nurse practitioners, all of whom specialize in the care of babies born with conditions that require surgery after birth, particularly congenital diaphragmatic hernia (CDH).
Babies with CDH are born in CHOP’s Garbose Family Special Delivery Unit (SDU). This unit is critically important in that it eliminates the detrimental risks of transport and provides immediate access to the team that will care for these fragile newborns.
Once stabilized, babies are taken to CHOP’s Level IV Harriet and Ronald Lassin Newborn/Infant Intensive Care Unit (N/IICU), which is close by the SDU. The Neonatal Surgical Team functions as a unit within a unit, providing care in a specially designated area within the N/IICU.
A unit within a unit
Every day, the Neonatal Surgical Team rounds on patients together and collaborates to make decisions around patient management. This model of a close working relationship between surgery and neonatology greatly improves patient management.
The team meets weekly with respiratory therapists, cardiologists, pulmonologists, pediatric anesthesiologists, ECMO specialists, nurses, nutritionists, social workers, child life therapists, and physical and occupational therapists to create a unified, cohesive, consistent path forward for each patient.
Getting babies to the point where they are ready for surgery can be a roller coaster, as blood gases can fluctuate from one hour to the next. Babies are placed on mechanical ventilation using a small lung volume/ rapid rate strategy allowing for permissive hypercapnia. If the baby requires escalation of support that may be damaging to fragile lungs, they are placed on extracorporeal membrane oxygenation (ECMO) at bedside in the N/IICU. Venoarterial ECMO is used to bypass the significant pulmonary hypertension seen in CDH.
Preparing for CDH repair
Once a child is strong enough to undergo repair of the diaphragmatic defect, the entire Neonatal Surgical Team comes to the baby’s bedside in the N/IICU, transforms the space into an operating room, and handles the surgery together as a team, from start to finish.
Diagnosis to Home
This avoids the stress of travel to and from the operating room, and reduces the need for transitions in care and handoffs. With a large, concentrated volume of neonatal surgical patients, the team has also been able to focus on the perioperative experience and has refined care of the surgical neonate by working closely with pediatric anesthesia colleagues.
After the diaphragm is surgically repaired, there are often still underlying issues including pulmonary hypoplasia and pulmonary hypertension that can necessitate a N/IICU stay of weeks to months. The postoperative course typically involves weaning sedation medications and mechanical ventilation as feeds are advanced.
After discharge, babies have regular visits to CHOP’s Pulmonary Hypoplasia Program (PHP) clinic, where they continue to be followed closely by an interdisciplinary team.
Continued advancements in CDH care
Congenital diaphragmatic hernia is a complex diagnosis that affects each child differently. Working together to co-manage care of a high volume of CDH patients over the past 15-plus years, the Neonatal Surgical Team has learned a great deal about the many ways the condition can impact babies.
Team members have become leaders in the field, creating CDH-specific care guidelines and collaborating with colleagues across the country and the world, many of whom have trained with the CHOP team and have gone on to replicate the team’s approach to care of surgical neonates at other centers.
Contributed by: Holly L. Hedrick, MD, Attending Pediatric and Fetal Surgeon, Surgical Director, ECMO Center, Co-director, Neonatal Surgical Team, and Director, Pulmonary Hypoplasia Program; Natalie E. Rintoul, MD, Attending Neonatologist, Co-director, Neonatal Surgical Team, and Medical Director, Neonatal ECMO Program; and Renee P. Ebbert, RN, MSN, CRNP, Manager, N/IICU Surgical Nurse Practitioners.
Featured in this article
Specialties & Programs

The Neonatal Surgical Team at Children’s Hospital of Philadelphia (CHOP), formed in 2004, is the first team of its kind in the United States. The team consists of neonatologists, surgical attendings, surgery fellows, bedside nurses and surgical nurse practitioners, all of whom specialize in the care of babies born with conditions that require surgery after birth, particularly congenital diaphragmatic hernia (CDH).
Babies with CDH are born in CHOP’s Garbose Family Special Delivery Unit (SDU). This unit is critically important in that it eliminates the detrimental risks of transport and provides immediate access to the team that will care for these fragile newborns.
Once stabilized, babies are taken to CHOP’s Level IV Harriet and Ronald Lassin Newborn/Infant Intensive Care Unit (N/IICU), which is close by the SDU. The Neonatal Surgical Team functions as a unit within a unit, providing care in a specially designated area within the N/IICU.
A unit within a unit
Every day, the Neonatal Surgical Team rounds on patients together and collaborates to make decisions around patient management. This model of a close working relationship between surgery and neonatology greatly improves patient management.
The team meets weekly with respiratory therapists, cardiologists, pulmonologists, pediatric anesthesiologists, ECMO specialists, nurses, nutritionists, social workers, child life therapists, and physical and occupational therapists to create a unified, cohesive, consistent path forward for each patient.
Getting babies to the point where they are ready for surgery can be a roller coaster, as blood gases can fluctuate from one hour to the next. Babies are placed on mechanical ventilation using a small lung volume/ rapid rate strategy allowing for permissive hypercapnia. If the baby requires escalation of support that may be damaging to fragile lungs, they are placed on extracorporeal membrane oxygenation (ECMO) at bedside in the N/IICU. Venoarterial ECMO is used to bypass the significant pulmonary hypertension seen in CDH.
Preparing for CDH repair
Once a child is strong enough to undergo repair of the diaphragmatic defect, the entire Neonatal Surgical Team comes to the baby’s bedside in the N/IICU, transforms the space into an operating room, and handles the surgery together as a team, from start to finish.
Diagnosis to Home
This avoids the stress of travel to and from the operating room, and reduces the need for transitions in care and handoffs. With a large, concentrated volume of neonatal surgical patients, the team has also been able to focus on the perioperative experience and has refined care of the surgical neonate by working closely with pediatric anesthesia colleagues.
After the diaphragm is surgically repaired, there are often still underlying issues including pulmonary hypoplasia and pulmonary hypertension that can necessitate a N/IICU stay of weeks to months. The postoperative course typically involves weaning sedation medications and mechanical ventilation as feeds are advanced.
After discharge, babies have regular visits to CHOP’s Pulmonary Hypoplasia Program (PHP) clinic, where they continue to be followed closely by an interdisciplinary team.
Continued advancements in CDH care
Congenital diaphragmatic hernia is a complex diagnosis that affects each child differently. Working together to co-manage care of a high volume of CDH patients over the past 15-plus years, the Neonatal Surgical Team has learned a great deal about the many ways the condition can impact babies.
Team members have become leaders in the field, creating CDH-specific care guidelines and collaborating with colleagues across the country and the world, many of whom have trained with the CHOP team and have gone on to replicate the team’s approach to care of surgical neonates at other centers.
Contributed by: Holly L. Hedrick, MD, Attending Pediatric and Fetal Surgeon, Surgical Director, ECMO Center, Co-director, Neonatal Surgical Team, and Director, Pulmonary Hypoplasia Program; Natalie E. Rintoul, MD, Attending Neonatologist, Co-director, Neonatal Surgical Team, and Medical Director, Neonatal ECMO Program; and Renee P. Ebbert, RN, MSN, CRNP, Manager, N/IICU Surgical Nurse Practitioners.
Contact us
Richard D. Wood Jr. Center for Fetal Diagnosis and Treatment