Urology Fellowship Training
The Division of Pediatric Urology at Children’s Hospital of Philadelphia (CHOP) values diversity and seeks talented fellowship applicants from varied backgrounds. The Division of Urology does not discriminate on the basis of race, color, ethnicity, sexual orientation or gender identity, religion, or disability.
About CHOP’s Pediatric Urology Fellowship Program
In 1976, Dr. John Duckett introduced the first fellowship in pediatric urology as he established the program for the Division of Urology. Since the beginning, the CHOP fellowship in pediatric urology consistently graduated future stars in pediatric urologic care and academia.
A few reasons why we attract the best candidates:
- Our fellow’s surgical volume is well over 1,000 cases each year, with unsurpassed complexity.
- There are four standard research track options available to our fellows after they complete their clinical year: an extensive basic science laboratory experience (one lab research year), clinical research including the Certificate Program in Clinical Epidemiology (one research year), a Master of Science in Clinical Epidemiology (MSCE) (two research years), or a Master in Translational Research (two research years).
- You make the choice about which research track you prefer. We will make it happen!
Until 1987, all fellowships in pediatric urology were one-year programs. Beginning in 1989, our Division has offered two- and three- year fellowship programs, with Dr. Stephen Zderic serving as CHOP’s first two-year fellow. Currently, the program is divided into a clinical year and a research year (with additional research years if desired).
Candidates often ask us what we are looking for in our fellows. Here are a few characteristics shared by CHOP fellows:
- Ability
- Affability
- Character
- Commitment
- Compassion
- Drive
- Integrity
- Intelligence
- Leadership
- Passion
- Respect
Fellowship program leaders
- Christopher J. Long, MD – Fellowship Program Director
- Thomas Kolon, MD – Division Chief
- Stephen Zderic, MD – Basic Science Research Director
- Arun Srinivasan, MD – Clinical Science Research Director
- Natalie Plachter, MHA, MSN, CRNP, CPNP – Director of Clinical Care
Additional faculty fellows will work alongside and learn from:
- Katherine Fischer, MD
- Karl Godlewski, MD
- Caleb Kovell, MD
- Sameer Mittal, MD, MSc
- Aseem Shukla, MD
- Gregory Tasian, MD, MSc, MSCE
- Jason Van Batavia, MD
- Dana Weiss, MD
- Mark Zaontz, MD
Fellowship goals
The pediatric urology fellow is representative of the CHOP Urology mission: “To be the world leader in the advancement of Urologic healthcare for children by integrating excellent patient care, innovative research and quality professional education into all of our programs”
The key goals of the Pediatric Urology Fellowship Program are to:
Develop collaborative clinical care expertise
- To lead the comprehensive care of children with urologic diseases, including but not limited to: reconstruction, andrology, uro-oncology, stone disease, chronic kidney disease, hypospadias, bladder exstrophy-epispadias complex, neuropathic bladder, and hydronephrosis, to pioneer new surgical techniques including minimally-invasive surgery and robotic surgery.
- To incorporate the role of medical and allied healthcare professionals in patient care with an interdisciplinary approach.
- To understand the role of community resources in the care of children with urologic diseases.
Foster independent basic science, translational and clinical investigation
- To offer formal post-doctoral course work in basic science, translational, and clinical research, in which each fellow can choose a path most in line with their interests and strengths.
- To provide mentoring to develop and complete innovative and feasible research projects.
- To ensure academic achievement by rigorously supervising academic progress.
- To provide an opportunity to present discoveries in presentations and publish those results.
Invest in the future of pediatric urology
- Bridge the gap between pediatric and adult care through our transitional urology program with the Hospital of the University of Pennsylvania, and CHOP attendings, including adult congenital urologist Dr. R. Caleb Kovell.
- To promote management skills for independent direction of a urology team, including formal participation in divisional quality and patient safety initiatives.
- To solidify research skills to further independent research careers.
- To foster mentoring skills to educate subsequent trainees.
- To cultivate leadership skills to advance the field of pediatric urology and patient care practices.
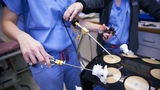
The pediatric urology fellow will be able to demonstrate competence in the various domains of Pediatric Urology, including proficiency in the following:
- Open surgery: Experience in all aspects of open surgery in the child with a urological problem. This includes major reconstructive renal, ureteral, bladder, and urethral surgery in the boy and in the girl. Genital surgery in both sexes as well as intersex surgery. Management of the fetus with a pediatric urological problem is also emphasized.
- Endoscopic surgery: Experience in endoscopic, including laparoscopic surgery. This should include diagnostic as well as therapeutic interventions for vaginal, urethral, vesical, and ureteral surgery.
- Outpatient pediatric urology: Experience in all aspects of outpatient care with graded responsibility.
- Spinal defects and neurourology: This includes the knowledge of the physiology and pharmacology of voiding dysfunction. This latter term includes obstructive and irritative phenomena, urinary incontinence and dysfunctional voiding. In addition, it includes knowledge of urodynamics, broadly defined as the data that relate to bladder and outlet parameters during the filling and emptying phases of micturition. It also includes the antenatal, newborn and subsequent care of children born with spinal defects.
- Pediatric andrology and differences of sex development (intersex): The long term care of children born with cryptorchidism or ambiguous genitalia or who develop a varicocele and the long term treatment to maximize fertility and minimize carcinoma formation for these children when they become adults.
- Stone disease: This includes endourology and lithotripsy. This includes the knowledge of the pathogenesis of urinary stone disease and the evaluation and management. Endourology and lithotripsy refer broadly to the specialized techniques used to treat some varieties of stone disease. Endourology further includes the use of special endoscopic techniques to diagnose and manage disorders of the upper urinary tract other than stone disease.
- Urologic trauma: This includes the evaluation and management of trauma to all parts of the genitourinary system in the male and female.
- Infectious disease: This includes a working knowledge of those factors involved in the pathogenesis of urinary infection, both lower and upper tract, of the bacteria, fungi, viral and other organisms involved, and of the various techniques used to diagnose and to treat infection. Expertise in the indications for specific use of antimicrobials and side effects of treatments are stressed.
- Reconstructive urology: This includes the use of innovative techniques for reconstruction of renal, ureteral, vesical, urethral, penile and vaginal congenital and acquired anomalies. This includes indications for and techniques for lower urinary tract reconstruction.
- Renal transplantation: This includes a working knowledge of the urologic factors involved in renal transplantation and their application. Also included is knowledge of the reconstruction required in the recipient born with bladder or ureteral congenital anomalies to provide for successful long-term function of the transplanted kidney.
- Urologic imaging: This broadly refers to all of those entities involved in the radiologic study of urologic disease including urography, retrograde upper tract studies, urethrography and cystography including imaging of the perineal anatomy in children born with intersex anomalies, urologic ultrasound, computerized tomography, magnetic resonance imaging, angiography, and the various types of interventional uroradiology.
The fellow will be able to work effectively in the aforementioned areas in a multidisciplinary setting.
A day in the life: Yearly routines
Weekly routine: Year 1
Each day begins with morning rounds at 6:30 a.m. and concludes with rounds in the evening. Fellows may have a case in the OR as early as 7:30 a.m. We emphasize the operating room experience in the first year. In subsequent years, fellows may have a light clinical schedule that will include an outpatient schedule and selected surgical cases to perform to increase independence both in and out of the operating room.
Each week there are several conferences and meetings for fellows to participate in, including:
- WEDNESDAY mornings: rotating Research Conference; Campbell’s Club; Faculty meeting
- WEDNESDAY evenings: Collaborative Urology/Radiology/Nephrology conference; dry (pre-op) rounds
- THURSDAY mornings: PENN Urology grand rounds
Sample Surgical Case List
Each year, CHOP Urology fellows consistently outperform the national averages and required surgical caseloads compared to other pediatric urologic fellowship programs across the nation. Below is a table showcasing the large number of procedures, including robotic cases, through which CHOP fellows will have the opportunity to learn and perform.
| Years | CHOP Fellow Total OR Cases | CHOP Fellow Total Index OR Cases | National Median Total Index OR Cases |
|---|---|---|---|
| 2019-2020 | 801 | 729 | 463 |
| 2020-2021 | 1,137 | 657 | 537 |
| 2021-2022 | 1,002 | 656 | 513 |
| 2022-2023 | 1,515 | 805 | 627 |
| 2023-2024 | 1,243 | 668 | 609 |
| As of 2024, the required Total Index OR Case minimum is 350. | |||
| Years | CHOP Minimally Invasive Surgery Cases | National Median Minimally Invasive Surgery Cases |
|---|---|---|
| 2019-2020 | 72 | 41 |
| 2020-2021 | 124 | 48 |
| 2021-2022 | 107 | 56 |
| 2022-2023 | 80 | 62 |
| 2023-2024 | 84 | 70 |
| As of 2024, the required Total MIS Case minimum is 20. | ||
Weekly routine: Year 2
The research year(s) for fellows offer a more flexible, less structured schedule. Fellows still participate in:
- Lab hours, Basic science/clinical research (if applicable)
- Travel for meetings
- Classes (if applicable)
- Clinical instruction in clinic/OR
- Wednesday conferences
- PENN Urology grand rounds/conferences
- Fellow call (split with the first year fellow)
Additional benefits and resources for fellows
Our team at CHOP has routinely supplied the fellows with:
- Custom fitted 4.5 x Loupes
- Computer, laptop, and appropriate software
- Cellphone
- Office space in both the laboratory and in the clinical office
- Adequate financial and tuition support in the clinic and the laboratory
- Travel expenses to meetings, including the annual US-India Bladder Exstrophy Collaborative Workshop
A day in the life: Follow along for a glimpse into the daily routine of a pediatric urology fellow at Children's Hospital of Philadelphia.
Didactic program
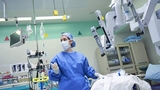
Each Wednesday evening, fellows and faculty from the Divisions of Urology, Radiology, and Nephrology convene for a case-based conference to review complex cases. With guidance from attending physicians, fellows will help plan an interdisciplinary approach for patient care. Fellows will learn invaluable management and critical thinking skills.
- Each Wednesday evening, the Division hosts a pre-operative planning meeting for upcoming cases (“Dry Rounds”). The clinical fellow helps to assign surgical cases for the upcoming week.
- On the first Wednesday morning of each month, fellows attend the Division Faculty meeting. Here we discuss safety, administrative, teaching, clinical and research strategy/organization and financials. This gives the fellows a valuable introduction to the process of running a division of pediatric urology
- On the 2nd and 3rd Wednesday mornings of each month, fellows attend the Division research meeting. In these meetings, members of the faculty discuss their current research projects and receive feedback from the other faculty members. At least twice a year the fellow will formally present their research at these meetings. This gives the fellows the opportunity to receive feedback from all of the faculty.
- Fellows with attendings teach a monthly Campbell’s Urology Textbook conference meeting to review specific pediatric urology research chapters.
- Every Thursday morning, fellows and faculty attend Urology Grand Rounds at the Hospital of the University of Pennsylvania with selected topics and lectures by esteemed medical professionals.
- The fellow is expected to attend the AUA and AAP meetings each year during fellowship. The fellow makes one or more presentations at the AUA meeting in the spring of the first and second year. Additionally, the fellow makes at least one presentation at the Society for Pediatric Urology (SPU) meeting in the fall of the second year of fellowship. Additional meetings are also possible depending on the fellows interest.
- Our faculty evaluates each fellow’s progress and competence at the end of 6 months, 12 months, 18 months, and 24 months of training, and as needed. Every 6 months during training, the fellow meets with the Division Chief and Program Director to review the evaluations. Fellows also provide feedback about their experience at each evaluation assessment.
- The fellow keeps a running log with academic projects assigned or undertaken, including research-focused projects (i.e. chapter, abstract, manuscript, lecture). Each month, logs will be reviewed to track progress.
- Fellows have the support of a clinical research coordinator and research team to meet their goals and facilitate data collection and analysis.
Duties and responsibilities of the pediatric urology fellow at CHOP
- Enforce the 80-hour work week regulations
- Oversee all aspects of the pediatric urology inpatient/consult service
- Scrub on all index cases, and any other cases as needed/desired
- Prepare and present at the Management Case Conference
- Ensure proper OR fellow/resident coverage
- Provide back-up call coverage for the residents
- Prepare and represent CHOP at annual meetings (ie. AUA, Pediatric Urology Fall Congress)
- Prepare monthly Campbell’s Urology Textbook conference
- Attend weekly Urology Research Meetings
- Attend weekly HUP Urology Grand Rounds
- Scrub with residents on more common cases (i.e. hernia, orchiopexy, circumcision, endoscopy)
- Participate in Outpatient Clinic as scheduled by the Nurse Manager and Program Director
- Attend Faculty meeting monthly
- Review the Wednesday Dry Rounds (preoperative) schedule
- Review the Wednesday Case Conference schedule
- Prepare and complete clinical (and/or basic science) research
- Competence in the area of service organization and management
- Competence in the area of practice based learning and improvement
- Teaching status in the attainment of interpersonal and communication skills
- Teaching status in the area of professionalism
- Teaching status in the area of systems based practice
- Teaching status in the area of the usage of knowledge and analytical thinking to address clinical questions
- Teaching status with respect to the management of in-house and emergency room consultants (with attending staff)
Testimonials from former fellows
“I was fortunate enough to do my pediatric training during urology residency at CHOP. When it came time to pick a program for fellowship, I naturally compared every other program to CHOP since I already knew it well. Though there are a lot of wonderful programs out there, I didn’t feel like anywhere else could offer me the same level of training as CHOP. The number and quality of attendings to learn from as well as the diversity, complexity, and volume of the patient population and operative cases at CHOP is simply unparalleled. I also loved that the CHOP fellowship allowed me to build the research year that I wanted to so that I could get the most out of it for my specific goals and research interests. Above all though, it is the people at CHOP who truly make the fellowship unique- they are the “special sauce” as Dr. Canning would say - with everyone focused on delivering the best patient care possible and teaching and mentoring the next generation of pediatric urologists. I wanted to ensure that when I finished fellowship, I would be prepared for a career in pediatric urology with the best training and skill set possible. Fellowship at CHOP certainly gave me that and more!” - Katherine Fischer, MD (CHOP Urology Fellow 2020-2022)
“I was a fellow here 20 years ago. Looking back at the fellowship's growth, the experience offered, case diversity, volume, etc., I am just astounded. I can't imagine that there is a training program that provides a more well-rounded experience. The opportunity to train with urologists of such skill and towering reputations was hard to pass up. Being a CHOP fellow immediately connected me with a network of alumni that have mentored and guided me along the path and opened doors and opportunities for global work, prestigious committees and societies, and research collaborations that I've leveraged throughout my career.” - Aseem Shukla, MD (CHOP Urology Fellow 2001-2004)
“After I finished [my fellowship] in 2014, I looked around at a number of programs and ultimately came back to CHOP. It provided the perfect environment and culture. It provided the resources to treat the most complex children and to develop a research program that is transformative for care in the future. The commitment to discovery permeates through every aspect of the Division of Urology. I am convinced the program we built and centers we developed can’t be done elsewhere. We have a remarkable infrastructure that allows us to bring what was once an idea to become operational and grow in the future. You will be pushed and will be able to meet your personal goals, and you will contribute to the legacy of the Division of Urology." - Gregory Tasian, MD, MSC, MSCe (CHOP Urology Fellow 2011-2014)
“The ability to learn how each attending operates and does a procedure was a great advantage to this program. We have a breadth of age ranges among our faculty, so you can see into the nuances of each generation and have a melting pot of techniques as you develop your own. CHOP also has a phenomenal basic science program led by Dr. Zderic. He’s one of the most outstanding people I’ve ever met in medicine. And a great thing about being associated with University of Pennsylvania is you can take classes and be supported by CHOP for extra years of learning. At CHOP you have a genuine quality of people and leaders...they’re good human beings and care about other people. That’s something I remember.” - Jason Van Batavia, MD (CHOP Urology Fellow 2015-2017)
“The Urology Fellowship Program has advanced in quantum leaps. We have new technology regarding minimally invasive surgery and robotics, and we have a better understanding of pathology of diseases. We have more faculty with a greater diversity in expertise and research. I wanted to have an academic career and work in a laboratory setting. Today, I get to come to the lab one to three days a week.” - Stephen Zderic, MD (CHOP Urology Fellow 1989-1991)
“The relationships with the patients and Urology staff are key to this fellowship. One of our former fellows and I still talk through complex cases and figure them out together. We take time to get to know each fellow and cultivate relationships that also allow us to provide the best patient care. If you want to have the best training and have fun, come here.” - Dana Weiss, MD (CHOP Urology Fellow 2012-2014)
Stories from MAGPIs: Hear from former and current CHOP Urology fellows about the history of the program, research and more.
Why CHOP is the Place to Train
The pediatric urology fellowship in the Division of Urology at Children's Hospital of Philadelphia is one of the best in the nation.
Where our fellows are now
One of our goals is to provide the tools for our employees to succeed once they graduate from our program. For over more than 45 years, we have had fellows come through the Division of Urology and become renowned physicians/surgeons, innovative researchers, program directors, and department chiefs. Below is a list of our previous fellows, including their years at CHOP and their highest academic appointment/current location.
- Howard J. Kaplan, MD, 1976-1977, Urologist, University of Maryland St. Joseph’s Medical Center, Towson, MD
- M. David Gibbons, MD, 1977-1978, Director of Pediatric Urology, Georgetown Medical Center; Associate Professor of Urology, George Washington University School of Medicine, Washington, DC
- James M. Betts, MD, 1978-1979, Chief of Surgery, Director, Trauma Services, UCSF Benioff Children’s Hospital, Oakland, CA
- Mark F. Bellinger, MD, 1979-1980, Pediatric urologist, Children’s Hospital of Pittsburgh of UPMC
- Dennis L. Hoover, MD, 1979-1980, Pediatric urologist, Tampa, FL… Children’s Urology Group and affiliated with St. Joseph’s Children’s Hospital - Tampa
- John M. Gazak, MD, 1980-1981, Pediatric urologist Huntsville, NC
- Michael Norris, MD, 1980-1981, Director, Pediatric Urology at Miller Children’s Hospital Long Beach, Los Alamitos, CA. Retired Colonel, US Army.
- Anthony A. Caldamone, MD, 1981-1982, Chief, Pediatric Urology, Hasbro Children’s Hospital, Professor of Surgery (Urology) and Pediatrics, Warren Alpert Medical School of Brown University, Program Director Urology Residency Program, Providence, RI
- William F. Tarry, MD, 1982-1983, Pediatric Urologist, Associate Professor, Surgery, University of Texas Medical Branch, Galveston, TX, West Virginia’s first pediatric urologist.
- Brent W. Snow, MD, 1983-1984, Division Chief, Urology, Primary Children’s Hospital; Professor of Surgery in Urology, University of Utah, Salt Lake City, UT
- Michael G. Packer, MD, 1984-1985, Pediatric Urologist, Abington-Jefferson Health, Private Practice, Voorhees, NJ
- Leon I. Smith-Harrison, MD, 1984-1985, Attending Pediatric Urologist, Chief of Staff, Board Member, Driscoll Children’s Hospital, Corpus Christi, TX
- William Hulbert, MD, 1985-1986, Attending Pediatric Urologist, Golisano Children’s Hospital; Associate Professor, Department of Urology and Pediatrics, University of Rochester, Rochester, NY
- J. Patrick Murphy, MD, 1986-1987, Former Chief, Pediatric Urology, Children’s Mercy, Kansas City, KS; Retired (2018)
- Jean G. Hollowell, MD, 1987-1988, Pediatric Urologist, Urological Institute of Northeastern New York; Associate professor of surgery (urology) and pediatrics, Albany medical Center, Albany, York
- Mark A. Rich, MD, 1988-1989, Chief, Pediatric Urology, Arnold Palmer Hospital for Children, Orlando, FL; Director of the pediatric urology residency program, Clinical Associate Professor, University South Florida, Tampa, FL
- Patrick C. Cartwright, MD, 1989-1990, Surgeon-in-Chief, Primary Children’s Hospital; Professor of Surgery in Urology, University of Utah, Salt Lake City, UT
- Stephen A. Zderic, MD, 1989-1991, Attending Pediatric Urologist, Children’s Hospital of Philadelphia, John W. Duckett, Jr. Endowed Chair in Pediatric Urology, Professor of Urology in Surgery, Perelman School of Medicine at the University of Pennsylvania, Philadelphia, PA
- David H. Ewalt, MD, 1990-1992, Associate Medical Director, Pediatric Urology, Cook Children’s Medical Center, Dallas, TX
- Laurence S. Baskin, MD, 1991-1993, Chief, Pediatric Urology, UCSF Benioff Children’s Hospital; Professor of Urology, University of California, San Francisco; Frank Hinman, Jr, MD, Distinguished Professorship in Pediatric Urology, San Francisco, CA
- Douglas E. Coplen, MD, 1992-1994, Division Chief, Pediatric Urology, St. Louis Children's Hospital, Associate Professor of Urology, Washington University in St. Louis School of Medicine, St. Louis, MO
- Harry P. Koo, MD, 1993-1995, Chief, Pediatric Urology, Joseph M. Sanzari Children’s Hospital, Professor of Urology, Hackensack Meridian School of Medicine at Seton Hall University, Hackensack, NJ
- Gregory E. Dean, MD, 1994-1996, Chief, Pediatric Urology, St. Christopher’s Hospital for Children, Philadelphia, PA, Associate Professor of Urology/Pediatrics Temple University/Temple Children's Medical Center
- William A. Kennedy, MD, 1995-1997, Chief, Pediatric Urology, Lucile Packard Children’s Hospital Professor of Urology, Stanford University School of Medicine Stanford, CA
- Andrew J. Kirsch, MD, 1996-1998, Chief, Pediatric Urology, Children’s Healthcare of Atlanta, Clinical Professor, Emory University School of Medicine, Atlanta, GA
- Christopher S. Cooper, MD, 1997-1999, Vice Chair, Senior Associate Dean for Medical Education, Professor of Urology, Professor of Pediatrics and Chief, Division of Pediatric Urology University of Iowa Healthcare, Iowa City, IA
- Joel C. Hutcheson, MD, 1998-2000, Pediatric Urologist, Pediatric Surgical Associates, Children’s Hospitals and Clinics of Minnesota, Minneapolis, MN, Associate Professor of Urology, Mayo Clinic, Rochester, MN
- Hsi-Yang Wu, MD, 1999-2002, Chief, Pediatric Urology, Hasbro Children’s Hospital, Professor of Surgery (Urology) and Pediatrics, Warren Alpert Medical School of Brown University, Program Director Urology Residency Program, Providence, RI
- J. Christopher Austin, MD, 2000-2002, Chief, Pediatric Urology, Doernbecher Children’s Hospital, Associate Professor, Surgery, Oregon Health and Science University School of Medicine, Portland, Oregon
- Michele Clement, MD, 2000-2003, Chief, Pediatric Urology, Lehigh Valley Health Network, Allentown, PA
- Aseem Shukla. MD, 2001-2004, Pediatric Urologist, Director of Minimally Invasive Surgery and Chairholder, Chair in Minimally Invasive Surgery, The Children’s Hospital of Philadelphia, Professor of Urology, Perelman School of Medicine at the University of Pennsylvania. Former Chief, Division of Urology
- Grace Hyun, MD, 2002-2005, Chief, Pediatric Urology, NYU Langone Hospital-Brooklyn, Clinical Associate Professor, Department of Urology, Mount Sinai School of Medicine
- Darcie Kiddoo, MD, 2003-2005, Pediatric Urologist, Associate Professor of Urology, University of Alberta, Edmonton, Alberta, CANADA
- Michael Nguyen, MD, 2003-2006, Division Chief, Urology, Phoenix Children’s Hospital, Adjunct Clinical Instructor of Urology, Mayo Clinic, Department of Urology, Scottsdale, AZ, Clinical Assistant Professor, Creighton University, Department of Urology, Omaha, NE, Clinical Assistant Professor, Division of Urology, University of Arizona College of Medicine – Phoenix
- Andy Chang, MD, 2004-2007, Vice Chief, Division of Pediatric Urology Children’s Hospital of Los Angeles, Assistant Professor of Clinical Surgery, Keck School of Medicine of USC
- Steve Kim, MD, MSCE, MBA, 2007-2010, Co-Founder, President and Chief Marketing & Strategy Officer, Voluware, Huntington Beach, CA
- Sarah Lambert, MD, 2008-2011, Pediatric Urologist, Yale New Haven Children’s Hospital, Associate Professor of Urology, Yale School of Medicine
- Kate Kraft, MD, 2009-2011, Pediatric Urologist, C.S. Mott Children’s Hospital, Clinical Associate Professor, Urology Residency Program Director, University of Michigan Dept of Urology
- Matthew Christman, MD, 2010-2012, Chief of Pediatric Urology, Commander, Medical Corps, United States Navy, Urology Residency Program Director, Associate Professor of Surgery, Uniformed Services University of the Health Sciences, Naval Medical Center San Diego, San Diego, CA
- Gregory Tasian, MD, MSc, MSCE, 2011-2014, Attending Pediatric Urologist, Children’s Hospital of Philadelphia, Associate Professor of Urology in Surgery, Associate Professor of Epidemiology in Biostatistics and Epidemiology, Perelman School of Medicine at the University of Pennsylvania
- Dana Weiss, MD, 2012-2014, Attending Pediatric Urologist, Children’s Hospital of Philadelphia, Assistant Professor of Urology in Surgery, Perelman School of Medicine at the University of Pennsylvania
- Christopher Long, MD, 2012-2015, Attending Pediatric Urologist, Children’s Hospital of Philadelphia, Assistant Professor of Urology in Surgery, Perelman School of medicine at the University of Pennsylvania
- David I Chu, MD, MSCE, 2014-2017, Attending Pediatric Urologist, Ann & Robert H. Lurie Children’s Hospital of Chicago, Assistant Professor of Urology, Northwestern University Feinberg School of Medicine
- Jason Van Batavia, MD, 2015-2017, Attending Pediatric Urologist, Children’s Hospital of Philadelphia, Assistant Professor of Urology in Surgery, Perelman School of Medicine at the University of Pennsylvania
- Diana K. Bowen, MD, 2016-2018, Attending Pediatric Urologist, Ann & Robert H. Lurie Children’s Hospital of Chicago, Assistant Professor of Urology, Northwestern University Feinberg School of Medicine
- Joan S. Ko, MD, 2017-2019, Attending Pediatric Urologist, Division of Pediatric Urology Children’s Hospital of Los Angeles, Assistant Professor of Clinical Urology, Keck School of Medicine of USC
- Sameer Mittal, MD, 2018-2020, Attending Pediatric Urologist, Division of Urology, Children’s Hospital of Philadelphia, Assistant Professor of Urology in Surgery, Perelman School of Medicine at the University of Pennsylvania
- John K. Weaver, MD, 2019-2022, Attending Pediatric Urologist, Rainbow Babies and Children's Hospital, Assistant Professor of Urology, Case Western Reserve University School of Medicine
- Katherine Fischer, MD, 2020-2022, Attending Pediatric Urologist, Division of Urology, Children’s Hospital of Philadelphia, Assistant Professor of Urology in Surgery, Perelman School of Medicine at the University of Pennsylvania
- Karl F. Godlewski, MD, 2021-2023, Attending Pediatric Urologist, Division of Urology, Children’s Hospital of Philadelphia, Assistant Professor of Urology in Surgery, Perelman School of Medicine at the University of Pennsylvania
- Maya R. Chandru, MD, PhD, 2022-2025, Attending Pediatric Urologist, Seattle Children’s Hospital, Assistant Professor of Urology, University of Washington
- Meghan F. Davis, MD, MPH, 2023-2025, Attending Pediatric Urologist, Division of Urology, Children’s Hospital of Philadelphia, Assistant Professor of Urology in Surgery, Perelman School of Medicine at the University of Pennsylvania
- Leah E. Beland, MD, 2024-2026, Current Pediatric Urology Research Fellow
- Tyler M. Gaines, MD, 2025-2027, Current Pediatric Urology Clinical Fellow
Basic science research opportunities
Both clinical research and basic science research tracks are available to the fellow. The fellow is expected to lead a research project, of either a clinical or basic science nature, during the last two years of the fellowship program.
50 Years of Innovation
The program ensures a meaningful, supervised research experience based on early establishment of a mentor appropriate for the fellow's interests. The fellow is guided into appropriate training in order to successfully complete a research project over the course of the three-year program. The fellow may choose a clinically-based research project for which several mentors are available through the Division of Urology or the fellow may choose a basic research laboratory-based project.
Basic science research lab
The basic science laboratory in the Division of Urology at CHOP started in 1988 when Dr. Michael Keating established a collaboration with Dr. Robert Levin, a PhD pharmacologist in charge of the urology research program at the University of Pennsylvania.
Their early research efforts centered on how bladder physiology changes with normal growth and development. Dr. Keating showed in the first CHOP laboratory science paper, that the neonatal rabbit bladder generates a much higher voiding pressure than the bladder of an older rabbit.
In 1989, in parallel to Keating’s work, Dr. John Duckett and Dr. Stephen Zderic established the first basic science program in the country dedicated to pediatric urology.
In 1995, the urology lab moved into brand new space on the 11th floor of the Abramson Research building where new CHOP Surgeon-in-Chief, Dr. N. Scott Adzick, established the Institute for Surgical Research. CHOP Urology also began to shift our focus from developmental physiology to the bladder response to outlet obstruction.
Led by Dr. Stephen Zderic, our laboratory research since 1994 has included:
- Unraveling the structural responses (collagen) to bladder outlet obstruction in the rabbit and mouse.
- Understanding the calcium stimulation loop at the cellular layer with bladder contraction.
- Understanding the expression of the components of the sarcoplasmic reticulum such as the sarcoplasmic endoplasmic reticulum calcium ATPase (SERCA) and the ryanodine channel. This basic model system proved to be the prime driver for 15 consecutive years of the NIH funded George O'Brien Urology research center at the University of Pennsylvania with the Division of Urology at CHOP serving as the central core lab (1998-2013).
- Developing a model of social stress and studying the effect of stress on bladder neurophysiology and contraction in the mouse.
- Understanding the brainstem drive and changes within Barrington’s Nucleus that result in stress pattern urination in the mouse.
- The effect of corticotropin releasing factor on Barrington’s Nucleus in the social stress model.
- The effect of cyclosporine A on this stress model.
- The relationship between bladder and brain signaling following bladder outlet obstruction in the rat (published in the proceedings of the National Academy of Sciences).
- Use of optogenetics to activate a select area of Barrington’s Nucleus to activate neurons known to stimulate stress patterns of micturition in the mouse. (Jack Lapides Essay Contest and NIH K grant).
Clinical research opportunities
Urology fellows have the choice of aligning their research in either the basic science lab or clinical investigation. For fellows with clinical research interests, there are several programs that have funding from NIH, PCORI, and the Pennsylvania Department of Health, including:
- Clinical outcomes research
- Machine learning of complex urologic data
- Comparative effectiveness studies
- Clinical epidemiology of benign urologic disease
- Microbiome of kidney stone disease
Additionally, fellows can work with urologic programs including, but not limited to minimally invasive surgery, hypospadias, bladder exstrophy-epispadias complex and reconstructive urology, neuropathic bladder, post-operative opioid usage, kidney stone disease, uro-oncology, uro-fertility, and Differences of Sex Development.
Once fellows identify their research interests, they can choose to work with one of our attending pediatric urologists.
Selected research projects fellows may join:
Under the guidance of Dr. Thomas Kolon as Division Chief and Dr. Chris Long as fellowship director, fellows have an opportunity to focus research and clinical research outcomes within uro-oncology, oncofertility, the CHOP Cryptorchidism Program and Adolescent Varicocele Program, as well as Difference of Sex Development.
Since 2018, the Division has worked extensively with the Children’s Hospital Additive Manufacturing for Pediatrics (CHAMP) Lab in the Department of Radiology printing 3D models of tumors within organs in the renal and bladder systems. These 3D models open the door to finding innovative ways to treat patients, resulting in faster surgery/less time under anesthesia, lower complications and, ultimately, organ preservation.
Using a library of more than 4000 testis biopsies on over 200 patients, we have examined closely the defects in germ cell maturation in the undescended testis (UDT). To date, this research has resulted in 20 published manuscripts, national and international lectures, as well as numerous research awards.
Additionally, CHOP Urology is part of an NIH-funded multi-institutional consortium assessing medical, surgical and psychological outcomes in children and families affected by atypical genitalia due to DSD.
With direction from Dr. Arun Srinivasan, fellows have three branches of research to partake in, including minimally invasive surgery and robotics, kidney stones and stone disease, and quality improvement.
The advantages to these research programs are the infrastructure and collaborative efforts. The Division has a dedicated staff of researchers to support fellows and faculty in their efforts. Along with this support, fellows will have research meetings and access to collaborations, such as the Pediatric Urology Robotic Study Group (PURS).
Dr. Srinivasan is leading quality improvement research work which has dramatically changed opioid use in outpatient surgery and carefully shifted antibiotic use in post-operative care. The goal is to lessen the rate of opioid prescriptions and the Division’s work is changing the way medications are prescribed post-op.
In addition, Gregory Tasian, MD, MSc, MSCE leads a research group that uses an epidemiologic framework, including randomized trials and multi-institutional observational studies, to examine the etiology of kidney stone disease and the comparative effectiveness of surgical interventions. Active projects include examination of metabolic pathways in the gut-kidney axis that could be targets for novel therapeutics to prevent kidney stones. Specifically, Dr. Tasian is investigating the impact of diet and antibiotic exposure on the gut microbiome and metabolites in the intestinal and urinary tract and their contribution to calcium kidney stones in children and adults. He is also performing prospective cohort studies to compare stone clearance and patients’ experiences after alternative surgical interventions for kidney stones. He also applies machine learning to improve understanding of the pathophysiology, diagnosis, risk stratification, and prediction of treatment responses of benign urological disease among children.
Dr. Tasian and his team have made the following discoveries:
- Characterized the rapid increase in kidney stone disease among children, adolescents, and young adult women.
- Defined the precise relationship between daily temperatures and kidney stone presentation, which has important implications for the impact of climate change on human health.
- Recently published the first evidence that oral antibiotics are associated with an increased risk of kidney stones. The risk was greatest for those exposed at younger ages, which could help explain the rapid increase in the incidence of nephrolithiasis among children.
- Found that lower renal parenchymal area was associated with an increased risk of end-stage renal disease in boys with posterior urethral valves. Collaborations with Yong Fan at the University of Pennsylvania determined that machine learning of ultrasound images accurately identified children with congenital urologic disease.
During his fellowship years, Dr. Tasian secured the following grants:
- Pediatric Hospital Epidemiology and Outcomes Research Training (PHEOT) Program
- Source: NIH
- Year awarded: 05/01/2010 - 04/30/2015
- Epidemiologic Trends in Pediatric Nephrolithiasis: Defining Incidence of Disease and the Prevalence, Efficacy, and Determinants of Alternative Management Strategies
- Source: NIH (Urologic Diseases in America Project)
- Year awarded: 01/01/2013 - 01/01/2015
- Renal Parenchymal Area: Development of a Novel Criterion for Predicting Kidney Failure in Children with Congenital Urologic Disease
- Source: Center for Pediatric Clinical Effectiveness (CHOP) (Pilot Grant)
- Year awarded: 05/15/2013 - 05/14/2014
- Societies of Pediatric Urology Research Grant
- Source: Society of Pediatric Urology
- Year awarded: 07/01/2014 - 06/30/2015
In addition to the works of Dr. Tasian and Dr. Zderic, several other faculty members completed their fellowship here at CHOP and focused their lab and clinical research efforts on the following:
- Aseem Shukla, MD
- Focus: Clinical outcomes research and long-term follow-up on primary obstructive megaureter and hypospadias; bladder and cloacal exstrophy outcomes; posterior urethral valves
- Awards: Basic Science Research Award, First Prize, American Association of Pediatrics (2002); Silver Award for UrologyHealth.org (2004)
- Christopher Long, MD
- Focus: Hypospadias surgical and clinical outcomes; urologic oncology, MIS outcomes, neurogenic bladder outcomes
- Awards: Research Scholar Program, Urologic Care Foundation (2012); Basic Science Prize, Society for Pediatric Urology Fall Congress (2014)
- Dana Weiss, MD
- Focus: Hypospadias surgical and clinical outcomes; urologic oncology, MIS outcomes, neurogenic bladder outcomes
- Awards: Research Scholar Award, Urology Care Foundation (2013), Hypospadias surgical and clinical outcomes; urologic oncology, MIS outcomes, neurogenic bladder outcomes
- Jason Van Batavia, MD, MTR
- Focus: Voiding dysfunction and bladder-brain connection in relation to urinating
- Awards: Research Scholar Award, Urology Care Foundation (2016); Best Clinical Prize Finalist, Pediatric Urology Fall Congress (2017); Best Science Prize – 2nd place, Pediatric Urology Fall Congress (2017)
- Sameer Mittal, MD, MSc
- Focus: minimally invasive approaches to urologic reconstruction, avoidance of narcotics/opioids after urologic surgery and pediatric urologic oncology outcomes
- Clinical Prize, 3rd Annual Hypospadias World Congress of the Hypospadias International Society (2019)
- Katherine Fischer, MD
- Focus: Non-neurogenic voiding dysfunction treatment & clinical outcomes; clinical outcomes in neurogenic bladder, hypospadias & testicular torsion; impact of social determinants of health on clinical outcomes in urology patients
- Awards: Research Scholar Program, Urologic Care Foundation (2021-2022)
- Karl Godlewski, MD
- Focus: Primary and redo hypospadias surgery, Bladder Exstrophy, minimally invasive urologic reconstruction
Research accolades, awards, honors
Former fellows and current attending physicians on staff, including Dr. Stephen Zderic, Dr. Chris Long, Dr. Dana Weiss and Dr. Jason Van Batavia, have, in addition to the rest of the attending staff, conducted innovative research supported through endowment and grants.
Under the leadership of Dr. Stephen Zderic, numerous pediatric urology fellows at CHOP have been awarded grants to support their research year of fellowship:
- NIH K12 (7 grant recipients)
- Urology Care Foundation of the AUA (formerly American Foundation for Urologic Disease) (5 recipients)
- NIH T32 grant (3 recipients)
- NIH CTSA KL2 (1 recipient)
- Societies for Pediatric Urology (1 recipient)
- Master of Science in Biostatistics and Clinical Epidemiology (MSCE) from University of Pennsylvania (3 recipients)
- Certificate in Biostatistics and Clinical Epidemiology from University of Pennsylvania (9 recipients)
Additional research honors include:
- Dr. Stephen Zderic was awarded the AUA Urology Care Foundation's inaugural John W. Duckett Pediatric Urology Research Excellence Award in 2010 for lifelong achievements and contributions to pediatric urologic research.
- Dr. Thomas Kolon was awarded the AUA Urology Care Foundation John W. Duckett Pediatric Urology Research Excellence Award in 2020 based on his andrology research.
- Dr. Jason Van Batavia was named a Rising Star in Urology by the AUA in 2019 based on his optogenetics research.
International clinical research fellowship
The Division of Urology at CHOP regularly hosts an international research fellow. The international fellows (in the past hailing from the Netherlands, Trinidad and Tobago, India and Iran, among other countries) spend their time at CHOP initiating and then developing independent clinical research programs spanning minimally invasive surgery to the repair of the bladder exstrophy complex. The fellows maintain the largest database in the world for pediatric robotic urological surgery, abstract data, perform statistical analyses and carry projects forward to presentation and writing. The international fellows have presented research at the most premier pediatric urology conferences in the United States and overseas (from Helsinki to Delhi) and their work has resulted in close to a dozen manuscripts published in peer-reviewed journals.
Most importantly, our international fellows have an immersive experience at one of the largest children's hospitals in the world. They participate in all clinical conferences, observe complex surgical procedures and often round with house staff. The fellows gain direct mentorship from pediatric urology experts and a deep understanding of the American healthcare ecosystem. Our fellows tell us that the insights and practice methodologies they gain while at CHOP inform and greatly improve their patient care back at home.
The U.S.-India Bladder Exstrophy Collaborative: World-class Care for More Children
The U.S.-India Bladder Exstrophy Collaborative serves children throughout Asia and Africa suffering from bladder exstrophy.
Select publications by CHOP fellows
This is a small selection of scholarly papers published by CHOP Urology Fellows. This collection showcases impactful work done by our trainees who are now attending physicians with CHOP’s Division of Urology.
Rohrmann D, Levin RM, Duckett JW, Zderic SA: The decompensated detrusor I: The effects of bladder outlet obstruction on the utilization of intracellular calcium stores. Journal of Urology 156(2 Pt 2):578-581, Aug. 1996
Austin JC, Chacko SK, DiSanto M, Canning DA, Zderic SA: A male murine model of partial bladder outlet obstruction reveals changes in detrusor morphology, contractility and Myosin isoform expression. Journal of Urology 172(4 Pt 1):1524-1528, Oct. 2004.
Lassmann, J., Sliwoski, J., Chang, A., Canning, DA, Zderic, SA: Deletion of one SERCA2 allele confers protection against bladder wall hypertrophy in a murine model of partial bladder outlet obstruction. Am J Physiol Regul Integr Comp Physiol. 2008 Jan;294(1):R58-65.
Rickenbacher, E, Baez, M., Leiser, S., Zderic, SA, Valentino, RJ: Impact of Overactive Bladder on the Brain: Central Sequelae of a Visceral Pathology. Proceedings of National Acad. Sciences USA, 2008 Jul. 105(30):10589-10594
Chang, A.C., Butler, S, Sliwoski, J., Valentino, R.J., Canning, D.A., Zderic, SA: Social stress in mice induces voiding dysfunction and bladder wall remodeling. Amer. J. Physiol. Renal 2009, Oct;297(4):F1101-8
Chang, A.Y., Sliwoski, J, Butler, S, Hearn, G, Lassmann, J, Chacko, S, Cannking D.A., Zderic, S.A.: Calcineurin mediates bladder wall remodeling following partial outlet obstruction. Am. J. Physiol. Renal Physiol. 2011, Oct;301(4):F813-22
Shukla Aseem R, Woodard Christopher, Carr Michael C, Huff Dale S, Canning Douglas A, Zderic Stephen A, Kolon Thomas F, Snyder Howard M: Experience with testis sparing surgery for testicular teratoma. Journal of Urology 171(1): 161-163, Jan. 2004.
Shukla Aseem R, Nguyen Trang, Zheng Yongmu, Zderic Stephen A, DiSanto Michael, Wein Alan J, Chacko Samuel: Over expression of smooth muscle specific caldesmon by transfection and intermittent agonist induced contraction alters cellular morphology and restores differentiated smooth muscle phenotype. Journal of Urology 171(5): 1949-1954, May 2004.
Patel Rakesh P, Shukla Aseem R, Snyder Howard M: The island tube and island onlay hypospadias repairs offer excellent long-term outcomes: A 14-year follow-up. Journal of Urology 172(4 Pt 2): 1717-1719, Oct. 2004.
Shukla Aseem R, Patel Rakesh P, Canning Douglas A: The 2-stage hypospadias repair: Is it a misnomer? Journal of Urology 172(4 Pt 2): 1714-1716, Oct. 2004.
Shukla Aseem R, Cooper Jeffrey, Patel Rakesh P, Carr Michael C, Canning Douglas A, Zderic Stephen A, Snyder Howard M: Prenatally detected primary megaureter: A role for extended follow-up. Journal of Urology 173(4): 1353-1356, Apr. 2005.
Denburg MR, Leonard MB, Haynes K, Tuchman S, Tasian G, Shults J, Copelovitch L: Risk of fracture in urolithiasis: A population-based cohort study using the health improvement network. Clinical Journal of the American Society of Nephrology 9(12): 2133-2140, Dec. 2014 Notes: (Epub Oct. 23, 2014).
Pulido JE, Furth SL, Zderic SA, Canning DA, Tasian GE: Renal parenchymal area and risk of ESRD in boys with posterior urethral valves. Clinical Journal of the American Society of Nephrology 9(3): 499-505, Mar. 2014 Notes: (Epub Dec. 5, 2013).
Tasian GE, Cost NG, Granberg CF, Pulido JE, Rivera M, Schwen Z, Schulte M, Fox JA: Tamsulosin and spontaneous passage of ureteral stones in children: A multi-institutional cohort study. Journal of Urology 192(2): 506-511, Aug. 2014 Notes: (Epub Feb. 8, 2014).
Tasian GE, Pulido JE, Gasparrini A, Saigal CS, Horton BP, Landis JR, Madison R, Keren R: Daily mean temperature and clinical kidney stone presentation in five U.S. metropolitan areas: A time-series analysis. Environmental Health Perspectives 122(10): 1081-1087, Oct. 2014 Notes: (Epub July 10, 2014).
Tasian GE, Pulido JE, Keren R, Dick AW, Setodji CM, Hanley JM, Madison R, Saigal CS: Use of and regional variation in initial CT imaging for kidney stones. Pediatrics 134(5): 909-915, Nov. 2014.
Abhijith SM, Nerli RB, Weiss D, Srinivasan AK: Laparoscopic retroperitoneal lymph node dissection for paratesticular rhabdomyosarcoma in older children/adolescents. Indian Journal of Surgical Oncology, 4(4): 341-344, Dec. 2013 Notes: Epub Aug. 28, 2013.
Weiss DA, Long CJ, Carr MC. Renal cystic dysplasia. Consultant for Pediatricians, accepted for publication, 2014.
Long CJ, Weiss DA, Kolon TF, Srinivasan AK, Shukla AR. Pediatric calyceal diverticulum treatment: An experience with endoscopic and laparoscopic approaches. Journal of Pediatric Urology 11(4):172 e1-6, Aug. 2015 (Epub May 21, 2015).
Weiss DA, Kadakia S, Kurzweil R, Srinivasan AK, Darge K, Shukla AR. Detection of crossing vessels in pediatric ureteropelvic junction obstruction: clinical patterns and imaging findings. Journal of Pediatric Urology 11(4):173 e1-5, Aug. 2015 (Epub May 27, 2015).
Weiss DA, Butler S, Fesi J, Long CJ, Valentino RJ, Canning DA, Zderic SA. Putting the past behind us: Social stress induced urinary retention can be overcome. Journal of Pediatric Urology 11(4):188-194, Aug. 2015 (Epub May 27, 2015).
Partridge EA, Canning DA, Long CJ, Peranteau WH, Hedrick JL, Adzick NS, Flake AW. Urologic and anorectal complications of sacrococcygeal teratomas: Prenatal and postnatal predictors. Journal of Pediatric Surgery 49(1):139-142, Jan. 2014 (Epub Oct. 8, 2014).
Long CJ, Butler S, Fesi J, Frank C, Canning DA, Zderic SA. Genetic or pharmacologic disruption of the calcineurin-NFAT axis prevents social stress induced voiding dysfunction in a murine model. Journal of Pediatric Urology Epub S1477, Apr. 14, 2014.
Sterling ME, Long CJ, Bosse KR, Bagatell R, Shukla AR. A rapid progression of disease after surgical excision of a malignant rhabdoid tumor of the bladder. Urology Epub Jan. 9, 2015.
Deutsch SA, Long CJ, Srinivasan AK, Wood JN. Child abuse mimic: Avulsion injury in a child with penoscrotal webbing. Pediatric Emergency Care. Pediatric Emergency Care Epub October 1, 2015.
Long CJ, Weiss DA, Kolon TF, Srinivasan AK, Shukla AR. Pediatric calyceal diverticulum treatment: An experience with endoscopic and laparoscopic approaches. Journal of Pediatric Urology, Epub May 21 2015.
Van Batavia JP, Kolon TF: Fertility in disorders of sex development: A review. Journal of Pediatric Urology 12(6): 418-425, Dec. 2016 Notes: EPub Nov. 23, 2016.
Van Batavia Jason P, Shukla Aseem R, Joshi Rakesh S, Reddy Pramod P: Pediatric urology and global health: Why now and how to build a successful global outreach program. Urologic Clinics of North America 45(4): 623-631, Nov. 2018 Notes: Epub Sept. 7, 2018.
Van Batavia JP, Crowley TB, Burrows E, Zackai EH, Sanna-Cherchi S, McDonald-McGinn DM, Kolon TF: Anomalies of the genitourinary tract in children with 22q11.2 deletion syndrome. 2017 Pediatric Urology Fall Congress, Montreal, Canada Sept. 2017 Notes: Podium presentation.
Van Batavia JP, Tong CB, Chu DI, Kawal T, Srinivasan AK: Laparoscopic inguinal hernia repair by modified peritoneal leaflet closure: Description and initial results in children. Journal of Pediatric Urology 14(3): 272.e1-272.e6, June 2018 Notes: Epub. Mar. 13, 2018
Van Batavia Jason P, Combs Andrew J, Fast Angela M, Glassberg Kenneth I: Overactive bladder (OAB): A symptom in search of a disease - Its relationship to specific lower urinary tract symptoms and conditions. Journal of Pediatric Urology 13(3): 277.e1-277.e4, June 2017 Notes: Epub Mar. 10, 2017
Mittal S, Hyacinthe N, Tan C, Weiss D, Tasian G, Van Batavia J, Zderic S, Shukla A, Kolon T, Srinivasan A, Canning D, Zaontz M, Long C: Quantifying glans width changes with and without testosterone in patients undergoing hypospadias repair. Podium Presentation at the 3rd Annual Hypospadias World Congress of the Hypospadias International Society, Philadelphia, PA, Oct. 30-Nov. 1, 2019 2019.
Mittal, S, Shukla, A, Sahadev, R, Lee, S, Siu, S, Gale, E, Plachter, N, Srinivasan, A: Reducing post-operative opioids in children undergoing outpatient urologic surgery: a quality improvement initiative. Journal of Pediatric Urology, 2020.
Mittal, S, Srinivasan, A, Bowen, D, Fischer K, Shah, J, Weiss, D, Long, C, Shukla, A: Utilization of robot-assisted surgery for the treatment of primary obstructed megaureters in children. Urology 2020
Mittal, S, El-Ali, A, Shah, J, Lawton, B, Back, S, Long C, Kolon, T: Is the renal nephrometry score reducible and predictive for pediatric renal tumors? Podium Presentation at the American Urologic Association and Society of Pediatric Urology Annual Meeting, May 2020.
Mittal, S, Weaver, J, Siu, S, Gruccio, D, Van Batavia, J, Srinivasan, A, Long, C, Pyle, L, Bamba, V, Kolon, T: Deferring gonadectomy in patients with Turner syndrome with a genetic Y component is not a safe practice. Podium Presentation and Clinical Prize Finalist at the American Urologic Association and Society of Pediatric Urology Annual Meeting, May 2020.
How to apply
Our pediatric urology fellowship seeks physicians who will have completed training in an accredited U.S. or Canadian urology residency program in order to sit for the American Board of Urology certifying examination. The Division of Urology accepts one ACGME pediatric urology fellow per year for a two or three year fellowship. The deadline for application submission is February 15.
- Navigate to the Societies for Pediatric Urology website to register for the Pediatric Urology Fellowship Match and complete a Universal Application.
- Each applicant is required to send three letters of recommendation, including one from the department chair, along with the Universal Application.
- Based on the application, a candidate may be invited to interview with the Division of Urology. The candidate will tour the Children’s Hospital of Philadelphia main campus and will meet with faculty.
Timeline for 2026 Fellowship:
- Mid-November 2024: Registration for match opens
- Late January 2025: Interview invitation emails sent to candidates
- Saturday evening, March 8, 2025: Social gathering with current fellows (Optional if your schedule permits)
- Sunday, March 9, 2025: Interviews / Dinner
- At this time, we are planning a hybrid interview process with both an in-person interview and a virtual option for candidates unable to attend in-person. All candidates will be evaluated equally regardless of interview type. We will help to defray the cost of visiting us in Philadelphia for candidates by booking an overnight stay at the Inn at Penn.
- Mid-May 2025: Rank list begins
- Early June 2025: Rank list deadline
- Late June 2025: Match results released
Candidates are also encouraged to explore these videos: day in the life of a urology fellow, what sets the CHOP Urology Fellowship apart.
Other requirements
To carry out its mission, it is of critical importance for the Children’s Hospital of Philadelphia (CHOP) to keep our patients, families and workforce safe and healthy and to support the health of our global community. In keeping with this, CHOP has mandated all workforce members (including trainees) on site at any CHOP location for any portion of their time be vaccinated for COVID-19 as a condition of employment.
This mandate also applies to workforce members or trainees performing work for CHOP at non-CHOP locations. Additionally, all workforce members based in or regularly scheduled to work at any New Jersey location are mandated to be both vaccinated and boosted for COVID-19, with booster timing consistent with applicable guidelines. The CHOP COVID-19 vaccine mandate is in alignment with applicable local, state and federal mandates. CHOP also requires all workforce members and trainees who work in patient care buildings or who provide patient care to receive an annual influenza vaccine. Employees may request exemption consideration for CHOP vaccine requirements for valid religious and medical reasons. Please note start dates may be delayed until candidates are fully immunized or valid exemption requests are reviewed. In addition, candidates other than those in positions with regularly scheduled hours in New Jersey, must attest to not using tobacco products.
Children's Hospital of Philadelphia is an equal opportunity employer. We do not discriminate on the basis of race, color, gender, gender identity, sexual orientation, age, religion, national or ethnic origin, disability, protected veteran status or any other protected category. CHOP is a VEVRAA Federal Contractor seeking priority referrals for protected veterans.
CHOP is committed to building an inclusive culture where employees feel a sense of belonging, connection, and community within their workplace. We are a team dedicated to fostering an environment that allows for all to be their authentic selves. We are focused on attracting, cultivating, and retaining diverse talent who can help us deliver on our mission to be a world leader in the advancement of healthcare for children.
We strongly encourage all candidates of diverse backgrounds and lived experiences to apply.