Severe Congenital Neutropenia: Emma’s Story
Severe Congenital Neutropenia: Emma’s Story
At 4 months old, Emma got an ear infection and fever she just couldn’t beat. As several days passed with no improvement, Emma became more and more lethargic. A trip to the local emergency department resulted in ear drops that weren’t effective. At a return trip the next day, Emma’s bloodwork showed dangerously low levels of white blood cells. Leukemia was mentioned — terrifying her parents — but a different diagnosis made several days later, after Emma was admitted to Children’s Hospital of Philadelphia (CHOP), was just as alarming.
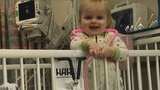
The local emergency department sent Emma and her parents, Lisa and Jeremy, to CHOP, where an oncologist quickly ruled out cancer. The diagnosis, however, remained elusive for a few days. “She was being seen by a team of hematologists and oncologists,” says Lisa. “They take such an interest in each case — you feel like you’re the only one they’re caring for.”
Emma was found to have severe congenital neutropenia, a very rare condition marked by a shortage of neutrophils, a type of white blood cell that helps fight infections. Emma’s care was directed by a team at CHOP’s Pediatric Comprehensive Bone Marrow Failure Center, part of the Division of Hematology. Bone marrow failure syndromes are diagnostically and therapeutically challenging. They occur when the bone marrow — the soft, spongy material in the center of the bones — doesn’t produce enough healthy blood cells to keep up with the body’s needs. The failure can occur with red blood cells, which carry oxygen throughout the body, platelets, which help blood to clot, or as in Emma’s case, white blood cells.
When the family was told about the disease and how it can turn an infection into a life-threatening situation, “We didn’t take it well,” says Lisa. “She couldn’t fight infections and she was very sick.” That initial stay at CHOP lasted 11 days, during which time Emma began getting injections that would stimulate her bone marrow to produce neutrophils.
The family’s new lifestyle
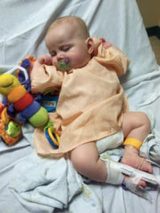
Once Emma was home, she needed to continue to get daily injections, a job Jeremy took on. “We had to give her a shot every day, and we knew it would be a while before she responded,” Lisa explains. Because Emma was so vulnerable, Lisa adds, “We had a new lifestyle: Everything had to be clean, everyone had to wash their hands. We were very isolated. We didn’t have a life because I was too worried.”
The ear infection that started everything had been so bad, it destroyed Emma’s left eardrum and three inner-ear bones. She’s partially deaf in that ear and wears a hearing aid — “Or we attempt to get her to wear it,” Lisa says with a small laugh.
After two weeks at home, Emma developed a fever and a skin infection, sending the family back to CHOP to be admitted for a few days. It was a pattern that repeated itself several times. One hospitalization occurred just before Emma’s baptism day. Luckily, they were cleared to be discharged in time for the big event. “That was my first outing with her since she was diagnosed,” says Lisa. “I told everyone you can look, but you can’t touch her — or even breathe on her!”
Her sister is a donor match
Every two weeks, Emma had an appointment at CHOP. The medication was helping, but the dose needed to be increased again and again — not an ideal solution for a tiny baby. A bone marrow transplant was suggested, and the family met with Timothy S. Olson, MD, PhD, Medical Director of the Blood and Marrow Transplant Program.
Emma’s sister Lilly, who was then 5 years old, was tested and found to be a 100% match. “Anything less would not have been good enough,” says Lisa. When Emma was 17 months old, in April 2014, the bone marrow transplant was performed.
The day of the transplant, Lilly enjoyed being the center of attention. “She got to be pushed in a wheelchair around the hospital, and everyone told her she was doing something great for her sister,” says Lisa. “She wanted to help, but she was too young to really understand what was happening. When Emma got that shot every night, Lilly would be there with us to sing to her and calm her down. So she knew the goal was to not have to give Emma that shot every night. But the magnitude of it? No.”
A steady recovery

In the beginning, Emma’s white blood cell counts were slow to rise, but incremental improvements reassured her care team. After a few months, her family noticed changes for the better in how Emma looked and acted. At the one-year mark after transplant, her neutrophils level was good, but her T cells still needed to build up. “We could breathe free at two years post-BMT,” says Lisa. In April 2019, 6-year-old Emma began being seen at the Cancer Survivorship Clinic — not because she ever had cancer, but because this clinic’s team members are experts in the care of children who have undergone a bone marrow transplant.
Although Emma’s care team has changed, Lisa still relies on Ellen M. Levy, RN, MSN, CRNP, a nurse practitioner in the Cancer Center: “She’s my go-to when I have a concern. I still text Ellen to this day. She’s not on our team, but I can still go to her, which means so much.” For Emma’s ongoing hearing issues, she sees Ken Kazahaya, MD, MBA, Associate Director of the Division of Otolaryngology.
Emma has blossomed after spending her first years very isolated. “She is an active child,” Lisa says. Emma plays softball and enjoys helping out with her cousin’s horses. “She took swimming lessons — that was a big step for us, because it was a community pool.” And Emma’s personality is blossoming: “She loves helping others and taking care of people,” says Lisa. “She’s very compassionate.”