
Today, Abby and Erin Delaney are able to sit independently from one another, be held separately in their mother and father’s arms, and can practice rolling over and crawling. Such everyday actions are extraordinary for the twin girls, because up until June 6, they were connected at the head. Abby and Erin were successfully separated at Children's Hospital of Philadelphia and are in the recovery phase of their treatment — continuing to amaze their family and care team with their resilience and determination.
Born in CHOP’s Garbose Family Special Delivery Unit (SDU), the 16-month-old girls, from Mooresville, N.C., have spent their entire lives living in the Hospital, until recently when Erin was discharged from CHOP. Abby still remains in the Hospital.
“Nearly five months after separation, we are happy to announce that both Erin and Abby Delaney are doing well as they continue to recover from this very complex surgery,” said neurosurgeon Gregory Heuer, MD, PhD, who co-led a multidisciplinary team alongside plastic and reconstructive surgeon Jesse Taylor, MD. In total, approximately 30 individuals helped carry out the complex 11-hour surgery. It was the 24th time that doctors at CHOP separated a pair of conjoined twins, more than any other hospital in the Western Hemisphere.
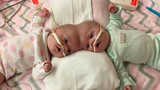
“This is one of the earliest separations of craniopagus conjoined twins ever recorded,” said Dr. Taylor. “We know that children heal better and faster the younger they are, therefore our goal for Erin and Abby was separation as soon as possible with minimum number of surgeries.”
“Although this has been a long journey, with many ups and downs, Riley and I are thrilled to see how well the girls are doing today,” said Heather Delaney, the twins’ mother. “We are so grateful for the Children’s Hospital of Philadelphia team, and for the support and encouragement that our families, our friends and the community have given us during this long journey.”
Watch this video to hear the girls’ story first-hand, as told by their parents and members of their medical team.
After a prenatal diagnosis, preparing for separation
Heather and Riley Delaney were told during a prenatal ultrasound that the twins they were expecting were joined at the top of their heads, a connection type called craniopagus conjoined twins. Craniopagus is the least common type of conjoined twins, accounting for only about 2 percent of cases. They were quickly referred to the Center for Fetal Diagnosis & Treatment at CHOP for prenatal care and delivery. Abby and Erin were born by C-section on July 24, 2016, in CHOP’s SDU, a unique unit exclusively for mothers carrying fetuses with known birth defects. The girls were 10 weeks premature, each weighing two pounds and one ounce.
Once the babies were born, Dr. Heuer and Dr. Taylor could get an even clearer picture of precisely how the twins were joined and developed a plan that would involve a series of procedures over the several months, ultimately culminating in the separation surgery.
In October 2016, they operated on the twins to cut through the bone where the skulls were joined, and to place a device that would be used to gradually push the two apart. Called “distraction,” the process would add one or two millimeters of separation a day. Similar procedures had been used successfully in other types of reconstructive surgery, but this was a new technique in the separation of conjoined twins. The distraction process added more than 2 centimeters of separation.
Over the next five months, the girls had several more surgeries as steps toward separation, including the placement of tissue expanders below the skin where their heads were joined. Like water balloons, the expanders were gradually filled with fluid to slowly stretch the skin. The extra skin was needed to cover the gap when the twins were separated.
While the surgical team worked and planned, Heather and Riley and the rest of the medical team took care of the twins. The physical and occupational therapy team at CHOP found creative ways to help the twins continue to develop, despite being conjoined. One innovation was a specially built swing large enough to hold both girls.
Complex separation surgery lasts over 11 hours

Months of preparation culminated during the early morning hours of June 6, 2017, as the anesthesiology team, led by Alison Reed Perate, MD, and Matthew Pearsall, MD, began to prepare the twins for their separation surgery.
Dr. Taylor first removed the skin expanders. Next, three neurosurgeons, including Dr. Heuer, worked for hours to separate the blood flow between the two girls. This required cauterizing blood vessels and separating their shared dura, the covering of the brain that lies under the skull. They found that the girls did share a small amount of brain tissue, and they separated this as well. More than halfway through the surgery, the teams flipped the girls, and the surgeons began the same process from the other side.
More About Conjoined Twins
As expected, separation of the sagittal sinus, the large vessel that carries blood from the brain to the heart, was the most complex part of the surgery. The girls were finally separated at 8:43 p.m. The surgeons then used artificial material to replace missing skin, and sewed the stretched skin created by the expanders to cover the gap.
“The ability to plan and carry out this type of surgery is testament to the skill and expertise available here at Children’s Hospital of Philadelphia,” said N. Scott Adzick, MD, CHOP’s Surgeon-in-Chief. “I’m extremely proud of Dr. Heuer, Dr. Taylor and the entire CHOP team, and I’m thrilled that Erin and Abby have a promising future because their courageous parents entrusted their daughters to our care.”
Recovery continues

Following the separation surgery, Abby and Erin recovered in CHOP’s Pediatric Intensive Care Unit, later moving to other units of the hospital and finally to CHOP’s rehab unit for more intensive occupational and physical therapy. The girls were closely followed by their surgeons, nutritionists, developmental pediatricians, and other specialists to ensure they received the best clinical care to thrive and grow. On July 24, they celebrated their first birthday, receiving more than 300 cards from people around the world.
Over the next few years, the twins will need additional plastic and reconstructive surgery to replace the missing bone areas at the tops of their heads and to normalize their hairlines and minimize scarring. For now, after spending more than a year at CHOP, their parents are preparing to take them home to North Carolina sometime later this year.
“The girls are inspiring,” said Heather. “As their parents, it is very neat for Riley and me to have a front row seat to this and watch them overcome these incredible obstacles. We cannot wait to see what their future holds!”
Featured in this article
Specialties & Programs
Today, Abby and Erin Delaney are able to sit independently from one another, be held separately in their mother and father’s arms, and can practice rolling over and crawling. Such everyday actions are extraordinary for the twin girls, because up until June 6, they were connected at the head. Abby and Erin were successfully separated at Children's Hospital of Philadelphia and are in the recovery phase of their treatment — continuing to amaze their family and care team with their resilience and determination.
Born in CHOP’s Garbose Family Special Delivery Unit (SDU), the 16-month-old girls, from Mooresville, N.C., have spent their entire lives living in the Hospital, until recently when Erin was discharged from CHOP. Abby still remains in the Hospital.
“Nearly five months after separation, we are happy to announce that both Erin and Abby Delaney are doing well as they continue to recover from this very complex surgery,” said neurosurgeon Gregory Heuer, MD, PhD, who co-led a multidisciplinary team alongside plastic and reconstructive surgeon Jesse Taylor, MD. In total, approximately 30 individuals helped carry out the complex 11-hour surgery. It was the 24th time that doctors at CHOP separated a pair of conjoined twins, more than any other hospital in the Western Hemisphere.

“This is one of the earliest separations of craniopagus conjoined twins ever recorded,” said Dr. Taylor. “We know that children heal better and faster the younger they are, therefore our goal for Erin and Abby was separation as soon as possible with minimum number of surgeries.”
“Although this has been a long journey, with many ups and downs, Riley and I are thrilled to see how well the girls are doing today,” said Heather Delaney, the twins’ mother. “We are so grateful for the Children’s Hospital of Philadelphia team, and for the support and encouragement that our families, our friends and the community have given us during this long journey.”
Watch this video to hear the girls’ story first-hand, as told by their parents and members of their medical team.
After a prenatal diagnosis, preparing for separation
Heather and Riley Delaney were told during a prenatal ultrasound that the twins they were expecting were joined at the top of their heads, a connection type called craniopagus conjoined twins. Craniopagus is the least common type of conjoined twins, accounting for only about 2 percent of cases. They were quickly referred to the Center for Fetal Diagnosis & Treatment at CHOP for prenatal care and delivery. Abby and Erin were born by C-section on July 24, 2016, in CHOP’s SDU, a unique unit exclusively for mothers carrying fetuses with known birth defects. The girls were 10 weeks premature, each weighing two pounds and one ounce.
Once the babies were born, Dr. Heuer and Dr. Taylor could get an even clearer picture of precisely how the twins were joined and developed a plan that would involve a series of procedures over the several months, ultimately culminating in the separation surgery.
In October 2016, they operated on the twins to cut through the bone where the skulls were joined, and to place a device that would be used to gradually push the two apart. Called “distraction,” the process would add one or two millimeters of separation a day. Similar procedures had been used successfully in other types of reconstructive surgery, but this was a new technique in the separation of conjoined twins. The distraction process added more than 2 centimeters of separation.
Over the next five months, the girls had several more surgeries as steps toward separation, including the placement of tissue expanders below the skin where their heads were joined. Like water balloons, the expanders were gradually filled with fluid to slowly stretch the skin. The extra skin was needed to cover the gap when the twins were separated.
While the surgical team worked and planned, Heather and Riley and the rest of the medical team took care of the twins. The physical and occupational therapy team at CHOP found creative ways to help the twins continue to develop, despite being conjoined. One innovation was a specially built swing large enough to hold both girls.
Complex separation surgery lasts over 11 hours

Months of preparation culminated during the early morning hours of June 6, 2017, as the anesthesiology team, led by Alison Reed Perate, MD, and Matthew Pearsall, MD, began to prepare the twins for their separation surgery.
Dr. Taylor first removed the skin expanders. Next, three neurosurgeons, including Dr. Heuer, worked for hours to separate the blood flow between the two girls. This required cauterizing blood vessels and separating their shared dura, the covering of the brain that lies under the skull. They found that the girls did share a small amount of brain tissue, and they separated this as well. More than halfway through the surgery, the teams flipped the girls, and the surgeons began the same process from the other side.
More About Conjoined Twins
As expected, separation of the sagittal sinus, the large vessel that carries blood from the brain to the heart, was the most complex part of the surgery. The girls were finally separated at 8:43 p.m. The surgeons then used artificial material to replace missing skin, and sewed the stretched skin created by the expanders to cover the gap.
“The ability to plan and carry out this type of surgery is testament to the skill and expertise available here at Children’s Hospital of Philadelphia,” said N. Scott Adzick, MD, CHOP’s Surgeon-in-Chief. “I’m extremely proud of Dr. Heuer, Dr. Taylor and the entire CHOP team, and I’m thrilled that Erin and Abby have a promising future because their courageous parents entrusted their daughters to our care.”
Recovery continues

Following the separation surgery, Abby and Erin recovered in CHOP’s Pediatric Intensive Care Unit, later moving to other units of the hospital and finally to CHOP’s rehab unit for more intensive occupational and physical therapy. The girls were closely followed by their surgeons, nutritionists, developmental pediatricians, and other specialists to ensure they received the best clinical care to thrive and grow. On July 24, they celebrated their first birthday, receiving more than 300 cards from people around the world.
Over the next few years, the twins will need additional plastic and reconstructive surgery to replace the missing bone areas at the tops of their heads and to normalize their hairlines and minimize scarring. For now, after spending more than a year at CHOP, their parents are preparing to take them home to North Carolina sometime later this year.
“The girls are inspiring,” said Heather. “As their parents, it is very neat for Riley and me to have a front row seat to this and watch them overcome these incredible obstacles. We cannot wait to see what their future holds!”
Contact us
Ashley Moore
Richard D. Wood Jr. Center for Fetal Diagnosis and Treatment