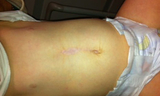
What is omphalocele?
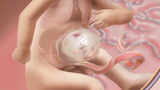
Omphalocele is a rare birth defect that occurs in 1 in 4,000 — 7,000 live births. It is a type of abdominal wall defect in which the bowel, liver and other abdominal organs extend into the abdomen near the base of the umbilical cord.
What causes omphalocele?
Omphalocele occurs very early in pregnancy when the abdominal wall fails to form normally. During typical fetal development, the intestines extend outside the fetal abdomen into the umbilical cord, then return back into the abdomen by about 11 weeks of gestation. If this process does not occur, an omphalocele develops.
No specific genetic mutation has been shown to cause an abdominal wall defect, and most cases of omphalocele are sporadic, meaning there is no history of other relatives with this diagnosis. However, omphalocele is a feature of many genetic syndromes, and affected individuals may have additional birth defects associated with these genetic changes.
What does this mean for my baby?
The prognosis for a baby with an omphalocele largely depends on the size of the herniation and the presence or absence of other birth defects.
More than half of all babies born with omphalocele have other birth defects, including brain, spine, heart, gastrointestinal issues or genitourinary problems. Omphalocele can also be seen alongside abnormalities involving the abdomen, heart, sternum and diaphragm, which are associated with a rare syndrome called pentalogy of Cantrell. Genetic anomalies commonly seen with omphaloceles include abnormalities of chromosome number, such as trisomy 18, or genetic syndromes such as Beckwith-Wiedemann syndrome.
A small omphalocele contains only bowel. This can also be referred to as “cord hernia,” where the fetal abdomen closes but a small loop of bowel remains in the umbilical cord. Small omphaloceles may be associated with higher incidence of chromosomal abnormalities.
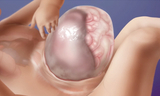
A large or “giant” omphalocele contains most of the liver and other abdominal organs. The fetal organs extend outside the abdomen and are covered by a thin membrane called a sac. Large omphaloceles are more likely to be associated with small fetal lung size (pulmonary hypoplasia), which can impact the amount of respiratory support the baby requires as well as the length of hospital stay after delivery. Up to one third can also have a heart defect which can also affect long-term outcomes.
Omphalocele may sometimes be mistaken for gastroschisis, another congenital abdominal wall defect. Omphalocele differs from gastroschisis in that the protruding organs are contained within a thin covered sac, while in gastroschisis the bowel is free floating.
Evaluation and diagnosis of omphalocele
Given the rarity of this condition, it is important to determine the specific type of abdominal wall defect. Accurate diagnosis is critical in guiding the best treatment plan.
The Center for Fetal Diagnosis and Treatment (CFDT) sees between 30 and 50 cases of omphalocele each year, making us one of the most experienced teams in the world when it comes to diagnosing and treating this rare condition.
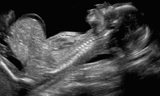
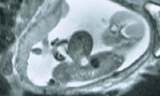
The diagnosis of omphalocele is usually made by prenatal ultrasound during the second trimester of pregnancy (about 20 weeks). An amniocentesis is recommended to evaluate for chromosomal abnormalities or genetic syndromes.
Families referred to the Center for Fetal Diagnosis and Treatment at Children’s Hospital of Philadelphia undergo a comprehensive one -day evaluation that includes:
- Detailed level II fetal ultrasound — a noninvasive, high-resolution imaging study used to determine the amount and type of abdominal organs within the umbilical sac and possible rupture of the sac, as evidenced by free floating bowel or the liver outside of the abdomen. The possibility of other anatomic abnormalities is evaluated. Lung size can also be estimated.
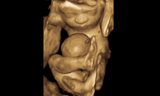
- Ultrafast fetal MRI — an additional imaging technique pioneered at CHOP that shows the omphalocele and the entire fetus. The MRI is used to confirm ultrasound findings and evaluate for the presence of any other anatomic abnormalities, especially central nervous system anomalies. Lung volumes are determined and compared to normal values at that gestational age (this comparison is called the observed-to-expected lung volume ratio, or O/E ratio).
- Fetal echocardiogram — an ultrasound of the fetal heart to look for heart defects. A unique collaboration with our specialized Fetal Heart Program, staffed by pediatric cardiologists with fetal expertise, ensures early diagnosis of heart defects.
For proper counseling and management of pregnancies diagnosed with omphalocele, it is important to distinguish fetal omphalocele from other abdominal wall defects and check for associated birth defects.
Management of omphalocele during pregnancy
After a comprehensive diagnostic evaluation, CHOP’s multidisciplinary team (pediatric surgeon, high-risk obstetrician/reproductive geneticist, nurse coordinator and genetic counselor) meets with your family to review test results, confirm the diagnosis, explain options and potential outcomes, and answer questions.
Our team works with you to develop a treatment plan tailored to the specific needs of you and your baby. Your family will also receive educational information about omphalocele and can tour CHOP’s Garbose Family Special Delivery Unit (SDU) and the Harriet and Ronald Lassin Newborn/Infant Intensive Care Unit (N/IICU).
Your pregnancy will be closely monitored, particularly in the third trimester. This care is overseen by the CFDT’s maternal-fetal medicine team. Regularly scheduled ultrasounds help us detect developing issues throughout the pregnancy. If monitoring indicates fetal distress, our team, with over 100 years combined experience, is prepared to move quickly and ensure the best outcome for both mother and baby.
For more information about the diagnosis, delivery and treatment of babies with omphalocele, watch our educational video series about abdominal wall defects. En Español »
Delivery of babies with omphalocele
Delivery of babies with omphalocele may be vaginal or cesarean (C-section) depending on the size and contents of the omphalocele. For a small omphalocele that does not involve the liver, vaginal delivery is possible, provided there are no obstetrical contraindications. Babies with liver in the omphalocele are delivered by C-section to protect the omphalocele sac and prevent organs from rupturing or bleeding, which can be life-threatening.
At CHOP, babies with omphalocele are born in the SDU, allowing for the highest level of immediate care for the newborn, as well as expert obstetric services for the mother — all within the same pediatric hospital. The world’s first birth facility designed exclusively for pregnancies complicated by birth defects, the SDU is a vital part of our team’s ability to provide comprehensive care.
Your baby is stabilized by a highly specialized team of pediatric surgeons, neonatologists, specially trained nurses and respiratory therapists, all with extensive experience in treating neonates with omphalocele. The omphalocele sac is wrapped with a sterile dressing and particular attention is paid to breathing assistance, as babies with giant omphaloceles typically have small lungs and often require a breathing tube and ventilator.
Once your baby is stabilized, you will have a chance to meet them before they are brought to the N/IICU.
Omphalocele treatment
Surgical repair of the omphalocele takes place after birth. The overall health of your baby, especially their respiratory status, the size of the omphalocele and the degree of liver involvement, determine the type of omphalocele treatment.
Omphalocele repair is typically performed at your baby’s bedside in the N/IICU by our unique Neonatal Surgical Team.
Babies with small omphaloceles are monitored closely until they are ready to undergo primary repair. This means the herniated organs are placed back into the abdominal cavity and the defect is completely closed in one operation.
For babies with giant omphalocele that contain the liver and other organs, a staged repair (involving several steps, also called the Schuster procedure) is needed to gradually return the abdominal contents to the belly. This gradual process provides time for the abdominal wall to stretch to accommodate the viscera, and ensures that the lungs can continue to grow and expand without immediate pressure of surgical closure.
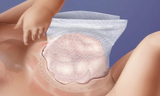
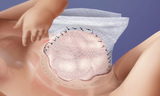
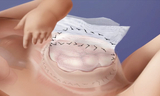
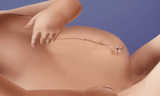
In a staged repair, a mesh fabric is sewn to the fascia (connective tissue) and muscle on each side of the omphalocele defect. The two pieces of fabric are then sewn together over the defect, and the omphalocele sac remains intact. Your baby returns to the N/IICU, where their organs are gradually returned to the abdominal cavity and the mesh is continuously tightened over the course of days or weeks. Once all of their organs are back in their belly, your child's surgeons can remove the mesh and safely perform the final closure. Babies are monitored very closely throughout this process in our N/IICU.
In some cases of babies with giant omphaloceles, the amount of organs protruding may be so large that there isn’t enough room in your baby’s body to fit them all inside, preventing omphalocele closure in the neonatal period. Small lung size may also delay closure. If this is the case, surgery may be postponed for months to allow the lungs and body to grow. During this time, a technique called “paint and wait” is used. The sac covering the omphalocele is painted with an antibiotic cream and covered with elastic gauze. Your baby’s skin will grow over the sac with time.
Some babies do not need to remain hospitalized during the paint and wait treatment. We will teach you how to do this technique so that you can bring your baby home. When all of the contents of the omphalocele are covered with skin and the lungs have had a chance to grow, your child's surgeon will talk with you about options for surgically closing the remaining hole.
N/IICU stay after omphalocele repair
N/IICU stays for babies with omphalocele can range from several days to several months, depending on your baby’s lung function, the size of the defect and timing of surgical repair. Infants are monitored for common complications of omphalocele, such as feeding difficulties, bowel obstruction and gastroesophageal reflux. Babies with omphalocele also frequently have inguinal hernias, another condition that requires surgical repair.
Before your baby is ready to go home, they will need to gradually meet certain milestones, including:
- Breathing on their own (may need supplemental oxygen)
- Full enteral feedings (by mouth or feeding tube)
- Maintaining their temperature
- Gaining weight
Another important milestone is making sure you and any other caretakers are ready to take care of your child at home. Our team is here to support you throughout that learning process.
Follow-up care for omphalocele
Parents are an integral part of the team and play an important role in caring for their baby from the start. During the stay in the N/IICU, a specialized team of surgeons, nurses, speech therapists (for feeding therapy), lactation consultants, respiratory therapists and social workers are available as needed to help educate your family about what you can do during the hospital stay, as well as caring for your baby after discharge. The nursing staff teaches you special feeding techniques and other specialized care that your child might need.
Families also have access to the Connelly Resource Center and CHOP’s Child Life department. These programs provide resources and support to make the hospital experience easier on the entire family. From sleeping rooms and laundry facilities to programs that help siblings adjust to having a new baby in the family that requires special medical care, the team can help every family make use of all resources available to them.
Long-term outlook for babies born with omphalocele
Babies who have had small omphaloceles receive follow-up through their pediatrician and the pediatric surgeon. Those without associated defects generally have good long-term outcomes. Babies with giant omphaloceles typically need to be followed more closely by a multidisciplinary team as part of ongoing omphalocele treatment. The pulmonary hypoplasia (small lungs) associated with giant omphalocele can affect not only breathing, but also heart function, ability to feed, and overall development. This represents a significant long-term health issue.
Children’s Hospital of Philadelphia has a unique Pulmonary Hypoplasia Program (PHP) that provides comprehensive, interdisciplinary care specifically focused on this challenging condition. The multidisciplinary team that follows children throughout infancy and well into school age includes:
- Pediatric surgeons
- Pediatric pulmonologists
- Pediatric cardiologists
- Developmental pediatricians
- Developmental psychologists
- Dieticians
- Audiologists
- Social workers
- Other specialties as needed, including gastroenterology, orthopedics, urology, physical therapy and occupational therapy.
The PHP team collaborates with each family to improve your child’s health and development, monitor growth, monitor for surgical issues that may develop, and help locate resources and support near the home.

Tour our Fetal Center
The Wood Center for Fetal Diagnosis and Treatment has cared for many families and will help you through your journey, too.

What to expect
From the moment of referral through delivery and postnatal care, your family can expect a supportive experience when you come to us with a diagnosis of a birth defect.
Resources to help
Omphalocele Resources
Richard D. Wood Jr. Center for Fetal Diagnosis and Treatment Resources
Learning your baby has a birth defect is a life-changing experience. We want you to know that you are not alone. To help you find answers to your questions, we've created this list of educational health resources.
Reviewed by Emily A. Partridge, MD, PhD, MHS