What is hyperhidrosis?
Hyperhidrosis is a condition characterized by excessive sweating in amounts greater than what is needed to regulate our body temperature. In most cases, the condition occurs for no apparent reason and is called primary hyperhidrosis. Primary hyperhidrosis usually affects only certain parts of the body, so it is also referred to as primary focal hyperhidrosis. The areas that are most commonly affected by primary focal hyperhidrosis are the palms of the hands, the axillae (armpits), and the feet. Primary focal hyperhidrosis affects 1 to 3 percent of the U.S. population. Males and females are affected equally, and in the majority of patients the condition starts during childhood or adolescence.
Hyperhidrosis can also occur as a result of several medical conditions, including hyperthyroidism and hypertension, in which case it is called secondary hyperhidrosis. Before starting any treatment for hyperhidrosis, all medical conditions that can lead to excessive sweating must be ruled out.
Signs and symptoms of hyperhidrosis
Patients with primary focal hyperhidrosis have constant excessive sweating in the affected areas, regardless of the environmental temperature and the emotional situation. Generally the excessive sweating only stops during sleeping hours and worsens in warm environments and stressful situations. In most patients, more than one area of the body is affected, hands and feet being the most common combination.
Most patients notice the excessive sweating for the first time when the moist palms begin to interfere with school and social activities. Excessive sweating in the hands can severely affect the ability to write, hold papers, use touch-screens, manipulate objects, and perform routine daily activities. It can also cause social embarrassment and impair the patient’s social interactions, which can lead to negative psychological and psychosocial consequences.
Testing and diagnosis of hyperhidrosis
After ruling out all potential causes of secondary hyperhidrosis, the diagnosis of primary focal hyperhidrosis is made by physical exam and a detailed evaluation of the patient’s signs and symptoms. No special diagnostic tests or imaging studies are required. The diagnosis is usually made by the patient’s pediatrician or dermatologist.
Treatment for hyperhidrosis
Hyperhidrosis can be treated non-surgically or with a surgical procedure. At Children’s Hospital of Philadelphia we are committed to treating the patient, not just the condition. Your child’s dermatologist, primary care physician and surgeon will work together to make sure that all hyperhidrosis treatment options are explored.
Patients who don’t have success with non-surgical options will be carefully screened through a comprehensive interview, a detailed self-assessment questionnaire, and a psychological evaluation to ensure that they are good candidates for surgery. Children (and their families) who are appropriate candidates for hyperhidrosis surgery will have an in-depth discussion with the surgeon about the risks and benefits of the operation. After the operation your child will be followed on a regular basis in the surgery clinic.
Non-surgical treatment of hyperhidrosis
Our expert pediatric dermatologists, led by Dr. Albert C. Yan, offer the full spectrum of non-surgical treatment options for hyperhidrosis.
- Topical agents: Hyperhidrosis can be treated with the application of antiperspirants that prevent sweating by mechanically blocking the sweat glands. The topical agents most commonly used in the treatment of hyperhidrosis are Drysol® (20 percent aluminum chloride) and Xerac® (6.25 percent aluminum tetrachloride). These products are applied to the affected area once a day, usually at night.
- Oral medications: The medications used to treat hyperhidrosis are called anticholinergic agents and work by blocking the innervation of the sweat glands. The most commonly used are Robinul® (glycopyrrolate) and Ditropan® (oxybutynin). These medications have a variety of side effects that include dry mouth, blurred vision and urinary retention.
- Iontophoresis: This is a type of low-voltage electrical therapy. The affected areas are submerged in water to which an electrical current is applied. The electrolytes of the water accumulate on the surface of the skin, blocking the sweat glands. Iontophoresis is done on a daily basis, and each session is 20 to 30 minutes long. This treatment requires a significant time commitment.
- Botox®: The botulinum toxin decreases the amount of sweating by inhibiting the release of acetylcholine from the nerves that stimulate the sweat glands. This treatment requires multiple skin injections to the affected areas and needs to be repeated every 3 to 9 months.
Other therapies such as lasers, herbal medicines, microwave energy, and high-intensity ultrasound are not standard options in pediatrics and their efficacy has not been scientifically proven. To learn more about the non-surgical options available to treat hyperhidrosis, contact the Dermatology Section.
When patients do not respond to non-surgical alternatives, we offer a surgical treatment option.
Surgery for hyperhidrosis
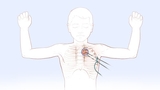
Patients with primary hyperhidrosis have the option of undergoing a surgical procedure called thoracoscopic sympathectomy. The operation is also known as endoscopic thoracic sympathectomy or minimally invasive thoracic sympathectomy.
Dr. Pablo Laje, a pediatric general surgeon at The Children’s Hospital of Philadelphia, offers surgery to children and teenagers who have primary focal hyperhidrosis of the hands, alone or in combination with armpits and/or feet. Patients whose hands are not involved are not candidates for the operation. Learn more about surgery for hyperhidrosis.
Whether your child’s doctor has recommended surgery or you are seeking help, our team is available to answer any questions you may have about the procedure.
To learn more about surgery for hyperhidrosis or to refer a patient, contact the Division of Pediatric General, Thoracic and Fetal Surgery or email us with any questions.
If your child is undergoing a surgical procedure at The Children’s Hospital of Philadelphia, we have a variety of resources available that can help you and your family prepare for the experience. Check out our Guide to Your Child’s Surgery to learn more about having surgery at CHOP.
Why choose CHOP for your child's surgery
If your child needs surgery, you want to know their care is in the hands of the best, most compassionate team. CHOP's world-class pediatric surgeons and experienced staff are here for you.

Preparing for surgery
Find tips to prepare for your preoperative visit with CHOP’s pediatric general surgeons, and resources to help prepare your child for surgery.
Resources to help
Hyperhidrosis Resources
Division of Pediatric General, Thoracic and Fetal Surgery Resources
We have created resources to help you find answers to your questions and feel confident with the care you are providing your child.
Reviewed by Pablo Laje, MD
