About Fetal Surgery for Spina Bifida (Myelomeningocele, MMC)
What is fetal surgery for spina bifida/myelomeningocele (MMC)?
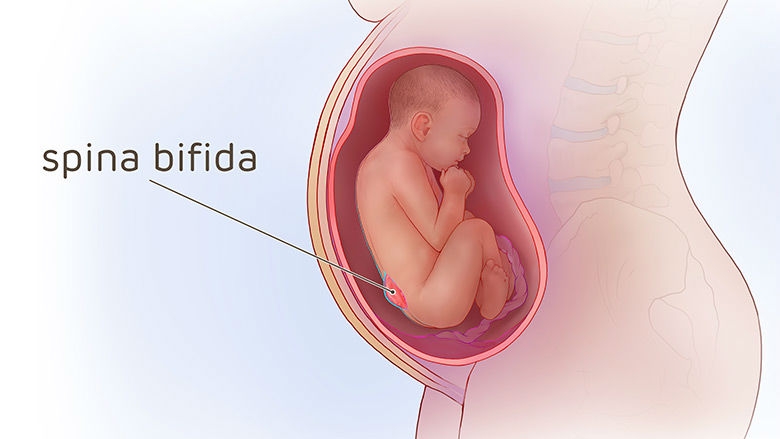
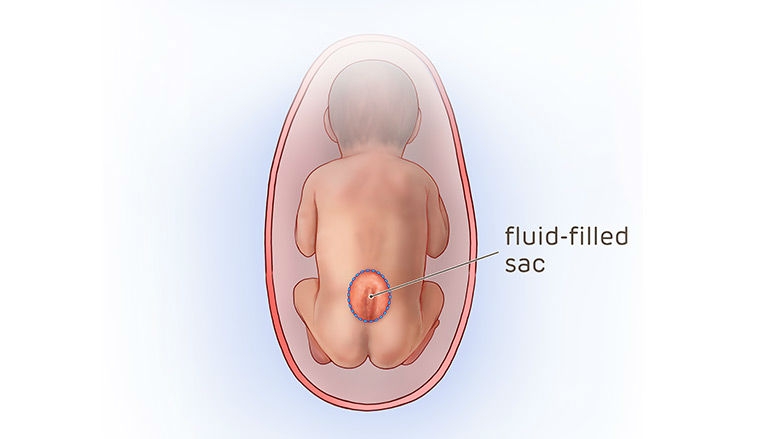
Prenatal repair of myelomeningocele (MMC), the most common and severe form of spina bifida, is a delicate surgical procedure where fetal surgeons open the uterus and close the opening in the baby's back while they are still in the womb. Because spinal cord damage is progressive during gestation, prenatal repair of myelomeningocele may prevent further damage.
Fetal spina bifida surgery is one of the most exciting developments in the history of treatment for birth defects. An extremely complex procedure available only to qualified candidates, fetal surgery for myelomeningocele requires significant commitment on the part of mothers who choose to go forward with it and extensive surgical experience to perform successfully.
Fetal surgery for spina bifida is not a cure, but studies show that prenatal repair can offer significantly better results than traditional postnatal repair. Fetal surgery for spina bifida greatly reduces the need to divert fluid from the brain, improves mobility and improves the chances that a child will be able to walk independently.
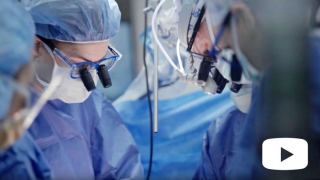
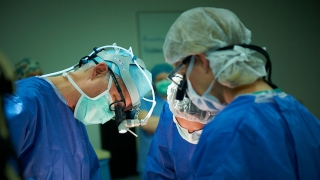
In this video, fetal surgeons and other team members explain spina bifida treatment options, the benefits of spina bifida surgery before birth, the team required to perform this complex procedure in utero, and the support services we offer families. The video also shares spina bifida fetal surgery stories from the perspective of families.
Before fetal spina bifida surgery
Mothers who choose fetal surgery require the most expert and carefully coordinated care from the time of diagnosis, for the spina bifida surgery itself, and through the baby's delivery and care afterwards. If you meet the criteria and are considering fetal surgery for myelomeningocele, you will receive comprehensive counseling on the condition and the risks involved in the procedure. Here are some questions to ask when considering your options for fetal surgery that can help you make an informed decision that is right for you and your baby.
Before proceeding with fetal surgery, you will undergo a physical exam and complete review of your medical history to obtain clearance for surgery. Read our criteria for fetal surgery to determine when prenatal myelomeningocele repair is an option.
Your pre-surgery consultation will include:
- A thorough explanation of care and monitoring both before and after delivery, including a review of medications necessary before, during and after fetal surgery
- A review of the surgical procedure and its risks, including preterm birth, uterine scarring, membrane separation, infection, bleeding, prematurity and fetal demise
- A consultation with a social worker and a psychological evaluation to assess readiness for surgery, coping mechanisms and family support
If you are not a candidate for fetal surgery, we will coordinate with your referring physician and will follow the progression of your pregnancy. You will have the option of having postnatal repair surgery here at Children’s Hospital.
For families who return to Philadelphia for delivery of their baby, we will co-manage your pregnancy with your referring physician and will assist in the timing of the delivery and coordination of services.
If you relocate to Philadelphia to receive your care in the Garbose Family Special Delivery Unit (SDU), you may need to bring a support person. Your support person is used in labor and for certain procedures. In the event of relocation to the Ronald McDonald House or a host family, the support person is required to be with you.
If you are being admitted to the SDU, we will ask you if you would like to choose a “lay caregiver.” A lay caregiver is an adult friend or family member who would be willing to help you with your healthcare needs at home. The lay caregiver is different from your support person. In Pennsylvania, it is legally required that hospital staff ask this question. You are not required to choose a lay caregiver, and you can change your mind at any time.
Your fetal surgery care team
Your multidisciplinary team includes fetal surgeons, neurosurgeons, maternal-fetal medicine specialists, fetal cardiologists, neonatologists, anesthesiologists, sonographers, advanced practice nurses, a psychologist, social workers and coordinators — all focused on the best outcome for you and your baby. Your child will also have immediate access to the full resources of Children’s Hospital of Philadelphia for whatever additional care they may require.
About the in utero MMC repair procedure
Prenatal repair of myelomeningocele is performed between 23 weeks and 25 weeks 6 days gestation. Mothers must be willing to stay in Philadelphia with a support person for the surgery and for the duration of the pregnancy to allow close monitoring.
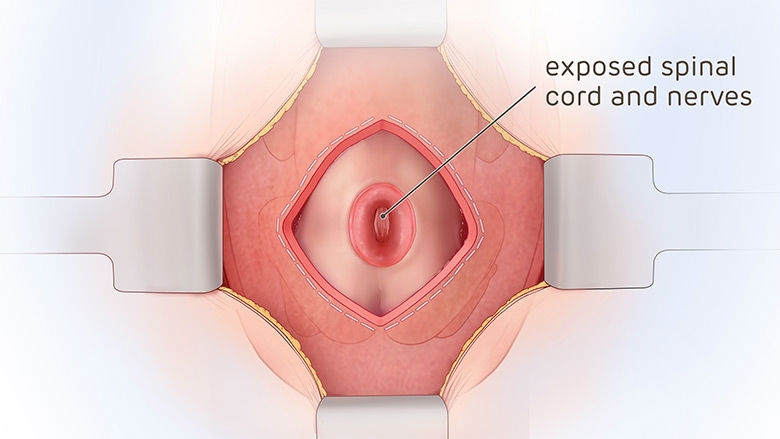
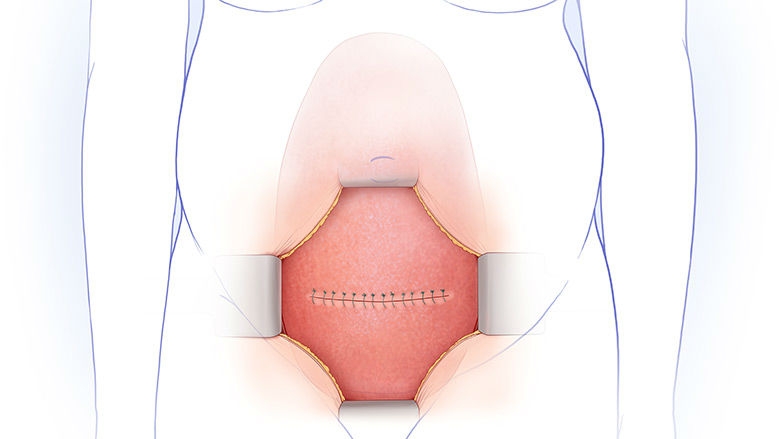
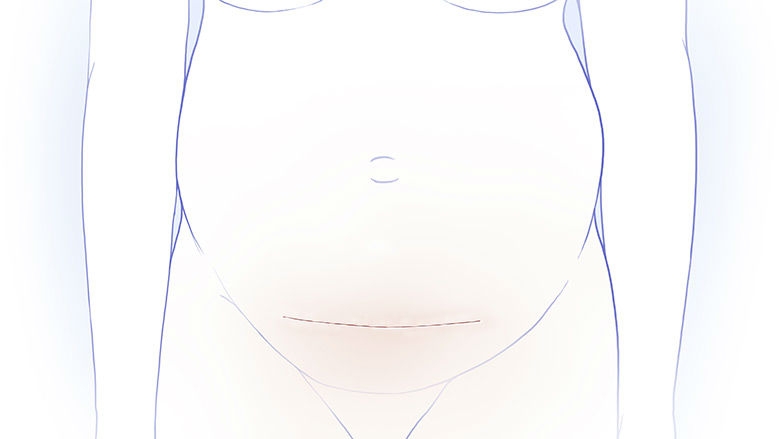
In prenatal repair, the mother receives general anesthesia, which also relaxes the uterus and anesthetizes the fetus. Fetal surgeons perform a laparotomy (an incision across the mother’s abdomen). A maternal-fetal medicine specialist performs sterile intraoperative ultrasound to map the position of the placenta and the fetus, and your baby’s back is rotated into view. The uterus is then opened with a uterine stapling device that pinches off all blood vessels and keeps membranes secured to the muscle.
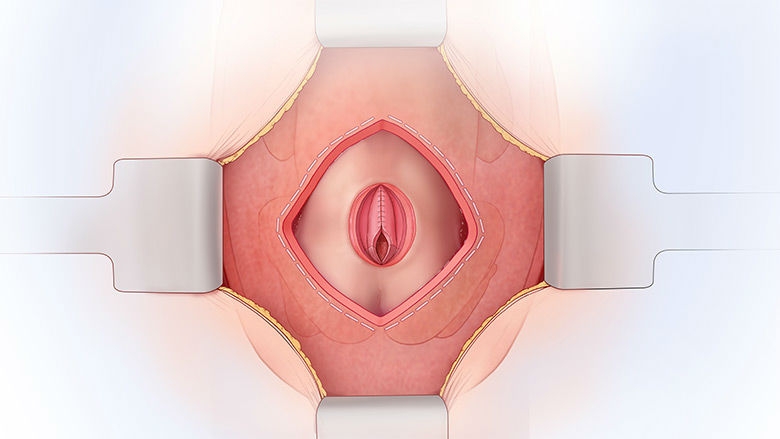
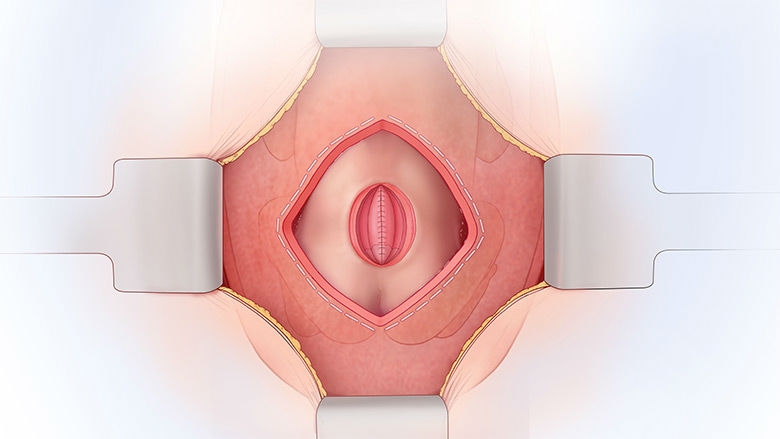
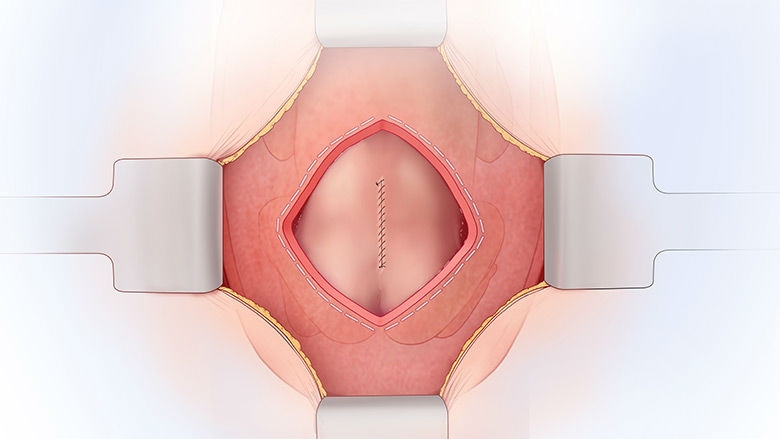
A pediatric neurosurgeon removes the MMC sac, if one is present, returns the spinal cord to the spinal canal, and closes the surrounding tissue and skin over the defect to protect the spinal cord from exposure to the amniotic fluid. The uterus and the abdominal incision are then closed.
Spina Bifida Surgery During Pregnancy
During surgery, a fetal cardiologist uses echocardiography to closely monitor your baby’s heart. All of these measures are used to ensure the utmost safety of both mother and baby.
Mothers usually remain in the hospital for three to five days and are on modified bed rest for three to four weeks after surgery to reduce the risk of preterm labor. For the remainder of the pregnancy, follow-up includes weekly visits to the Center for ultrasound monitoring and routine prenatal care. If labor does not begin sooner, your baby will be delivered by planned cesarean section at 37 weeks. After delivery, your baby will be cared for in our Newborn/Infant Intensive Care Unit (N/IICU).
Mothers who elect fetal repair will also be asked to sign a consent for postnatal follow-up of your baby by our Center. This follow-up will require your family to return to Philadelphia for evaluation when your child reaches 12 months, 30 months and five years of age. Detailed follow-up not only provides excellent care for the child, it adds to a growing base of knowledge that will benefit future generations of children with spina bifida.
Watch the following video for more details about having spina bifida surgery during pregnancy, including how it is done and what to expect before, during and after the procedure.
After fetal surgery for spina bifida
Delivery of baby with MMC
Babies who undergo prenatal repair of MMC will be delivered in the Garbose Family Special Delivery Unit (SDU), the world’s first delivery unit within a pediatric hospital created specifically for healthy mothers carrying babies diagnosed with birth defects. The SDU not only allows the most advanced care for neonates immediately upon delivery, it allows you and your baby to remain together in the same hospital for the duration of your care.
N/IICU stay
After your baby is born, they will stay in the N/IICU where they will be closely monitored by a multidisciplinary team of specialists who are experienced in caring for babies born with spina bifida. This team includes neurosurgery, urology, orthopaedics, physical therapy and others from the Spina Bifida Program.
Here’s what you can expect during your baby’s N/IICU stay:
- Head ultrasounds on the day of delivery and prior to discharge.
- MRI to evaluate your baby's brain and spine.
- Daily head circumference measurement.
- Renal and bladder ultrasound at 2 days old.
- Bladder scans with a handheld ultrasound device every four hours for the first 48 hours to estimate the amount of urine in the bladder and whether your baby will require a catheter.
- Clean intermittent catheterization if your baby's bladder volume is greater than 50 percent of expected volume.
- Video-urodynamics at 2 days and 2 months of age. A special catheter measures pressure when the bladder is full. A soft catheter in the rectum measures abdominal pressure on the bladder. A uroflo chair measures urine flow rate and time needed to empty bladder.
- Measures to prevent urinary tract infection.
- Evaluation for shunt.
Follow-up care after fetal spina bifida surgery
Children receiving follow-up care through CHOP are seen by our dedicated Spina Bifida Program, the nation’s first program to bring a multidisciplinary approach to long-term follow-up of children with spina bifida. This clinic brings together specialists from neurosurgery, urology, orthopaedics, physical therapy, social work, genetics, pediatrics and nursing.
Follow-up includes visits every four to six months until age 2, then annually, with urodynamic testing and renal bladder ultrasounds to ensure kidneys function properly and bladder function is stable.
Prenatal spina bifida repair research
The Center for Fetal Diagnosis and Treatment conducted extensive laboratory research, the findings from which supported the theory that performing spina bifida surgery in utero could minimize neurologic damage. Between 1998 and 2003, the Center team performed prenatal spina bifida repair in 58 mothers and observed significant benefit in the babies.
To answer the question conclusively, the Center co-led the groundbreaking Management of Myelomeningocele Study (MOMS), a landmark national study that directly compared prenatal to traditional postnatal repair of myelomeningocele.
The randomized, controlled clinical trial was initiated and funded by the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), comparing outcomes after prenatal and postnatal repair in 183 patients.
The study showed that fetal surgery for spina bifida greatly reduces the need to divert fluid from the brain, improves mobility and improves the chances that a child will be able to walk independently.
Phase two of the Management of Myelomeningocele Study (MOMS 2) continued to monitor the 183 patient families from the initial trial at participating clinical sites. Follow-up research supported the original findings that prenatal repair of myelomeningocele improves motor outcomes at 30 months of age, compared to postnatal repair. Children in the prenatal surgery group were more likely to walk independently (at 44.8 percent compared to 23.9 percent in the postnatal group). The prenatal group also performed better on two scales: the Bayley Motor Development Index and the Peabody Developmental Motor Scales.
MOMS2 Study Findings
In January 2020, after following those two groups of patients for up to 10 years after birth, researchers have shown those benefits continue into childhood. Findings show significant physical and emotional benefits in school-age children who received corrective surgery in the womb for MMC. The MOMS2 study findings provide valuable insight into the lasting outcomes of prenatal repair versus standard postnatal repair, and provide both clinical teams and families with additional information to make better informed choices about the treatment options available.
Ongoing follow-up is critical when it comes to advancing treatment for patients with myelomeningocele, and an integral part of the Center’s commitment to the families we treat.