Pediatric Rheumatology Fellowship
About the program

The Fellowship Program in Pediatric Rheumatology is a three-year program designed for physicians trained in pediatrics and selected on the basis of excellence in their credentials and training programs.
Our program combines a one-year clinical experience followed by at least two years of scholarly work, which can include advanced training in basic, translational or clinical research, while continuing a longitudinal patient care experience. The program is led by a broadly experienced faculty who will train physicians to be pediatric rheumatologists and leaders in pediatric rheumatology.
Fellowship training program director
Jay Mehta, MD, MSEd
Children's Hospital of Philadelphia
Leonard and Madlyn Abramson Pediatric Research Center
Division of Rheumatology
3615 Civic Center Boulevard - Room #1102
Philadelphia, PA 19104-4399
215-590-2547
mehtaj@chop.edu
The history, expertise and compassion that make Children’s Hospital of Philadelphia unique are also what makes it the best place for medical trainees.
Fellowship goals
The key goals of the fellowship program are to:
Develop collaborative clinical care expertise
- To lead the comprehensive care of children with rheumatic diseases.
- To incorporate the role of medical and allied healthcare professionals in patient care.
- To understand the role of community resources in the care of children with rheumatic diseases.
- To work within interdisciplinary teams.
Foster independent basic science, translational and clinical investigation
- To offer formal post-doctoral course work in basic science, translational and clinical research.
- To provide mentoring to develop and complete innovative and feasible research projects.
- To ensure academic achievement by rigorously supervising academic progress.
Invest in the future of pediatric rheumatology
- To promote management skills for independent direction of a rheumatology team, including formal participation in divisional quality and patient safety initiatives.
- To solidify research skills to further independent research careers.
- To foster mentoring skills to educate subsequent trainees.
- To cultivate leadership skills to advance the field of pediatric rheumatology.
Unique information about the program
An independent Division of Rheumatology was established in 1999 within the Department of Pediatrics. In 2000, the American College of Graduate Medical Education (ACGME) accredited the Rheumatology Fellowship Program. We have eleven pediatric rheumatology faculty members and two fellowship slots available each year. Our faculty are actively engaged in both basic and clinical investigation,and have a longstanding commitment to Childhood Arthritis and Rheumatology Research Alliance's (CARRA) efforts. Additionally, CHOP Rheumatology has a long-term involvement in participation and leadership within the Pediatric Rheumatology Care & Outcomes Improvement Network (PR-COIN) Network.

Clinical training occurs in our busy outpatient clinic, as well as on the inpatient side with both our primary rheumatology service and a robust consult service. CHOP not only serves as the main pediatric care site for much of Philadelphia, but also welcomes patients from throughout the mid-Atlantic region, the United States, and the world. We conduct four multi-disciplinary clinics which fellows actively participate in, the Uveitis Coordinated Care Clinic, the Lupus Integrated Nephritis Clinic, Rheumatology-Dermatology Clinic, and the Immune Dysregulation Clinic. In addition to these, we have an Amplified Musculoskeletal Pain Multidisciplinary Clinic which is available for interested fellows. Rheumatology clinicians are supported by 5 nurses and 2 social workers, including a dedicated lupus social worker.
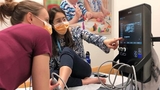
Musculoskeletal ultrasound, arthrocentesis, and intraarticular corticosteroid joint injections are commonly performed. In addition to clinic-based training, fellows enroll in ultrasound educational offerings at the ACR Annual Scientific Conference or at the CARRA Annual Conference. We currently have two ultrasound devices for use in our clinic, which has enhanced our diagnostic and therapeutic capabilities.
Pediatric rheumatology has a strong clinical and research relationship with the Penn Division of Adult Rheumatology. We have shared conferences, and pediatric fellows attend adult clinics periodically. Importantly, we have a shared NIH fellowship training grant (T32) and have recently developed a Medicine-Pediatrics Rheumatology Fellowship.
Specific information by years and/or rotation
First year
Fellows become proficient in the history, physical exam, differential diagnosis, diagnostic evaluation, and treatment of pediatric rheumatic diseases. Sensitivity to psychosocial aspects of chronic illness is emphasized.

First year fellows split the year between our inpatient and outpatient services, and spend 16 weeks on our recently developed longitudinal rotation, which includes experiences in our multidisciplinary clinics, adult rheumatology clinics, and other subspecialty clinics. First year fellows have a once-weekly continuity clinic in which they follow patients for whom they are the primary rheumatologist.
The fellows share night and weekend care with the pediatric rheumatology attending. Additionally, the fellows prepare multidisciplinary conferences and take a major role in teaching residents and students rotating through the service.
During the first six months, under the mentorship of the faculty, the fellows consider available research training opportunities. In the second half of the first year, the fellows develop an appropriate research training plan and identify a research mentor.
Second and third year
Clinical responsibilities during the second and third years consist of a longitudinal patient care experience in continuity clinic and 4-6 weeks of inpatient service. Fellows are encouraged to take advantage of a number of opportunities to further their teaching skills with CHOP residents, Penn medical students, and other hospitals within the region.

The majority of time in the second and third years is devoted to research training — a critical component of the fellowship program. Fellows interested in basic/translational science may enroll in courses offered through the UPENN Graduate Program in Immunology and work as a post-doctoral fellow in their mentor’s laboratory. Fellows planning on a career in clinical research can enroll in the two-year Master of Science in Clinical Epidemiology (MSCE) Program at the UPENN Center for Clinical Epidemiology and Biostatistics (CCEB).
Those seeking formal training in translational research may enroll in the two-year Masters in Translational Research (MTR) Program.
If you have other scholarly interests, please let us know so we can connect you with opportunities across the extensive CHOP and Penn campuses.
Didactic program

Division chair holding an impromptu teaching session in the fellow workroom Each week, faculty and fellows participate in a 60-minute didactic session, and a 30-minute inpatient and outpatient case discussion. Our didactic curriculum is designed on a three-year cycle to ensure that fellows have exposure to outstanding CHOP and UPenn faculty with diverse expertise. Dr. Mehta reviews the Petty Textbook of Pediatric Rheumatology chapters each week with the first-year fellows.
- Every month, fellows lead a journal club with guidance from faculty. Major current or recent manuscripts in basic or clinical investigation relevant to rheumatic diseases as well as seminal articles are prioritized. Fellows receive feedback on their knowledge of the content in the manuscript and their analysis of study methods.
- Fellows participate in all divisional QI activities. Fellows learn improvement methodology and tools to systematically shepherd projects through define, diagnose, test/implement, and sustain phases. We actively participate in the Pediatric Rheumatology Care & Outcomes Improvement Network (PR-COIN), which focuses on QI training and improvement activities. One fellow has the opportunity to attend each biannual PR-COIN conference. Fellows have access to the Institute for Healthcare Improvement (IHI) curriculum, and a resident/fellow QI lecture series.
- We augment didactic sessions with interdisciplinary conferences with Radiology, Nephrology, Dermatology, Neurology, and UPenn Rheumatology. With guidance from attendings, fellows organize case presentations during these interdisciplinary conferences. Additionally, fellows are encouraged to attend the weekly Immune Dysregulation and monthly Interstitial Lung Disease interdisciplinary conferences.
- CHOP and, specifically, our division have a strong interest in helping fellows and faculty identify and address health disparities. We have a four-part didactic series, including 1) The role of implicit bias in patient care; 2) rheumatology health disparities and social determinants of health; 3) Using QI methodology to address healthcare disparities; 4) Communication skills for a diverse patient population.
- At the start of fellowship, we conduct a one-week didactic Introduction to Fellowship, focusing on major pediatric rheumatic diseases, therapeutics, laboratory testing and imaging, and how to be an effective consultant pediatrician. In addition, from September through December of each year, fellows attend the Immunology Lecture Series. Led by Dr. Behrens and Dr. Canna, and taught by leading basic investigators, this 10-lecture curriculum covers innate and adaptive immunity and prepares fellows to understand the pathophysiology of rheumatic diseases and rational choice of disease modifying and biologic therapies.
- Fellows are encouraged to participate in the Department of Pediatrics Fellowship Core Curriculum with a variety of fellows from across the institution.
- Fellows are encouraged to integrate opportunities for patients and families to participate in clinical research (trials, national registries, ongoing interventional and non-interventional studies) in the everyday clinical care setting.
Department of Pediatrics Fellows’ core curriculum
The Department of Pediatrics organizes a common core curriculum for all fellows at CHOP. Fellow Core Curriculum will cover multiple topics relevant to all pediatric subspecialty fellows, including professional development. Core Curriculum begins with sessions during the Departmental New Fellow Orientation and continues with multiple offerings throughout the year. Topics included include:
- Quality Improvement Methodology
- Half day retreats by year of training
- Orientation First Year: Time management, Fatigue mitigation, Introduction to CHOP and Penn, Wellbeing, Tips and Tricks to Success as a Fellow; Diversity, Equity, and Inclusion
- Spring First Year: Grant funding, Mentee-Mentor Relationship, Research Design, Advanced library skills
- Second Year: Leadership, Communication skills, Presentation, Health Care Disparities, Teaching skills
- Fall Third Year – Success in the Job Search: Job search overview, interview skills, CV and Cover letter workshop,
- Spring Third Year – Transition to Attending: Leadership skills, Work-life integration, Time management, Billing, Life-long learning, Personal Finance
These sessions occur multiple times per year and offer the added benefit of allowing fellows from different subspecialities an opportunity to engage and network over the course of their training at CHOP. Additional educational and community building events are offered by the Fellows Association (FA). The FA is a volunteer organization that is comprised of multi-disciplinary senior fellows and a faculty advisor. The FA’s mission is dedicated to representing the interests of subspecialty fellows at CHOP and to promoting the continuous improvement of their training experience.
More information about the Department of Pediatrics Graduate Medical Education office, Fellow Core Curriculum and the Fellows Association can be found at the following website.
General information on outcomes of fellows

The CHOP Pediatric Rheumatology Fellowship is designed to allow graduates the flexibility to seek the career of their choice. Most graduates seek academic positions at tertiary care centers.
In addition to the ten graduates who currently hold faculty positions at CHOP, recent graduates have positions at Toronto Hospital for Sick Children, Riley Children’s Hospital, Children’s Hospital of Atlanta, Dell Children’s Hospital, Hackensack University Medical Center, University of Utah, Boston Children’s, Vanderbilt University Medical Center, Lurie Children’s Hospital at Northwestern, Children’s Hospital of Alabama at UAB, Nationwide Children’s Hospital, Seattle Children’s Hospital, Mayo Clinic, University of California San Francisco Benioff Children’s Hospital, University of Texas Southwestern Medical Center, Golisano Children’s Hospital at the University of Rochester, Children’s Mercy Kansas City, the University of Iowa Children’s Hospital, University of Michigan, and the University of Kentucky.
About the faculty
Edward Behrens, MD (Division Chief): Ed first discovered his passion for Pediatric Rheumatology during his medical school rotation in the Division at CHOP in 2000. It was so awesome that he never left. Now as chief, he aspires to lead the Division to provide the same incredible training experience he was fortunate to receive. His research interests include Toll-like Receptor and cytokine biology, particularly as they relate to cytokine storm syndromes. Dr. Behrens started the CHOP Immune Dysregulation Program. When not at work he enjoys duplicate contract bridge, playing the trombone, and watching The Office with his daughter.
Jay Mehta, MD (Fellowship Program Director): Jay came back to CHOP after 5 years away after fellowship. He was drawn back to CHOP by the incredible fellows, faculty, and resources (both clinical and research) that are here. Nationally, he serves as the Vice President for CARRA. Jay's fun fact: he won a car on an episode of Wheel of Fortune in high school, but sadly lost the evidence when he left the VHS tape on top of a toaster oven in college. When not at CHOP, Jay loves exploring Philly restaurants with his wife, throwing spontaneous dance parties with his 12-year old daughter, and watching Premier League soccer and cheering on the Philadelphia Union with his 7-year old son.
Melissa Lerman, MD PhD MSCE (Associate Fellowship Director): Melissa moved to Philadelphia for medical/graduate school, completed her pediatrics residency and fellowship in rheumatology at CHOP, and has been on the faculty since 2011. Dr. Lerman is a full-time clinician at CHOP and is the assistant Fellowship Director for the division. Her particular clinical and research focus is in uveitis. Along with an ophthalmology colleague, Dr. Stefanie Davidson, she co-founded and co-directs the Uveitis Coordinated Care Clinic. She is also actively involved in the Uveitis Study Group of the Childhood Arthritis & Rheumatology Research Alliance. She is particularly interested in using, and helping others to perform, MSK ultrasound. Dr. Lerman, her husband and two children are committed city dwellers who love the ability to walk or bike almost anywhere. She looks forward to introducing new fellows both to rheumatology and to Greater Philadelphia.
Jon (Sandy) Burnham, MD MSCE (Clinical Director): Sandy has lived in Philly since coming to medical school at Penn in 1993. After completing his training at CHOP, he joined the Rheumatology faculty in 2004, served as Fellowship Director from 2013-2019, and is now the Rheumatology Clinical Director. He is currently involved in numerous quality improvement activities within CHOP focusing on treat-to-target approaches in juvenile idiopathic arthritis and developed the Lupus Integrated Nephritis Clinic (LINC). LINC is a multidisciplinary clinic that launched in 2018 and includes rheumatology, nephrology, social work, and psychology providers. Nationally, he is a member of the Pediatric Rheumatology Care and Outcomes Improvement Network (PR-COIN) Executive and Steering Committees, and co-leads its Outcomes Committee. He is co-leading PR-COIN’s efforts to deploy a treat-to-target approach across its centers in the United States and Canada. He enjoys spending time with his wife and two daughters, and in his free time can be found playing squash or tennis, taking photographs, cheering for the Phillies, barbecuing, and fly fishing.
Lehn Weaver, MD PhD: Lehn is a former graduate of the CHOP Rheumatology Fellowship with a particular interest in the basic immunologic mechanisms driving systemic inflammation in autoimmune and autoinflammatory diseases. He enjoys spending time with his wife and 2 children, coaching and playing sports with Carter (11) and Annabelle (9), mountain biking, and planning the next family adventure.
Pam Weiss, MD MSCE (Director of Clinical Research): Pam joined the rheumatology faculty in 2008 after completing her training at CHOP. She directs the Rheumatology Research Core which facilitates the recruitment and conduct of patient-oriented studies leveraging the clinic population. Her own research focus is on the epidemiology and clinical trials of children with juvenile arthritis and spondyloarthritis. Pam leads the Clinical Trials Research Affinity Group at CHOP and serves as the Clinical Futures’ Associate Co-Director for Clinical Trials,. Pam enjoys serving as a taxi cab for her 2 daughters as well as cooking (especially spicy foods), gardening, skiing, and walking her dogs.
Sabrina Gmuca, MD MSCE: Sabrina joined the faculty in 2017 after completing her fellowship training at CHOP and an MSCE degree at Penn. She cares for patients in both our rheumatology and AMPS clinic. Sabrina is a core faculty member in Clinical Futures and PolicyLab at CHOP. Her research interests are neurocognitive impairment in adolescents with juvenile fibromyalgia syndrome and the role of resilience among youth with chronic musculoskeletal pain syndromes. Her current work, conducting a randomized controlled trial of a resilience coaching program for youth with chronic musculoskeletal pain, is supported by a K23 from NIAMS. She and her husband enjoy taking their dog and daughter on long walks and hikes out in the burbs.
Emily Liebling, MD: Emily completed her fellowship at CHOP in June 2020. She currently cares for patients at the CHOP Specialty Care Center in Princeton-Plainsboro, NJ. Her clinical interests lie in uveitis, particularly JIA-associated uveitis. She is a born and bred New Yorker and completed residency training at the Children’s Hospital at Montefiore, but now calls Philadelphia home. In her spare time, she enjoys spending time with family (at home and at work), being the brunt of divisional jokes, reading, exploring Philadelphia museums, and being a champion board gamer.
Beth Rutstein, MD, MSCE: Beth completed medical school, residency, and fellowship in Philadelphia at UPENN/CHOP. She has a particular interest in the infectious complications and vaccination recommendations for immunosuppressed patients and is always happy to field any vaccine-related questions you may have. She is an 100% clinician and thinks that clinic is the best! She mostly sees patients at the Brandywine Valley CHOP Specialty Care Center but has also recently started a joint rheumatology/dermatology clinic twice monthly at CHOP main campus. She loves to share her awesome and interesting patients with her trainees at both locations. At home, she has a rambunctious and opinionated 3-year-old boy as well as a new baby boy born in April 2024. In her free time, she mostly just tries to keep her kids alive, but also tries to work in some long runs whenever possible.
Scott Canna, MD: Scott was born in the Philly suburbs but trained in Baltimore, DC, Denver, Philly (as a CHOP rheum fellow), Bethesda, and Pittsburgh before returning home as faculty in 2021. He is clinically focused on providing exemplary care to immunologically complex patients as part of the CHOP Immune Dysregulation Program. Dr. Canna has been studying mechanisms of autoinflammation and hyperinflammation since 2005 and has led a translational research program since 2016. He also enjoys geeking out about immunology with fellows, embarrassing his two daughters, and testing his mettle in the outdoors. He is an insufferable advocate of bike commuting and thinks you should be too.
Malki Peskin, MD: After completing medical school, residency, and fellowship at Albert Einstein College of Medicine and the Children's Hospital at Montefiore in Bronx, NY, Malki recently made the big move down to Philly to begin as an academic clinician here at CHOP.. Her clinical interests include lupus, particularly patients with lupus nephritis. Her research interests include quality improvement work, specifically focused on improving medication adherence among adolescents with rheumatologic disease. When not at work, she enjoys spending time with her husband and 3 children, running, spinning, and finding the best coffee shops. Malki sees patients on the main hospital campus as well as at the CHOP specialty care center in Princeton-Plainsboro, NJ.
Dori Abel, MD MSHP: Dori grew up outside of Philly, where she developed her Philly pride. She earned her bachelor’s degree from Duke University, then gradually made her way back up the east coast, completing her medical education at Georgetown and her pediatric residency training at Columbia in NYC. She recently graduated from fellowship at CHOP, during which she completed a Master's in Health Policy Research with a Concentration in Healthcare Quality and Safety. Her research and QI interests relate to medication adherence, self-management support, and health equity, and she loves seeing the clinical impact of this work. She is now an attending physician working 100% clinically, splitting her time between general rheumatology and amplified pain. In addition to her love for clinical medicine and the CHOP rheum fam, she loves anything active (especially hiking beautiful mountains and biking), eating at Philly's amazing restaurants, and quoting The Parent Trap!
Julia Rood, MD, PhD: Julia joined the faculty in 2024, after completing her MD/PhD at Penn and clinical training at CHOP. She discovered her love for pediatric rheumatology while pursuing her graduate studies in Dr. Behrens' lab and continues to be inspired by her patients to unravel the immunologic mechanisms underlying autoimmune disease. Her research and clinical interests focus on lupus, particularly the role of viral infections in driving disease. When not at work, she can be found in the pool, biking through Fairmount Park and Wissahickon, or exploring Philly with her husband and daughter.
About the fellows

Adam Mayer, MD: Adam is a fourth-year Med/Peds rheumatology fellow. He hails from the distant land of Baltimore, MD. For his undergraduate studies he attended the University of Maryland Baltimore County (UMBC) where he studied Biology and German. Fun fact, UMBC has one of the top chess teams in the country, but not much in terms of other (actual) sports. He then came to Philadelphia for medical school at Penn followed by Med/Peds residency at Penn/CHOP. After 10 years, Philly is truly his new home! Adam chose to stay at Penn/CHOP for rheumatology fellowship given the breadth of interesting pathology, high quality research and exceptional mentorship. Adam is interested in adult and juvenile spondyloarthritis, with a specific interest in understanding optimal diagnostics and therapeutics for patients with IBD-associated arthritis. When not in the hospital, Adam can be found telling dad jokes (to his wife's chagrin), going on hikes with his wife, son Oliver and daughter Charlotte, and watching every type of football (i.e. football and soccer).
Sarah Capponi, MD: Sarah is a fourth-year Med Peds Rheumatology fellow. She went to Johns Hopkins for college and majored in Writing Seminars, and then migrated back to her home state of Pennsylvania for medical school at Jefferson and Med Peds residency at Penn and CHOP. She is interested in transitions of care, medical education, and excellent clinical care for medically complex Rheumatology patients across the lifespan. She loves playing tennis, reading Romantasy novels, eating at all the amazing Philadelphia restaurants, watching reality TV, and hanging out with her husband, two daughters, and mini Australian pup Theo.
Hallie Carol, MD: Hallie is a third-year fellow, born and raised in Massachusetts. Her love of the east coast and outdoor activities was solidified at Bowdoin College, where she studied Biochemistry. She completed her medical school training at Columbia University, followed by pediatric residency at Lurie Children's hospital in Chicago. Hallie was initially drawn to Rheumatology for its close tie with the immune system and diagnostic dilemmas. She knew CHOP was for her after she met the enthusiastic, welcoming faculty and heard about the immune dysregulation program. She is particularly interested in autoinflammatory diseases and the dermatologic manifestations of rheumatic disease. Her third year of fellowship will be focused on honing her rheum/derm skills, while continuing her work in the Canna Lab. Hallie considers herself a Trader Joe's enthusiast. She loves the outdoors, especially enjoying an afternoon along the Schuylkill river (which must involve picnicking and/or hammocking). When stuck inside, she is known to brew kombucha and watch F1.
Anna Costello, MD: A third-year fellow, Anna is from Connecticut originally and attended Brown University as part of the Program in Liberal Medical Education for undergraduate and medical school. She completed her Pediatrics Residency at CHOP and then survived a tumultuous chief year during the start of the COVID-19 pandemic. She then worked as a Pediatric Hospital Medicine Attending at CHOP for two years before applying for Rheumatology fellowship. She is so excited to continue training with the amazing group at CHOP. She wanted to stay because CHOP offers an amazing balance of being the local hospital for the city of Philadelphia and being a referral center for patients from all over the world. This lets you learn about everything from bread-and-butter cases to incredibly rare diseases and provides you with incredible clinical training. She is a student in the Master’s in Health Policy Research program at UPenn and studies diagnostic delay in JIA. Her husband is a Pediatric sports medicine attending at CHOP and they have a daughter named Zoe who was born a couple of months prior to the start of fellowship! They love taking family walks around all the beautiful trails and parks in the Philly area.
Sarah McCuaig, MD, PhD: Sarah is a second-year fellow from Waterloo, Ontario, Canada. She has had a long-standing scientific passion for immunology and discovered her clinical love of pediatric rheumatology as a medical student. She completed her PhD (DPhil) at the University of Oxford with Fiona Powrie studying mucosal immunology. She then completed her medical degree at UPenn and her Pediatric Residency at CHOP. She is on the Accelerated Research Pathway and hopes to pursue a career as a physician-scientist. She is interested in tissue-specific drivers of inflammation in multi-organ system inflammatory disease. Most of all, she is excited to take care of our incredible patients and to have the privilege of being part of their journey! When not in the hospital or in the lab, she is an avid runner, enjoys all things outdoors (with a predilection for Nordic pursuits like cross country skiing), learning new skills (guitar, raised bed gardening), and spending time with friends and family. She is blissfully unaware of her Canadian accent and quintessentially loves maple syrup.
Brittney Newby, MD, PhD: Brittney is a second-year rheumatology fellow. Originally from Atlanta, she completed her undergraduate studies at FAMU before pursuing her MD-PhD at the University of Florida. Her thesis focused on unraveling the diabetogenic potential of Type 1 Interferon in Type 1 Diabetes. Following medical school, she completed her residency and a chief year at CHOP, where she discovered her true clinical passion in Rheumatology. Brittney has joined Dr. John E. Wherry's lab to utilize advanced immunoprofiling, proteomic, and transcriptomic approaches to predict clinical responses in rheumatologic and autoinflammatory diseases. She is particularly intrigued by the interplay between environmental factors and the shaping of the immunological landscape, leading to autoinflammation, autoimmunity, and immune dysregulation. Brittney aims to contribute valuable insights to this dynamic field to enhance the lives of her patients.
Outside of her professional pursuits, Brittney finds joy in spending quality time with her friends and family. Some of her favorite pastimes include softball, roller skating, reading, and traveling. Additionally, she indulges her passion for R&B and Soul music by attending concerts whenever her schedule allows, embracing the artistic and creative aspects of life.
Isabel Armendi, MD: Isabel Armendi is a first-year Rheumatology fellow and active-duty medical officer in the U.S. Army. She received her medical degree at the Jacobs School of Medicine and Biomedical Sciences in Buffalo, New York. She then completed her residency training at Madigan Army Medical Center in the Pacific Northwest. Isabel was drawn to Pediatric Rheumatology given the field’s breadth of complex pathology, its multidisciplinary nature, and opportunities to forge long-lasting relationships with patients, their caregivers, and fellow care-team. She is eager to partake in the field’s strong research efforts to better understand novel therapeutic potential to the full, and in turn, continue to improve the quality of life for those with Pediatric Rheumatologic disease. She also has strong interests in medical education, community outreach, and global health. Outside of work, she enjoys spending quality time with her partner and two pups – whether that be at a dog park, on a paddleboard, or somewhere exploring all that Philly has to offer.
Vinchelle Hardison, MD: Vinchelle is a 1st year fellow from rural Waynesville, MO. Though originally from the south (Mobile, AL) she spent most of her time in the mid-west, attending Mizzou for undergrad and Northeast Ohio Medical University for medical school. She completed her pediatric residency at Nationwide Children's Hospital. Vinchelle has always had interest in rheumatology, as she herself was diagnosed with various rheumatologic conditions as a child, and as she grew, decided to pursue medicine with a particular interest in Lupus and Mixed Connective Tissue Disease.
Outside of work, Vinchelle enjoys reading and geeking out on all things Marvel, Nintendo, and Anime. She's not above watching reality TV as well, snuggled on the couch with family, friends, and her 16 year old toy poodle.
Matthew Grunewald, MD: Matt is a first year Rheumatology fellow at CHOP. He attended Texas A&M for college where he majored in Biochemistry and Genetics. He then completed his MD/PhD at the University of Iowa with research focus in the immunologic response to coronavirus infection (finishing ironically the year before the COVID pandemic). He completed his pediatric residency training at Washington University in St. Louis before heading to Philadelphia. Matt is fascinated by immune dysregulation and how many diseases can be both pro- and anti-anti-immune at that the same time. Matt enjoys traveling with his family and can be found exploring the Philadelphia food scene with his wife and young daughter (who can be found choreographing dances to the Frozen soundtrack).
Research opportunities

Both clinical research and basic science research tracks are available to the fellow. The fellow is expected to lead a research project, of either a clinical or basic science nature, during the last two years of the fellowship program.
The program ensures a meaningful, supervised research experience based on early establishment of a mentor appropriate for the fellow's interests. The fellow is guided into appropriate training in order to successfully complete a research project over the course of the three-year program. The fellow may choose a clinically-based research project for which several mentors are available through the Divisions of Rheumatology at Penn or CHOP, or the fellow may choose a basic research laboratory-based project, for which there are dozens of mentors throughout the CHOP/Penn immunology community.
Related programs
CHOP clinical programs
Immune Dysregulation Program
Lupus Integrated Nephritis Clinic
Uveitis Coordinated Care Clinic
Amplified Musculoskeletal Pain Center
Pediatric Immunology
Pediatric Nephrology
Pediatric Dermatology
Pediatric Neuroinflammatory Disorders
Penn clinical programs
Adult Rheumatology
Adult Allergy and Immunology
Dermatology- Rheumatology
Clinical research
Center for Pediatric Clinical Effectiveness
Penn Master of Science in Clinical Epidemiology
Penn Master of Science in Health Policy Research
PolicyLab
CARRA
PR-COIN
Basic/translational research
Penn Immunology Graduate Group
Penn Institute for Immunology
Penn Cell and Molecular Biology Graduate Group
Penn Master of Science in Translational Research
Recent publications by fellows (last 5 years)
Basiaga ML, Burrows EK, Denburg MR, Meyers KE, Grossman AB, Mamula P, Grundmeier RW, Burnham JM. Variation in preventive care in children receiving chronic glucocorticoid therapy. J Pediatr, 179:226-232, December 2016. Epub September 2016.
Raslan A, Boneparth A, Leibowitz K, Bhise V, Basiaga ML, Burnham J, Moorthy N: Anti-MDA-5 associated arthritis and fasciitis in an 11-year-old Boy. Annals of Paediatric Rheumatology, January 2016 Notes: Online First.
Das R, Guan P, Sprague L, Verbist K, Tedrick P, An QA, Cheng C, Kurachi M, Levine R, Wherry EJ, Canna SW, Behrens EM, Nichols KE. Janus kinase inhibition lessens inflammation and ameliorates disease in murine models of hemophagocytic lymphohistiocytosis. Blood, 127(13):1666-75, March 31 2016. Epub Jan 29, 2016
Gmuca S, Boos MD, Treece A, Narula S, Billinghurst L, Bhatti T, Laje P, Perman MJ, Vossough A, Harding B, Burnham J, Banwell B. Degos disease mimicking primary vasculitis of the CNS. Neurol Neuroimmunol Neuroinflamm, 2;3(2):e206, February 2016.
Hoffart CM, Sherry DD: Fibromyalgia--toward a definition in children. J Pediatr, 169: 9-10, February 2016. Notes: epub December 9, 2015.
Weaver LK, Chu N, Behrens EM. TLR9-mediated inflammation drives a Ccr2-independent peripheral monocytosis through enhanced extramedullary monocytopoiesis. Proc Natl Acad Sci U S A, 27;113(39):10944-9, September 2016. Epub September 12, 2016.
Rood JE, Canna SW, Weaver LK, Tobias JW, Behrens EM. IL-10 distinguishes a unique population of activated, effector-like CD8+ T cells in murine acute liver inflammation. J Leukoc Biol, 101(4):1037-1044, April 2017. Epub December 29 2016.
Gmuca S, Lieberman SM, Mehta J. Pediatric neuromyelitis optica spectrum disorder and Sjögren Syndrome: More common than previously thought? J Rheumatol, 44(6):959-960, June 2017.
Manos CK, Xiao R, Brandon TG, Burnham JM, Zemel BS, Weiss PF. Obesity and pediatric psoriatic arthritis. Ann Paediatr Rheumatol, 6(2):34-40, 2017. Gmuca S, Xiao R, Brandon TG, Pagnini I, Wright TB, Beukelman T, Morgan EM, Weiss PF. Multicenter inception cohort of enthesitis-related arthritis: variation in disease characteristics and treatment approaches. Arthritis Res Ther, 19(1):84, May 2017.
Tiao J, Feng R, Berger EM, Brandsema JF, Coughlin CC, Khan N, Kichula EA, Lerman MA, Lvovich S, McMahon PJ, Rubin AI, Scalzi LV, Smith DM, Taxter AJ, Treat JR, Williams RP, Yum SW, Okawa J, Werth VP : Evaluation of the reliability of the cutaneous dermatomyositis disease area and severity index and the cutaneous assessment tool binary method in juvenile dermatomyositis among paediatric dermatologists, rheumatologists and neurologists. Br J Dermatol, 177(4):1086-1092, October 2017.
Chang JC, Knight AM, Xiao R, Mercer-Rosa LM, Weiss PF. Use of echocardiography at diagnosis and detection of acute cardiac disease in youth with systemic lupus erythematosus. Lupus, 27(8):1348-1357, July 2018. Epub 2018 Apr 2018.
Chang JC, Xiao R, Mercer-Rosa L, Knight AM, Weiss PF. Child-onset systemic lupus erythematosus is associated with a higher incidence of myopericardial manifestations compared to adult-onset disease. Lupus, 27(13):2146-2154, November 2018. Epub 2018 October 14, 2018.
Chang JC, Mandell DS, Knight AM. High Health Care Utilization Preceding Diagnosis of Systemic Lupus Erythematosus in Youth. Arthritis Care Res (Hoboken), 70(9):1303-1311, September 2018. Epub August 16, 2018.
Gmuca S, Xiao R, Weiss PF, Waldman AT, Gerber JS. Use of rituximab and risk of re-hospitalization for children with neuromyelitis optica spectrum disorder. Mult Scler Demyelinating Disord, 3:3. Epub April 17, 2018.
Gmuca S, Yu J, Weiss PF, Treat JR, Sherry DD: Erythema Ab Igne in an adolescent with chronic pain: An alarming cutaneous eruption from heat exposure. Pediatric Emerg Care, March 2018. Gmuca S, Sherry DD. Fibromyalgia: Treating Pain in the Juvenile Patient. Paediatr Drugs,19(4):325-338, August 2017.
James KE, Xiao R, Merkel PA, Weiss PF. Variation in the Treatment of Children Hospitalized With Antineutrophil Cytoplasmic Antibody-Associated Vasculitis in the US. Arthritis Care Res (Hoboken), 69(9):1377-1383, September 2017. Epub August 13, 2017. James KE, Xiao R, Merkel PA, Weiss PF. Clinical course and outcomes of childhood-onset granulomatosis with polyangiitis. Clin Exp Rheumatol, 35 Suppl 103(1):202-208, March/April 2016. Epub October 2016.
Brandon TG, Manos CK, Xiao R, Ogdie A, Weiss PF. Pediatric psoriatic arthritis: a population-based cohort study of risk factors for onset and subsequent risk of inflammatory comorbidities. J Psoriasis Psoriatic Arthritis, 3(4):131-136, October 2018. Epub 2018 Sep 18.
Le Coz C, Nolan BE, Trofa M, Kamsheh AM, Khokha MK, Lakhani SA, Novelli A, Zackai EH, Sullivan KE, Briuglia S, Bhatti TR, Romberg N. Cytotoxic T-lymphocyte-associated protein 4 haploinsufficiency-associated inflammation can occur independently of T-cell hyperproliferation. Front Immunol, 24;9:1715, July 2018.
Buckley L, Ware E, Kreher G, Wiater L, Mehta J, Burnham JM: Outcome monitoring and clinical decision support in polyarticular juvenile idiopathic arthritis. J Rheumatol, 47(2): 273-281, February 2020.
Chang JC, White BR, Elias MD, Xiao R, Knight AM, Weiss PF, Mercer-Rosa L: Echocardiographic assessment of diastolic function in children with incident systemic lupus erythematosus. Pediatric Cardiology, 40(5):1017-1025, June 2019.
Liebling EJ, Peterson R, Victoria T, Burnham JM: Aortic ulceration in a tocilizumab-treated patient with Takayasu arthritis. Ann rheum Dis, 78(10), October 2019.
Romberg N, Le Coz C, Glauzy S, Schickel JN, Trofa M, Nolan BE, Paessler M, Xu ML, Lambert MP, Lakhani SA, Khokha MK, Jyonouchi S, Heimall J, Takach P, Maglione PJ, Catanzaro J, Hsu FI, Sullivan KE, Cunningham-Rundles C, Meffre E. Patients with common variable immunodeficiency with autoimmune cytopenias exhibit hyperplastic yet inefficient germinal center responses. J Allergy Clin Immunol,143(1):258-265, January 2019. Epub June 2018.
Chang JC, Buckley LH, Goldberg T, Nolan BE, Peterson R, Liebling EJ, Waqar LN, Burnham JM. Enhancing communication and social engagement among clinicians and research teams to improve reliability of research recruitment. BMJ Open Qual, 8(4), November 2019.
Kushner CJ, Tarazi M, Gaffney RG, Feng R, Ardalan K, Brandling-Bennett H, Castello-Soccio L, Chang JC, Chiu YE, Gmuca S, Hunt RD, Kahn P, Knight AM, Mehta J, Pearson DR, Treat JR, Wan J, Yeguez A, Concha JS, Patel B, Okawa J, Arkin LM, Werth VP: Evaluation of the reliability and validity of the cutaneous lupus erythematosus disease area and severity index (CLASI) in pediatric cutaneous lupus among pediatric dermatologist and rheumatologists. British Journal of Dermatology, 180(1):165-171, January 2019.
Gmuca S, Xiao R, Weiss PF, Sherry DD, Knight AM, Gerber JS. Opioid prescribing and polypharmacy in children with chronic musculoskeletal pain. Pain Med, 20(3):495-503, March 2019.
Liebling EJ, Sze RW, Behrens EM. Vitamin C deficiency mimicking inflammatory bone disease of the hand. Pediatr Rheumatol Online J,18(1):45, June 2020.
Gordon SM, Nishiguchi MA, Chase JM, Mani S, Mainigi MA, Behrens EM. IFNs Drive Development of Novel IL-15-Responsive Macrophages. J Immunol. 2020 Aug 15;205(4):1113-1124. doi: 10.4049/jimmunol.2000184. Epub 2020 Jul 20.
Vella LA, Giles JR, Baxter AE, Oldridge DA, Diorio C, Kuri-Cervantes L, Alanio C, Pampena MB, Wu JE, Chen Z, Huang YJ, Anderson EM, Gouma S, McNerney KO, Chase J, Burudpakdee C, Lee JH, Apostolidis SA, Huang AC, Mathew D, Kuthuru O, Goodwin EC, Weirick ME, Bolton MJ, Arevalo CP, Ramos A, Jasen CJ, Conrey PE, Sayed S, Giannini HM, D'Andrea K; UPenn COVID Processing Unit, Meyer NJ, Behrens EM, Bassiri H, Hensley SE, Henrickson SE, Teachey DT, Betts MR, Wherry EJ. Deep immune profiling of MIS-C demonstrates marked but transient immune activation compared to adult and pediatric COVID-19. Sci Immunol. 2021 Mar 2;6(57):eabf7570.
Diorio C, McNerney KO, Lambert M, Paessler M, Anderson EM, Henrickson SE, Chase J, Liebling EJ, Burudpakdee C, Lee JH, Balamuth FB, Blatz AM, Chiotos K, Fitzgerald JC, Giglia TM, Gollomp K, Odom John AR, Jasen C, Leng T, Petrosa W, Vella LA, Witmer C, Sullivan KE, Laskin BL, Hensley SE, Bassiri H, Behrens EM, Teachey DT. Evidence of thrombotic microangiopathy in children with SARS-CoV-2 across the spectrum of clinical presentations. Blood Adv. 2020 Dec 8;4(23):6051-6063
Anderson EM, Diorio C, Goodwin EC, McNerney KO, Weirick ME, Gouma S, Bolton MJ, Arevalo CP, Chase J, Hicks P, Manzoni TB, Baxter AE, Andrea KP, Burudpakdee C, Lee JH, Vella LA, Henrickson SE, Harris RM, Wherry EJ, Bates P, Bassiri H, Behrens EM, Teachey DT, Hensley SE. Severe Acute Respiratory Syndrome-Coronavirus-2 (SARS-CoV-2) Antibody Responses in Children With Multisystem Inflammatory Syndrome in Children (MIS-C) and Mild and Severe Coronavirus Disease 2019 (COVID-19). J Pediatric Infect Dis Soc. 2021 May 28;10(5):669-673
Vella L, Giles JR, Baxter AE, Oldridge DA, Diorio C, Kuri-Cervantes L, Alanio C, Pampena MB, Wu JE, Chen Z, Huang YJ, Anderson EM, Gouma S, McNerney KO, Chase J, Burudpakdee C, Lee JH, Apostolidis SA, Huang AC, Mathew D, Kuthuru O, Goodwin EC, Weirick ME, Bolton MJ, Arevalo CP, Ramos A, Jasen C, Giannini HM, DAndrea K, Meyer NJ, Behrens EM, Bassiri H, Hensley SE, Henrickson SE, Teachey DT, Betts MR, Wherry EJ. Deep Immune Profiling of MIS-C demonstrates marked but transient immune activation compared to adult and pediatric COVID-19. medRxiv [Preprint]. 2020 Sep 27:2020.09.25.20201863. doi: 10.1101/2020.09.25.20201863. Update in: Sci Immunol. 2021 Mar 2;6(57)
Diorio C, Anderson EM, McNerney KO, Goodwin EC, Chase JC, Bolton MJ, Arevalo CP, Weirick ME, Gouma S, Vella LA, Henrickson SE, Chiotos K, Fitzgerald JC, Kilbaugh TJ, John ARO, Blatz AM, Lambert MP, Sullivan KE, Tartaglione MR, Zambrano D, Martin M, Lee JH, Young P, Friedman D, Sesok-Pizzini DA, Hensley SE, Behrens EM, Bassiri H, Teachey DT. Convalescent plasma for pediatric patients with SARS-CoV-2-associated acute respiratory distress syndrome. Pediatr Blood Cancer. 2020 Nov;67(11):e28693. doi: 10.1002/pbc.28693. Epub 2020 Sep 4.
Anderson EM, Diorio C, Goodwin EC, McNerney KO, Weirick ME, Gouma S, Bolton MJ, Arevalo CP, Chase J, Hicks P, Manzoni TB, Baxter AE, Andrea KP, Burudpakdee C, Lee JH, Vella LA, Henrickson SE, Harris RM, Wherry EJ, Bates P, Bassiri H, Behrens EM, Teachey DT, Hensley SE. SARS-CoV-2 antibody responses in children with MIS-C and mild and severe COVID-19. medRxiv [Preprint]. 2020 Aug 18
Diorio C, Henrickson SE, Vella LA, McNerney KO, Chase J, Burudpakdee C, Lee JH, Jasen C, Balamuth F, Barrett DM, Banwell BL, Bernt KM, Blatz AM, Chiotos K, Fisher BT, Fitzgerald JC, Gerber JS, Gollomp K, Gray C, Grupp SA, Harris RM, Kilbaugh TJ, John ARO, Lambert M, Liebling EJ, Paessler ME, Petrosa W, Phillips C, Reilly AF, Romberg ND, Seif A, Sesok-Pizzini DA, Sullivan KE, Vardaro J, Behrens EM, Teachey DT, Bassiri H. Multisystem inflammatory syndrome in children and COVID-19 are distinct presentations of SARS-CoV-2. J Clin Invest. 2020 Nov 2;130(11):5967-5975
Argraves M, Mehta JJ. Pediatric rheumatology: Not just a little adult workforce issue. Semin Arthritis Rheum. 2020 Dec 21:S0049-0172(20)30288-2.
Rutstein BH, Gmuca S, Gerber JS, Lim T, Argraves M, Ogdie A. Validation of coding algorithms for the identification of herpes zoster among children. Pharmacoepidemiol Drug Saf. 2021 May 7.
Peterson RG, Xiao R, James KE, Katcoff H, Fisher BT, Weiss PF. Variation in treatment of children hospitalized with new-onset systemic juvenile idiopathic arthritis in the United States. Arthritis Care Res (Hoboken). 2020 Aug 16
Liebling EJ, Faig W, Chang JC, Mendoza E, Moore N, Ledesma Vicioso N, Lerman MA. The temporal relationship between juvenile idiopathic arthritis disease activity and uveitis activity. Arthritis Care Res (Hoboken). 2020 Oct 12.
Bayefsky, S.D., DeQuattro K., & Sadun R.E. “Tips for Transitioning Patients from Pediatric to Adult Rheumatology Care.” The Rheumatologist (pgs. 27–29), Oct. 2021.
How to apply
Our three-year fellowship seeks physicians who will have completed two to three years of training in an accredited residency program in order to sit for the American Board of Pediatrics certifying examination. Our fellowship program participates in the ERAS universal application process. Please visit their Web site for application information about this program.
The following information should be uploaded into this program:
- Completed ERAS application
- At least three letters of reference, including one from your residency program director
- MSPE and medical school transcript
- A personal statement describing career goals and reasons for continuing training in pediatric rheumatology
- Parts 1, 2 and 3 of the USMLE taken within the seven year time frame as required by the Commonwealth of Pennsylvania or equivalent scores
- If a graduate of a medical school outside the United States, Canada or Puerto Rico, valid ECFMG certificate or one that does not expire prior to the start of the fellowship
- If not a citizen of the United States, copy of permanent resident card or copy of current, appropriate visa
National resident matching program (NRMP)
The Pediatric Rheumatology Fellowship program participates in the National Resident Matching Program (http://www.nrmp.org).
Other requirements
To carry out its mission, it is of critical importance for the Children’s Hospital of Philadelphia (CHOP) to keep our patients, families and workforce safe and healthy and to support the health of our global community. In keeping with this, CHOP has mandated all workforce members (including trainees) on site at any CHOP location for any portion of their time be vaccinated for COVID-19 as a condition of employment.
This mandate also applies to workforce members or trainees performing work for CHOP at non-CHOP locations. Additionally, all workforce members based in or regularly scheduled to work at any New Jersey location are mandated to be both vaccinated and boosted for COVID-19, with booster timing consistent with applicable guidelines. The CHOP COVID-19 vaccine mandate is in alignment with applicable local, state and federal mandates. CHOP also requires all workforce members and trainees who work in patient care buildings or who provide patient care to receive an annual influenza vaccine. Employees may request exemption consideration for CHOP vaccine requirements for valid religious and medical reasons. Please note start dates may be delayed until candidates are fully immunized or valid exemption requests are reviewed. In addition, candidates other than those in positions with regularly scheduled hours in New Jersey, must attest to not using tobacco products.
Children's Hospital of Philadelphia is an equal opportunity employer. We do not discriminate on the basis of race, color, gender, gender identity, sexual orientation, age, religion, national or ethnic origin, disability, protected veteran status or any other protected category. CHOP is a VEVRAA Federal Contractor seeking priority referrals for protected veterans.
CHOP is committed to building an inclusive culture where employees feel a sense of belonging, connection, and community within their workplace. We are a team dedicated to fostering an environment that allows for all to be their authentic selves. We are focused on attracting, cultivating, and retaining diverse talent who can help us deliver on our mission to be a world leader in the advancement of healthcare for children.
We strongly encourage all candidates of diverse backgrounds and lived experiences to apply.
Contact
Claire O’Malley
Fellowship Administrator
Children's Hospital of Philadelphia
Pediatric Rheumatology Fellowship
3615 Civic Center Blvd., 1102 ARC
Philadelphia PA 19104-4318
215-590-7180
omalleyc@chop.edu